Advanced Regenerative Healing through UC-MSCs for Back Pain in Thailand
Chronic spinal discomfort has transitioned from a localized orthopedic concern to a global socioeconomic crisis. Among the various triggers, Degenerative Disc Disease (DDD) stands as the primary culprit behind persistent Back Pain, affecting millions of individuals by stripping away their mobility and psychological well-being. DDD is more than just a sign of aging, it is a complex pathological breakdown of the spine’s structural and biochemical harmony. UC-MSCs Therapy offers a breakthrough by addressing these root causes at a cellular level.
1.The Pathophysiology of Spinal Degeneration
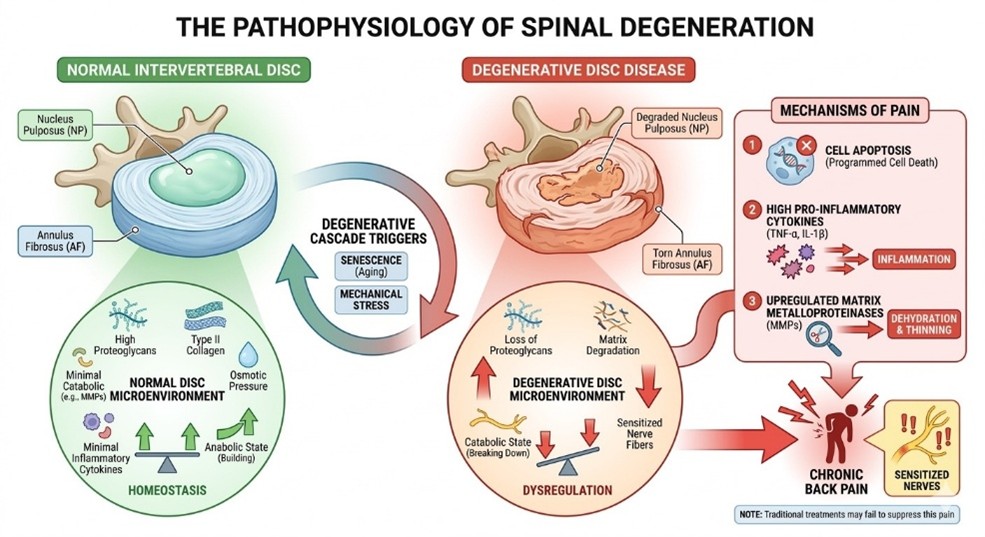
To understand why the spine fails in Back Pain, one must examine the microenvironment of the intervertebral disc. The disc is composed of a gelatinous core called the nucleus pulposus (NP), surrounded by a fibrous ring known as the annulus fibrosus (AF). Under normal conditions, the NP is rich in proteoglycans and type II collagen, which maintain osmotic pressure and provide cushioning.
The onset of Back Pain usually involves the breakdown of this matrix. As senescence or mechanical stress takes hold, the cells within the NP begin to undergo apoptosis (programmed cell death). This loss of cellularity results in a shift from an anabolic (building) state to a catabolic (breaking down) state. High levels of pro-inflammatory cytokines, specifically Tumor Necrosis Factor-alpha (TNF-α) and Interleukin-1 beta (IL-1β), are released into the disc space. These molecules accelerate the degradation of the extracellular matrix by upregulating enzymes like matrix metalloproteinases (MMPs). As the disc dehydrates and thins, the nerve fibers in the outer layers of the AF are sensitized, leading to the debilitating sensation of chronic pain that traditional medicine often struggles to suppress.
2.Limitations of Current Therapeutic Modalities
Historically, the management of Back Pain has followed a linear path starting with conservative treatments such as physical therapy, non-steroidal anti-inflammatory drugs (NSAIDs), and epidural steroid injections. While these methods provide temporary symptomatic relief, they fail to address the underlying cellular depletion. They are essentially band-aiding solutions that mask pain while the disc continues to deteriorate.
When conservative measures fail, surgical intervention—such as spinal fusion or discectomy—is often recommended. However, surgery is invasive and carries substantial risks, including adjacent segment disease, where the vertebrae above and below the fused site undergo accelerated wear due to altered biomechanics. Furthermore, surgery does not restore the natural biological function of the disc. This therapeutic gap has created an urgent demand for a biological solution that can stop or reverse the degenerative cascade rather than just managing the wreckage.
3.The Regenerative Potential of UC-MSCs
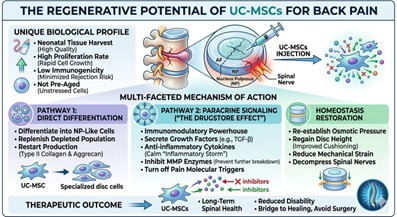
Umbilical Cord-Derived Mesenchymal Stem Cells (UC-MSCs) have emerged as a superior candidate for treating Back Pain due to their unique biological profile. Unlike bone marrow-derived cells, UC-MSCs are harvested from neonatal tissue, meaning they possess higher proliferative rates, lower immunogenicity, and haven’t been pre-aged by the patient’s own environmental stressors. The therapeutic mechanism of UC-MSCs is multifaceted. Once injected into the degenerative disc, these cells perform through two pathways and one restoration for Back Pain Therapy
- Direct Differentiation: UC-MSCs can differentiate into NP-like cells, directly replenishing
the depleted cell population and restarting the production of type II collagen and aggrecan.
- The Drugstore Effect (Paracrine Signaling): Perhaps more importantly, UC-MSCs will
secrete a cocktail of growth factors (such as TGF-β) and anti-inflammatory cytokines that re-engineer the disc’s microenvironment. These secretions inhibit the destructive MMP enzymes and reduced the inflammation, effectively turning off the molecular triggers of Back Pain.
- Homeostasis Restoration: By re-establishing the osmotic pressure within the NP, UC-
MSCs help the disc regain its height and shock-absorbing capabilities, which reduces the mechanical strain on the surrounding spinal nerves.
4.Why Thailand is the Future of UC-MSCs Stem Cell Therapy for Back Pain
The adoption of UC-MSCs for spinal health for Back Pain is gaining significant momentum in Thailand, positioning the country as a primary hub for regenerative excellence. Thailand has invested heavily in medical biotechnology, ensuring that local laboratories meet international Grade A Cleanroom standard. This infrastructure allows for the high-purity cultivation of UC-MSCs that are essential for safe clinical application.
The reason Thailand stands out is the synergy between advanced medical expertise and a favorable regulatory environment. The Thai Food and Drug Administration has been proactive in establishing frameworks for cell-based therapies, allowing patients to access cutting-edge treatments that might still be tied up in the bureaucratic red tape of Western nations. Furthermore, the integration of regenerative medicine into Thailand’s world-renowned medical tourism sector means that patients receive holistic care—combining advanced UC-MSCs injections with specialized rehabilitation—at a fraction of the cost found in Europe or North America. The concentration of highly skilled specialists in Bangkok and other major hubs ensures that the precision required for intradiscal delivery of UC-MSCs is met with the highest surgical standards.
In summary, spinal therapy is moving away from traditional surgical correction and embracing a regenerative healing approach. Chronic Back Pain no longer has to be an inevitable sentence of disability. By leveraging the potent regenerative capabilities of UC-MSCs, clinicians can now target the molecular roots of disc decay. This transition toward cellular therapy offers a bridge between ineffective medications and high-risk surgeries. As Thailand continues to refine these protocols and lead in the application of mesenchymal cell research, the prospect of long-term spinal health becomes a reachable reality for patients worldwide. The fusion of biological science and precision medicine ensures that the future of spinal therapy is not just about living longer, but living without the burden of pain.

