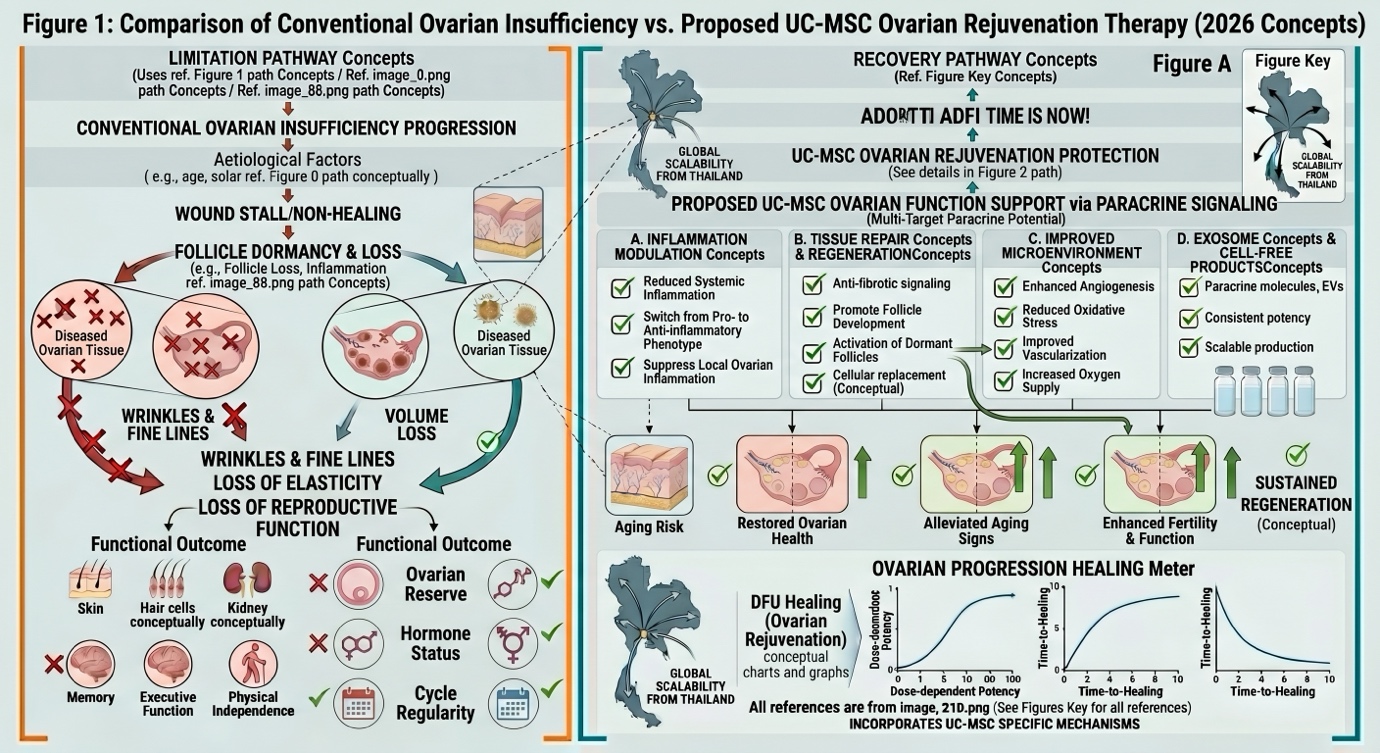
How Is Stem Cells Processed In Thailand To Enhance Female Fertility?
Infertility has emerged as an important global health problem, impacting millions of women and couples worldwide with considerable emotional suffering, psychological distress, and social pressure. Modern reproductive technologies such as in vitro fertilization (IVF), hormonal therapies and surgical interventions have helped innumerable couples conceive — but they do not always address infertility at its source.
Regenerative medicine is paving the way for the fertility care of tomorrow. UC-MSC is one of the potential ways. These cells have powerful properties of regenerative, anti-inflammatory and immunomodulatory potentials for repair reproductive tissue failure and restoring appropriate biological environment for conception. The new method is already in clinical trial as UC-MSC stem cell therapy for women who are unable to get pregnant with conventional fertility remedy, rapid growing Thailand regenerative remedy.
CELLULAR INSIGHTS INTO FEMALE INFERTILITY
The causes of female infertility are numerous. It may be related to a number of issues such as declining ovarian reserve with age, premature ovarian failure, damage due to chemotherapy or radiation therapy, autoimmune disorders and endometrial remote secretion of cytokines and hormonal imbalance as well as uterine structural abnormality. In most cases, the actual cause is deterioration of cells and tissues all in involvement annexed either egg generation, hormone handling or embryo joining.
Stem cell therapy is directed at restoring function rather than simply compensating. Unlike surgery, which removes blocked tubes and bypasses the problem altogether, regenerative treatment aims to repair the ovarian and uterine ecosystem as a whole to help make natural reproduction systems function more effectively.
