Degenerative musculoskeletal disorders are one of the most common causes of chronic pain, reduced mobility, and quality of life deterioration in aging populations. Disease can affect joints, cartilage, tendons, ligaments and the tissue surrounding them, which may over time limit Mobility independence and daily function. For lots of individuals, the problem equally isn’t just a occasional discomfort. Joint stiffness, inflammation and structural tissue changes progressive can gradually make simple activities more difficult, such as walking, climbing stairs or exercising or even standing for long periods of time.
In modern medicine there is more interest in approaches that accomplish more than just short-term symptom alleviation. This has resulted in increased interest in Anti-Aging Stem Cell Nutrition and Improves Joint Mobility Therapy as part of expansive regenerative medicine. These strategies are all designed to enhance the biology of aging tissues, support those cells that do survive from genetic damage and infection as time progresses on.
I. The Biological Basis for Degeneration of a Joint
Aging tissues at the cellular level are frequently characterized by reduced mitochondrial efficiency, limp repair signaling pathways, and increased oxidative stress. These alterations may impair the chondrocyte, synovial cell and connective tissue cells’ capacity for maintaining healthy joint structure. This “compliance deficit” can lead to stiffness, delay recovery time and worsen slumped posture leading to a concern that the joints eventually lose flexibility.
This is why the new regenerative medicine of today tends to view joint health through a lens that transcends that of simple mechanical failure. A cellular and biochemical problem, too. Therefore, supporting the tissue microenvironment may have significance for long-term joint mobility.
Common Treatments for Joint Mobility
Standard treatment for degenerative joint disease typically involves managing pain with analgesic or nonsteroidal anti-inflammatory drugs, physical therapy, corticosteroid or hyaluronic acid injections, and in advanced cases surgery to replace the joint. These choices can be useful and have been significant, because in clinical practice it still matters. These treatments may palliate the clinical signs somewhat, [but] will not reverse the underlying biological changes that lead to tissue degeneration.
Pain medication can make it easier to bear but does not regenerate cartilage. Despite the conjugation of anti-inflammatory drugs to ameliorate local inflammation, normal quality of the joint microenvironment may not be restored. Invasive procedure, surgery may be needed for serious structural damage. Consequently, a vast number of patients and clinicians are looking for integrative options that may cover the factors contributing to factors affecting mobility, tissue health and cellular resilience more thoroughly.
Cellular Support and Anti-Aging Stem Cell Nutrition
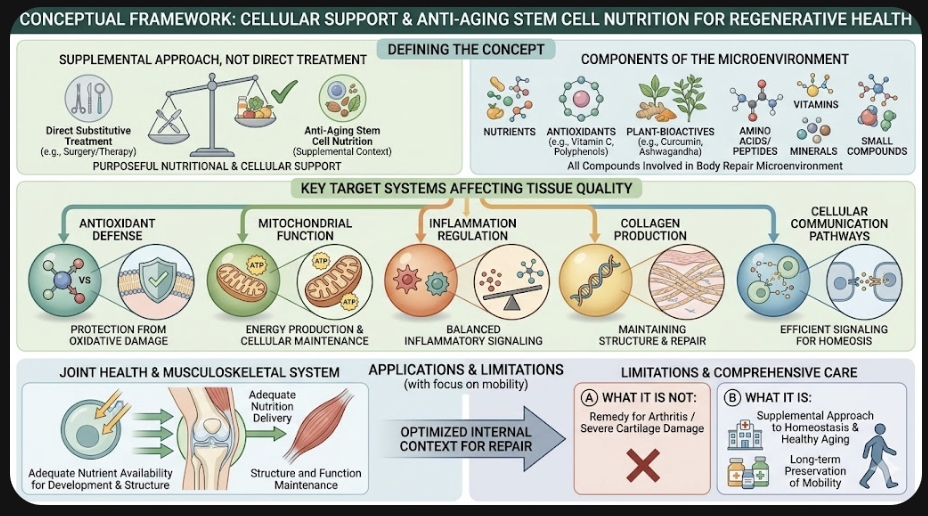
Anti-Aging Stem Cell Nutrition, A concept based on the idea that healthy biological function can be maintained by purposeful nutritional and cellular support as the body ages. Instead of being a direct substitution for the treatment itself, this mechanism might enable cellular maintenance by means of nutrients, antioxidants and/or plant–bioactives, amino acids/peptides, vitamins, minerals and all other small compounds that participate in the microenvironment involved in body repair.
