Ulcerative colitis is a chronic inflammatory bowel disease that is limited to the colon and the rectum. Clinical feature include regrowth of intestinal mucosa, rectal bleeding, diarrhea, abdominal pain/discomfort, fatigue and weight loss. It has also a relapsing disease course with flare and remission. Ulcerative colitis can have a substantial negative impact on health related quality of life, psychological status, nutritional state, work productivity and long-term health in many patients.
Its not a simple digestve issue. In idiopathic UC-MSCs, development probably depends on a combination of genetic susceptibility, immune dysregulation, epithelial barrier dysfunction and imbalance in gut microbiota along with environmental factors. For this reason, managing those with ulcerative colitis typically involves long-term medical supervision and treatment planning.
In recent years, UC-MSCs (umbilical cord-derived mesenchymal stromal/stem cells) have received considerable interest as an adjunctive regenerative medicine approach. Characterization of the UC-MSCs showed their immunomodulatory, anti-inflammatory, paracrine and tissue-supportive properties. Their application in ulcerative colitis, however, must be addressed cautiously. UC-MSCs should not be presented as an absolute cure or replacement of standard gastroenterology treatment. It is more scientifically accurate to state that UC-MSCs may be investigated as a supportive and investigational strategy in selected ulcerative colitis treatment regimens.
Disease Mechanism: Understanding Ulcerative Colitis
Ulcerative colitis: it is characterized by persistent inflammation of the colonic mucosa, whose pathophysiology is unclear. Ulcerative colitis starts in the rectum and continuously affects the colon to different degrees, unlike the transmural inflammation of Crohn’s disease throughout any part of the GI tract.
At a tissue level, ulcerative colitis is characterized by loss of epithelial barrier integrity, immune cell infiltration and inflammatory cytokine release, and distortion of crypt structure along with mucosal ulceration and inadequate recovery of the intestinal lining. The mucosa becomes inflamed and eroded, during disease activity results in symptoms including bloody diarrhea, urgency, abdominal cramping, mucus discharge and fatigue.
At the heart of this process is the immune system. And rather than balancing how it interacts with the gut microbiota and the intestinal lining, its immune response goes awry. This can give rise to continuous signalling of the inflammation, damage to epithelium and malfunction in mucosal healing. Frequent episodes of inflammation, over time may lead to structural and functional changes in the colonic area.
