Best Stem Cell Clinic and chronic diabetic wounds: Is There Really a Cure for Diabetes Wound?
Why this topic needs a more honest conversation
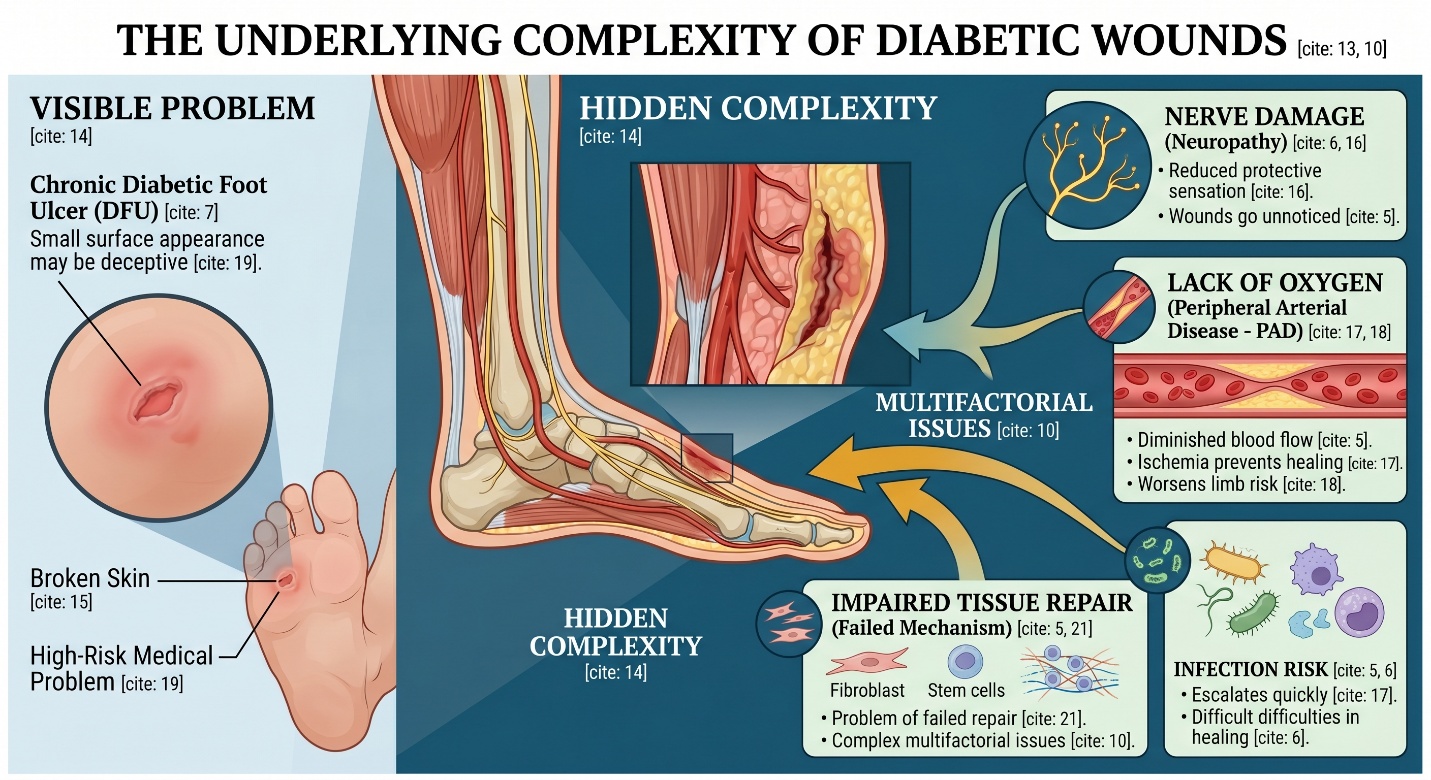
So if you are anybody looking for the best stem cell clinic for a chronic diabetic wounds, it typically brings more than curiosity. They frequently come with a sense of urgency, an unhealed wound that is working itself into higher levels of infection, and sometimes their brother worries about amputation. This urgency is why this topic deserves exact language. Wounds heal poorly in diabetes as nerve damage, lack of oxygen due to diminished blood flow, infection risk, and impaired tissue repair all happen simultaneously. According to the CDC, diabetes decreases blood flow and causes nerve damage, making wounds more susceptible to infections and difficulties in healing; IWGDF guidelines identify diabetes related foot ulcers as a major cause of morbidity, mortality, and costs.
