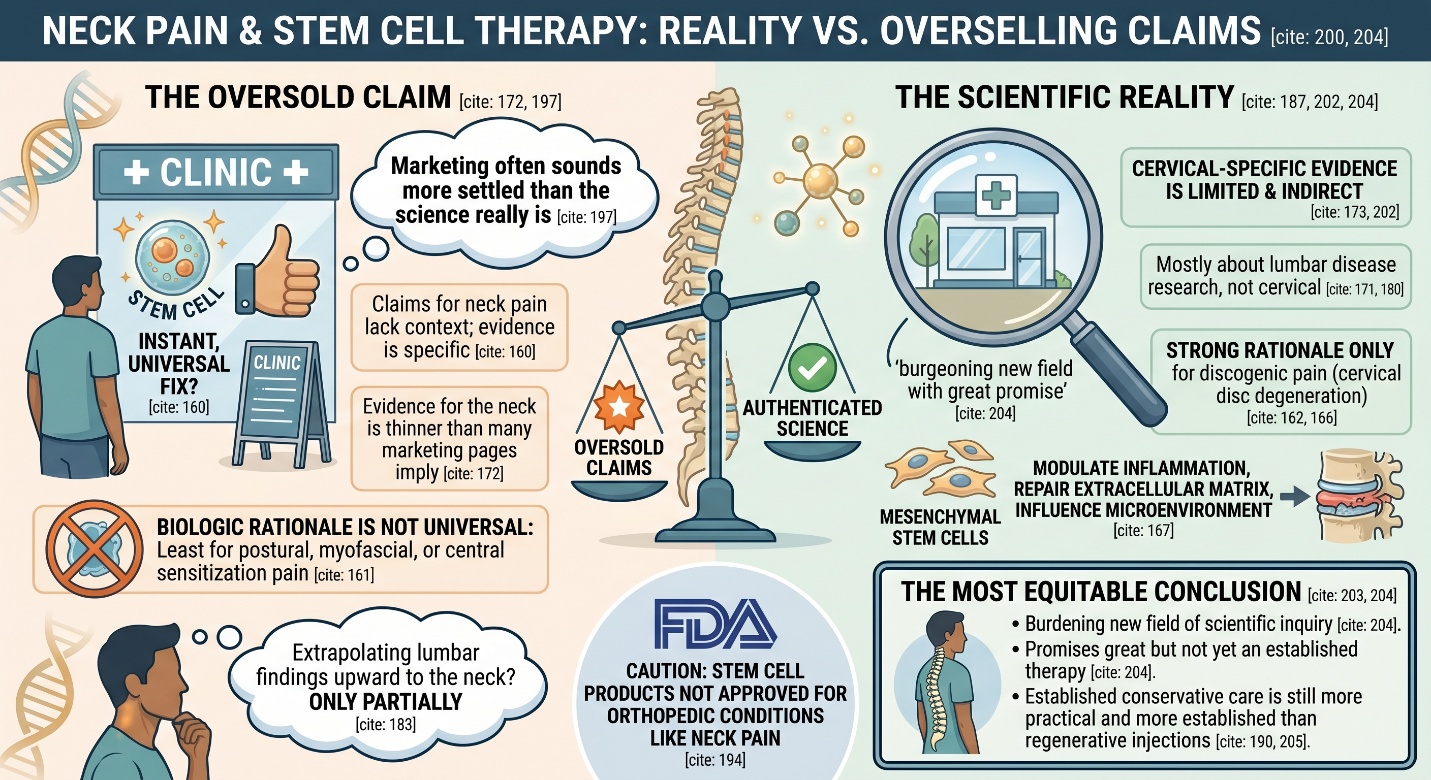
Why this topic gets searched so often
Anyone searching stem cell for neck pain is usually looking for something more meaningful than short-term relief. Neck pain can be stubborn, recurrent, and surprisingly disruptive. The American College of Radiology notes that cervical spine pain is one of the most common reasons people seek medical care and ranks among the top five causes of years lived with disability globally. That alone explains why regenerative medicine keeps entering the conversation.
Still, this is also one of those subjects where the internet seems to outpace the evidence. The word combination “stem cell for neck pain” may seem simple enough but the problem is cervical spine pain is not one diagnosis. Nonspecific muscular pain; degenerative disc disease, facet-related pain or cervical radiculopathy (nerve irritation). Realising that, the research reads more easily: not all types of neck pain are studied in an identical fashion; and not every patient issue falls neatly into a regenerative treatment paradigm.
