Lung disease can harm your breathing, energy levels, oxygen exchange process, sleep cycle and daily activities. Diseases like COPD, pulmonary fibrosis, chronic inflammatory lung disease, post-infection lung injury and acute respiratory distress syndrome (ARDS) could also be marked by inflammation, immune imbalance, oxidative stress and destruction/ damage of sensitive lung tissue. Because of this, more patients are wanting to explore stem cell therapy for lung disease as an adjunctive treatment with standard pulmonary care.
In this context, most studies were focused on mesenchymal stem cell — also known as MSCs. The key point, however, is that MSCs are not primarily effective because of the fact they “turn into new lung cells.” Rather, their worth is connected to how they signal the body biologically. MSCs as having immunomodulatory, anti-inflammatory, paracrine and tissue-supporting properties which may be important in research relevant to the lung.
Mechanism of Stem Cell Therapy for Lung Disease
Paracrine signaling is thought to be the principal mechanism of stem cell therapy for lung disease. That is, MSCs secrete beneficial biological factors including cytokines, growth factors, extracellular vesicles and other signaling molecules. These signals could potentially affect neighboring immune cells, inflammatory pathways and tissue-repair responses. Instead of replacing tissue damaged in the lungs, MSCs may support homeostasis for repair and regeneration.
Anti-Inflammatory Support
Chronic inflammation appears to be a prominent theme in many lung diseases. Chronitis airway inflammation leading to cough, breathlessness and mucus is a common symptom in COPD patients which contributes to progressive airflow limitation, for example. In Pulmonary fibrosis, repeated bouts of injury and aberrant repair could induce scarring. Due to their potential contributions to mitigate the hyper-inflammatory signaling pathway and more tolerogenic immune milieu, MSCs are currently being evaluated.
Immune Modulation
It is essential for non-specific immune modulation. MSCs can interact with various immune cells including macrophages, T cells, and other inflammatory cells. MSC, they also play a role in changing immune activity from an inflammatory to a regenerative one. This is of particular importance to lung disease where uncontrolled immune activation can exacerbate tissue injury and make recovery more difficult.
Stem Cell Therapy for Lung Disease
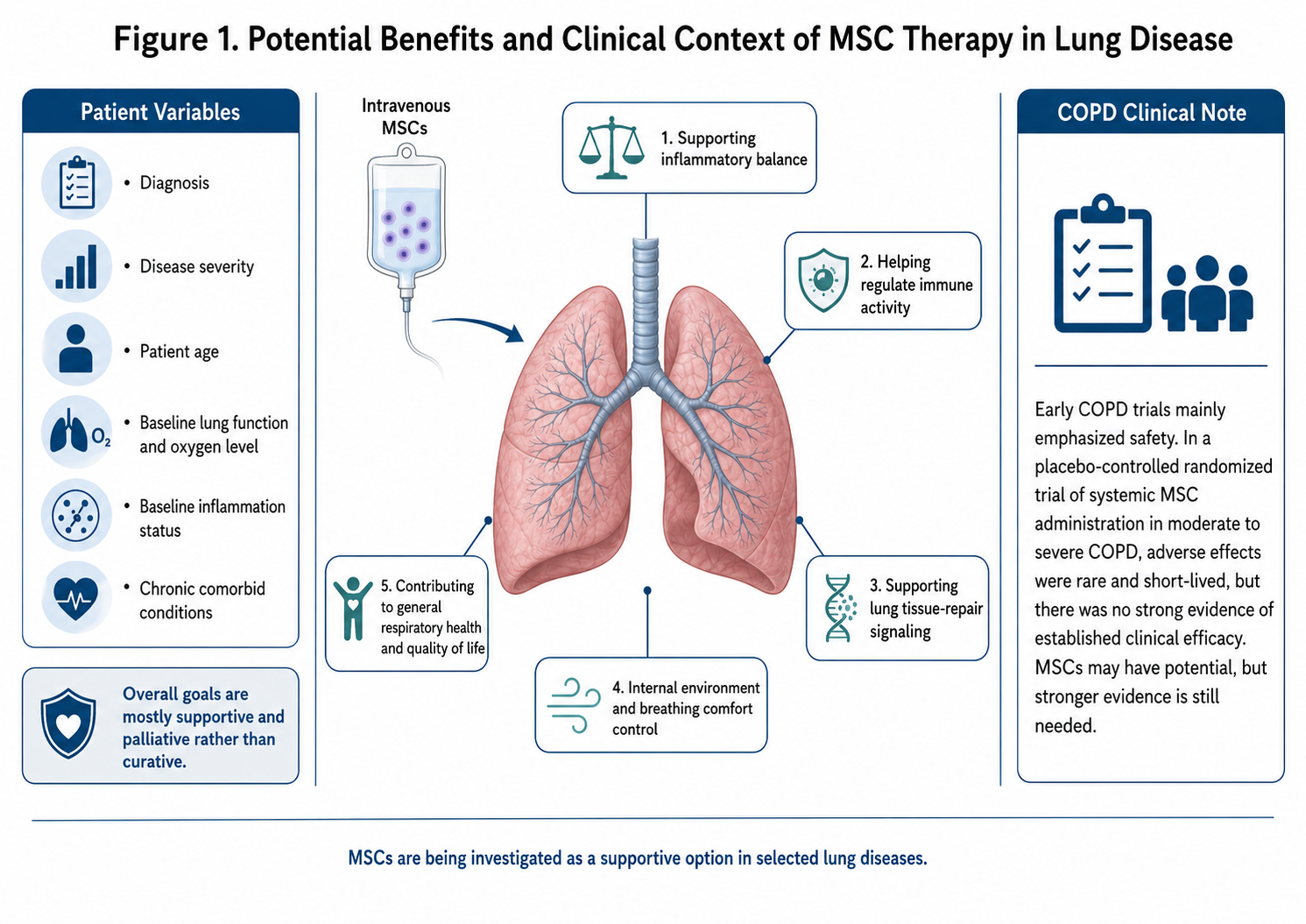
Stem cell therapy can offer potential benefits for lung disease in patients based on the following variables: diagnosis, disease severity, patient age, baseline lung function and oxygen level as well as levels of inflammation present at baseline and any other chronic comorbid conditions. These are mostly palliative aims instead of curative in general.
Potential benefits may include:
Supporting inflammatory balance
Helping regulate immune activity
Supporting lung tissue-repair signaling
Internal Environment and Breathing Comfort Control
