Advances in Stem Cell Therapy at a Stem cell clinic for the Treatment of Pulmonary Fibrosis
Idiopathic illnesses are some of the most troubling in medicine. One of the more vexing illnesses within this category is Pulmonary Fibrosis. For the unfortunate patient, the insidious process of this condition leads to the irreparable scarring of lung parenchyma. This invariably compromises patients’ lung function in their daily activities and lung function in general. This leads to the gradual process of the respiratory system succumbing to total system failure. Finding proper therapeutic interventions for this is the greatest challenge of the medical community. A specialized stem cell clinic can be a beacon in the process of healing those lungs. Medical researchers’ hopes of healing the fibrotic lungs are discouraged with the often obsolete, and in some cases, cruelly designed, medical paradigms of passive lung fibrosis. Patients with Pulmonary Fibrosis should be prioritized, and their care should be designed specifically, to correct the cellular imbalances and deficiencies of the lung fibrosis.
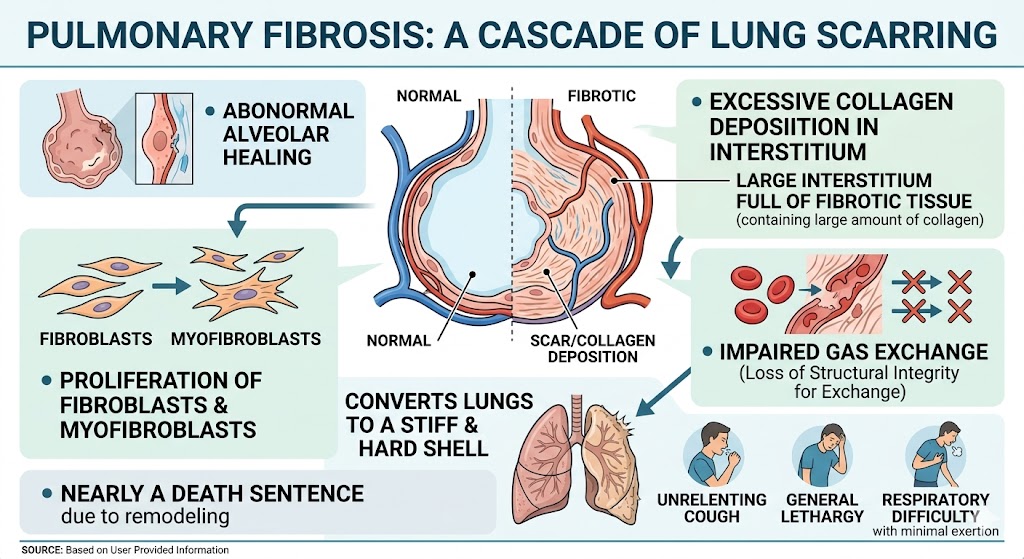
Basically, Pulmonary Fibrosis is the formation of fibrotic tissue (scar) in the lung parenchyma that occurs as a result of the abnormal healing process of the alveolar epithelium. These injuries cause a cascade of pathological processes that result in the proliferation of fibroblasts. These fibroblasts also have the potential to become myofibroblasts and subsequently deposit a large interstitium full of fibrotic tissue that contains a large amount of collagen. As a result, they destroy the alveolar capillary bed and the alveolar interstitium structural integrity required for gas exchange. Patients develop an unrelenting cough accompanied by general lethargy and respiratory difficulty with little to no exertion. These forced cascades into this fibrotic tissue renders the lungs a stiff and hard shell. Sadly, the fibrotic remodeling of the lungs is nearly a death sentence. This strongly encourages these individuals to seek out a stem cell clinic.