Why cervical spine pain is more complex than it looks
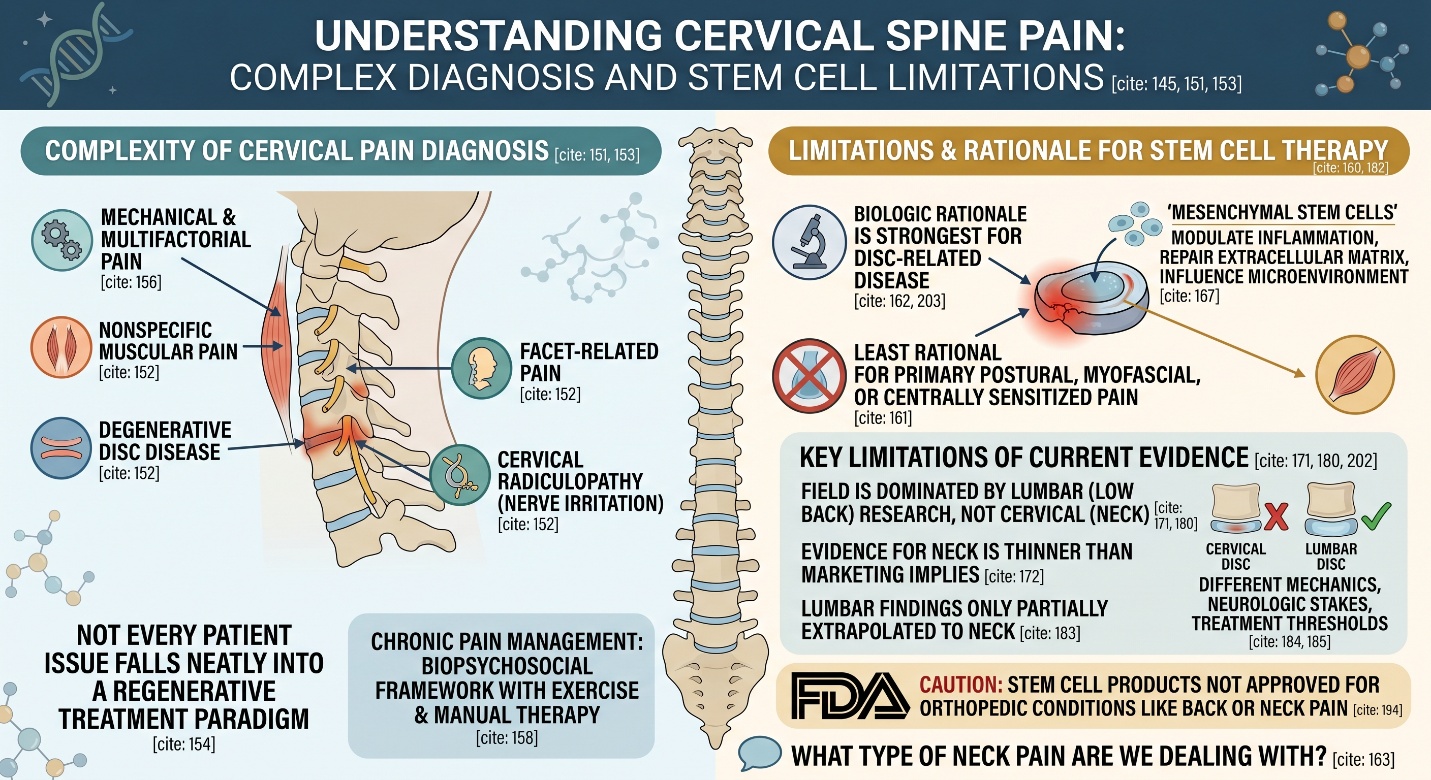
Neck pain is often mechanical, multifactorial, and not purely “disc damage.”
This is where many articles become too simplistic. People often imagine neck pain as one damaged structure that simply needs to be repaired. In reality, clinical practice literature describes chronic neck pain as a condition usually managed through a biopsychosocial and conservative framework, with exercise therapy, education, and manual therapy commonly recommended. Recent umbrella and systematic reviews also report that exercise and manual therapy improve pain and function better than no treatment, even if no single approach fixes every case.
