Stem Cell Clinic and Multiple Sclerosis: What the Cost of Stem Cell Therapy for MS Really Means
Why does this topic keep drawing attention
When people search for stem cell clinics and multiple sclerosis, they are usually not looking for abstract science. They are looking for something more hopeful than symptom control and more decisive than another medication switch. That reaction is understandable. multiple sclerosis is a chronic immune-mediated disease of the central nervous system, and for many people, it becomes a long story of relapses, MRI activity, treatment fatigue, and fear about future disability. Stem cell therapy enters that story because it sounds like a reset, not just a delay.
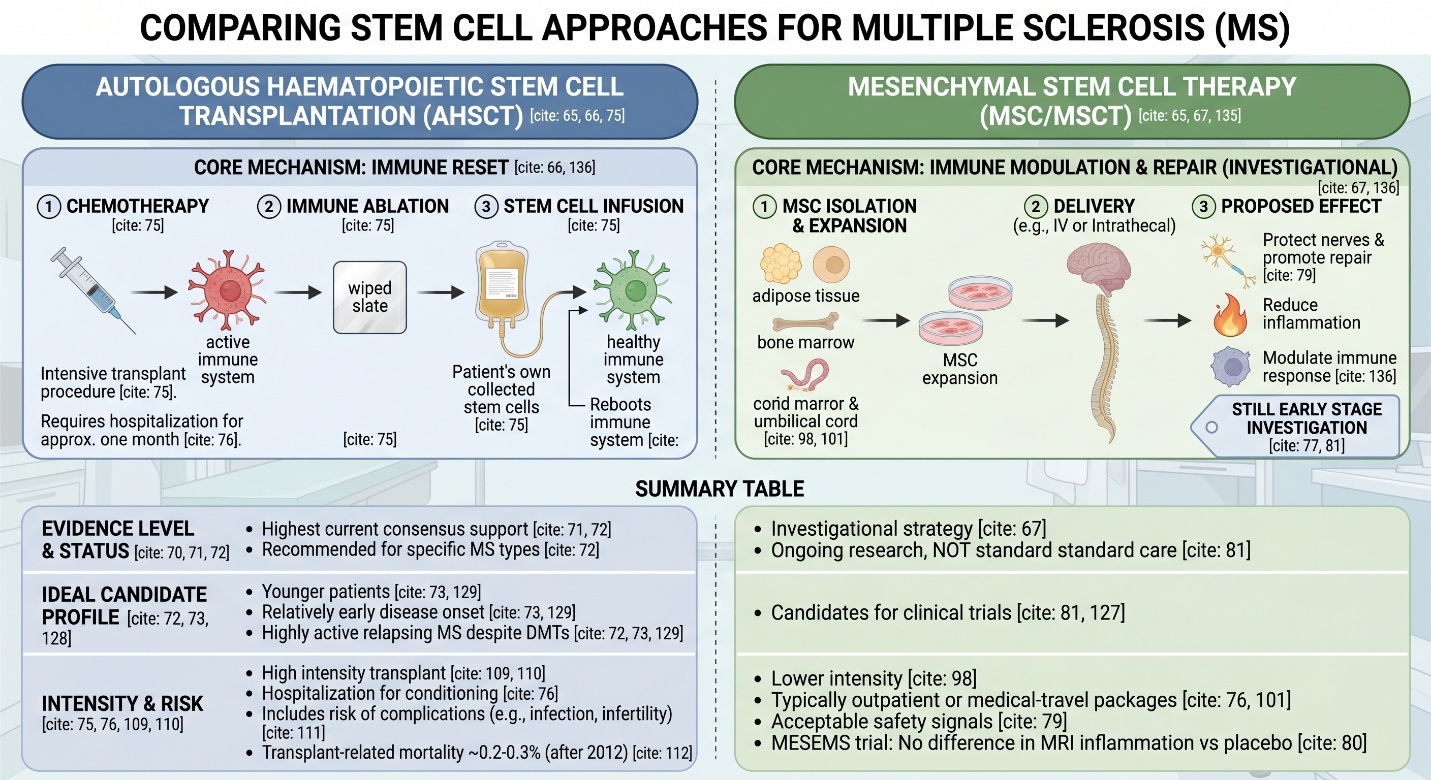
The complication is that “stem cell therapy for multiple sclerosis” is not one single thing. In real medicine, the two big categories are autologous haematopoietic stem cell transplantation (AHSCT) and mesenchymal stem cell therapy (MSC/MSCT), and they are not interchangeable. AHSCT is the more intensive, transplant-based approach aimed at rebooting the immune system. MSC therapy is a separate investigational strategy being studied for immune modulation and repair. Good writing on multiple sclerosis should separate those worlds clearly, because a good stem cell clinic conversation starts with precision, not branding.
