Type 2 diabetes is one of the most common metabolic disorders in the world, but it is far more than just high blood sugar. Such as insulin resistance, pancreatic beta-cell dysfunction, chronic low-grade inflammation, oxidative stress and impaired vascular health; abnormal lipid metabolism; long-term metabolic imbalance.
The body still makes insulin, but it does not work as well at first. As time passes, the pancreas may become overworked, beta-cell operate can deteriorate and blood glucose levels may be tougher to control. This is the reason type 2 diabetes can damage many organs, including heart, kidneys, nerves, eyes, blood vessels and liver and immune system.
Due to this complexity, increasing number of patients is looking for other supportive solutions like UC-MSC Thailand, stem cell for type 2 diabetes and type 2 diabetes treatment through regenerative medicine. The increasing interest is certainly warranted, in particular for patients that are motivated to support their metabolic health, mitigate inflammation, enhance quality of life and long-term management of risk.
Nonetheless, UC-MSCs should not be introduced as a miracle cure for type 2 diabetes or a substitute for conventional medical care. Instead, a responsible discussion will centered upon science, safety, metabolic monitoring, and reasonable expectations.
UC-MSC Thailand: Discussed For Your Type 2 Diabetes
Umbilical cord-derived mesenchymal stem/stromal cells (UC-MSCs) have been a target of much inquiry in the field of regenerative medicine due to their properties as a source of biological signaling. These cells can secrete bioactive substances, affecting various processes such as immune function, inflammation, oxidative stress and tissue repair signaling vascular functions or crosstalk with different cell types.
In type 2 diabetes treatment, the science is much more focused than merely lowering blood sugar rapidly. Researchers are investigating the potential role of UC-MSCs in restoring a healthier metabolic milieu by modulating pathways associated with inflammation, mechanisms related to insulin resistance, pancreatic stress and vascular repair signaling.
The term UC-MSC Thailand became more apparent because of medical travel, hospital-based care, wellness medicine international patient coordination and laboratory-supported regenerative programs. International patients may be lured by Thailand because of its provision of advanced medical services within an organized and structured framework for patient support.
What UC-MSCs, may do with Type 2 Diabetes Research
UC-MSCs and there is no focused study on UC-MSCs repopulating or directly “becoming a new pancreas.” The more scientific explanation is related to paracrine signaling. Consequently, UC-MSCs can secrete growth factors, cytokines, extracellular vesicles and other bioactive molecules that interact with surrounding cells and tissues.
In studies regarding type 2 diabetes, the mechanisms triggered by UC-MSC are being studies related to their possible impact on:
Inflammatory balance
Insulin resistance pathways
Beta-cell stress reduction
Oxidative stress regulation
Vascular and endothelial support
Tissue repair signaling
Pancreatic microenvironment support
Immune-metabolic communication
Type 2 diabetes, as a condition highly associated with chronic inflammation and malfunctioning metabolic mechanisms, is particularly biologically interesting mechanism across these actions. All of these mechanisms eventually lead to disease progression, stemming from excess visceral fat and the resulting other conditions including impaired mitochondrial function, cytokines/insulin resistance, inflammatory cytokines/endothelial dysfunction/oxidative stress.
Should UC-MSCs contribute to the modulation of biological environment, they might be incorporated into a larger supportive approach in favored patients. But this does not imply that UC-MSCs are already validated standard therapy for type 2 diabetes. The field remains in its infancy, and much needs to be cautiously assessed for clinical translation.
What Must Be Evaluated Prior to Considering UC-MSCs
Important assessments may include:
