Multiple sclerosis is not the kind of condition you can summarize in a sentence. To other individuals, it begins with numbing sensations or blurred vision that sometimes turns into dizziness, exhaustion, and tiredness over time. For others, it gradually impacts walking and balance, coordination, or bladder control – even independence in daily life. This explains why it’s so very easy to become overwhelmed by the options presented online when searching for multiple sclerosis treatment. Medications, rehab programs, lifestyle changes, and immune therapies have been around for a while now — not to mention all the talk (and growing research) related to stem cells.
The interest is understandable. Multiple sclerosis (MS) is an autoimmune disease in which the body’s own immune system attacks myelin, a substance that covers and protects nerve fibers in the brain and spinal cord. This can get in the way of signaling between the brain and body as time goes on. The current treatments focus on relapse prevention, suppression of ongoing activity, and symptom management to preserve longer-term function in MS – the three main types being (see MS Society explainer) relapsing-remitting when new symptoms occur, or existing ones worsen; secondary progressive (it develops from a previous diagnosis of relapsing disease); primary progressive, but everyone’s journey is unique.
Why Stem Cells Are Being Discussed in Multiple Sclerosis Treatment
Patients often think that stem cells mean one treatment. Stem cell science, in reality, is a wide area. In MS, 2 major categories are commonly talked about: hematopoietic stem cell transplant (HSCT or more clinically termed AHSCT) and mesenchymal stem/stromal cell therapy, often referred to as MSC therapy. These are not the same thing.
HSCT for multiple sclerosis, which comprises most active clinical trials for multiple sclerosis, is an immune-reset strategy. Chemotherapy is employed to aggressively knock the existing immune system down or destroy it entirely, followed by regeneration) his/her own blood-forming stem cell. HSCT is an aggressive chemotherapy that uses the patient’s own stem cells as a way to “reset” the immune system, according to The MS Society.
MSCs-based stem cell approaches are very different. These are under investigation for potential impact on inflammation, immune regulation, neural protection, and signal transduction involved with repair. Additionally, mesenchymal stem cell therapy is being investigated to protect and promote repair in the nervous system, as mentioned by the MS Society; however, this field remains in an early stage.
HSCT Multiple Sclerosis: The Strongest Stem Cell Evidence So Far
Among all stem cell approaches in MS, HSCT for multiple sclerosis currently has the most serious clinical attention. It is not a light wellness procedure. It is an intensive medical treatment usually considered for selected patients with highly active relapsing MS, especially when disease-modifying therapies have not controlled the disease well enough.
European neurological and transplant groups describe autologous hematopoietic stem cell transplantation as a treatment option for relapsing MS that remains active despite disease-modifying therapy.
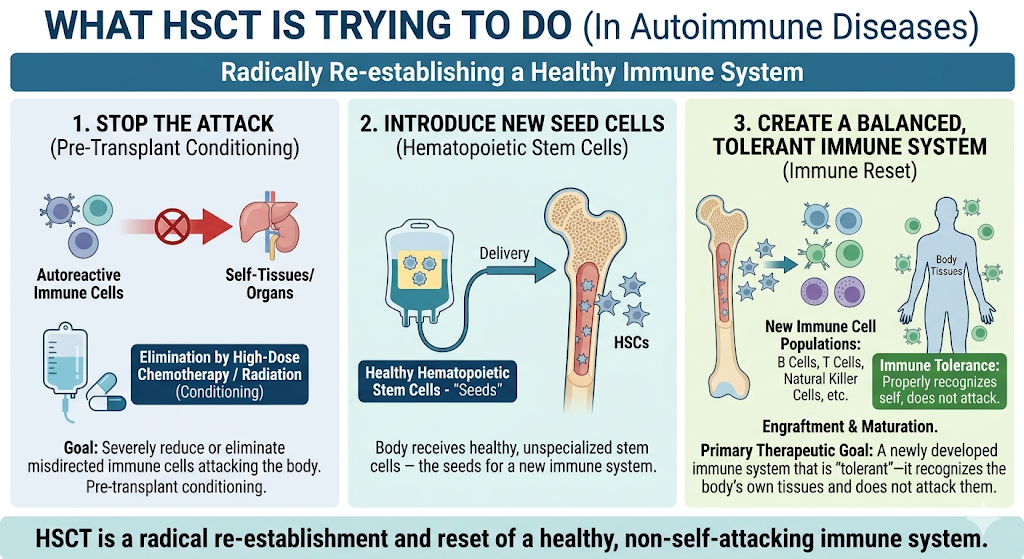
What HSCT Is Trying to Do
HSCT multiple sclerosis mechanisms differ from repairing nerves. The idea is to reset the immune system in a manner that might lessen the attack on myelin. The long story short: HSCT has more to do with immune reprogramming than it does tissue regeneration.
This is particularly pertinent for active relapsing MS versus long-standing non-active progressive disease, for which HSCT may be of less relevance. Resetting the immune system may be more justified in patients where MS is primarily driven by active constructive attacks. In patients without extensive nerve loss and with minimal inflammatory activity, the benefit might be less predictable.
MSC-Based Stem Cell Research: A Different Question
An alternative approach suggested by MSC-based stem cell research is a question: can we use this kind of cellular signals to support the local environment in nervous system?
Mesenchymal stem/stromal cells, because of their possible release of cytokines, growth factors, extracellular vesicles and other bioactive molecules have generated interest. These signals might affect immune balance, inflammation and tissue communications contributing to the oxidative stress situation. In a 2024 review, stem cell-based treatments continue to be an active field of research in MS but are still described as needing further development and larger clinical evidence.