Why this point matters: Because stem cell research is often treated as if it applied to all neck pain. It does not. The biologic rationale is least for pain that is primarily postural, myofascial, centrally sensitized or an obvious surgical problem requiring decompression or stabilization; it is strongest when the suspected source of neurologic injury (e.g., cervical disc degeneration/related discogenic pain). So put simply, before asking do stem cells help neck pain — the more useful question is: what type of neck pain are we dealing with?
Where stem cell enters the cervical spine conversation
Most regenerative thinking in the neck comes from disc-degeneration biology
Intervertebral disc degeneration is the main regenerative argument for stem cell use in the spine. The biological rationale is appealing to allow mesenchymal stromal or stem cells to modulate inflammation, repair the extracellular matrix and positively influence disc microenvironment via paracrine action rather than strictly through structural replacement. Recent reviews on DD suggest that this remains one of the most active spine regeneration research areas.
However, there is an important limitation that patients rarely hear clearly. Much of the published clinical literature on cell-based disc therapy is drawn from lumbar discogenic pain, not the cervical spine. A 2026 review of cell-based therapies for intervertebral disc degeneration identified 42 clinical studies overall, but the field remains dominated by lumbar disease research rather than mature, neck-specific evidence. That does not make cervical applications impossible; it just means the evidence for the neck is thinner than many marketing pages imply.
Cervical-specific evidence exists, but it is still limited
There are signs of cervical examination. For example, Clinical Trials. A trial of autologous bone marrow mesenchymal stem cell transplantation in patients with cervical disc degeneration on Clinical trials. gov And it makes sense because this is a real research area, not just a sales term. Even so, this could not be taken as a standard clinic verification and resting study is still cannot on its own scenario important long-term advantage.
What the evidence actually supports right now
The strongest positive data are still indirect for neck pain
If someone wants the cleanest honest summary, it is this: the best current evidence for spine-related stem cell treatment comes mainly from discogenic pain studies, especially lumbar studies, not from large definitive trials in cervical spine pain. A 2025 systematic review of mesenchymal stromal cells for chronic discogenic pain reported signals of pain and disability improvement, but again, that body of evidence is mostly about low back pain rather than neck pain. That makes the cervical conversation more cautious by default.
So, can those lumbar findings be extrapolated upward to the neck? Only partially, and carefully. The cervical and lumbar discs share some biologic principles, but they are not interchangeable clinical problems. The cervical spine has different mechanics, different neurologic stakes, and often different treatment thresholds. That is why claiming that stem cells “work for neck pain” as a finished fact goes beyond what the current evidence can honestly support.
Conservative care still has a stronger evidence base
This part may sound less exciting, but it is more clinically useful. Recent reviews of non-surgical treatment for cervical pain continue to support exercise, physical therapy, and manual therapy as meaningful components of care, with improvements in pain and function shown across multiple analyses. For many patients with chronic neck pain, that evidence base is still more practical and more established than regenerative injections.
Why caution still matters
FDA has been very direct about orthopedic and neck pain claims
The clear regulatory sentence in this whole discussion comes to us from the FDA. According to a consumer alert regarding regenerative medicine products released by the FDA, products intended as stem cells, exosomes, stromal vascular fraction, Wharton’s jelly, and amniotic fluid and related biologics are not approved for use in orthopedic conditions such as disc disease, back pain, or neck pain. The FDA further cautions that patients may be deceived by illegally marketed products without proof of safety or effectiveness.
That does not mean all stem cell research in spine care is meaningless. It means the field is still investigational, and the marketing language often sounds more settled than the science really is. For patients, that distinction matters. A promising mechanism is not the same as a standard of care, and an early clinical signal is not the same as a mature treatment pathway.
The most honest conclusion
The truth about stem cell and neck pain is more nuanced than a yes-or-no headline. There is a real scientific rationale for studying cell-based therapy in degenerative disc disease, and some broader spine literature suggests potential for pain and functional improvement. But when the question is narrowed specifically to cervical spine pain, the evidence is still limited, more indirect than many people realize, and far from routine clinical certainty.
Regenerative medicine has, to its credit, made research relevant for neck pain more biologically interesting — particularly in disc-related disease — but it alone isn’t yet a tried-and-true solution to monotonous cervical discomfort; that is the most equitable way of stating things. At the moment, even stem-cell-based interventions should be viewed as a burgeoning new field of scientific inquiry with great promise but not yet akin to an established therapy; instead, proper examination is still best executed by methodically sussing out etiology while responsibly deploying over-proven conservative care.