Hepatitis causes a wide range of devastating effects on a patient’s health and is associated with a high risk of death. This complication can be caused by a gradual assault on the body’s ability to maintain homeostasis via injury to the hepatic microenvironment. This injury, often the result of an infection from microbes or from the introduction of foreign chemicals to the body, can severely impact the health of a patient, resulting in severe fatigue, a risk of uncontrollable bleeding, and an increased risk of infection due to the damage to the immune system. The deterioration of health caused by this injury is an affront to a patient’s dignity. There remains a dismal prognosis for patients even with all of the advances in medicine due to the intractable nature of this injury, which is driven by a high rate of cellular death. Unfortunately, the damage caused to a patient’s health by this injury demonstrates a sharp decrease in the ability and likelihood of restoration of a patient’s health via the administration of pharmaceutical interventions. There is a vitally important loss of the ability to restore a patient’s health from all partial organ failure via the administration of advanced stem cell interventions, such as UC-MSCs, that can be used as a last resort in an emergency to restore a patient’s health from severe hepatic injury.
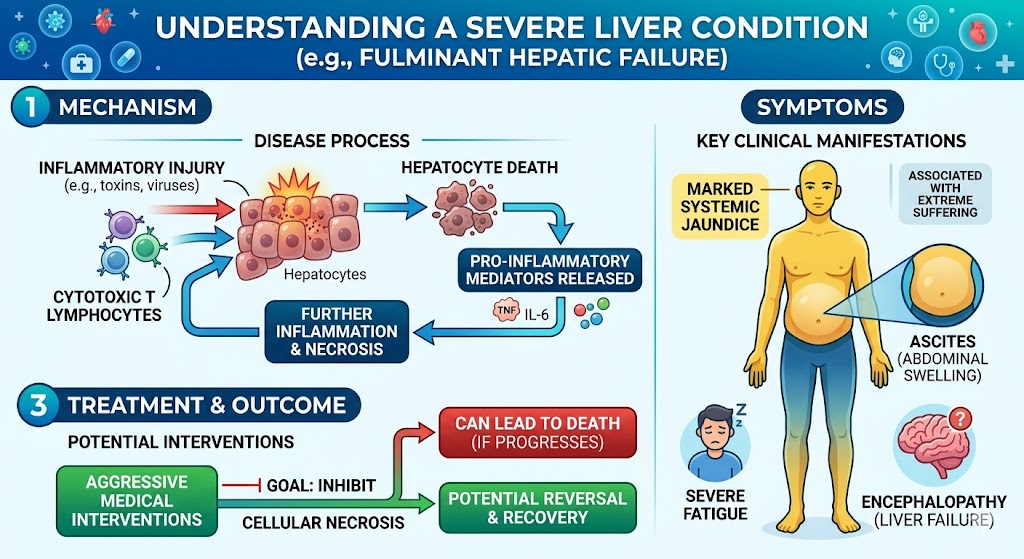
The mechanism of this condition includes the death of hepatocytes initiated by the cytotoxic T lymphocytes recruited following inflammatory injury to the cells. This leads the body to secrete pro inflammatory mediators furthering inflammation and necrosis. The condition manifests in the body as marked systemic jaundice together with large swelling of the abdomen due to presence of ascitic fluid, marked fatigue, and encephalopathy due to liver failure. This condition is associated with extreme suffering and can lead to death due to the suffering and can potentially be reversed by aggressive medical interventions to inhibit the progress of cellular necrosis.
