A stroke can change a person’s life in a single moment. One day, walking, speaking, swallowing, writing, or remembering may feel normal. The next day, the body may no longer respond in the same way. For many patients and families, the most difficult part of Stroke is not only the emergency itself, but the long recovery journey that follows.
This is exactly the reason why a lot of people are now looking for a stem cell clinic that views Stroke in wider medical terms. Conventional care, of course, is still important with respect to emergency treatment, drugs, and rehabilitation, as well as long-term risk control. However, once that acute phase is past, some patients start to ask a new question: Is there any way they can more powerfully support the brain recovery environment?
Within regenerative medicine, the answer is nevertheless in progress. Due to their capacity for attenuating inflammation, signaling vascular repair, neuroprotection, and inter-tissue communication might be modified cold with an extensive range of stem-cell-based programs for Stroke. Contemporary reviews illustrate that mesenchymal stem/ stromal cells are an appealing source for a candidate cell type in Stroke, but continue to emphasize the requirement of stronger clinical data and standardized procedures.
Understanding Stroke Beyond the Initial Event
A Stroke happens when the blood supply to part of the brain is interrupted or when bleeding occurs inside or around the brain. Ischemic Stroke, caused by blocked blood flow, is the most common type. Hemorrhagic Stroke, caused by bleeding, has a different biological profile and often requires different medical decisions.
The Biology After Stroke
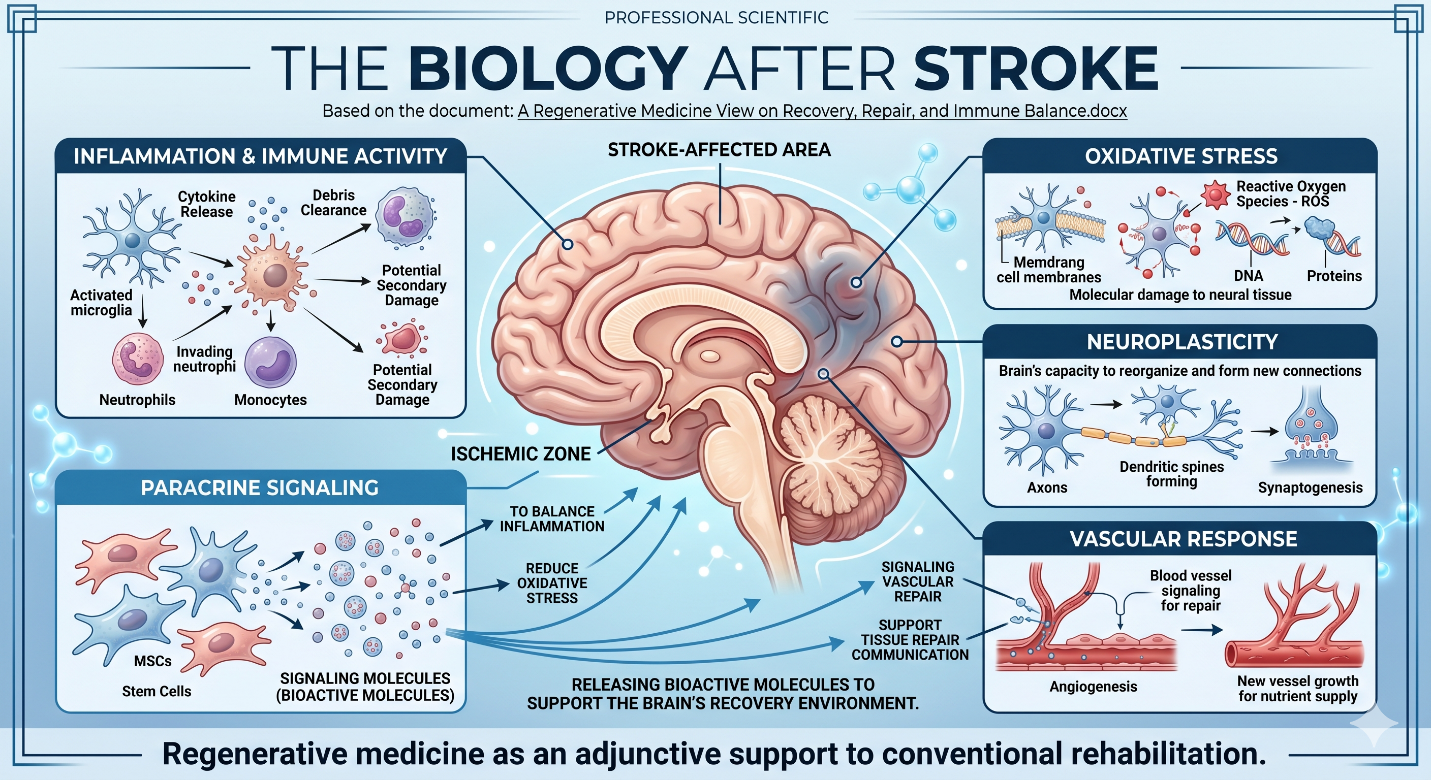
After a Stroke, the brain does not simply “stop healing.” In fact, many biological processes become active. Inflammation, oxidative stress, immune cell activity, blood vessel response, scar formation, and neuroplasticity all influence recovery.
This is where a responsible stem cell clinic should be careful with language. The goal is not to claim that cells can reverse Stroke damage or rebuild the brain overnight. A more realistic and scientific view is that regenerative medicine may help support the biological environment around recovery.
For patients, that distinction matters. Stroke recovery is usually gradual. It depends on the location of injury, severity, age, timing of treatment, rehabilitation intensity, underlying health conditions, and the brain’s ability to reorganize itself.
Why Patients Search for a Stem Cell Clinic After Stroke