What stem cell treatment for multiple sclerosis actually means
AHSCT is the most serious and most evidence-backed form
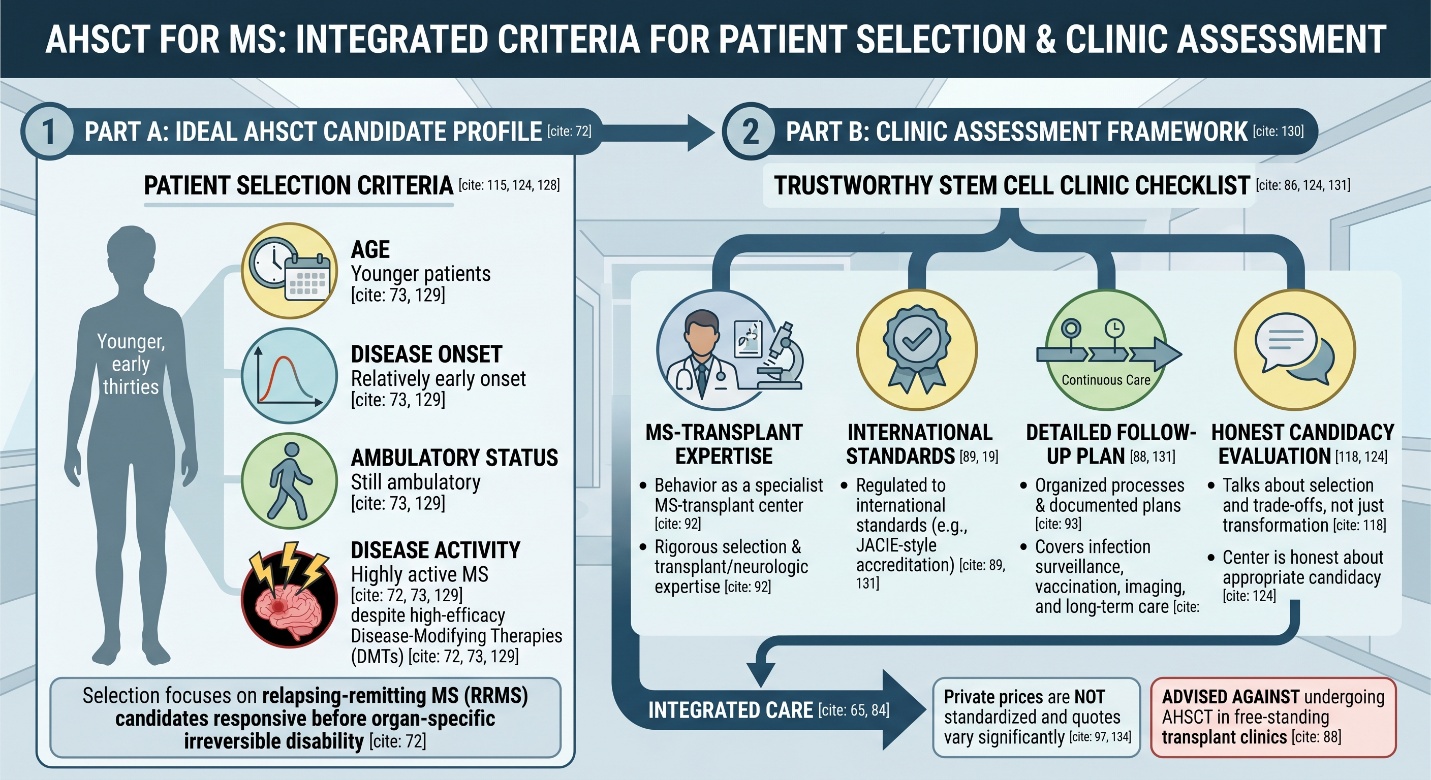
AHSCT shows the highest level of current consensus support, but not every product marketed under the stem cell banner. AHSCT was recommended for certain multiple sclerosis types, particularly among adequate relapsing-remitting multiple sclerosis candidates who had been unresponsive to high-efficacy disease-modifying therapy and prior to organ-specific irreversible disability in a 2025 ECTRIMS/EBMT consensus summary. Cleveland Clinic defines the optimal patients in similar terms; generally younger, still ambulatory with relatively early disease onset, but highly active multiple sclerosis despite use of high-efficacy DMTs.
That matters because many people hear “stem cell clinic” and imagine a broad menu of equivalent options. They are not equivalent. AHSCT is a transplant procedure with chemotherapy, stem cell collection, hospitalization, and close follow-up. It is not a casual add-on. Cleveland Clinic notes that patients are typically hospitalized for about a month for conditioning, transplantation, and initial recovery, which already tells you this is much closer to transplant medicine than to outpatient wellness marketing.
MSC therapy is still much earlier
Although it is scientific in nature, the use of mesenchymal stem cells for therapy is still investigational. MSC therapy is being investigated to protect nerves and promote repair, according to the UK MS Society, which also added that early clinical studies show safety and tolerability with mainly mild side effects. However, that same source states that MSC therapy did not lower MRI inflammation relative to placebo in the MESEMS trial. MS Society and multiple sclerosis Society UK also put it this way: ongoing research, not standard clinical care.
This distinction is probably the most important “layer” in the whole topic. If a clinic says it offers stem cell treatment for multiple sclerosis, the next question should not be “how much?” but “which stem cell approach?” AHSCT and MSC therapy differ in mechanism, evidence level, intensity, risk, and follow-up requirements. A serious clinic should be able to explain that in plain language.