Chronic ulcerative colitis may predispose patients to complications such as anemia, malnutrition, acute severe colitis requiring hospitalization, and in select patients with extensive longstanding bowel involvement an increase risk of colorectal cancer. Hence, the long-term treatment of IBD must include effective disease control and surveillance to ensure mucosal healing as well as appropriate gastroenterology follow-up in order to monitor for early detection of signs of dysplasia.
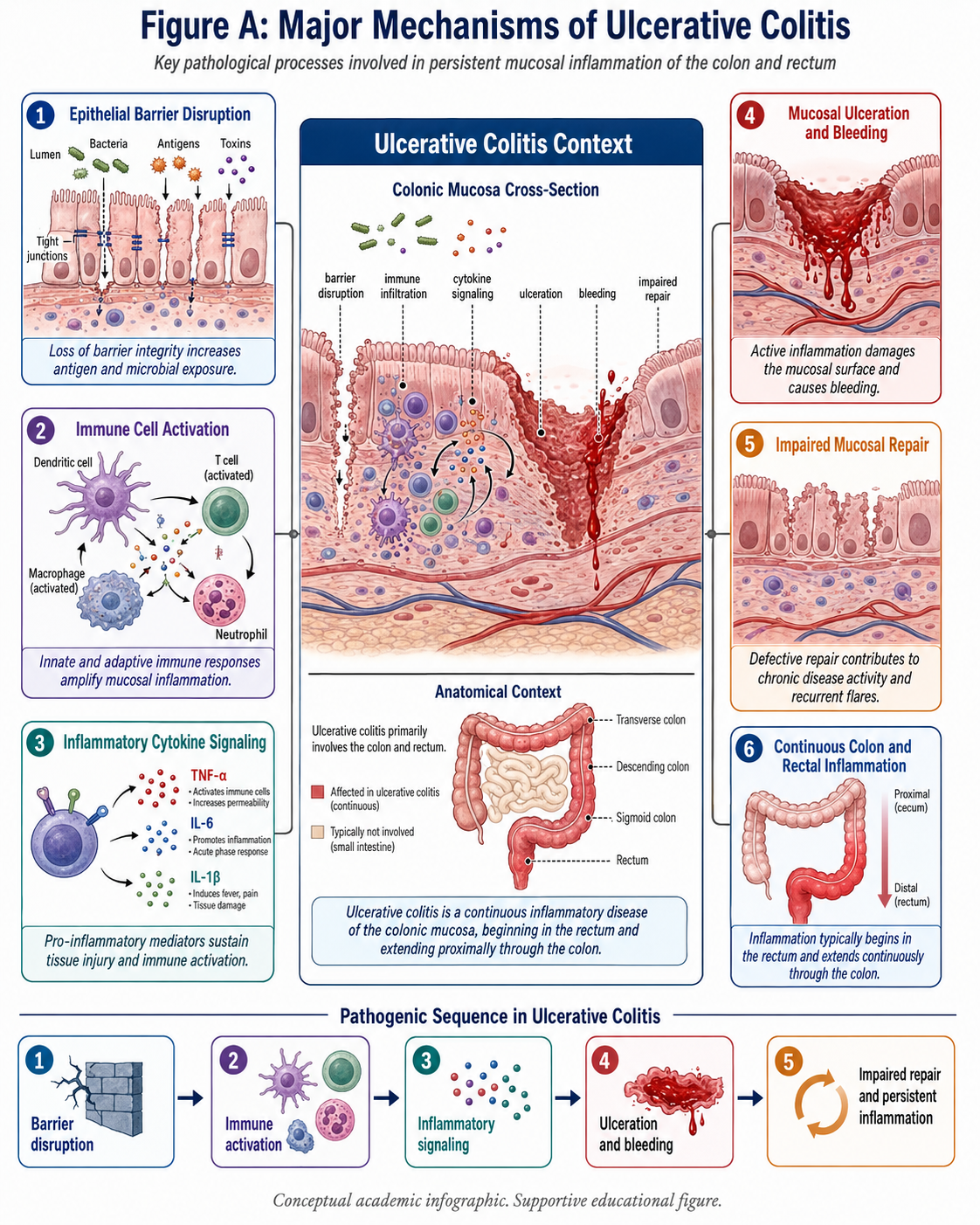
Figure A: Major Mechanisms of Ulcerative Colitis, This figure depicts the key mechanisms in ulcerative colitis: epithelial barrier disruption, immune cell activation, inflammatory cytokine signaling, mucosal ulceration and bleeding at inflamed sites and impaired mucosal repair leading to continuous inflammation of colon and rectum.
Conventional Ulcerative Colitis Treatments
New treatments for the treatment of ulcerative colitis aim at reducing inflammation and inducing, maintaining remission while preventing complications and improving quality-of-life. Selection of treatment is based on severity, extent of disease, previous response to treatment, age and comorbidities the patient has, dose tolerability, as well as risk of relapse.
Common treatment categories include:
2.1 Aminosalicylates
Aminosalicylates are the most used for mild and moderate ulcerative colitis. They work to decrease inflammation in the colonic mucosa and can be used orally, rectally or a combination based on where disease is.
2.2 Corticosteroids
Corticosteroids for short-term management of moderate to severe flares. Although these agents may be appropriate for short-term treatment, they are not suitable for chronic maintenance due to associations with metabolic effects and potential damage including, but not limited to infection risk, opportunistic infections (eg local infection), adrenal suppression, and bone loss.
2.3 Immunomodulators
Immunomodulatory drugs may also be employed in selected cases to help temper immune activity and maintain disease control. They involve well-monitored drugs with significant effects on the immune system, liver function, blood counts and infection risk.
2.4 Biologic and Targeted Therapies
The treatment landscape for ulcerative colitis has expanded with the introduction of biologic therapies and small-molecule targeted treatments. These therapies may act on inflammatory pathways including TNF-α, integrins, interleukin signalling or even intracellular immune-pathways. These are effective in moderate to severe disease, but not all patients. So some patients will need to lose response, suffer from side effects or not reach complete remission.