Figure 1: The mechanism of Hepatitis
Proposed Therapeutic Mechanisms of Stem cell Therapy via UC-MSCs
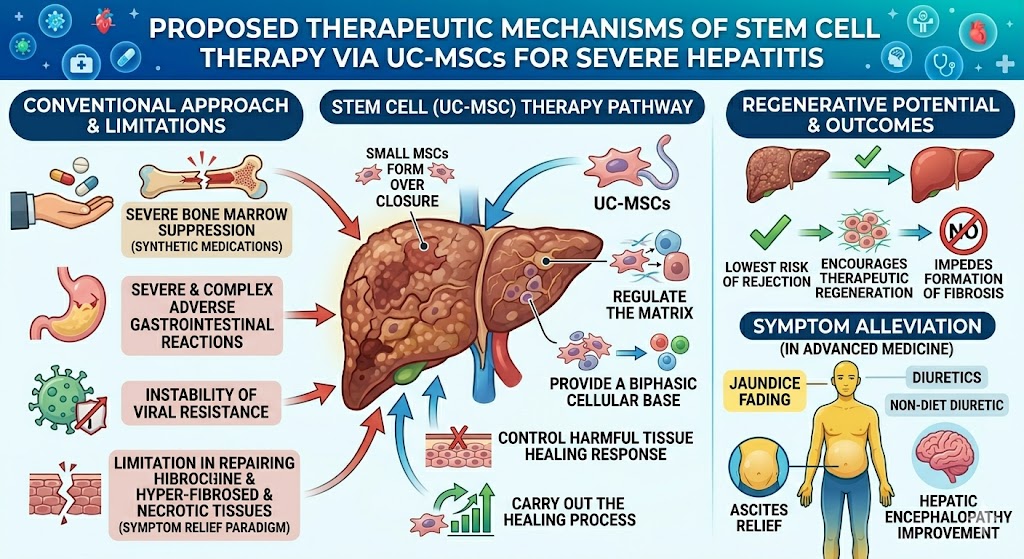
Severe hepatitis can be treated by several conventional medical therapies and advanced pharmaceuticals, including the use of immunomodulators and restorative stem cell therapy. The advanced UC-MSCs treatment methods proposed here can potentially be used to treat severe hepatitis, where function loss has caused the organ to transition to the next stage of deterioration. Medical practitioners use various methods to impede the process of viral replication and help to reduce tissue damage associated with inflammation and auto-immunity. In advanced medicine, removal of dangerous sequelae of the condition, such as ascites and hepatic encephalopathy, is treated through the use of powerful diuretics and a strict non-diet diuretic. Current treatment methods impose significant constraints. Considering the clinical therapies, severe bone marrow suppression associated with synthetic medications is also the result of a severe and complex adverse gastrointestinal reaction. The instability of viral resistance is a major clinical concern. Classical medical therapies for this condition primarily focus on the use of a symptom relief paradigm and are limited in their ability to address the biological build up associated with the repair and restoration of hyper fibrosed and necrotic tissues and organs to counter the process of hyper fibrosis affecting the organ necrosis and tissues.
The greatest difficulty facing modern medicine lies in the support for the development of regenerative medicine. The mainly approach of the modern scientists is the adoption of renal target stem cell therapy. Among all biological options, isolated UC-MSCs pose the lowest risk of rejection, while providing the best therapy for hepatitis. These structures can form a closure with the ability to regulate the matrix and carry out the healing process. At the tissue level, they provide a biphasic cellular base, while controlling the harmful tissue healing response. These biological structures work the matrix healing the ailing response. Through the utilization of these cellular constructs, the healing response of the tissue is enhanced and the ailing response of the tissue is significantly decreased. This methodology encourages the therapeutic regeneration of organs and impedes the formation of fibrosis.
Figure 2: Proposed Therapeutic Mechanisms of Stem cell Therapy via UC-MSCs
Future Trends Thailand
This new advanced stem cell technology of medicine is being directed to Southeast Asia. Thailand is one of the new leading countries in the development of this UC-MSCs protocol for regenerative medicine. The country is working with world class biomedical research and high specialized medical training. Thailand’s law is a mixture of therapy law and clinical trials of protective law, directed for medical tourism. With these features, this country will be at the forefront of the world to treat acute hepatitis.
Steady deterioration of liver function is a serious, life-threatening condition in hepatitis, and the decline in liver function exacerbates the decline of other systems in the body. Furthermore, virtually no current pharmaceutical therapies are beneficial, and in fact are more of a placebo with respect to the other systems. The incorporation of UC-MSCs into standard stem cell medical practice will help to restore not only liver function but also the damaging inflammation associated with it. The further advancement in medical science makes this protocol even more applicable. The South Eastern Countries are the forerunners in the application of this protocol and therefore the rest of the World will follow to address severe hepatic failure.