What is Stem Cell Therapy Thailand has ever discussed medical therapy for complex neurological patients like Amyotrophy Lateral Sclerosis; ALS is a type of disease that progressively affects the nerve cells (neurons) in the brain and spinal cord. Over time, as these motor neurons slowly deteriorate, patients may find themselves with weakness and wasting of the muscles, stiffness in limbs and body trunks/regions, difficulty speaking (dysarthria), swallowing problems leading to aspiration or choking sensations, fatigue that is constant with little periods of recovery if not rare breaks from it in the course of their life as they knew it and respiratory function that will decline.
Due to the multiple biological pathways involved in ALS (including neuroinflammation, oxidative stress, mitochondrial dysfunction, immune imbalance and progressive motor neuron injury) enabled many patients to explore integrative regenerative programs. At this site, UC-MSCs and DFPP treatment may also be included as part of a medically managed supportive setting.
Let me put that plainly: stem cell therapy for ALS is not a proven cure, and does not replace conventional neurological care. Regenerative medicine products such as stem cells and exosomes are not approved by the FDA to treat diseases of the nervous system such as ALS. Still, it is worth noting that MSC-based strategies still have to be investigated for their potential trophic, immunomodulatory and neuroprotective effects.
ALS and the application of supportive regenerative care
ALS is more than a muscle weakness disease. Progressive neurological disorder involving degeneration of the motor neuron network. In the disease environment there are activated immune cells, inflammatory mediators that result in oxidative injury, impaired cellular repair and less supportive work by surrounding glial cells.
This is why stem cell therapy Thailand for ALS tends to be considered as a supportive biological approach rather than the goal of replacing the diseased cell. Rather to help support the environment around remaining motor neurons rather than immediately creating new ones.
In many patients the practical goals in these areas when applied with standard ALS therapies, rehabilitation, respiratory support and nutritional management are to promote functional stability, decrease excessive pro-inflammatory signaling, and improve overall biological resilience.
How DFPP Treatment Can Be Beneficial Prior to Stem Cell Therapy
DFPP is a blood purification technique aimed at plasma filtration with the aim of reducing directed circulating elements. DFPP has been studied in clinical applications to remove pathogenic molecules of different origins, including immunoglobulins, immune complexes and inflammatory mediators as well as other high-molecular-weight plasma components. Recent reviews characterize DFPP as a therapeutic plasma-separation technique for a variety of immune-mediated or neuroimmune diseases.
Are ALS Patients Altered for Repeat DFPP? DFPP should not be portrayed to ALS patients as a direct treatment to their motor neuron disease. DFPP may help ameliorate systemic inflammatory burden and improve internal biological environment prior to UC-MSCs administration, hence can be a viable supportive therapy in suitable candidates.
In the context of a regenerative medicine program, DFPP could be performed as part of pre-conditioning. While the aim is to prepare the body by decreasing circulating inflammatory elements, immune complexes, oxidative burden and plasma-associated stressors that may confound cellular signalling. That is, DFPP can be easily adapted to construct a cleaner and more balanced systemic microenvironment prior to UC-MSC infusion.
This is why the combination of DFPP and stem cell therapy for ALS typically occurs in more integrative clinics: while DFPP facilitates systemic purification, UC-MSCs facilitate modulatory and paracrine regenerative signaling.
How UC-MSCs May Work in ALS
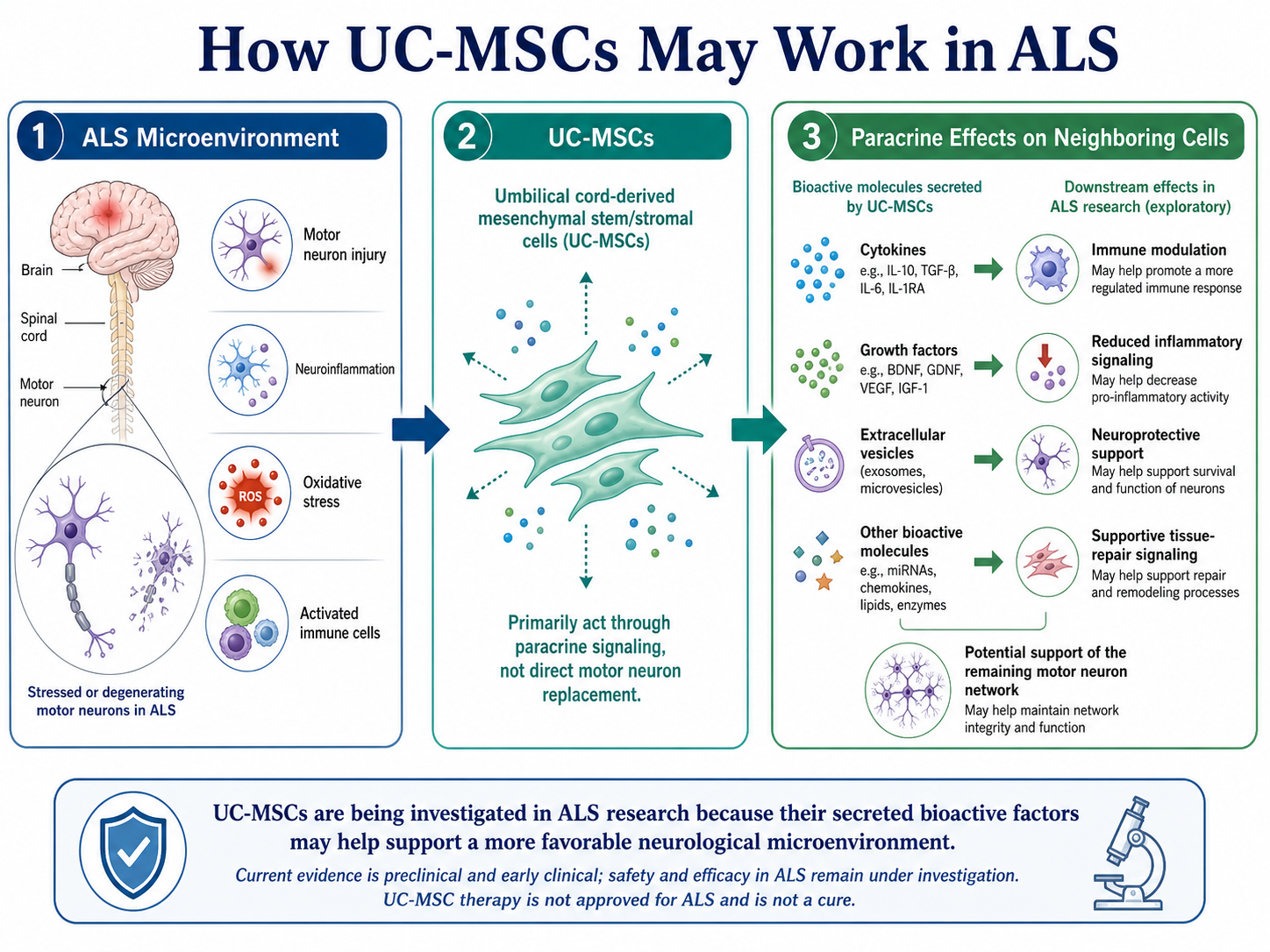
In particular, UC-MSCs (umbilical cord-derived mesenchymal stem/stromal cells) seem to have a unique advantage relative to other MSC types due their capacity to communicate with damaged tissues through paracrine signaling. Right away, they are not expected to replace dying motor neurons. Instead, they secrete cytokines, growth factors, extracellular vesicles and other bioactive molecules that exert an effect on neighboring cells.
