Why this topic is getting so much attention
If someone searches best stem cell clinic and how can stem cells cure diabetes, they are usually not looking for theory. They are looking for something bigger than better glucose control. They are looking for the possibility that insulin dependence, dangerous lows, and constant monitoring might one day be reduced by rebuilding the missing biology itself. That hope is not irrational. Some of the most significant news on diabetes cure have come over two years from stem-cell-derived islet research in type 1 diabetes, with early human studies reporting native insulin production and major decrease external insulins load. However, that news too must be read with caution: Early promising results don t automatically translate into a regular cure fit for the clinic.
How can stem cells cure diabetes, in theory?
The real target is not “sugar,” but the beta cell
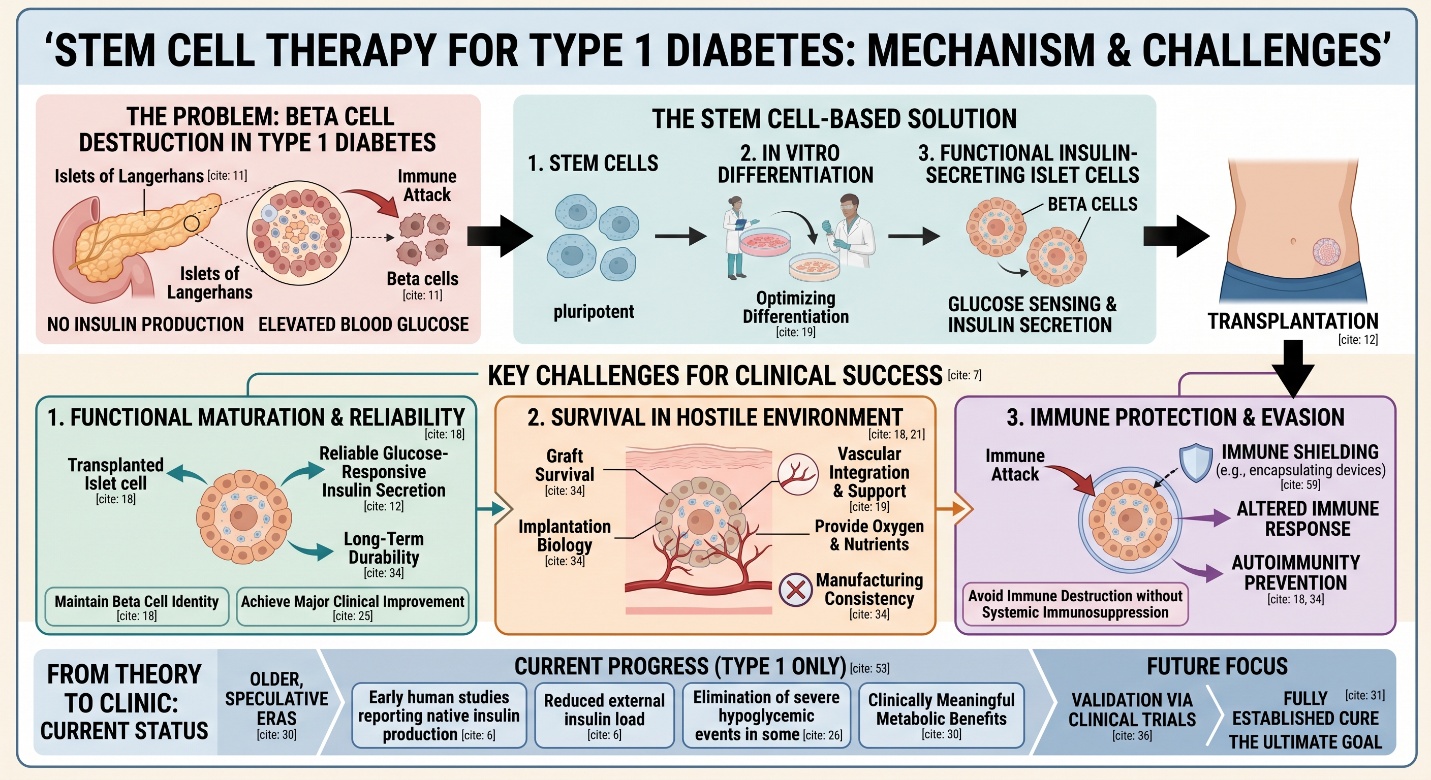
Word-wise, how to cure diabetes with stem cells looks facile — but the science behind that wording is too narrow. Type 1 diabetes is developed because beta-cell destruction (the cells that produce insulin from the pancreas). You have stem-cell-type interventions, which solve that problem by making new insulin-secreting islet cells in vitro and injecting them into the body where they recognize glucose and secrete insulin more physiologically. That is a big reason why some of current excitement focuses on stem cell-derived action—rather than fuzzy “regeneration” language. NIDDK continues to promote islet transplantation as valid route of diabetes therapy, especially in selected people with type 1 diabetes.