Contributing to general respiratory health and life quality
For COPD, initial trials have emphasized safety. In patients with moderate to severe COPD receiving systemic MSC in a placebo-controlled randomized trial, adverse effects were rare and short-lived and there was no strong evidence for any established clinical efficacy. That means MSCs could have potential, but perhaps we ought not get carried away until the science catches up.
Figure 1: Clinical Context and Supportive Role of MSC Therapy in Lung Disease
Due to the severe inflammatory nature of ARDS and the injury of lung barrier function, studies and reviews have examined MSCs for ARDS. Although meta-analyses and clinical reviews suggest potentially promising safety signals and efficacy for MSC-based approaches, the level of evidence is limited, thus larger studies are still needed to provide definitive confirmation.
Studies on MSC for pulmonary fibrosis are still in the early stages. Pulmonary fibrosis is marked by abnormal scarring with stiff, less flexible lungs. Although the anti-inflammatory and anti-fibrotic potential of MSCs has attracted considerable attention, this is yet largely untested clinically.
Who Can Apply For This Supportive Program?
When an alternative adjunctive management option may be appropriate for some patients with chronic or inflammatory lung conditions, a stem cell therapy for lung disease program. This could be an appropriate option for patients already in pulmonary specialist care seeking advanced regenerative support in a medically supervised environment.
Patients need to be adequately assessed prior to treatment. Relevant data would include lung function tests, CT scans, oxygen saturation, inflammatory markers, medication history and status on infection, smoking history, and medical condition.
Important Medical Note
Stem cell therapy for lung disease should never be advertised as a cure or alternative to conventional treatment. Patients with COPD, pulmonary fibrosis, asthma, a history of ARDS or other lung condition should maintain appropriate follow up care with their pulmonologist. Conventional therapies (i.e., inhalers, oxygen therapy, pulmonary rehabilitation, anti-fibrotics, infection control and lifestyle management) continue to play a critical role.
Conclusion
Stem cell therapy for lung disease is an evolving supportive strategy that aims to restore immune equilibrium, serve as vehicles for anti-inflammatory signaling, promote paracrine communication and provide structural support to the tissue during repair. MSCs are likely to carry benefit in selected patients where there is important inflammation/immune dysregulation. That said, such evidence is still emerging & outcomes can differ from patient to patient
Ideally, how the stem cells can benefit you should be part of a medical care that involves diagnosis and evaluation by your doctor, realistic expectations about outcomes which are not based on anecdotal information alone, and is coupled with continued standard lung care.