Figure 1: Schematic overview of the proposed role of UC-MSCs in ALS research, highlighting paracrine secretion of bioactive factors, modulation of inflammatory activity, neuroprotective signaling, and potential support of the remaining motor neuron network.
Neuroinflammatory Modulation
Chronic autoimmune inflammatory activity with neuromuscular involvement, is a hallmark of ALS. The interaction between UC-MSCs and immune cells may regulate inflammatory responses by reducing overactive cytokine signaling.
Neurotrophic Support
UC-MSCs might secrete factors that stimulate survival pathways for neurons. Those signals could protect the remaining lower motor neurons from this continuous cellular stress.
Oxidative Stress Regulation
Motor neuron injury is exacerbated by oxidative stress. Factors secreted from the MSC lineage may aid in providing antioxidant protection to mitigate cellular damage within the neurological microenvironment.
Immune System Balance
UC-MSCs may affect T cells as well as macrophages, microglia and other immune cells. Itcould draw the body down from an over-activated inflammatory state and transitions it toward a more balanced, regulated, immune environment.
Microenvironment Support
A wide spread goal of UC-MSC therapy in ALS research is to promote a healthy surrounding tissue environment for optimal functioning of the remaining motorneurons. MSCs are studied for trophic support and immunomodulation, tissue repair signaling.
Potential Benefits for ALS Patients
Naturally, the benefits of enough stem cell therapy Thailand with DFPP ought to be introduced in a cautious style. It does not seek a promise at reversing ALS, but to ameliorate the biology of the patient and enhance quality-of-life.
Possible benefits may include:
Support for systemic inflammatory balance
Decreased levels of specific circulating inflammatory or immune-related factors by DFPP
Help maintain a better environment pre UC-MSC infusion
Neuroprotective and trophic signalling of UC-MSCs
Resulting in delaying functional deterioration only in few selected patients
Improved fatigue, stiffness, comfortor overall resilience in a few instances
Enhanced tracking in conjunction with rehabilitation and neurological care
Patients should expect that not all will get a full recovery, but rather supportive improvement or slowed decline.
How long before you see changes?
Response time varies between patients. The disease course of ALS is highly individual, and objective follow up over time are needed.
Hydration, blood pressure status, fatigue, dizziness and tolerance over the first 24–72 h of DFPP are all assessed. After UC-MSC administration, regular monitoring is done for fever, headache, fatigue or discomfort at the injection site (when administered systemically) or neurological evaluation (if injected into the CNS).
In the first 1–4 weeks, patients may report improved energy, sleep, stiffness or well-being. Nevertheless, these early changes are not evidence of disease modification.
Although all assessments should be matched to the interval between assessment points, periods of 1–3 months are usually the most meaningful for tracking trends in strength, swallowing, speech and walking, fatigue and daily activity. Usually the primary assessment duration is three to six months, with evaluation parameters such as ALSFRS-R score, respiratory function, muscle strength, swallowing ability and speech or quality-of-life.
It is significant to note that while longer follow-up over 6–12 months would inform whether the decline of the patient appears slower compared to baseline trajectory.
Conclusion
The DFPP for stem cell therapy Thailand honors the integrative regenerative medicine paradigm that aids in nurturing the patient´s endogenous microenvironment. DFPP is associated with selected inflammatory and immune-related plasma components that may serve as a supporting pre-treatment. Thereafter, UC-MSCs might exert paracrine, immunomodulatory, neurotrophic and microenviron-mental-stromal effects.
This combination has to be presented responsibly. It is not a cure for ALS and must not substitute standard, neurologist-directed care. The best positioning appears to be for DFPP treatment may preconditioning the body, and that UC-MSCs potentially supporting the neurological microenvironment. Each alone may provide selected ALS patients a supportive and protective trajectory toward inflammatory balance, functional stability, and quality-of-life support.