Psoriasis is frequently mistaken for a skin ailment; however, anyone who has lived with it knows it’s often much deeper than skin level. Those include the red plaques, scaling, itching, cracking nail plate, rubbing off gloving disease, arthritis-like discomfort, among others. Psoriasis, however, is fueled by immune activation, inflammatory signaling, and genetic susceptibility accelerated through a cycle of skin renewal.
That is how people looking for the best stem cell clinic for Psoriasis typically ask questions that will not only relate to the skin. Then they question whether regenerative medicine can maintain the immune environment responsible for the condition. That is: can we think differently about inflammation? And they also pose serious stem cell questions: What type of cells are being used? Is there real evidence? Is it safe? Can this work with dermatology care?
An answer holds a double-decker by nuanced, responsible Psoriasis is an immune-mediated chronic disease, and standard modern care comprises topical therapy, phototherapy, systemic medication, as well as biologicals targeting the TNF-alpha IL-17 or IL-23 pathway. Biologics — proteins that target specific immune cells or proteins, the National Psoriasis Foundation says, are used for the treatment of psoriasis and psoriatic arthritis.
Psoriasis Is an Immune Conversation, Not Just a Skin Cycle
Why this matters for the best stem cell clinic
A best stem cell clinic should not describe psoriasis as a simple cosmetic skin issue. It should understand the immune layer behind the disease. Patients may have skin plaques, but they may also have joint pain, fatigue, metabolic risk, emotional stress, or reduced quality of life.
This is why any clinic discussing stem cells and Psoriasis should ask about the whole patient, not only the visible skin.
Where Stem Cells Enter the Psoriasis Discussion
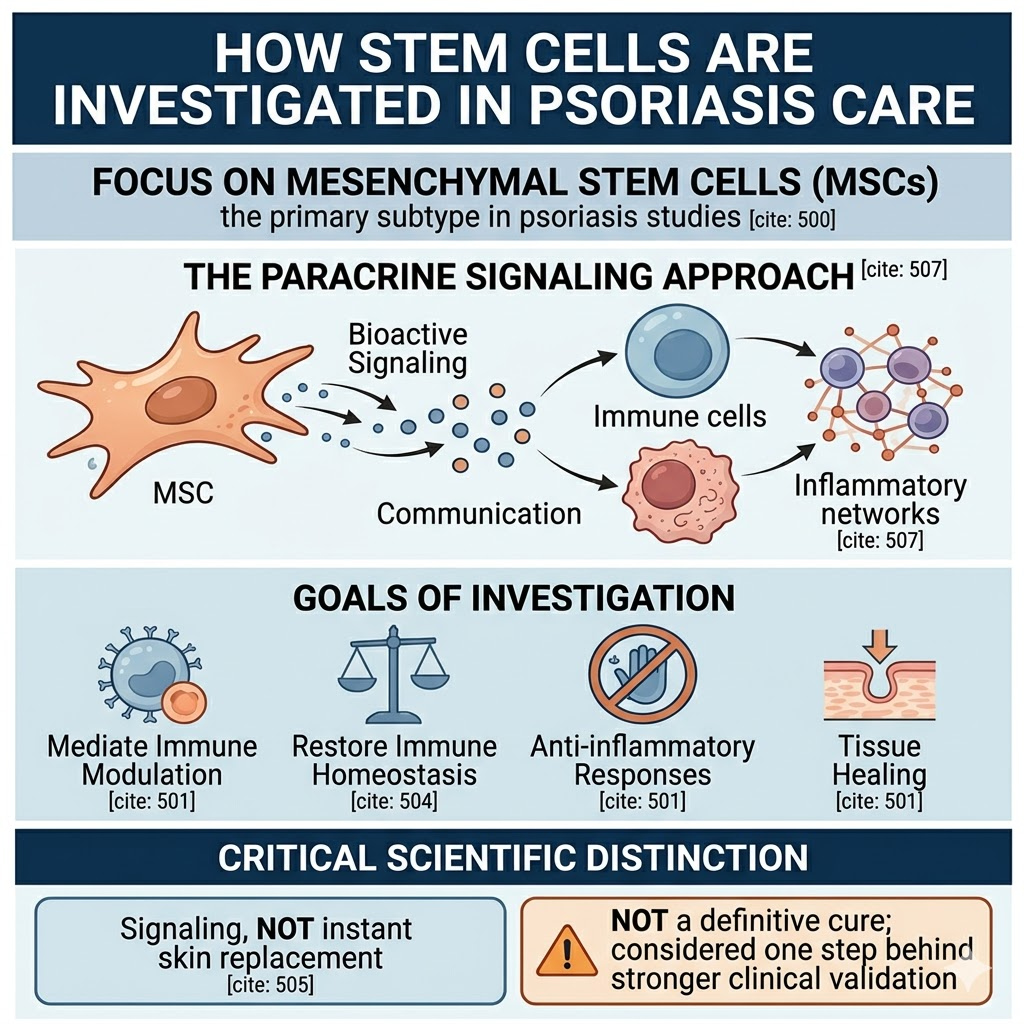
Here, the most frequently reported pluripotent stem cell subtype in psoriasis studies is called mesenchymal stem cells (MSC). MSCs are investigated as they may provide bioactive signaling that can mediate immune modulation, anti-inflammatory responses, tissue healing, communication, and cellular signaling.