Ovarian Function Restoration
Ovary is a major target for regenerative treatment of fertility. Ovarian aging or damage may result in difficulty conceiving, due to fewer oocytes (eggs) available at any one time, or because of a poorer quality of the oocyte population.
Ovarian restorative properties of stem cells have been elucidated through various mechanisms. In addition, they secrete growth factors and signalling molecules that participate in tissue repair and improve blood perfusion while reducing inflammation within the ovaries. Increased blood flow helps provide oxygen and nutrients to developing follicles, which may also result in healthier egg development.
Based on research reports and clinical experience stem cell therapy is effective for hormonal balance, follicularity as well as the menstruation in women with premature ovarian insufficiency. All of which may create a more conducive ovarian microenvironment and, therefore, elevate the possibility for natural conception or success with assisted reproductive technologies.
Improving Egg Quality
While the quantity of available eggs is of course significant, quality is another big factor in successful fertilization and embryo development. This has been attributed to age-specific oxidative stress, mitochondrial malfunction and epigenetic influence impairing the viability of oocytes.
Immune improvement to boost reproductive performance in female animals is indirectly provided by stem cells through the reduction of oxidative damage and the increase of metabolic status in ovarian tissue. Notably, the factors that these cells secrete promote both mitochondrial function and cellular repair thus establishing an environment conducive to appropriate egg development. Improved egg quality means improved fertilisation rates and less risk of miscarriage.
Uterine and Endometrial Regeneration
A healthy uterine landscape is equally as important for a successful pregnancy as there being healthy eggs. AbstractThe implantation of an embryo requires that the endometrium, the inner lining of the uterus, be sufficiently thick and well-vascularized (active), as well as functionally competent to promote attachment.
Chronic inflammation, an infectIon or surgery or disorder such as Asherman’s syndrome can damage this lining. Then, the endometrium could become thin or scarred or not implant at all.
Stem cell therapy offers a regenerative approach to repair the uterus. These cells are able, if implanted within the uterine micro-environment, to reduce inflammation response, limit fibrotic scarring and promote neovascularisation. They also promote angiogenesis — the reformation of blood vessels which allows more oxygen and other nutrients to conveniently reach the endometrium.
Subsequent clinical research showed that women with impaired uterine receptivity may possibly benefit from improved implantation outcomes and increased endometrial thickness post-treatment. Therefore,those treatments may also give a new perspective to those patients who have had multiple implantation failure or with thin endometrium.
Immunomodulatory Benefits
In some cases infertility is immune-related due to excessive inflammation or inappropriate immune responses that preclude embryo implantation or survival. Due to their strong immunomodulatory effect on the body, these stem cells can maintain immune homeostasis and minimize inflammation as well as provide a more balanced reproductive environment in systemically (non-implant) induced endometrium. Inhibits inflammatory cytokines which act against effector functions and modulate immune tolerance in the lung providing a favorable environment for implantation of embryo and preservation of pregnancy.
Fertility eco system: Thailand — The country for Regenerative Fertility Treatment
Thailand is a hub of advanced regenerative treatments. This country accounts for doctors with enormous experience, lab constructions that are prepared to meet the challenges of global tendencies, and clinical standards that open up a window to a real world stage. Some clinics run as a full-service clinic while offering stem cell therapy alongside treatment including hormones, imaging and assisted reproductive technologies if needed.
This comprises the two and allows treatment according to a condition regardless is practiced by natural conception or embryo transfer success by IVF.
Opening New Doors For Her With Uncommon Alternatives
These women have been left with little option other than egg donation, until regenerative therapy resurrected out of sight the hopes for assisting those suffering recurrent IVF failure, overcoming damage caused by early ovarian decline or uterine injury. And although data remains sparse and seemingly heavily dependent on patient factors including age and comorbidity, early findings suggest stem cell therapy may restore reproductive potential in select cases.
And most importantly, this is an approach to entire reproductive health, not just symptom management. When used appropriately, regenerative treatment might boost fertility potential and promote long term reproductive health via its ability to enhance tissue quality, reduce inflammation, and maintain cellular repair processes.
Conclusion
The introduction of cell-based therapies from UC-MSC stem cell therapy is a novel and most remarkable area of female reproductive medicine. This regenerative approach is particularly powerful as it addresses the physiological causes of failure to conceive —including ovarian dysfunction, impaired oocyte quality and uterine injury—leading best to repair and allow the organ system to return properly and have its natural ability to achieve conception.
This new approach may provide an alternative therapy for women who have failed traditional therapies, or face reproductive challenges due to age, medical treatments, and tissue injury. As clinical research continues, and technologies rapidly advance, regenerative medicine is poised to lead the way as a critical part of comprehensive fertility care further down this path by giving women greater family building.