2.5 Surgery
In cases of severe and/or refractory or complicated ulcerative colitis, surgery can be necessary. Colectomy for; removal of the pathologic colon is a life-sparing but complex intervention with significant long-term implications.
Conventional uc treatments remain the bedrock of care. Unfortunately, despite these new advances in therapy some patients still experience unremitting symptoms, incomplete mucosal healing, treatment refractoriness or recurrent flares. This has prompted interest in adjunctive strategies which promote immune homeostasis, tissue remodelling and mucosal repair.
Scientific position of UC-MSCs in Ulcerative Colitis
Umbilical cord-derived mesenchymal stromal/stem cells (UC-MSCs) have been investigated in regenerative medicine due to their secretion of diverse bioactive molecules like cytokines, growth factors, extracellular vesicles, and other paracrine signaling factors. These signals act is gonna cross talk with immune cells, endothelial cells-it could be epithelial cell as well and also induce tissue repair pathways.
Finally, in relation of UC-MSC and therapies in ulcerative colitis, here we are not trying to define a cell for use as directly replacing the lost or damaged intestine. Instead, ways in which they might be relevant are usually discussed via a number of putative mechanisms:
Immunomodulatory signaling
Anti-inflammatory communication
Regulation of cytokine activity
Support for epithelial barrier function
Paracrine signaling through extracellular vesicles
Enhancement Of A Better Mucosal Healing Environment
Interaction with local immune and repair pathways
That is, UC-MSCs must be pitched as a complementary biological approach and not the panacea. The scientific rationale is that patients with ulcerative colitis are known to have immune dysregulation and impaired mucosal repair, and UC-MSCs may affect the inflammatory microenvironment in selectively chosen patients.
Proposed Mechanisms of UC-MSCs in Ulcerative Colitis
4.1 Immune Regulation
A central feature in the characterization of UC-MSCs is their ability to modulate immunity. Immune activity in the intestinal mucosa becomes excessive and prolonged in ulcerative colitis. UC-MSCs may exert immunomodulatory effects on immune cells, which, in turn, are associated with a more balanced immune response. This does not tell us that UC-MSCs switch the disease off. So, the real academic statement looks like:
Under medically supervised treatment conditions, UC-MSCs may positively augment immune regulation by regulating the activation of effector cells and modulating cytokines signalling pathways.
4.2 Anti-Inflammatory Signaling
Ulcerative colitis: Inflammation and immune mediated tissue destruction related to characteristic cytokines. A promising option lies in the use of UC-MSCs which are known to release anti-inflammatory and regulatory signals that potentially limit excessive inflammatory conversation.
This mechanism is important because prolonged inflammatory responses can lead to impaired healing of the protective mucosal lining and persistent symptoms. Nevertheless, the influence of UC-MSCs is determined potentially by disease severity, route of administration, cell quality, dose and patient biology as well as concomitant medical treatment.
4.3 Backup of the Epithelial Defense
Two features that you can see on your own screens are peripheral endothelial cells and long-lived intestinal epithelial (IE) renewal. This protective barrier can be compromised in ulcerative colitis, leading to enhanced immune exposure and inflammatory activation.
Lineage via paracrine signaling and cell-to-cell contact with local tissue cells may support UC-MSCs in the repair of barrier functions. This notion is significant given that mucosal healing is one of the main objectives in contemporary management of ulcerative colitis.
4.4 Paracrine and Signaling from Extracellular Vesicles
The paracrine effect of UC-MSCs are well characterised. Instead of directly becoming intestinal cells, they perhaps secrete vesicles and soluble factors that communicate with neighbouring or distant cells. Such signals potentially play a role in immune regulation, tissue support, vascular homeostasis, and cellular repair responses.
In academic wording:
The role of UC-MSCs in ulcerative colitis may be related less to cell replacement and more towards the signaling-based modulation of both the inflammatory and mucosal repairing microenvironment.
