Thailand Stem Cell Consultants has started getting more popular among individuals searching for additional support in case of complex chronic neurological disease like Amyotrophic Lateral Sclerosis or ALS. ALS is a progressive neuromuscular disease affecting the motor neurons — the nerve cells controlling voluntary muscle movement. This is the time when these motor neurons slowly start to degenerate and cause weakness, stiffness, muscle contraction impairment by affecting walking, changes in speech, issues with swallowing, fatigue as well as weakened lungs.
ALS is still a difficult disease in modern neurology as of today. Regular medical treatment aims to slow the progress of illness, maintain breathing and nutritional intake, and restore mobility and quality of life for as long as feasible. In this regard, ALS stem cell treatment is under research as a supportive and investigational regenerative strategy. We cannot call this a cure, it could support the biological environment around damaged motor neurons.
Regenerative medicine programs utilizing UC-MSCs (umbilical cord-derived mesenchymal stem/stromal cells) are growing in popularity in Thailand as they promote immunomodulatory, anti-inflammatory and neuroprotective capabilities.
What you need to know about ALS and the degeneration of motor neurons
ALS involves upper and lower motor disease. They are critical for relaying messages from the brain and spinal cord to muscles everywhere in the body. Damaged motor neurons send fewer signals to muscle, and gradually muscles become weaker, smaller, crampy, stiff and lose function.
The course of ALS is not straightforward. There is no one biological pathway that causes it! Conversely, there are multiple mechanisms involved in the injury of motor neurons such as neuroinflammation; oxidative stress; mitochondrial dysfunction; glutamate toxicity; abnormal protein accumulation; compromised cellular repair and impairment of communication between neuron-sustaining microglia.
And this complexity is part of the reason that ALS is so challenging to treat. One possible target is that one medication may focus on a certain pathway, but the disease itself has so many different biological processes that overlap. This is why scientists are exploring whether regenerative approaches like stem cell therapy Thailand could help create a more favorable environment for the nervous system.
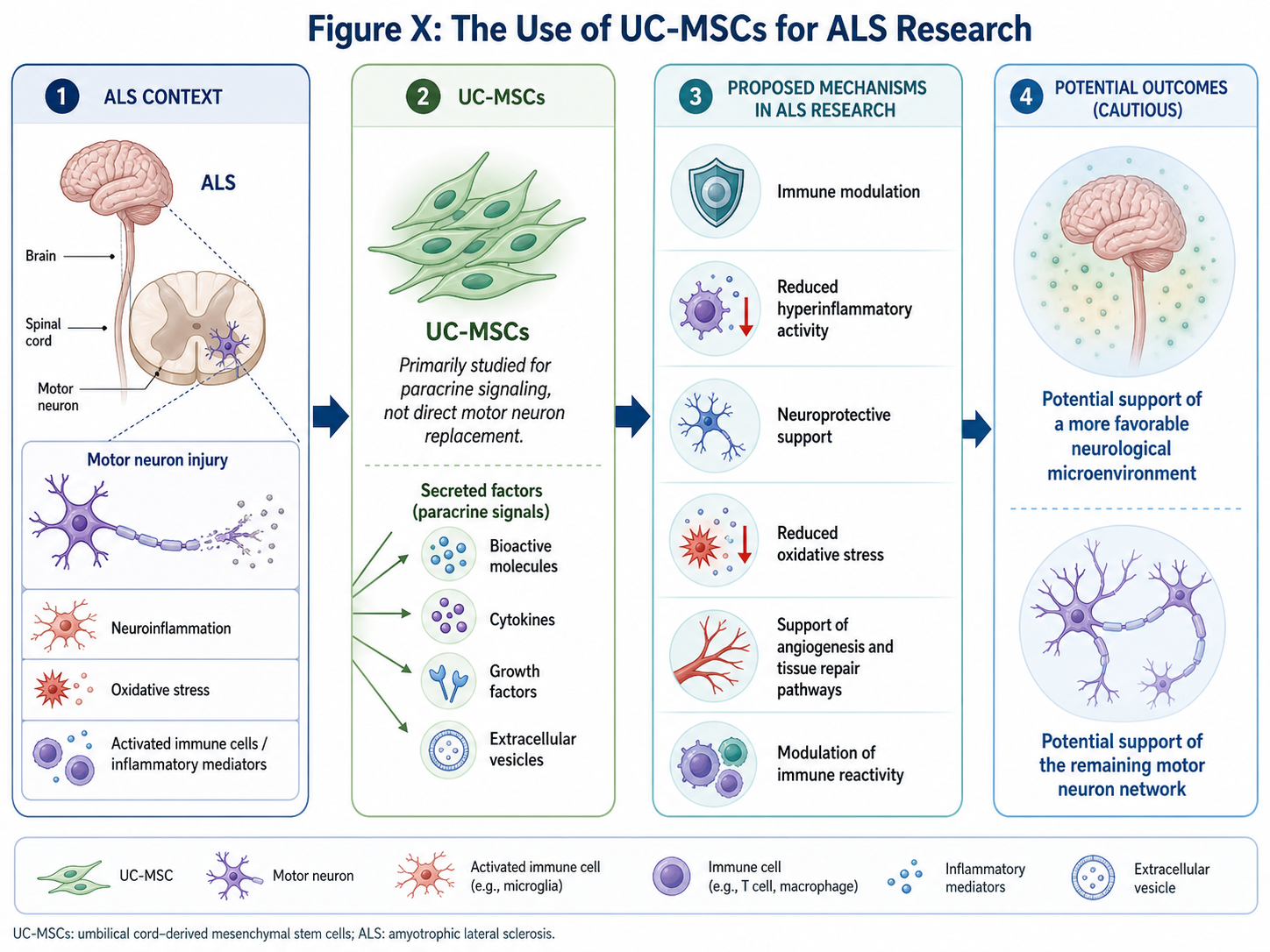
The Use of UC-MSCs for ALS Research
UC-MSCs are not typically used to replace dead motor neurons. They are mostly useful for paracrine signaling, according to current theories of regeneration medicine. These properties infer that UC-MSCs can secreting bioactive substances, cytokines, growth factor as well as extracellular vesicles acting on the local cells and tissues.