A large number of Stroke patients get to the point where conventional rehabilitation challenges or helps, but slower progress is made. In particular, this can occur months after the event, particularly when weakness, speech difficulty, balance problems, fatigue, or cognitive changes persist.
When patients seek ways to amplify their recovery beyond traditional rehab, a stem cell clinic may come up in the conversation. That, however, should not be positioned as an alternative to neurologists or physiotherapists or occupational therapists — speech therapists too, in that, also medication management.
What a Responsible Stem Cell Clinic Should Explain
A reputable stem cell clinic will detail that regenerative care for Stroke is a new area of medical science. Regenerative medicine therapies have not been approved by the U.S. FDA to treat neurological disorders like Stroke. It warns that unapproved regenerative products could pose risks, such as infection or unwanted immune responses, tumor formation, and other serious side effects.
This does not mean science is meaningless. Patients need to see the truth in guidance. Separate marketing promises from research potential at a serious stem cell clinic.
· Stem Cells and Stroke: What Researchers Are Studying
Not all stem cells are created equal. Various reasons have been proposed to study stroke research focusing on mesenchymal stem/stromal cells, neural stem cells, and other cell-based approaches. Among these, mesenchymal cells are particularly cited for their potential to secrete bioactive molecules that modulate inflammation and immune responses, as well as angiogenesis and tissue regeneration signals.
Paracrine Signaling: The More Realistic Explanation
A common misunderstanding is that stem cells simply become new brain cells after infusion. In reality, much of the interest comes from paracrine signaling. This means the cells may release molecules that communicate with surrounding tissues and immune cells.
For Stroke, this may include signals related to:
inflammatory balance
blood vessel support
oxidative stress response
neurotrophic support
immune regulation
tissue repair communication
A stem cell clinic that presents Stroke treatment responsibly should focus on these supportive mechanisms rather than promising complete neurological restoration.
Stroke Recovery Needs More Than One Tool
Stroke recovery is rarely solved by one intervention. The strongest long-term plan is usually layered. Medication may reduce future Stroke risk. Rehabilitation helps retrain movement, speech, balance, and daily function. Nutrition supports metabolic and vascular health. Sleep, stress control, and exercise influence brain recovery.