The aim is to impact those systems which affect tissue quality, e.g. antioxidant defense, mitochondrial function, inflammation regulation, collagen production and cellular communication pathways. These mechanisms are of interest in a joint health context as musculoskeletal tissues develop, maintain structure and function by virtue of adequate nutrient availability and balanced inflammatory signaling.
At the right place, Anti-Aging Stem Cell Nutrition can be defined as a supplemental approach to cellular homeostasis, maintenance of healthy aging and long-term preservation of mobility. They should not be represented as a remedy for arthritis or severe cartilage damage but rather as part of a comprehensive system that enhances the internal context for repair and regeneration.
Figure 1: Conceptual Framework of Cellular Support and Anti-Aging Stem Cell Nutrition.
Therapeutic Strategies to Improve Joint Mobility in Regeneration
The treatment of Joint Mobility Therapy may include a combination of medically supervised activities aimed at improving movement patterns, reducing stiffnes and maximizing functional ability. This could be cellular support strategies, modified training paradigms in rehabilitation, anti-inflammatory lifestyle and nutritional planning, as well as careful monitoring for optimal joint function.
The main concept is the combination of joint movement from different perspectives. An integrative program might assess for inflammation, tissue quality, muscle strength, flexibility, biomechanics; metabolic health; and recovery capacity instead of focusing only on pain suppression. This model is particularly applicable to joint discomfort in chronic conditions, however also for those with early degenerative changes, or some small component of reduced mobilitm associated with ageing.
Cell-based regenerative approaches may also be covered under physician supervised selected conditions. Mesenchymal stem/stromal cells (MSCs), which may exhibit certain immunomodulatory and paracrine signaling effects, have been investigated in this regard as an effector or mediator of inflammation and tissue-repair signaling when bioactive molecules released from these cells are present. Nonetheless, the clinical expectations should be adjusted to reality and every regenerative procedure should always rely on valid medical assessment and safety parameters with monitoring.
Antioxidants and Nutritional Bioactives Role
Oxidative stress is one of the major biological factors related to aging and degeneration of tissues. Reactive oxygen species that accumulate beyond the capability of the body to eliminate them by antioxidant defenses may cause damage to cells, tissue inflammation and impairment in regenerative processes. Oxidative stress, in particular, could affect cartilage cells, synovial tissue, and the surrounding connective structures for joint health.
Nutrition rich in antioxidants may protect the cell from oxidative burden and therefore maintain the defense of key biomolecules such as lipids, proteins and DNA contributing to cellular health, thus supporting cellular resilience. Additionally, natural compounds that promote collagen metabolism, mitochondrial function and inflammatory homeostasis may also help for better musculoskeletal aging.
Accordingly, Anti-Aging Stem Cell Nutrition can be positioned as an adjunct to Enhancing Joint Mobility Therapy. Not to replace clinical treatment but once again affords the opportunity for a supportive biological milieu, beneficial joint function and tissue maintenance with augmentation of sustained mobility.
Toward a Personalized Mobility Program
Although personalized, consumer driven care is an immediate answer to the future of mobility for our knee and hip joints. Advanced clinical programs may utilize varying approaches to care by taking into account our patients’ age, activity level, joint status, imaging results, inflammatory state, metabolic health, nutritional profile and functional objectives rather than opting for a one size fits all methodology.
A tailored Enhancing Joint Mobility Therapy program might incorporate medical evaluation, movement analysis, nutritional support, Select cellular care, and autograph rehabilitation planning. They are systematic about not just taking care of short term comfort, but also cognitive function, biomechanics to keep mobility up and resilience so that changes with age don’t become excessive biological stress.
Conclusion
Symptom control is the foundation for treating degenerative musculoskeletal conditions; however, this approach overlooks other aspects. With ongoing research and acceptance of the dynamic nature of medicine, more focus is being put upon factors such as cellular environment, inflammatory balance, oxidative stress and tissue-support mechanisms that affect long-term joint health.
Anti-Aging Stem Cell Nutrition and Improving Joint Flexibility Therapy are elements of integrative direction in modern regenerative medicine. If used appropriately, they can provide for cellular stress, joint function and healthy aging. These modalities should not be characterized as fail-proof treatments but may comprise a medically supervised approach for persons looking to enhance mobility, optimize tissue support and take a more proactive role in musculoskeletal health.