Stroke is a common cause of permanent disability and mortality throughout the world. Millions of individuals remain with a major functional deficit following neurovascular insults. Lives are drastically changed, and families disrupted due to the sudden changes caused by the loss of the neurovascular supply to the brain. For nearly all patients, the psychological impact and loss of motor skills, and frequently loss of the ability to communicate, are the most devastating effects of the disease. Moreover, the society incurs a great deal of economic impact associated with the need for long-term rehabilitation of affected individuals. It is of high importance that therapeutic interventions for the rehabilitation of patients help them to be more independent. Mainstream medicine is challenged by the aim of completely reversing established disability. It suggests that the rehabilitation of patients with stroke is a goal of high priority. It is the best available of effective treatments in the area of stroke rehabilitation. To accomplish meaningful Stroke Recovery, Stem Cell-driven brain reconstruction must occur. Most of restoration of brain reconstruction must occur deep in the restorative brain rehabilitation mechanisms.
1. Stroke Disease Mechanisms
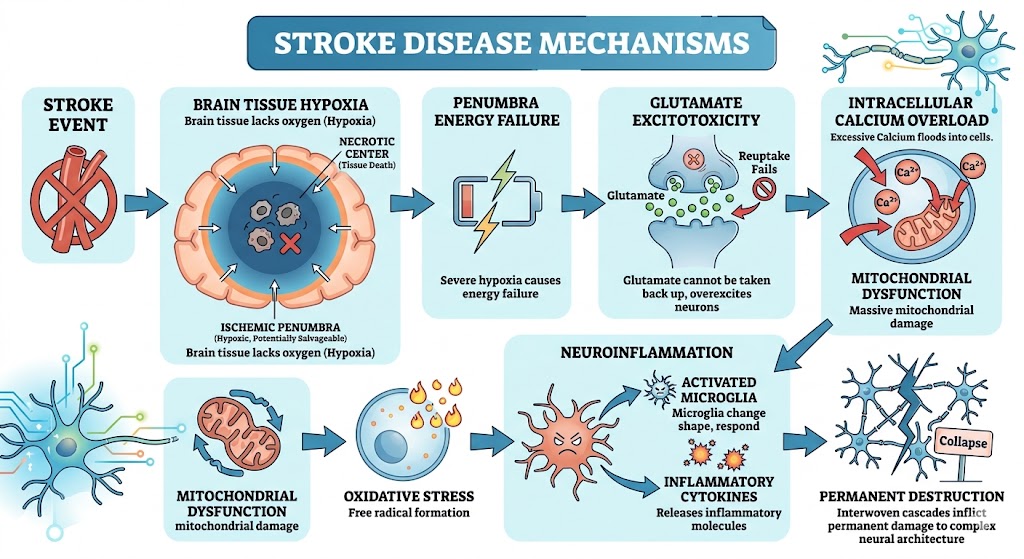
Brain tissue undergo necrosis due to hypoxia. In addition to leading to a rapid demise of cells in brain tissue, hypoxia creates a necrotic center of the brain surrounded by a penumbra. The tissue in the penumbra is called the ischemic penumbra, and while still hypoxic, it is salvageable. Severe hypoxia in the penumbra creates an energy failure, which causes the excitatory neurotransmitter, glutamate, to fail to be taken back up by neurons. Thus, the glutamate remains in the synaptic cleft and causes an excitotoxic response. This excitotoxic response causes massive mitochondrial dysfunction due to intracellular calcium overload. Rapid neuroinflammation follows due to oxidative stress associated with neuroinflammation. The microglia are activated in the brain and in turn release inflammatory cytokines. These interwoven destruction cascades inflict permanent destruction of the intricate neural architectures. During acute interventions, preservation of the penumbra is the most important priority to maximize later potential for Stroke Recovery and future Stem Cell treatments.