The potential utility of UC-MSCs in ALS is linked to their immunomodulatory effects, which are intended to promote a more favorable neurological microenvironment. This could also mean dampening hyperinflammatory activity, protecting residual neurons from stressors of cell health in a neuroprotective capacity, modulating repair pathways involved in angiogenesis and tissue restoration or the modulation of immune reactivity.
In ALS, the nervous system is postulated to be in a continued state of mens stress. Ongoing motor neuron injury may be a result of systematic pathological events, such as activated immune cells and inflammatory mediators, and oxidative injury. UC-MSCs are being studied because they can potentially dampen some of these deleterious biological signals and promote the survival of the remaining motor neuron network.
Figure 1: Proposed Immunomodulatory and Neuroprotective Effects of UC-MSCs in ALS
Stem Cell Therapy for ALS: Proposed Mechanism
Stem cell therapy for ALS is thought to operate though several important mechanistic biological actions.
Neuroinflammatory Modulation
ALS is associated with inflammation in the central nervous system (CNS). UC-MSCs might affect microglia or macrophages, T cells, and inflammatory cytokines to modulate immune responses. This may decrease motor neuron stress due to excessive neuroinflammation.
Neurotrophic Support
UC-MSCs are considered to secrete growth factors and neurotrophic molecules involving pathways promoting neuron survival. Such signalling could protect vulnerable motor neurons and enhance communication between the nerve cells and their local environment.
Oxidative Stress Reduction
Oxidative stress is a major process that has been implicated in the pathogenesis of neurodegenerative disease. Factors derived from UC-MSCs may assist in fortifying the antioxidant defense, decreasing the damage to cells, and enhancing the tolerability of neuronal tissue under stress.
Mitochondrial and Cellular Support
Motor neurons are energetically demanding cells. In ALS, it is thought that mitochondrial dysfunction could play a role in the cellular degeneration. It is possible that UC-MSCs indirectly promotes metabolic homeostasis through paracrine signaling and tissue-supportive modalities.
Systemic Immune Balance
ALS is more than a local neural disease. Disease progression may also be influenced by systemic inflammation and immune imbalance. Per local ease, intravenous UC-MSC infusion may be given to provide general immunomodulatory support systemically; [or] deliver signal guidance closer to the central nervous system via intrathecal delivery.
Potential Benefits for ALS Patients
However, such possibilities of stem cell therapy Thailand for ALS must be prudently and judiciously communicated. This is not about promising to revers ALS but rather what we can do to help maintain function and prevent where possible deterioration.
Possible patient-centered goals may include:
Support for neuroinflammatory balance
Estimated slowing of functional decline in selected patients
Support for health of motor neurons
Motility trait: Making the animal better able to not tire or otherwise a general biological robustness
Improved quality-of-life support in conjunction with rehabilitation
Swallowing, mobility, stiffness or muscle function monitoring
Integration with standard neurological care
For some patients it may be a change in terms of energy or comfort and stiffness, functional stability and for others, they do not have much improvement. ALS is known to have widely variable outcomes based on clinical stage in the disease, progression rate, which tends to be age-associated and where patients are assessed (respiratory status), baseline function and overall health.
How Long Should It Take to Make Results?
Recovery time in stem cell therapy for ALS is months, not days. ALS is, in its majority, a chronic progressive disorder that must be interrogated through objective tracking rather than by evaluating immediate symptom evolution.
In the first few days, safety monitoring is really all that matters. Patients can be monitored for fever, headache, fatigue, discomfort or alterations within the neurological symptoms. In the first few weeks, clinicians may evaluate general tolerance, energy level, sleep and appetite changes, stiffness and daily activities.
The meaningful evaluation time frame is generally between 1 to 3 months where the early functional trends are more easily identifiable. For any specific patient with ALS, the critical follow-up period is generally 3 to 6 months, which allows clinicians to assess a change in the rate of decline pre- and posttreatment. Assessment through 6 to 12 months of follow-up may be used to determine if the treatment was responsible for functional stability or slower progression.
Conclusion
Stem cell therapy Thailand and ALS is an upcoming branch of regenerative medicine. UC-MSCs are being investigated for their ability to maintain a balanced state of neuroinflammation, their capacity to secrete neurotrophic factors, and reduce oxidative stress levels in the environment surrounding affected motor neurons.
But, it should not be sold as a cure for ALS through stem cells. Best expressed in terms of being investigational and supportive, this concept might offer select patients the opportunity to optimize functional stability, slow decline, and better quality-of-life support. The most rigorous model involves a combination of UC-MSCs with standards of care for neurological management, rehabilitation, respiratory support, and objective long-term monitoring in a medically supervised format.