Many individuals suffer from pelvic organ prolapse and urinary incontinence. Prolapse causes emotional and physical irritation and discomfort worsening quality of life. Such conditions occur due to the failure of the structure of the pelvis. In the past, most practitioners employed mechanical Pelvic Floor Repair. There is an increasing emphasis in the scientific community for repairs that restore the anatomy rather than suspend their functionality. This is a reconstructive biological repair approach often championed by Regenerative Medicine Thailand. It is the first time that providing sustainable, natural pathways to healing has been available through addressing the underlying reasons at the center of the tissues at issue. Out of the innovative cellular therapies that appear to be of great assistance for deteriorated tissues.
1. Understanding the Underlying pelvic floor Mechanisms
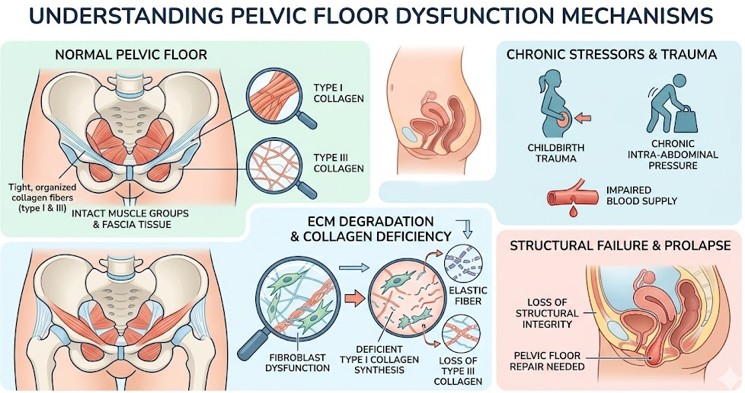
The pelvic floor is made of an intricate network of levator ani muscle groups and fascia tissues. Structural failure of the system requiring Pelvic Floor Repair is due to extreme degradation within the extracellular matrix. This degradation causes fibroblasts to become deficient in the synthesis of type 1 collagen. In addition, the changes in type I collagen and the loss in type III collagen led to loss of integrity for supporting and sustaining structures. There is mechanical trauma from childbirth and intra-abdominal pressure becomes chronic. This causes further degradation of elastic fibers. Also, the nutrient blood supply is impaired by some small bleeding within the pelvic cavity. This adverse microenvironment incites cellular senescence; hence, the local stem cells are unable to replicate or repair the damaged myofascial layers properly, a challenge increasingly addressed by Regenerative Medicine Thailand.
Figure 1: Understanding the Underlying pelvic floor Mechanisms
2. Current Conventional Therapies Alongside Inherent Limitations
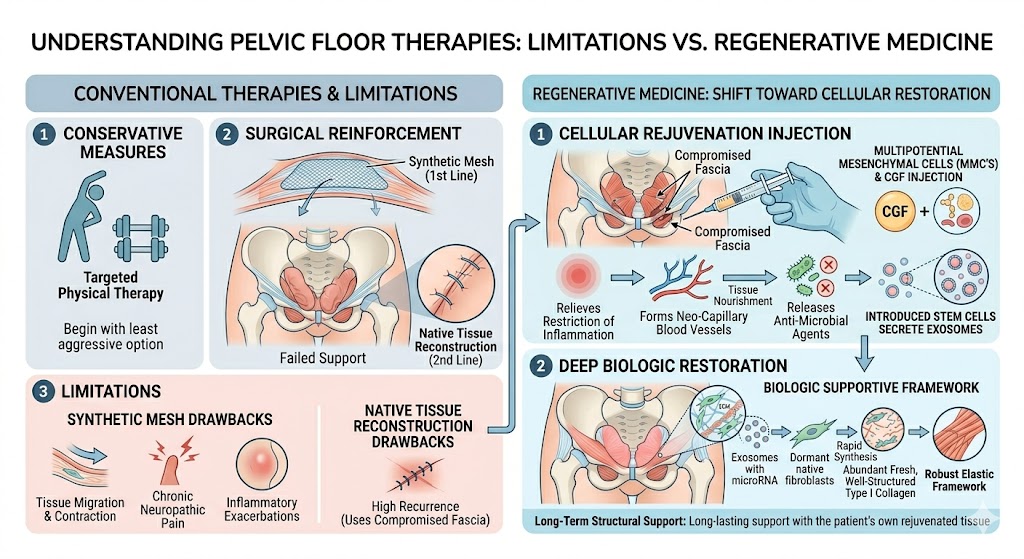
In the medical community, the typical course of action when initiating treatment for Pelvic Floor Repair is to begin with the least aggressive option, such as targeted physical therapy. If the conservative measures do not yield desired results, the first line of defense becomes surgery. When surgeons opt to perform surgery, the first line is mesh synthetics, and the second line used is to perform native tissue reconstruction of the damaged systems. Even with their widespread implementation, all of the traditional methods of reinforcement offer significant drawbacks compared to advances in Regenerative Medicine Thailand. Synthetics of such mesh may encourage migration to the underlying tissues, resulting in the formation of contraction within the tissue, along with the development of chronic, neuropathic pain, and inflammatory exacerbations. The reconstruction of native tissue often depends on compromised fascial planes, resulting in high recurrence. These traditional methods afford rudimentary scaffolding; however, they do not bridge the biologic divide, failing to restore the extracellular matrix.
3. The Shift toward Cellular Restoration
To address the critiques of the current methods, the clinical community must refocus on deep biologic restoration, a standard in Regenerative Medicine Thailand. With the modern Pelvic Floor Repair, in addition to Concentrate Growth Factors, the introduction of MMC’s (multipotential mesenchymal cells) is critical. These biologics change the landscape of the healing response. When injected to the compromised fascia in targeted areas, the cells then begin to heavily engage in cellular signaling that relieves the restriction of inflammation. Additionally, they stimulate the formation of neo-capillary blood vessels to provide nourishment to the previously ischemic tissue, along with the release of anti-microbial agents. Furthermore, the introduced stem cells secrete exosomes packed with regenerative microRNA.
These vesicles lead dormant native fibroblasts toward the rapid synthesis of collagen, ultimately prompting the tissues to lay down an abundance of fresh, well-structured type I collagen fibers essential for proper Pelvic Floor Repair. This process of natural biologic reconstruction replaces the disrupted matrix with a robust elastic supportive framework. By avoiding the use of synthetic scaffolding, this advanced methodology offers the practitioners confidence that the structural reconstructions will exclusively consist of the patient’s rejuvenated tissue. Thus, Regenerative Medicine Thailand in this context provides a unique biological framework for the practitioner to attain the ultimate objectives of long-term structural support.
Figure 2: Conventional inventions compared with Regenerative Medicine in Pelvic Floor Repair
4. Future Prospects Within the Southeast Asian Medical Landscape
Certainly, the future of sophisticated tissue reconstruction appears bright in some of the global healthcare hubs, prominently featuring Regenerative Medicine Thailand. Thailand has become a leading place for innovative medical services. The regulatory environment allows for active participation in advanced clinical research on cellular therapies. These institutes have a steadfast commitment to bioengineering cutting edge laboratories for the creation of high yield, purely therapeutic cellular products. Patients flock to this area because of the available advanced Pelvic Floor Repair surgery that will be prohibited for advanced surgical incorporation in their nations. Members of this medical community have a vast level of knowledge of the art and craft of merging cellular and surgical techniques. The country has a commitment to science, providing new methods for biological reconstruction, and the combination of safety in medicine. The most basic pelvic disorder will still require sophisticated reconstruction solutions beyond mechanical temporary fixes.