Where Regenerative Medicine May Fit
A stem cell clinic may discuss cell-based support as an adjunctive option for selected Stroke patients, especially when the patient is medically stable and has already completed a proper neurological evaluation. The timing, route, cell source, dosage concept, and follow-up plan should be individualized.
But the foundation should remain clear: regenerative care must work alongside standard Stroke care, not against it.
NK Cell Expansion and Stroke: A Careful Immune Perspective
The secondary keyword, NK cell expansion, needs a careful explanation. Natural killer cells are part of the innate immune system. They are best known for their role in immune surveillance, especially in cancer biology and viral defense. In medical research, NK cell expansion usually refers to laboratory methods used to grow and activate NK cells for clinical or investigational immune applications.
Recent reviews describe NK cell expansion as an active field mainly connected with adoptive cell therapy and immunotherapy development, not as a standard treatment for Stroke.
Why NK Cell Expansion Should Not Be Overlinked to Stroke
A responsible stem cell clinic should not claim that NK cell expansion directly repairs Stroke damage. That would be scientifically misleading. However, immune balance is still relevant to recovery. After a stroke, the immune system can influence inflammation, infection risk, and tissue response. For this reason, some advanced clinics may evaluate immune status as part of a broader regenerative and wellness assessment.
The key is positioning. NK cell expansion may belong in the broader field of immune cell science, but it should not be marketed as a proven Stroke recovery method. For Stroke patients, safety and evidence must come first.
What Patients Should Look for in a Stem Cell Clinic
Choosing a stem cell clinic for Stroke-related support should be done carefully. Patients and families are often vulnerable after a serious neurological event, and unrealistic promises can create false hope.
Medical Evaluation First
A proper clinic should review the Stroke type, date of onset, MRI or CT findings, neurological deficits, current medications, blood pressure, cardiovascular risk factors, and rehabilitation history.
Clear Safety Standards
A reliable stem cell clinic should provide transparent information about cell source, laboratory standards, sterility testing, physician supervision, and follow-up care.
No Guaranteed Claims
A serious clinic should avoid phrases such as “cure Stroke,” “reverse paralysis,” or “guaranteed recovery.” Stroke recovery is complex, and outcomes vary widely.
Integration With Rehabilitation
A good regenerative plan should encourage rehabilitation, not replace it. Physical therapy, speech therapy, occupational therapy, and neurological monitoring remain central to functional recovery.
A Balanced Future for Stroke Support
Stroke care could be individualized in the future. Patients may experience support for emergency treatment and rehabilitation, but also biological benefits intended towards inflammation, vascular health, cellular conversation, or immune balancing.
This is where the role of a stem cell clinic might be evolving next. This model is not permissive of miracle claims, which by definition are miraculous. It is based on rigorous patient selection, achievable endpoints, Good Manufacturing Practice (GMP)-certified cellular processing, and neurological collaboration with long-term clinical follow-up.
Currently, stem cell approaches for Stroke must be regarded as experimental or adjunctive depending on the clinical setting and applicable regulations. You have compelling science, but it is not yet fully baked.
Conclusion
A modern stem cell clinic should approach Stroke with both hope and discipline. Hope matters because patients and families need options, motivation, and continued support. Discipline matters because Stroke is a serious neurological condition, and exaggerated claims can be harmful.
Stem cell research may offer meaningful insight into inflammation balance, neurovascular repair signaling, and recovery support after Stroke. At the same time, NK cell expansion should be discussed only in its proper scientific context: an advanced immune cell technology field, not a proven Stroke treatment.
For patients exploring regenerative medicine after a stroke, the best path is a medically guided one. A responsible stem cell clinic should support the patient’s recovery journey with honesty, safety, and science — not shortcuts.