Figure 1: Stroke Disease Mechanisms
2.Standard Methods of Treatment and Their Natural Limits
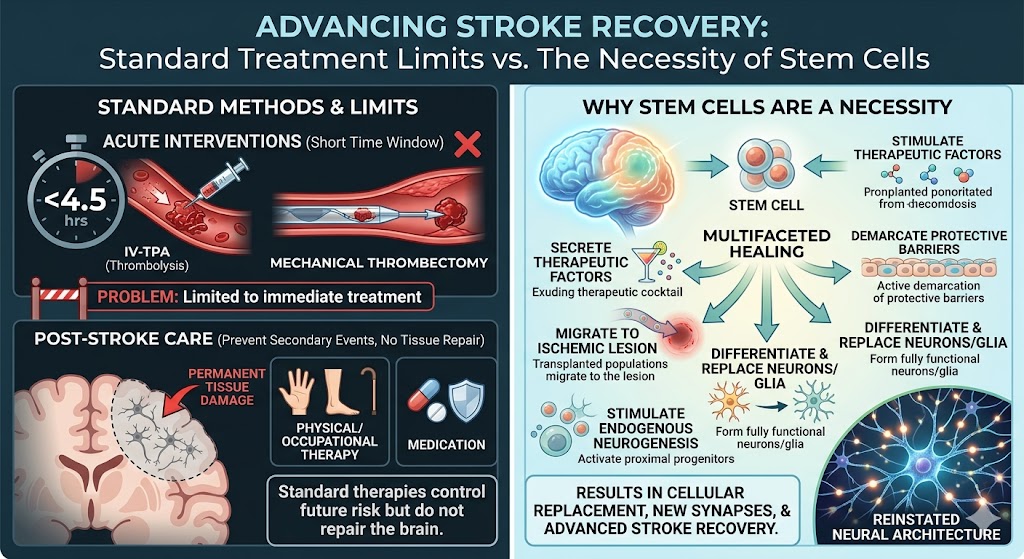
The priority in today’s clinical world is rapid reperfusion. Typically, the first action of physicians is to administer the intravenous tissue plasminogen activator to clear the occlusive thrombus. There is also mechanical thrombectomy to retrieve the thrombus that caused the arterial blockage. However, the acute interventions have a very short therapeutic time. Treatment must be given within hours of symptom onset. Patients in the majority of instances do not arrive early enough for the first stage of treatment. In the acute phase of Stroke Recovery, blockade of patient care is a continuum of physical therapy and occupational therapy. There is also a continuum of medication prescribing which is meant to prevent a secondary event rather than repair the dead tissue. Clearly the standard techniques of therapy can control further occurrences but they do not repair the tissue, and there is no possibility of completing the repair of the lost neural structures with the commensurate gap without Stem Cell assistance.
3. Why Stem Cells are a Necessity
For the first time addressing a partial Stem Cell loss of the neural tissues supports reparative processes. The healing is Stem Cell-based and is multifaceted but at the very least must be sophisticated. To put it in a simplistic way: the repair cell, induced to participate in the healing process, supports numerous cellular constructs thus exuding a cocktail of therapeutic factors to the site of injury. This also allows for the repair cell to be free to alter the injury state by supporting neural repair through the active demarcation of protective barriers. The locks on the blood barriers have been opened. Beyond supportive secretions, Stem Cells have remarkable plasticity. Transplanted populations can migrate directly to the ischemic lesion through various local inflammatory signals. After traveling to the site of injury, Stem Cells can differentiate into fully functional neurons or glial cells. This mechanism replaces missing elements in the disrupted neural pathway. They also catalyze neurogenesis, activating proximal progenitors in the brain. This multifactorial method conveniently stimulates the brain in its repair capacities. As a result, cellular replacement, in conjunction with stimulating endogenous neurogenesis, diminishes secondary damage and promotes advanced Stroke Recovery through the formation of new synapses.
Figure 2: Advancing Stroke Recovery with Stem Cell
4. Future Trends in Medical Research in Thailand
There are many dynamic sectors in Thailand’s healthcare system, with the potential to develop rapidly, especially regenerative medicine. Thailand has married its developing healthcare system with world-class model affordable care to the patient. Thailand has an integrated healthcare system with developed and progressive frameworks for the protection of the patient and optimally controlled clinical research. This has fueled the rapidly evolving assisted reproductive therapy where a geared Stem Cell is available in the system for advanced therapy. The evolving intermediate level of private healthcare in the country is integrating with bilateral research and advanced technology healthcare, world class in affordable care that is caring and not paternalistic, with the country’s treasure, a rich clinical database and highly diversified people. Advanced research in the country is promising and offers the perfect model for innovating Stroke Recovery therapy.