Human growth involves complex genetic and endocrine signaling that dictates the eventual stature of a child. Delays in growth is sometimes what makes psychical and social problems. True failure occurs due to hormonal deficiency or ability of growth plate to resist dhestr. When children fail to keep pace, it affects their self-worth. However, limitations of hormonal interventions are emerging over time with non-responders particularly in the domain of biology. This directs researchers towards Regeneartive Medicine to reboot growth process. Introduction of UC-MSCs represents a paradigm shift with its effect on targeting skeletal foundation towards Height Enhancement in Children. This presents a comprehensive treatment both by regulating the growth plate cell environment and not just giving hormones.
Understanging the Mechanisms of Growth in Height and Bone
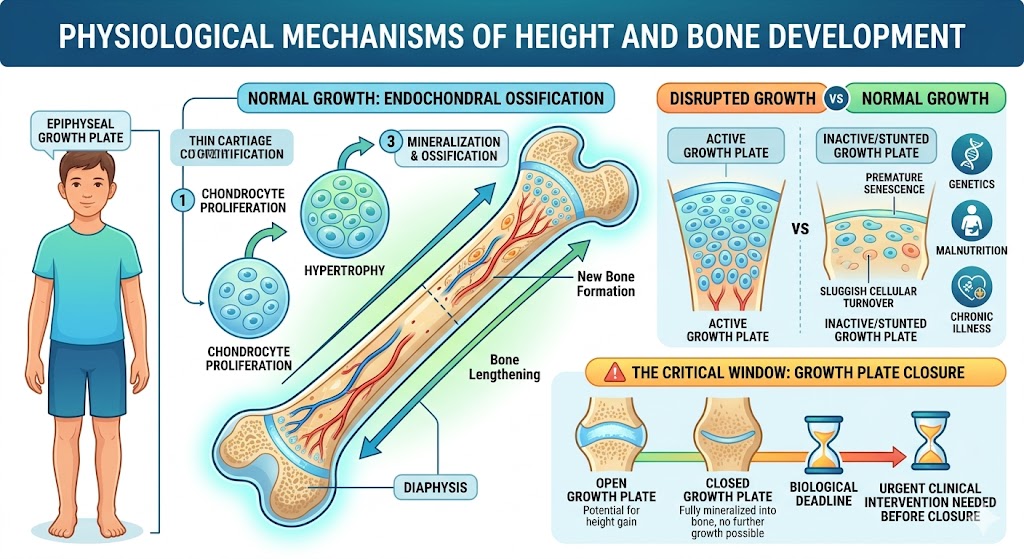
Height Enhancement in Children is closely associated with a specific physiological mechanism based on the epiphyseal growth plate, which is a thin layer of hyaline cartilage located at the ends of long bones. This region of cartilage often undergoes accelerated senescence or loss of chondrocyte proliferation in children with growth retardation. Growth usually occurs through endochondral ossification, in which chondrocytes proliferate, undergo hypertrophy and being mineralized to bone. However, when this mechanism is impaired by genetics, malnutrition or a chronic illness the growth plate becomes prematurely thin and stature is therefore stunted. The clinical manifestations of this condition are largely physical, including short extremities and a low height-for-age percentile, but the underlying biological reality is cellular dolente or diminished cellular turnover. When the growth plates are attempted to be closed forever, if the child reaches its genetic potential. Once the cartilage is completely supplanted by bone, no amount of hormonal or cellular stimulation can reactivate the lengthening process; hence this biological deadline focuses us on clinical intervention.