The real challenge is not only making cells, but keeping them alive and protected
This is where the story becomes more interesting, and more honest. Scientists have known for years that stem cells could potentially become insulin-producing cells. The harder part has been making those cells function reliably after transplantation, survive in the body, and avoid immune destruction. A 2024 Nature review on the “odyssey” toward a stem cell cure for type 1 diabetes explains that major recent progress has come from optimizing differentiation, survival, and function of transplanted stem-cell-derived tissue, including devices and approaches that support vascular integration. In other words, the field is not only about creating beta cells. It is about making a living graft work in a hostile biologic environment.
What the latest diabetes cure news is actually showing
The biggest recent news is in type 1 diabetes
The strongest recent diabetes cure news has come from type 1 diabetes, not type 2 diabetes. In a 2025 New England Journal of Medicine paper on zimislecel, an allogeneic stem-cell-derived islet-cell therapy, participants with type 1 diabetes and impaired awareness of hypoglycemia showed endogenous insulin production and major clinical improvement after a single infusion. The American Diabetes Association summarized the same findings by noting that all 12 participants in the full-dose group had restoration of endogenous insulin secretion, severe hypoglycemic events were eliminated, insulin use fell in all participants, and 10 of 12 no longer required external insulin at one year. Those are extremely important results. But they still come from an early-phase study in a highly selected patient group.
Encapsulated and alternative stem-cell strategies are also moving forward
The zimislecel story is not the only one. A 2024 Nature Biotechnology paper reported that encapsulated stem-cell-derived beta cells exerted glucose control in patients with type 1 diabetes, showing measurable beta-cell function, improved continuous glucose monitoring outcomes, and reduced insulin dosing in the higher-dose study group. Nature’s 2024 review of the field described these as clinically meaningful metabolic benefits, which is one reason the current moment feels very different from older, more speculative eras of stem cell diabetes research. Still, “clinically meaningful” is not the same phrase as “fully established cure.”
Why this still is not a blanket cure announcement
This is probably the most important paragraph in the whole article. Even the strongest current studies are still dealing with issues such as immune protection, graft survival, implantation biology, manufacturing consistency, and long-term durability. The NEJM study itself was interim phase 1–2 data, not a final universal answer. ClinicalTrials.gov also lists ongoing studies of VX-880/zimislecel in defined type 1 diabetes populations, which is exactly what you would expect in a field that is promising but still being validated. So yes, the current diabetes cure news is real. But no, it does not mean every clinic offering stem cells for diabetes is operating at the level of these trials.