Fasting blood glucose
HbA1c
Fasting insulin
C-peptide
Lipid profile
Kidney function
Liver function
Inflammatory markers
Urine microalbumin
Blood pressure
Body composition
Medication history
Diabetes duration
Neuropathy or retinopathy assessment
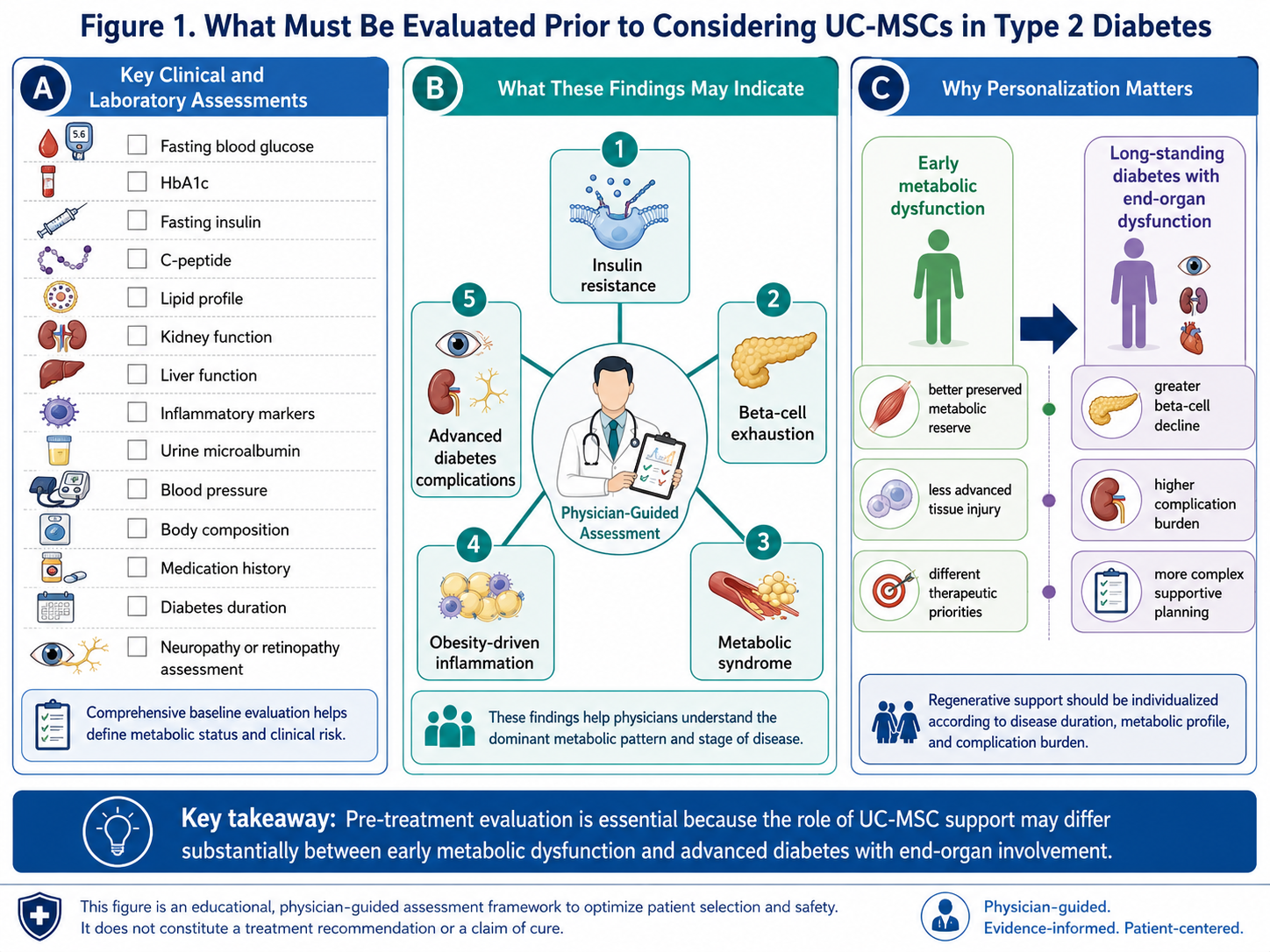
These tests largely convey to physicians if the patient primarily has insulin resistance, beta-cell exhaustion (from long-standing hyperglycemia), metabolic syndrome, obesity-driven inflammation or advanced complications of DM.
Regenerative support should be targeted, and this is important. For example, what UC-MSC might say to a patient with early metabolic dysfunction may differ sharply from that in the presence of long-standing diabetes associated with advanced end-organ dysfunction.
Figure 1: Clinical and laboratory evaluation prior to UC-MSC consideration in type 2 diabetes. Comprehensive baseline assessment may help define disease stage, metabolic phenotype, beta-cell reserve, complication burden, and the suitability of individualized regenerative support.
UC-MSC Thailand as an Enabling Rejuvenative Program
The UC-MSC Thailand program for type 2 diabetes can be positioned as supportive care in a more extensive metabolic health plan. It should not be considered a substitute for medication, nutrition, exercise, glucose monitoring or endocrinology follow-up.
An example of a medically guided framework could appear as follows:
Assessment – Metabolic Staging – Medical Optimization – UC-MSC Supportive Program- Lifestyle Intervention- Monitoring and Follow Up
This framework is more biologically rational than applying UC-MSCs as a monotherapy. By addressing glucose control with combined methods of diet, exercise, weight loss (IF overweight), sleep management, stress reduction, medication if necessary, and monitoring tools together WITH vascular risk factors; T2D is best managed most safely.
In some instances, patients can be offered regenerative medicine as an adjunct service. However, the core of care should continue to be long-term metabolic management and physician-led surveillance.
A Different Way to Describe the End Result
This indelibly makes it difficult to describe the role of UC-MSCs in type 2 diabetes as there is no definition for what curing diabetes or stopping medication would mean. A more scholar-esque explanation would be:
UC-MSCs have been evaluated in selected patients as a potentially supportive regenerative strategy that may modulate inflammatory balance, insulin-resistance-associated pathways, vascular function, tissue repair signaling and pancreatic microenvironment support.
This verbiage is also more medically responsible and would be more believable to potential patients from outside the USA who are doing their research online as UC-MSC Thailand, stem cell for type 2 diabetes and type 2 diabetes treatment.
Conclusion
Regenerative medicine has emerged as a growing area of research for UC-MSC Thailand and the treatment of type 2 diabetes. First, it is easy to understand the interest, for type 2 diabetes is far more than a chronic elevation of blood glucose. This involves inflammation, insulin resistance, oxidative stress, vascular dysfunction, beta-cell stress and progressive metabolic disorder.
UC-MSCs have been investigated due to their possible immunomodulatory, anti-inflammatory, vascular-supportive, and tissue-messaging roles. Such mechanisms might be applicable in type 2 diabetes, particularly with the objective to support a healthy metabolic milieu.
On the contrary, UC-MSCs should not be represented as a panacea option or substitute for standard diabetes treatment. Careful diagnosis, metabolic evaluation, physician supervision, quality control in laboratories, optimal lifestyle and long-term follow-up are the most responsible alternatives.
Modern day regenerative medicine relies on genuine science to build trust. In the care strategy for patients exploring stem cell type 2 diabetes or UC-MSC Thailand, the best regime is not one with rapid claims but qualities of safety of therapeutically feasible levels to de-risk metabolic improvement and realistic health expectations.