What a trustworthy stem cell clinic should sound like
More transplant centers than miracle centers
The best clue is usually tone. Cleveland Clinic explicitly advises against undergoing AHSCT in free-standing transplant clinics, especially without a detailed follow-up plan for post-transplant medical and neurologic issues. The multiple sclerosis Society UK similarly warns that private centres can have different criteria and safety standards, and recommends checking whether a clinic is regulated to international standards, such as JACIE accreditation, and whether it has real follow-up care in place.
That is a far superior method of looking at the term best stem cell clinic for multiple sclerosis. The very finest center is not always one with the newest pledge. It behaves like a specialist MS-transplant center — rigorous selection, transplant expertise, neurologic expertise; organized processes and documented plans if complications arise for infections surveillance, vaccination, imaging, and long-term follow-up.
What the cost of stem cell therapy for MS really means
Why is price such a sensitive issue
The phrase cost of stem cell therapy for MS is emotionally loaded because it sits at the intersection of hope, uncertainty, and private medicine. The most honest way to discuss it is in broad bands only. Private prices are not standardized. They vary by country, cell type, whether the treatment is hospital-based AHSCT or a lower-intensity commercial package, how long hospitalization lasts, and whether follow-up medications, flights, hotels, or complication management are included. The multiple sclerosis Society UK specifically warns that overseas quotes vary between centres and may or may not include travel, hotel, or follow-up medications.
Broad price ranges, not false precision
At the lower end, commercial medical-travel listings for multiple sclerosis stem cell packages often advertise prices in the low five figures USD. At the higher end, a major hospital-based AHSCT program can reach the low six figures USD, with Cleveland Clinic estimating an uncomplicated AHSCT course at about $150,000. So a fair broad range is: from tens of thousands of US dollars to around the low six figures, depending heavily on what is actually being offered. That is why price by itself tells you almost nothing about quality.
A more valuable inquiry is whether the quote represents actual transplant-level healthcare or simply appealing packaging. Cheaper is not better, and in multiple sclerosis, more expensive isn’t always smarter. How the clinic is handling such a treatment over, to whom, in what sort of regulated program, and with follow-ups that are open — those details matter.
Why risks still need to be part of the conversation
AHSCT is promising, but it is not low-intensity medicine
One reason experienced centers sound more cautious is that AHSCT is not trivial. Cleveland Clinic lists early toxicities, including relapse during mobilization, leukapheresis complications, cytotoxic drug side effects such as nausea and infertility, complications of myelosuppression such as infection or bleeding, and engraftment syndrome. It also notes that transplant-related mortality used to be 2% or higher, though current estimates for AHSCT performed after 2012 are around 0.2–0.3%. That is improved safety, not zero risk.
This is another reason the stem cell clinic question cannot be separated from the multiple sclerosis question itself. Not every person with multiple sclerosis is a candidate. Not every form of multiple sclerosis responds the same way. And not every promising therapy is worth pursuing in every disease stage. The more responsible a clinic sounds, the more likely it is to talk about selection and trade-offs, not just transformation.
The most honest conclusion
The truth is more useful than the sales pitch. Stem cell therapy for multiple sclerosis is not fiction, and it is not one thing. AHSCT has the strongest current support in carefully selected people with highly active relapsing multiple sclerosis, particularly after failure of high-efficacy DMTs, while MSC therapy remains at the clinical-trial stage. Private pricing varies widely, from low-five-figure advertised packages to low-six-figure hospital-based transplant programs, but cost should never be the first filter. In multiple sclerosis, the better question is not “Which stem cell clinic is cheapest?” It is “Which center is honest enough to tell me whether I am actually an appropriate candidate?”
Frequently Asked Questions
1) Is stem cell therapy already standard treatment for multiple sclerosis?
Not across the board. AHSCT is a serious treatment option used in selected multiple sclerosis cases at experienced centers, especially for highly active relapsing disease, while MSC therapy is still considered investigational and remains at the clinical-trial stage.
2) Who is most likely to benefit from AHSCT?
Current guidance points most strongly toward younger people with relatively recent disease onset, who are still ambulatory and have highly active relapsing multiple sclerosis despite high-efficacy DMTs.
3) What should I ask a stem cell clinic before deciding?
Ask exactly which therapy is being offered, whether it is AHSCT or MSC, whether the center has MS-transplant expertise, whether it meets international standards such as JACIE-style accreditation, and what follow-up care is included after treatment.
4) What is the cost of stem cell therapy for MS in broad terms?
A cautious broad range is tens of thousands of US dollars up to the low six figures, depending on whether the offering is a commercial low-intensity package or a hospital-based AHSCT program. Cleveland Clinic estimates uncomplicated AHSCT at about $150,000, and the multiple sclerosis Society notes that private quotes vary and may exclude travel, lodging, or follow-up medication.
5) Is MSC therapy the same as AHSCT?
No. They are fundamentally different. AHSCT is a transplant-based immune reset strategy with chemotherapy and stem cell rescue, while MSC therapy is an experimental repair/immunomodulation approach still being studied in trials.