In 2025, a review summary of in vitro, animal, and clinical findings on psoriasis MSCs described them as an attractive avenue for further study but nonetheless pointed out that stem cell therapy for the treatment of psoriasis is still considered one step behind stronger clinical validation.
That distinction is important. A best stem cell clinic would never claim that Stem cells are a definite cure for Psoriasis. A more accurate explanation would be that MSC-based approaches are being considered for their ability to selectively modulate inflammatory pathways and restore immune homeostasis.
Signaling, not instant skin replacement
For psoriasis, the goal is not to inject cells and grow new, perfect skin. That is not how the disease works. Much of the interest in MSCs comes from paracrine signaling, meaning the cells may release molecules that interact with immune cells and inflammatory networks.
This is why the better medical conversation is not “stem cells will erase psoriasis.” The better question is whether cell-based signaling may help influence the inflammatory environment involved in Psoriasis, especially in complex or treatment-resistant cases.
The Best Stem Cell Clinic Should Respect Standard Dermatology
A legitimate top stem cell clinic will not put regenerative medicine in a battle against dermatology. PsA already has evidence-based therapies available. Topical medication that works for others. Phototherapy, oral systemic medications, biologics, or combination care will be needed by others.
Because biologics target specific immune pathways, their role in the treatment of moderate-to-severe psoriasis has expanded considerably. Ongoing psoriasis research remains centered around IL-17 and IL-23 inhibitors, indicating the key role of immune-targeted therapy in contemporary psoriasis management.
When patients start asking stem cell questions
In general, when patients begin to feel stuck, they start asking stem cell questions. Perhaps topical creams will never be enough. Perhaps the biologics worked well initially, but later lost their effectiveness. Perhaps there are joint symptoms or fatigue, or systemic inflammation as well. Perhaps the patient requested a more integrative approach.
These questions are valid. Answers need to be medically cautious, however.
Stem Cell Questions Patients Should Ask Before Treatment
Instead of asking only, “Is this the best stem cell clinic?” patients should ask better and more specific stem cell questions.
What cell type is being used?
Not all stem cells are the same. MSCs from umbilical cord, adipose tissue, bone marrow, and other sources may differ in biology, processing, and clinical rationale. A clinic should explain this clearly.
Is there evidence for psoriasis specifically?
A clinic should not rely only on general stem cell language. Psoriasis has its own immune mechanisms. Patients should ask whether the clinic can explain published evidence related to psoriasis, psoriatic disease, or immune modulation.
Is the goal skin clearance or immune support?
These are different goals. A responsible best stem cell clinic should not guarantee complete plaque clearance. It may discuss supportive immune balance or inflammation modulation, but outcomes should be measured honestly.
How are the cells tested?
Patients should ask about donor screening, sterility testing, viability, endotoxin testing, cell identity, and laboratory standards. Stem cell quality is not a marketing detail; it is a safety issue.
Will dermatology care continue?
The safest answer should be yes. A best stem cell clinic should encourage patients to continue working with their dermatologist or rheumatologist, especially if psoriatic arthritis, severe skin disease, or systemic medication is involved.
What Current Research Suggests — and What It Does Not
Early clinical reports and small studies investigating MSC-based strategies have been published in psoriasis. Meanwhile, a 2025 Frontiers report on MSCs as rescue therapy in biologic-refractory psoriasis indicated that while published clinical trials so far involved small patient numbers and noted that there were no serious adverse events reported by four MSC trials of just 35 total psoriasis patients, the same context highlights why controlled studies with larger cohorts are still required.
That is precisely how the best stem cell clinic should sound: optimistic, but not overstated.
What research may suggest
MSC-based approaches may be interesting because of possible immunomodulatory, anti-inflammatory, and tissue-signaling effects.
What research does not prove yet
Current evidence does not prove that stem cells can cure Psoriasis, replace biologics for every patient, or permanently reset the immune system. Patients should be cautious if a clinic promises guaranteed skin clearance or permanent remission.
Safety Should Not Be an Afterthought
Quality of product, medical screening, route, and follow-up are vital to stem cell medicine. Cell products that have not been properly regulated carry risks.
US FDA warns of cases of misleading marketing for many regenerative medicine products, such as stem cells and exosomes. As such, blood-forming stem cells derived from umbilical cord blood (for diseases of hematopoiesis) are the only US-FDA approved products, not for non- hematopoietic conditional use as with immune or skin disorders.
That does not mean all stem cell research should be ruled out. This means one of the best stem cell clinics will be very clear, careful, and only perform medical-level procedures.