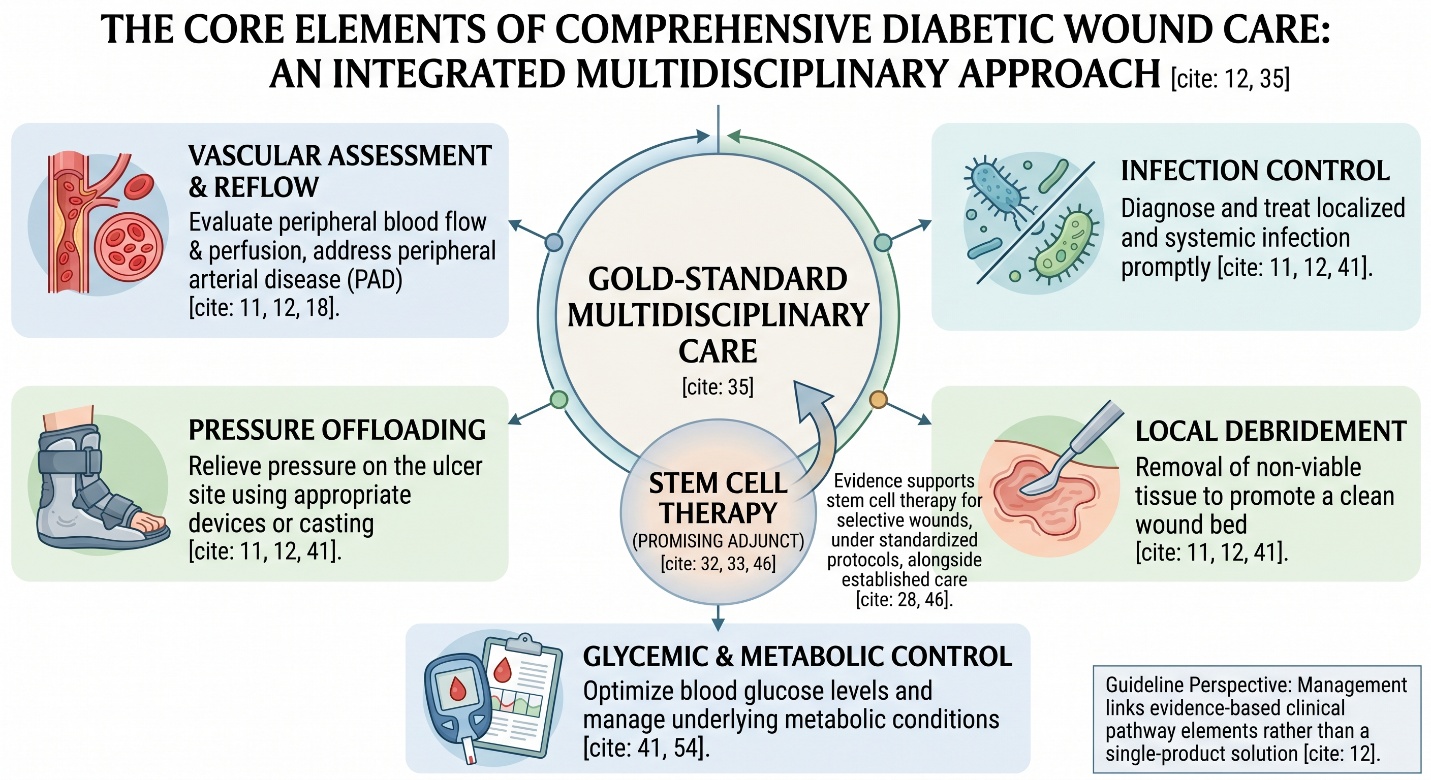
And that is also why the term cure for diabetes holds out an emotion-based promise which, in clinical reality, can not be fulfilled with any effective and lasting result. One magic ingredient or one magical procedure does not usually solve the problem of chronic diabetic wounds permanently. Our contemporary guideline perspective is weighed with added complexity: Wound healing compromises a range of multifactorial issues; local debridement, pressure offloading, treatment for infection, and vascular assessment or revascularisation, where poor perfusion had played its part. In the management of diabetic foot ulcer, the best standard care is defined by IWGDF as local debridement, offloading, revascularisation, and treatment of infection where appropriate, while NICE continues to represent diabetic foot management as a scaffold linking evidence-based clinical pathway elements rather than a single-product solution.