What “best stem cell clinic” should really mean
It should mean regulated, trial-aware, and clinically specific
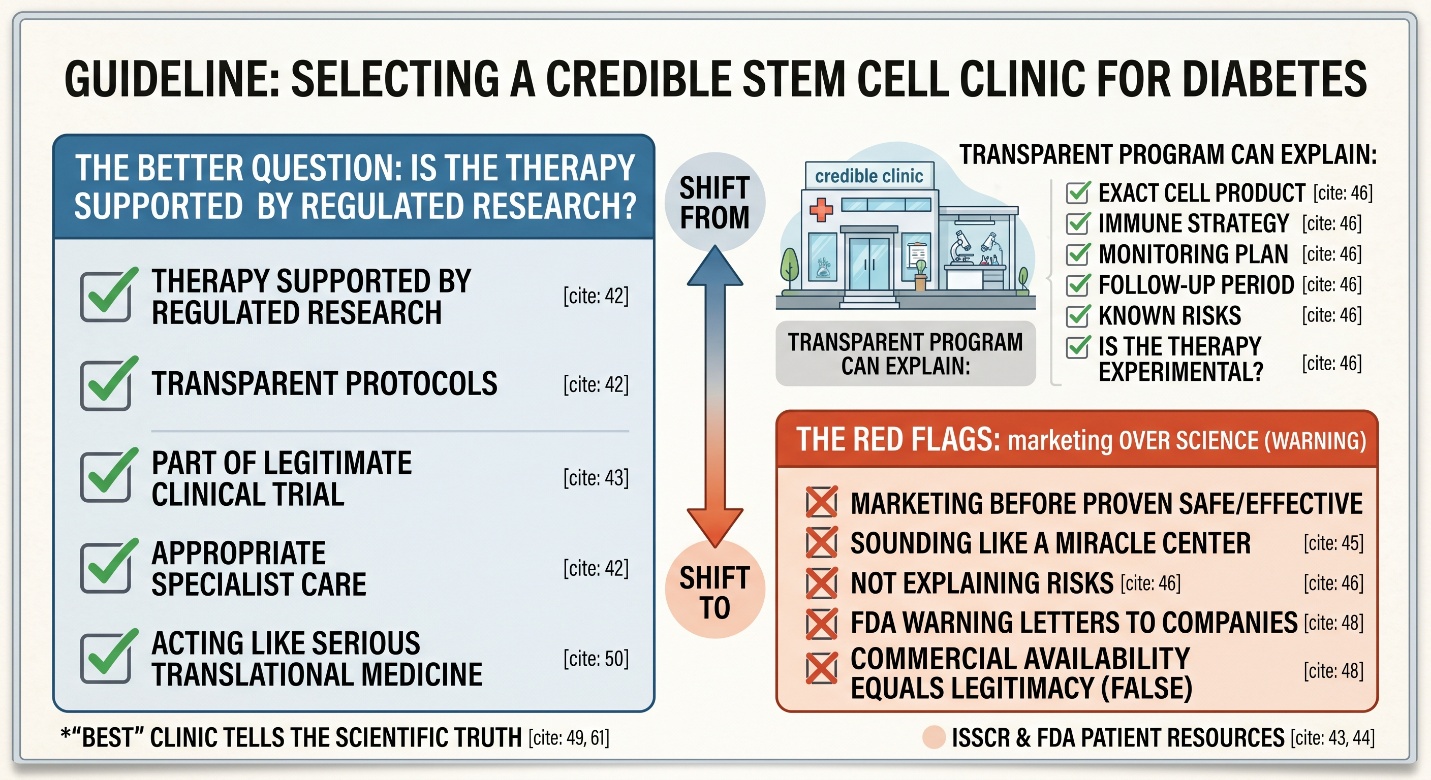
The phrase best stem cell clinic is emotionally understandable, but scientifically it is the wrong first question. The better question is whether the clinic is using a therapy that is actually supported by regulated research, transparent protocols, and appropriate specialist care. ISSCR’s patient resources stress the importance of understanding what kind of stem cell therapy is being offered, whether it is part of a legitimate clinical trial, and what evidence actually supports it. FDA makes the same point more sharply, warning consumers that many regenerative medicine products are marketed before they are shown to be safe or effective.
A credible clinic should sound more like a transplant program than a miracle center
This is where language becomes a practical clue. A credible program for diabetes stem cell therapy should be able to explain the exact cell product, the immune strategy, the monitoring plan, the follow-up period, the known risks, and whether the therapy is experimental. It should also sound narrower and more careful than its marketing department wants it to sound. FDA warning letters to companies marketing stem-cell products for diabetes and other serious diseases are a reminder that commercial availability does not equal legitimacy. In a field as sensitive as diabetes, the “best” clinic is not the one promising the biggest transformation. It is the one acting most like serious translational medicine.
The part people miss: this is mostly a type 1 diabetes story right now
Most “cure” headlines do not apply equally to all diabetes
This is another layer people deserve to hear clearly. The most impressive stem-cell diabetes advances right now are mainly in type 1 diabetes, where replacing or restoring insulin-producing cells makes direct biologic sense. That is not the same as saying stem cells have already “cured diabetes” in the broad everyday way the phrase is often used. Type 2 diabetes includes insulin resistance, metabolic stress, and progressive beta-cell dysfunction, which makes the therapeutic problem more diffuse. So when people read how can stem cells cure diabetes, the honest answer is: current headline-level progress is mostly about stem-cell-derived islet replacement in selected type 1 diabetes patients.
The most honest conclusion
More saleable than the nothing but direct truth As I write this, the hottest diabetes cure news is that those stem-cell-derived islets have shown humans real signs of interior insulin secretion — and even in some cases, at least temporary independence from injected insulin! That is a big moment for medicine. But this early, still confined to specialized type 1 diabetes programs limited in scope and satiated with questions about longevity of effects, immune shielding, access and long-term benefits. Which brings us to the following: So if you ask what is the best stem cell clinic, then it probably is not a branded name. This: that the best clinic is the one willing to tell you if what it provides lines up with evidence at a scientific level or not.