Figure 1: Pathophysiology of Pulmonary Fibrosis
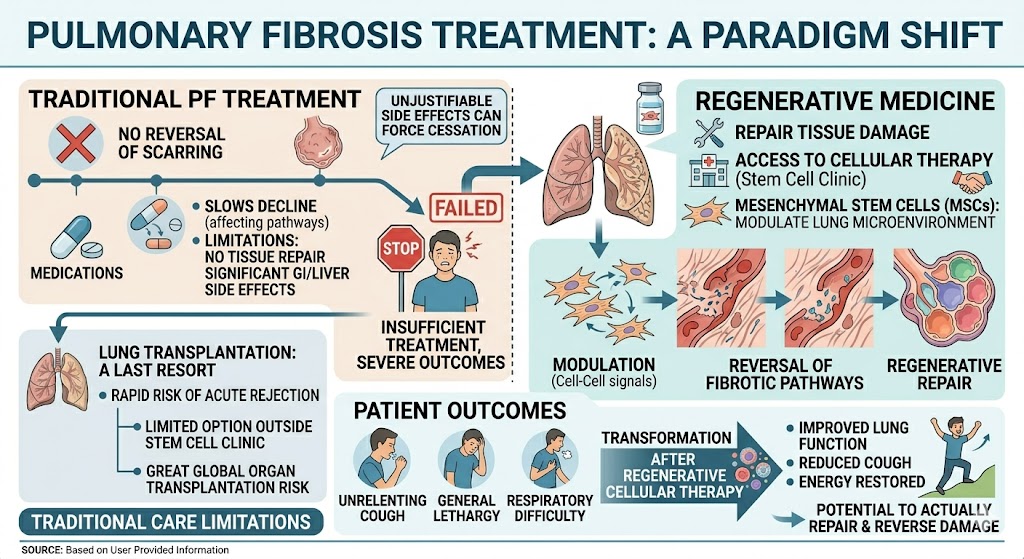
Traditionally, how Pulmonary Fibrosis is altered is dependent on the chronic use of immunosuppressants and the use of antifibrotic therapy. Pirfenidone and other medications slow lung function decline by affecting fibrogenic biological pathways. Although they alter fibrotic pathways, pirfenidone and other drugs available today have multiple limitations. These drugs don’t reverse the damage done to the tissue and lungs of the patients, nor do they reverse scarring. Additionally, they have significant gastrointestinal and liver side effects. While patients take the medications, if any of these side effects are intolerable, the medications must be discontinued. If all of these drugs become ineffective, the last resort is lung transplantation. Alternative options outside a stem cell clinic are limited by the rapidly growing and serious risk of acute transplant rejection. In sum, this is insufficient treatment. The risk of serious outcomes from the ongoing and primary side effects of this treatment is unjustifiable. Additionally, the need to endure this treatment to the end is unreasonably prevented by the great global organ transplantation risk.
Regenerative medicine has the potential to actually repair tissue damage, and significant progress has been made in this area. There are undeniable benefits of access to cellular therapy in the stem cell clinic. Mesenchymal stem cells have the ability to modulate the lung microenvironment to aid tissue repair. These cells can even reverse and modulate severe fibrotic pathways. Moreover, they can even reverse and modulate pathological tissue changes in the lung microenvironment and repair the damage. These cells can help and even reverse the damage done to the lung microenvironment. Providing treatment to the subject is a premier stem cell treatment clinic. Cellular therapy can even reverse and modulate tissue damage in the lungs of patients with Pulmonary Fibrosis.
Figure 2: A Paradigm shift of Pulmonary Fibrosis treatment
Recently, the focus on advanced therapies based in the association of the three regions centered in the Greater Mekong Subregion has become prominent. Thailand is one of the three regions and is considered the earliest mover (and probably the most accomplished) in establishing a center for the integration of higher medical infrastructures and supervised biological research. In the tropical zone, a globally accredited stem cell clinic is compliant with international standards on safety while using better biomedical technologies. The component of the National Government to subsidize medical innovation promotes a safe realm for cellular therapies to flourish. This, paired with the low cost of health, attracts a lot of medical tourists. Actively treating Pulmonary Fibrosis in this developing medical framework entails providing international patients with elite clinical facilities right at their doorstep. The short-term trend that indigenously embodies the evolving medical framework in Thailand suggests that personalized cellular medicine will very soon respond to the needs of all citizens.
Fatal lung scarring calls for the integration of therapies that go beyond symptom control. Cellular therapies, through their ability to control lung-targeted inflammation, can rejuvenate the lung and control other systemic inflammation. Attending a dedicated stem cell clinic can help those afflicted by a medical condition that is universally regarded as incurable by providing them with additional medical options that can help them combat their condition. Delivering a better prognosis relies on the breakthrough potential that great risks and great rewards possess. Ultimately, a healthier tomorrow depends on a breakthrough in Pulmonary Fibrosis and the pursuit of other living biological tests.