Why are chronic diabetic wounds so difficult to heal
The wound is only the visible part of the problem
A diabetic foot ulcer or chronic lower-extremity wound is not just broken skin. It is often the surface sign of deeper metabolic and vascular trouble. Nerve injury can reduce protective sensation. Peripheral arterial disease can limit oxygen delivery. Infection can escalate quickly. IWGDF’s PAD guideline notes that about half of people with diabetes and a foot ulcer have peripheral artery disease, which significantly worsens healing and limb risk. That is why a wound that looks “small” on the outside may still behave like a high-risk medical problem.
This is why regenerative medicine attracted attention in the first place.
Once you understand that chronic diabetic wounds are a problem of failed repair, the appeal of stem cells becomes obvious. Researchers are not interested in stem cells for wounds just because the term sounds futuristic. They are studying them because mesenchymal stromal or stem cells may influence inflammation, angiogenesis, fibroblast activity, extracellular matrix remodeling, and paracrine signaling in ways that could improve healing biology. Recent reviews of diabetic foot ulcers and chronic diabetic wounds describe stem cell therapy as a promising adjunctive approach for precisely those reasons.
What the evidence actually shows about stem cells in chronic diabetic wounds care
The signal is real, but it is still an adjunctive signal
This is the part that should be said clearly. The evidence is not empty. A 2025 meta-analysis of randomized controlled trials found that mesenchymal stem cell therapy significantly improved complete healing rates in diabetic foot ulcers overall, especially in smaller ulcers under 5 cm². But the same study also found no stable benefit for amputation prevention, recurrence reduction, or serious adverse events, and the authors called for multicenter phase III trials with standardized protocols. That is not a dismissal of stem cell therapy. It is a mature description of a field that is promising, but not finished.
That same pattern appears in broader evidence summaries. A 2025 umbrella review of chronic lower-extremity ulcers described stem cell therapy as a promising adjunctive therapy with potential benefits and acceptable safety signals, while recent network and source-comparison meta-analyses in diabetic foot ulcers also reported positive effects on wound healing with variation by stem cell source and study design. In other words, the research trend is encouraging, but it is still describing adjunctive wound-healing support, not a universal cure.
The most important word is still “adjunctive.”
This matters because the strongest wound-healing studies do not suggest that stem cells replace standard care. IWGDF’s 2023 wound-healing guideline explicitly states that interventions to improve healing should be used in conjunction with established aspects of gold-standard multidisciplinary care. That phrase is crucial. It means stem cell therapy, even where promising, belongs inside a wound-care system — not above it, and not instead of it.
What “best stem cell clinic” should really mean
It should mean better clinical judgment, not louder marketing
The phrase best stem cell clinic is popular because people want a shortcut. But in chronic diabetic wounds medicine, the better question is not “Who markets stem cells best?” It is “Who manages chronic diabetic wounds properly?” A credible clinic should first sound like a wound clinic: careful vascular assessment, infection recognition, offloading, debridement, glycemic control, and realistic staging of what the wound actually is. Only after that should regenerative options even come into the conversation. That approach is much closer to IWGDF and NICE than to the kind of branding that treats stem cells as a stand-alone rescue answer.
A good clinic should also be honest about what is not proven.
This is another place where wording matters. The current evidence does not support saying stem cells are a proven cure for diabetic wounds. It supports saying that some stem cell approaches may improve healing rates in selected chronic diabetic wounds, especially diabetic foot ulcers, when used alongside established care. A clinic that cannot say that clearly is not making the science sound stronger — it is making the science sound less trustworthy.
Why caution still matters
Regulators have been explicit about unapproved regenerative products.
FDA’s patient and consumer guidance says there is broad marketing of unapproved regenerative medicine products intended for the treatment or cure of many diseases and conditions, and that these products require FDA oversight in clinical trials before approval. FDA also warns that if patients are being charged for such products outside a properly overseen clinical trial, they are likely being deceived, and it lists risks including infections, tumor formation, immune reactions, and product contamination. Those warnings are not theoretical. They exist because regenerative language can be used long before evidence and oversight are solid enough to protect patients.
The most honest conclusion
The truth is more useful than the sales pitch. Chronic diabetic wounds are difficult because the biology is difficult. Stem cell therapy has become one of the more interesting regenerative strategies in this space, and current trials and meta-analyses suggest that it may improve wound closure in some patients, particularly as an adjunct to strong multidisciplinary wound care. But that is still very different from offering a guaranteed cure for diabetes wound, and it is also very different from assuming the best stem cell clinic is simply the one making the biggest promise. Right now, the most credible answer is this: in chronic diabetic wounds care, the “best” clinic is the one that treats stem cells as part of careful medicine — not as a shortcut around it.