2.Traditional Treatment Approaches and Limitations
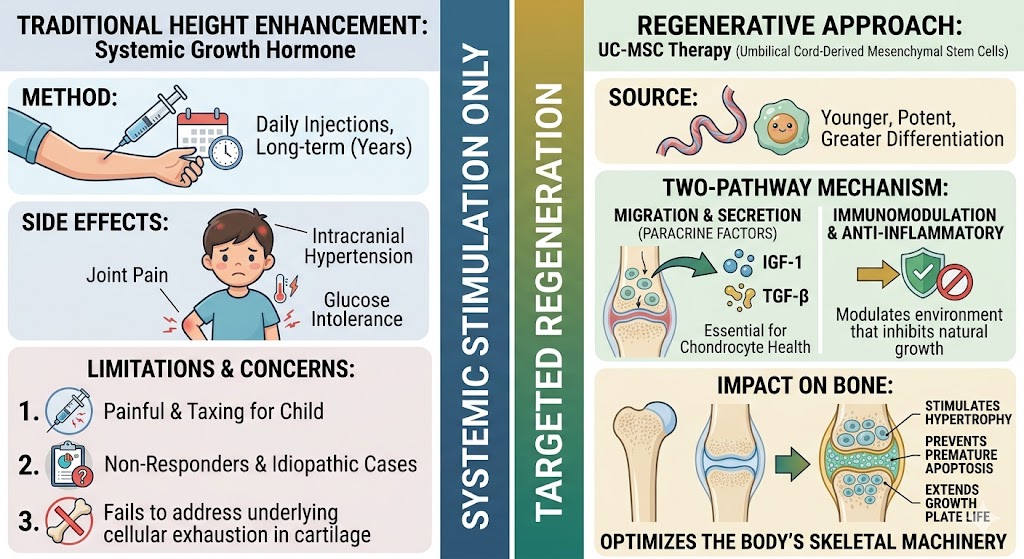
Current medical Height Enhancement in Children protocols for treating short stature primarily rely on daily injections of recombinant human growth hormone. While effective for many, this traditional route is not without significant hurdles. For one, the treatment requires years of consistent, often painful, daily administration, which can be taxing for a young child. Furthermore, there is a subset of the population known as non-responders who possess a resistance to these hormones or suffer from idiopathic short stature where standard hormone therapy provides only marginal gains. The side effects can also be a deterrent, ranging from glucose intolerance and joint pain to more rare but serious intracranial hypertension. These limitations underscore a critical gap in pediatric endocrinology, which is the need for a therapy that acts directly on the regenerative capacity of the bone tissue itself. Traditional methods focus on systemic stimulation, but they often fail to address the underlying cellular exhaustion within the cartilage of the long bones, which is why the medical community is pivoting toward regenerative alternatives.
3.The Role of UC-MSCs in Height Enhancement in Children
The transition toward UC-MSCs as a primary tool for Height Enhancement in Children is driven by the unique immunomodulatory and proliferative properties of these cells. Umbilical cord-derived mesenchymal stem cells are younger and more potent than those derived from adult bone marrow, possessing a higher rate of doubling and a greater capacity for differentiation. In the context of skeletal growth, these cells function through two primary pathways. First, they can migrate to the site of the growth plate and secrete a rich cocktail of paracrine factors, including Insulin-like Growth Factor-1 and Transforming Growth Factor-β, which are essential for chondrocyte health. Second, they help modulate the inflammatory environment that might be inhibiting natural growth. By stimulating the chondrocytes to undergo hypertrophy and preventing premature apoptosis, UC-MSCs effectively extend the active life of the growth plate. This application of Regenerative Medicine ensures that the body’s own skeletal machinery is optimized, providing a regenerative boost that systemic hormones alone cannot achieve. The integration of UC-MSCs into treatment protocols offers a targeted approach that respects the natural physiology of the child while pushing the boundaries of biological potential.
4.Future Trends and the Significance of Treatment in Thailand
Thailand has rapidly emerged as a global epicenter for advanced cellular therapies, making it a premier destination for families seeking Height Enhancement in Children. The nation’s medical infrastructure combines world-class laboratory standards with a regulatory environment that encourages the ethical application of Regenerative Medicine. In the coming years, the trend in Thailand is moving toward personalized cellular dosing, where UC-MSCs are tailored to the specific epigenetic profile of the patient. The reason Thailand stands out is the seamless integration of specialized pediatric clinics with high-tech biotechnology hubs, allowing for the fresh cultivation and immediate application of stem cells. As the global medical community looks for validated, safe, and effective alternatives to lifelong hormonal therapy, Thailand’s clinical trials and successful case studies in MSC applications provide a roadmap for the future. The country’s commitment to medical innovation ensures that it remains at the forefront of treating complex growth issues, offering hope through science that was once considered futuristic.
In summary, the pursuit of physical growth and skeletal health is being redefined by the intersection of pediatric care and cellular science. While the traditional challenges of short stature remain a significant concern for many, the arrival of Regenerative Medicine offers a sophisticated path forward. By leveraging the potent regenerative capabilities of UC-MSCs, clinicians can now address height-related issues at the cellular level, focusing on the health and longevity of the epiphyseal growth plates. This shift from simple hormone replacement to complex cellular modulation marks a new chapter in how we approach Height Enhancement in Children. With Thailand leading the charge in clinical excellence and accessibility, the future of pediatric growth therapy looks increasingly promising. The synergy of specialized expertise, ethical research, and advanced biotechnology ensures that children have the best possible chance to reach their full physical potential through safe and innovative biological interventions.