A Better Model for Psoriasis Regenerative Care
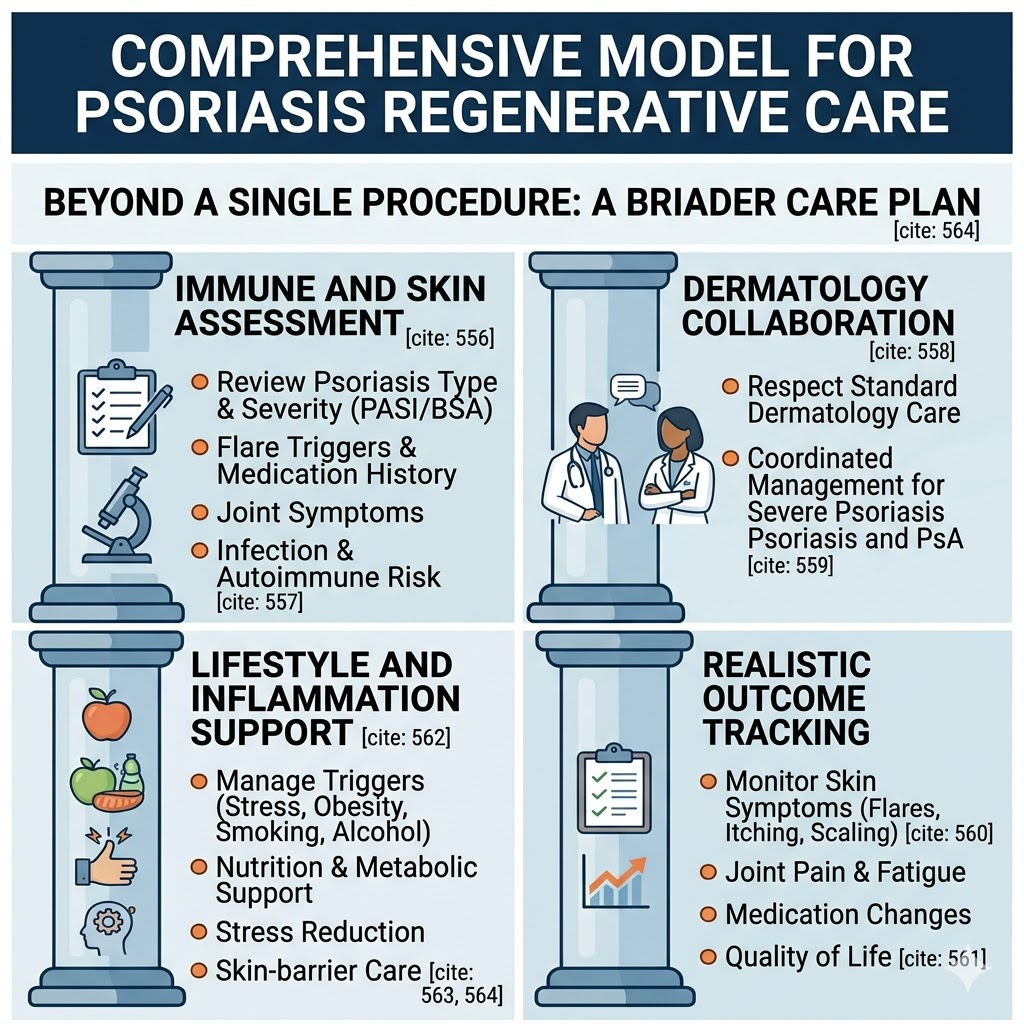
For Psoriasis, a thoughtful regenerative program should look beyond one injection or one procedure. It should include:
Immune and Skin Assessment
The clinic should review psoriasis type, severity, PASI or body surface area when available, joint symptoms, flare triggers, medication history, infection risk, and autoimmune background.
Dermatology Collaboration
A strong clinic should respect dermatology care, not replace it. Severe psoriasis and psoriatic arthritis need coordinated management.
Realistic Outcome Tracking
Progress should be tracked through skin symptoms, flare frequency, itching, scaling, joint pain, fatigue, medication changes, and quality of life.
Lifestyle and Inflammation Support
Psoriasis may be influenced by stress, obesity, smoking, alcohol, metabolic syndrome, sleep, and systemic inflammation. A broader care plan may include nutrition, metabolic support, stress reduction, and skin-barrier care.
Conclusion: The Best Stem Cell Clinic Should Answer Clearly, Not Promise Loudly
Although locating the ideal Psoriasis Stem Cell Treatment center, it ought not to end up about identifying the swankiest assertion. It should be about a clinic that understands psoriasis as an immune-mediated disease; appreciates the role of dermatology care and education; distills science without over-simplifying it, while still willing to answer hard stem cell questions nicely.
The study of stem cells, particularly MSCs, is scientifically fascinating for the possible role they could play in immune modulation and inflammatory equilibrium. However, it is still an evolving area of psoriasis and not a definitive cure.
The most appropriate medical approach for patients with Psoriasis is cautious, gradual, and transparent: dermatology rooted in evidence-based medicine, minimal regenerative discourse, cell preparation focusing on safety genome-managed therapy cord, and out-of-the-box lifestyle support with ongoing downrange follow-up. We never sell certainty where science is still developing. It guides patients in understanding what is shaping up, what remains hazy, and how to make decisions balancing hope with caution.