Meniscal injury is one of the major causes of knee pain, func- tional limitation and diminished joint stability. The biomechanical function of the meniscus is paramount, contributing to load distribution, shock absorption, joint congruity, and protecting the articular cartilage. Acute trauma or chronic mechanical stress to this fibrocartilaginous structure can cause a breakdown of normal hip biomechanics, and patients often present with pain, swelling, loss of range of motion (ROM), and difficulty with weight-bearing activity. Untreated or poorly healing meniscal pathology may also be a factor in the progressive degenerative process within the joint and therefore promoted long-term osteoarthritic change.
While the management of rotator cuff tears can be viewed as conservative with surgical intervention remaining the cornerstone of contemporary management, a growing interest in regenerative approaches that may aid tissue healing and alter the local inflammatory milieu is being pursued. Out of these strategies, the use of umbilical cord-derived mesenchymal stromal or stem cells (UC-MSCs) has garnered significant interest, partly due to both immunomodulatory and paracrine signaling capacity. However, their role in meniscal injury should currently be designated investigational rather than established standard therapy.
Biological Mechanisms of Meniscal Injury
Meniscal tears are usually created in situations of excessive rotational force, compressive loading, or unaccustomed mechanical repetition that exceeds the structural limit of meniscal fibrocartilage. Acute injury usually results from sports or twisting trauma, while degenerative tearing favours progressive thinning of tissue that takes place due to age and chronic overuse. Collagen meshwork disruption causes loss of load distribution across the knee but, at the tissue level as well, incapacitates the meniscus.
The meniscus has a key role in injury as abnormal contact mechanics can subsequently increase stress between the femoral condyle and tibial plateau once compromised. The modified pattern of loading may be involved in not only local pain and swelling, but also secondary irritation of the synovium and progressive damage to adjacent cartilage. Due to its poor vascularity, the meniscus has limited capacity for spontaneous healing; hence spontaneous healing is likely biologically restricted in complex or poorly perfused tears.
Ultimately, the clinical impacts of meniscal injury are not limited solely to the original tear. Ongoing disruption to the structure should predispose to chronic inflammation, poor biomechanics, impaired joint stability and perhaps over time enhanced cartilage degeneration. Consequently, meniscal tears have been recognized as not just an isolated orthopedic lesion, but rather a biologically significant injury affecting the overall health status of adjacent articulations in relation to joint preservation.
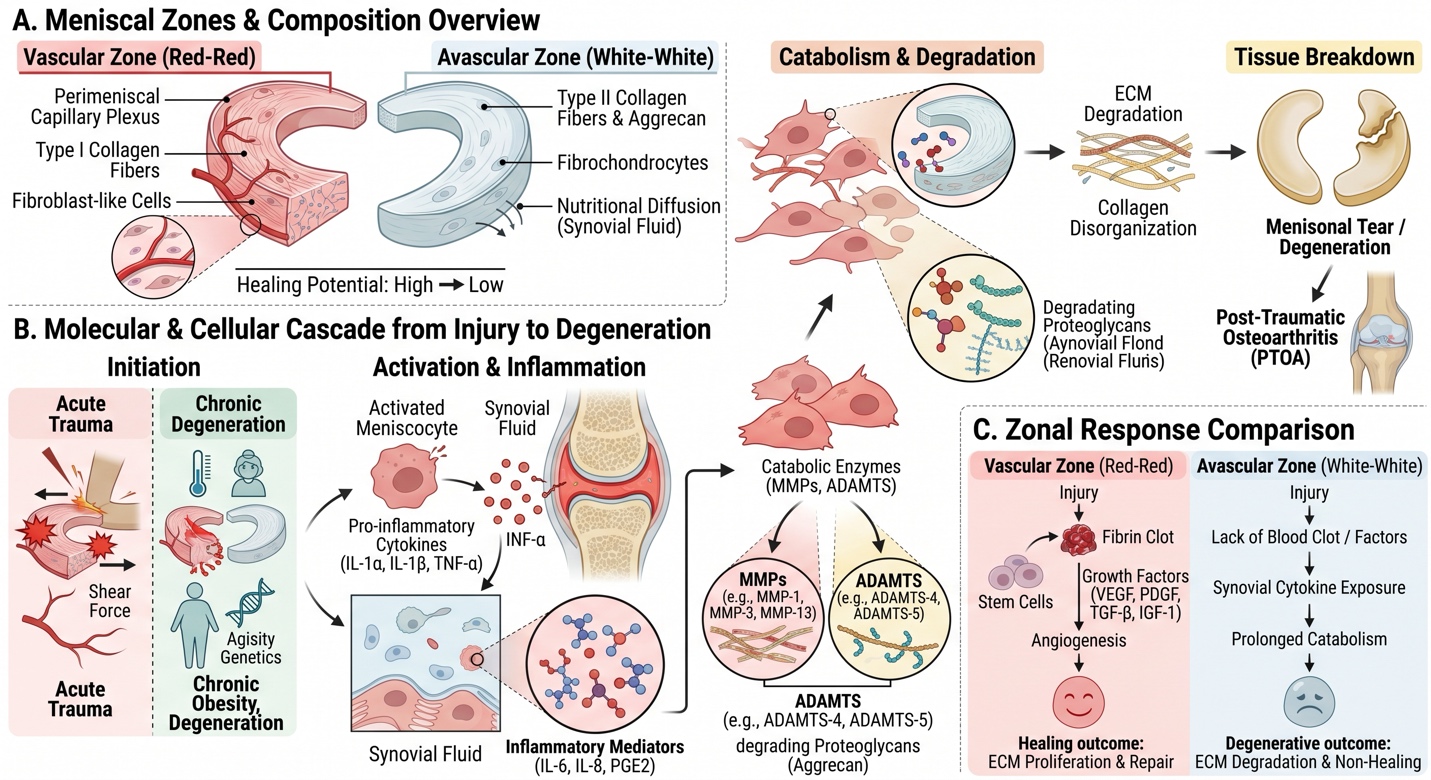
Figure 1: Biological Mechanisms of Meniscal Injury
The Limitation of Current Treatment Strategies
The treatment of meniscal tears is guided chiefly by the tear pattern and location, severity of symptoms, age and activity level of the patient, and presence or absence of mechanical symptoms. Activity modification, physiotherapy, and use of nonsteroidal anti-inflammatory drugs (NSAIDs), in the form of structured rehabilitation is often used as initial treatment. Supported: TherapeuTic aTherapies; deQuita TM joint bracing These modalities could help patients with particular non-displaced or degenerative tears by diminishing agony and enhancing function.