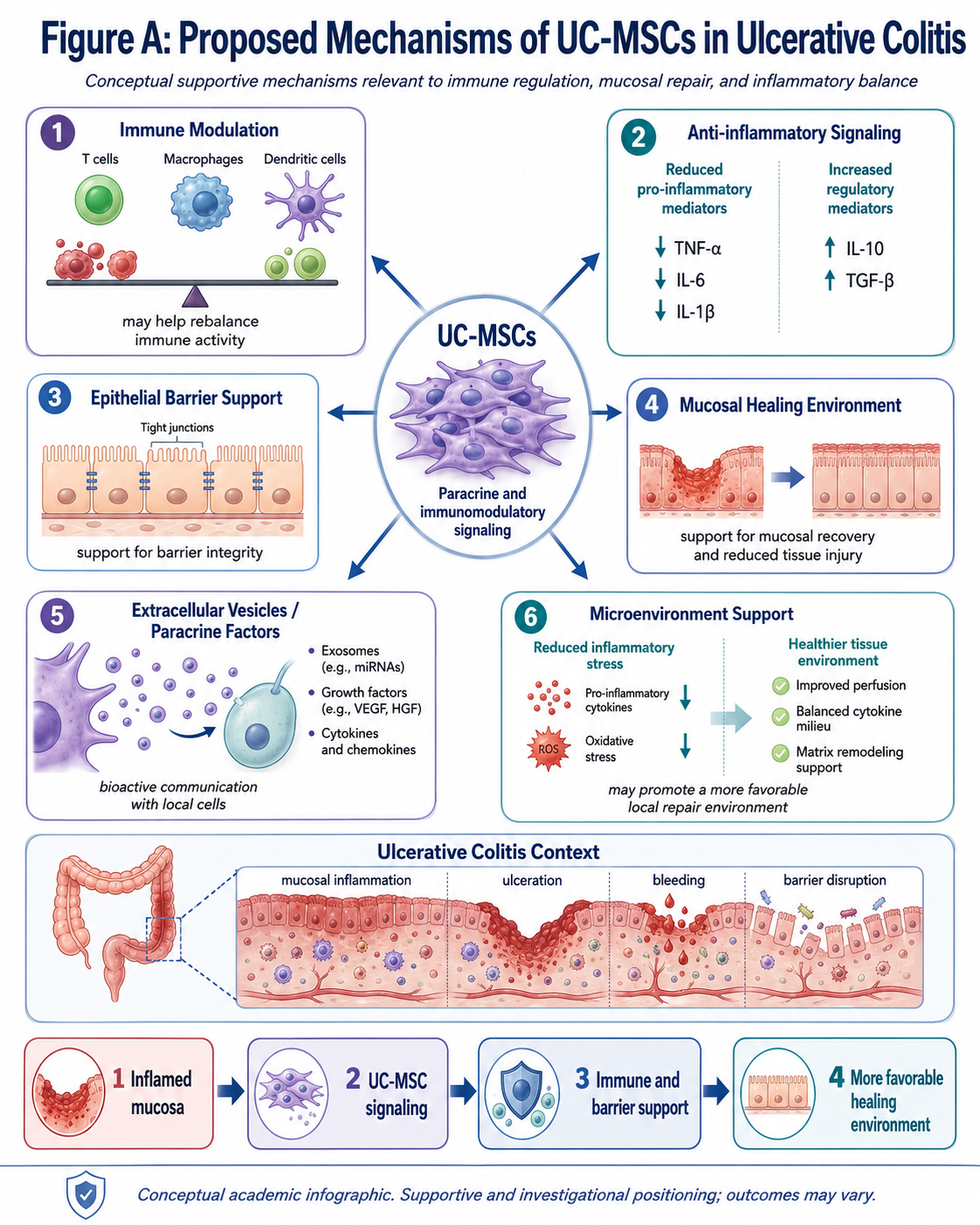
Figure B: Proposed Mechanisms of UC-MSCs in Ulcerative Colitis
This figure summarizes the proposed biological actions of UC-MSCs in ulcerative colitis such as immune modulation, anti-inflammatory signaling, epithelial barrier support, extracellular vesicle communication and promotion of a more favorable microenvironment for mucosal healing.
Combination Therapy with UC-MSCs and Conventional Therapies for Ulcerative Colitis
UC-MSCs isn’t positioned in a responsible clinical model as an alternative for routine ulcerative colitis therapy. Alternative approaches include discussing UC-MSCs as part of an integrated care pathway for specific patients.