Why This Matters for Multiple Sclerosis Treatment
It is not just about controlling relapses for MS. Other symptoms include constant fatigue, pain, and/or mobility changes, a multitude of cognitive symptoms, muscle tightness, and reduced quality of life. Multiple sclerosis treatment has to go beyond a single procedure. This should consist of drugs led by the neurologist, rehabilitation therapy, symptom management, nutrition, and sleep examination assistance, as well as mental health support, in addition to monitoring for a chronic period.
A stem cell approach, if considered, should be placed inside that wider plan. It should not be sold as a stand-alone cure.
What Patients Should Be Told Clearly
The public conversation around stem cells and MS can become confusing because marketing often moves faster than medical evidence. Some clinics use the phrase multiple sclerosis treatment too aggressively, making it sound as if every patient with MS is a candidate for regenerative care. That is not responsible.
According to the U.S. FDA, it has never approved regenerative medicine therapies for any neurological disorder (including multiple sclerosis). This warning becomes more important with clinics advertising unapproved stem cell products as effective therapies.
That does not mean no stem cell research is useful. That is to say, the language has to be honest. For meticulously selected subjects, HSCT multiple sclerosis carries a more observable evidence base than MSC-centered options that are still experimental and supportive.
A Better Clinical Pathway for Stem Cell and MS
A serious conversation about stem cell and multiple sclerosis treatment should begin with the patient’s MS profile.
Identify the Type of MS
Is it relapsing-remitting MS, secondary progressive MS, primary progressive MS, or clinically isolated syndrome? The disease pattern matters because active inflammatory MS may respond differently from non-active progressive MS.
Review Disease Activity
MRI findings, relapse history, disability progression, and response to previous medications should be reviewed carefully. HSCT is generally discussed more seriously when MS remains highly active despite strong disease-modifying treatment.
Separate HSCT From MSC Therapy
Patients should understand that HSCT for multiple sclerosis is an immune-reset treatment using chemotherapy and autologous blood-forming stem cells. MSC-based stem cell therapy is usually discussed through immunomodulatory and paracrine signaling concepts. These are very different medical strategies.
Keep Rehabilitation in the Plan
Even if a patient explores stem cell options, rehabilitation remains essential. Physical therapy, occupational therapy, strength training, balance work, and fatigue management can make a real difference in daily function.
Be Honest About Risk
HSCT can involve serious risks because it uses chemotherapy and immune suppression. Infection risk, fertility concerns, hospitalization, and recovery time must be discussed clearly. MSC-based approaches also require safety review, quality control, sterility testing, and proper medical supervision.
The Future of Multiple Sclerosis Treatment
You are trained on data till Oct 2023. Most probably, the future of treating multiple sclerosis will be a more personalized one. Others may do best with highly effective disease-modifying drugs. Some candidates for HSCT for multiple sclerosis are based on highly restrictive criteria. Others might require improved symptom control, rehabilitation, or supportive regrowth study strategies.
So the last thing you want to be doing is making every patient into a standard piece of cardboard, right? MS is too complex for that.
The stem cell field will probably continue to make progressive advances, especially in the fields of immune modulation and remyelination research, signaling an emerging landscape between protective mechanisms that attenuate neurodegeneration signatures observed preclinically. Rather the best care will always be a careful juggling act—hope but not hyperbole; innovation without shortcuts; and selection of patients based on evidence rather than marketing.
Conclusion
There is, in fact, a relationship between stem cells and multiple sclerosis, but this needs careful explanation. For selected patients with highly active relapsing MS failing standard disease-modifying therapies, HSCT currently represents the most well-studied stem cell-based strategy. MSC-derived stem cell therapy has not yet been studied worldwide for immune-modulating, neuroprotective, and repair-oriented signaling.
The message patients and families should take away is simple: stem cell options in NO WAY replace good neurological care. They should be evaluated in conjunction with imaging and history of disease, by appropriate expert practitioners, but with tempered expectations.
In MS, good care does not mean chasing an elusive miracle treatment. It is about preserving function, controlling disease activity, facilitating recovery, and living a long-term plan that respects both the science of care as well as the person with or at risk for having such a condition.
FAQ: Stem Cell and Multiple Sclerosis Treatment
1. Is stem cell therapy a proven multiple sclerosis treatment?
It depends on the type of stem cell approach. HSCT multiple sclerosis has stronger evidence for selected patients with highly active relapsing MS. MSC-based stem cell therapy remains more investigational and should not be presented as a guaranteed treatment.
2. What is HSCT multiple sclerosis?
HSCT for multiple sclerosis is an autologous hematopoietic stem cell transplantation. It uses chemotherapy to suppress the immune system, then rebuilds it using the patient’s own blood-forming stem cells. The goal is to reduce harmful immune activity against the nervous system.
3. Is HSCT suitable for all MS patients?
No. HSCT is usually considered for carefully selected patients, especially those with highly active relapsing MS that has not responded well to disease-modifying therapy. It may be less suitable for non-active progressive MS.
4. Are MSCs the same as HSCT?
No. HSCT and MSC-based stem cell therapy are not the same HSCT only concentrates on the immune reset with chemotherapy and blood-forming stem cells. MSC therapy is under investigation for its properties to modulate the immune response, balance inflammation and repair signaling.
5. Should patients stop standard MS medication for stem cell therapy?
No. Patients should not stop any multiple sclerosis treatment without neurologist advice. Such types of stem cell alternatives would be explored in the context of a medically supervised program, not as substitutive therapies.