Surgical options are indicated when there is persistent intra-articular hemorrhage, locking or ifthe tear becomes structurally unstable. Rehabilitation protocol Meniscal Repair/Partial meniscectomy Surgical procedure and rehabilitation Common procedures are indicated as meniscal repair or partial meniscectomies. Although these interventions can temporarily relieve symptoms, they also come with limitations. Partial meniscal resection decreases meniscal volume and has been associated with increases in contact stress throughout the knee joint that may ultimately result in cartilage wear over time. Meniscal repair preserves more tissue but is not appropriate for all tear types and can be affected by vascular zone as well as the geometrical classification of meniscal tears and their healing characteristics.
However, these limitations have prompted ongoing interest in biologically focused strategies designed to address both symptom relief and tissue repair while minimizing the effects on joint mechanics. Regenerative medicine represents an active area of research in this setting.
What is UC-MSC: Why Therapies Based on These Cells Are Being Investigated
UC-MSCs were chosen for use in meniscal injury as they are known to modulate the local tissue environment via anti-inflammatory, immunomodulatory and trophic signaling. Mesenchymal stromal cells are commonly described as biologically active signaling cells that may augment endogenous repair pathways instead of only acting as direct replacement cells.
These proposed mechanisms are suggested through modulation of inflammatory cytokine activity, support of matrix synthesis and resident cell behavior, or secretion of growth factors and extracellular vesicles which may influence remodeling. These signals have been associated with effects on chondrocytes, synovial inflammation, matrix homeostasis and zona microenvironment in experimental and translational settings.
This is particularly relevant to meniscal injury as structural failure is often accompanied by the creation of a biologically hostile in situ healing environment. Possible factors limiting repair include reduced blood supply, chronic inflammation and abnormal joint mechanics. This is why there has been interest in using UCMSCs for enhancing the potential of preservation and biological recovery at a time when healing is otherwise impaired.
But, certainly also a word of caution not to overstate it. The biological rationale is strong but current evidence precludes an assertion on UC-MSCs as a complete or generalizable regenerative approach for meniscal tears. The clinical role of these therapies is still being defined, and a number of fundamental questions remain regarding cell source, dose, delivery method, treatment timing, patient selection and the durability of long-term outcomes.
Emerging Translational Opportunities in Thailand
As an area for translational and clinical activity in regenerative medicine, Thailand has came more into view as of late. Interest in cell-based approaches to musculoskeletal disorders has been witnessed as laboratory infrastructure, orthopedic specialization, and advanced biologic processing systems have developed during the last 20 years. This now puts the area in a position to partake in novel studies utilizing non-surgical and adjunctive regenerative therapies for joint injury.
For the academic disciplines, it is not in the woo-factor of this development that significance rests but rather from the potential to support better-constructed research settings. Advances in this area require compliance with quality controls, rigorous regulatory processes, harmonized product characterization, physician-directed treatment regimens, and appropriate long-term clinical follow-up. If all of these things happen, the region may play a role in the larger story about where and how biologic therapies could be integrated into orthopedic care.
Contextualisation and the Healing Meanings
If the goal is to preserve the normal function of menisci, it has become critical that we also understand biologic healing in meniscal injury as the orthopaedic practice paradigm moves from extraction of pathology against preservation of joint. In this context, what makes UC-MSCs appealing is their ability to potentially enhance a more regenerative repair environment instead of just alleviating symptoms. That includes, management of inflammatory burden if appropriate, rescues of matrix stability and supportive in maintaining tissue function when selected.
Still a well-balanced interpretation is needed regardless. Introduction: Meniscal tears are heterogeneous and not all injuries confer the same biologic or mechanical consequences. Some cases rehabilitate well, while some demand surgical stabilization and others ultimately may warrant consideration for adjunctive biologic inquiry. The essential question for patients is not so much whether one therapy sounds sexier than another, but if the treatment plan is appropriate in relation to matching up with their tear pattern, structural status of the knee and long-term goals of care.
Conclusion
Meniscal injury is a common and clinically important problem affecting biomechanics, pain, function and long term disease of the joint. Contemporary care has treatment modalities hinged around conventional treatments, however critical limitations remain especially within tissues limited in their natural healing potential. Hence, UC-MSC will capture interest as a new scientific approach due to its anti-inflammatory and tissue-supportive biology.
Currently, it is best to think of these therapies are exploratory and developing rather than properly standard treatment. Their worth will rely on better-standardized protocols and stronger clinical evidence combined with improved identification of which patients stand to benefit most. The progressive implementation of not only symptom control, but also biologically informed strategies related to meniscal retention in order to maintain joint structure and function from a modern orthopedic, regenerative medicine perspective.