A structured pathway may include:
Evaluation of gastrointestinal gastroenterology Assessment → assessment of disease severity → standard medical treatment → UC-MSCs for identified cases in only a few instances → nutrition and rehabilitation support → longterm follow-up
This combined approach is crucial, because ulcerative colitis needs medical management in the long term. Disease activity cannot be inferred by symptoms alone. Guidance of care may require laboratory markers, endoscopy, imaging, stool markers, nutritional status and medication history or physician evaluation.
For selected patients, UC-MSCs offer a promising adjunct in situations where the aim is to harmonise mucosal repair pathways with inflammatory and immune control. Yet, realistic treatment expectations are important. The clinical and regulatory context should determine whether UC-MSCs are presented as investigational or supportive, with outcomes varying accordingly.
Unveiling the Truths Behind UC-MSCs and Ulcerative Colitis Treatments in Thailand
Thailand has also developed into a regional hub for medical tourism, sophisticated wellness programs and integrative medicine. Thailand could allow access to private hospitals, gastroenterology services for international patients, rehabilitation assistance and supervised regenerative medicinal programm.
The attractions of Thailand for UC-MSCs and ulcerative colitis treatments also lie in the clinical services, patient coordination activities, hospitality infrastructure as well as accessibility to multidisciplinary care. Patients might be looking for programmes that include a gastrointestinal assessment, supportive therapy using cells, nutrition strategies and follow-up assessments.
Nonetheless, the clinical message needs to strike a good equilibrium. Why UC-MSC be discouraged as remedy for ulcerative colitis. Patients should be told that he standard ulcerative colitis treatments remains paramount and any regenerative treatment should be mediated through properly trained doctors.
A more academically defensible positioning would be:
UC-MSCs may be considered for a medically supervised adjunctive support regimen in select individuals with ulcerative colitis, particularly where clinical endpoints are to orientate mechanisms implicated in those mucosal healing and inflammatory resolution processes that manifest as dysregulated immune regulation.
Limitations and Safety Considerations
UC-MSCs are potentially powerful stem cells for regenerative medicine, however clinical use need to be considered with caution. Key considerations include the source of cells, donor screening, manufacturing standards, sterility testing, characterization of cells including purity and content level assessment as well as route of administration dosing patient selection and post treatment monitoring.
Immunosuppressive drugs, biologics, corticosteroids, anticoagulants, antibiotics and other medications may be administered to patients with ulcerative colitis. To make UC-MSCs available, medical review is established first as the health effects of this cell are uncertain.
Potential issues include: infection, immune activation and illness in poorly selected patients, unsubstantiated claims that effects observed in low-quality animal studies can be extrapolated to humans (without limits), and variable quality of treatment from one provider to another. It is because of this that UC-MSCs should only be delivered in the presence of medical supervision, supported by explicit and practical guidelines.
The most responsible statement is:
Our hope is that the role of UC-MSCs will be framed as an adjunct supportive and exploratory approach to ulcerative colitis, rather than a replacement for gastroenterologist-directed treatment, pharmacotherapy, endoscopy assessment of left sided disease or management for life threatening exacerbations.
Closing
Although the application of UC-MSCs in clinical practice remains to be validated, these cells have become a focus of scientific interest for their potential contributions to immune regulation, anti-inflammatory signals, paracrine communication and mucosal support for patients with advanced ulcerative colitis that are maintaining mucosal healing. In contrast to conventional therapies that are directed mostly towards modulating inflammation and maintaining remission, UC-MSCs target the biological milieu of tissue repair and immune homeostasis.
On the other hand, UC-MSCs should not be touted as a cure or substitute in place of standard ulcerative colitis treatment. The most appealing framework integrating UC-MSCs and ulcerative colitis therapies is as elements of a comprehensive, medically managed treatment regimen incorporating conventional gastroenterology therapy, rigorous monitoring, nutritional support and certain regenerative medicine approaches. Under this equilibrium, UC-MSCs may enhance a well-regulated support service while upholding sustainability/enforceable scrutiny/credible benchmarks/mature forecasting.