Why this topic sounds simple but really is not
- OA is often described as a “bad knee,” but the biology is much bigger than that.
When someone says they have a bad knee, usually they mean pain or stiffness, maybe swelling. They might even have trouble walking or getting out of bed in the morning. This kind of thing can make that joint less and less dependable over time. A lot of times in public health messages or technical terms for medical conditions, you’ll see things that suggest OA–especially knee osteoarthritis. This is what the CDC says makes people have stiff joints in the morning. More recent reviews continue to describe osteoarthritis as one of the most common chronic joint disorders and one of those that tend to create significant disability.
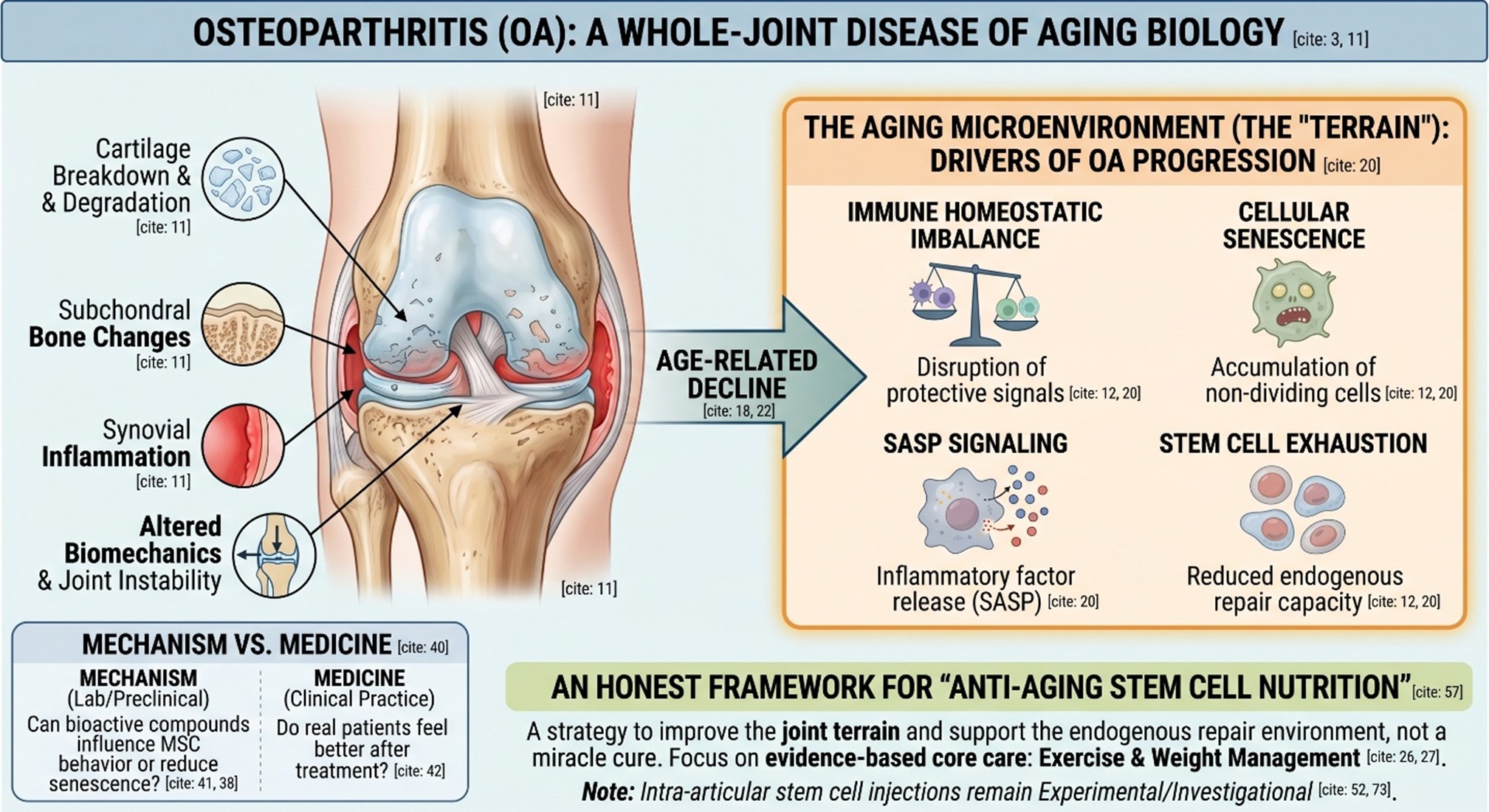
That matters because the phrase stem cell therapy for a bad knee sounds very direct, almost like a one-step answer to a one-joint problem. But OA is not just a worn hinge. It is a whole-joint disease involving cartilage breakdown, subchondral bone changes, synovial inflammation, altered biomechanics, and—especially in older adults—an aging tissue environment that becomes less able to repair itself well. Reviews from 2025 describe OA as increasingly tied to immune imbalance, cellular senescence, and even stem cell exhaustion inside the joint microenvironment.
What “Anti-Aging Stem Cell Nutrition” should mean if we are being honest
- It is not a formal OA treatment category
It was a powerful keyword, but Anti-Aging Stem Cell Nutrition is not a recognized guideline category in osteoarthritis care. Perhaps we should view this idea in another way. In addition to diet quality, body composition, inflammation, and oxidative stress, military exposures of some kinds may shape the aging joint environment and thus subtly affect how it behaves after endogenous repair systems come into action. These could also change the outcomes for stem cells. In scientific terms, that is precisely what is wrong with it but it is not the same thing as saying that one supplement or one anti-aging plan can reverse OA.
Aging biology is part of OA, not just a side note.
This is where the “anti-aging” part becomes more than branding. Bone Research’s 2025 review on the aging microenvironment in OA highlights immune homeostatic imbalance, senescent cells, SASP signaling, and stem cell exhaustion as important components of osteoarthritis progression. In other words, aging does not just happen in the background while OA develops. Aging biology is one of the reasons OA develops the way it does. That makes the idea behind Anti-Aging Stem Cell Nutrition more interesting: not as a miracle menu, but as an attempt to improve the terrain in which joints age.
Where nutrition actually fits in OA
- Diet matters most when it changes the joint environment.
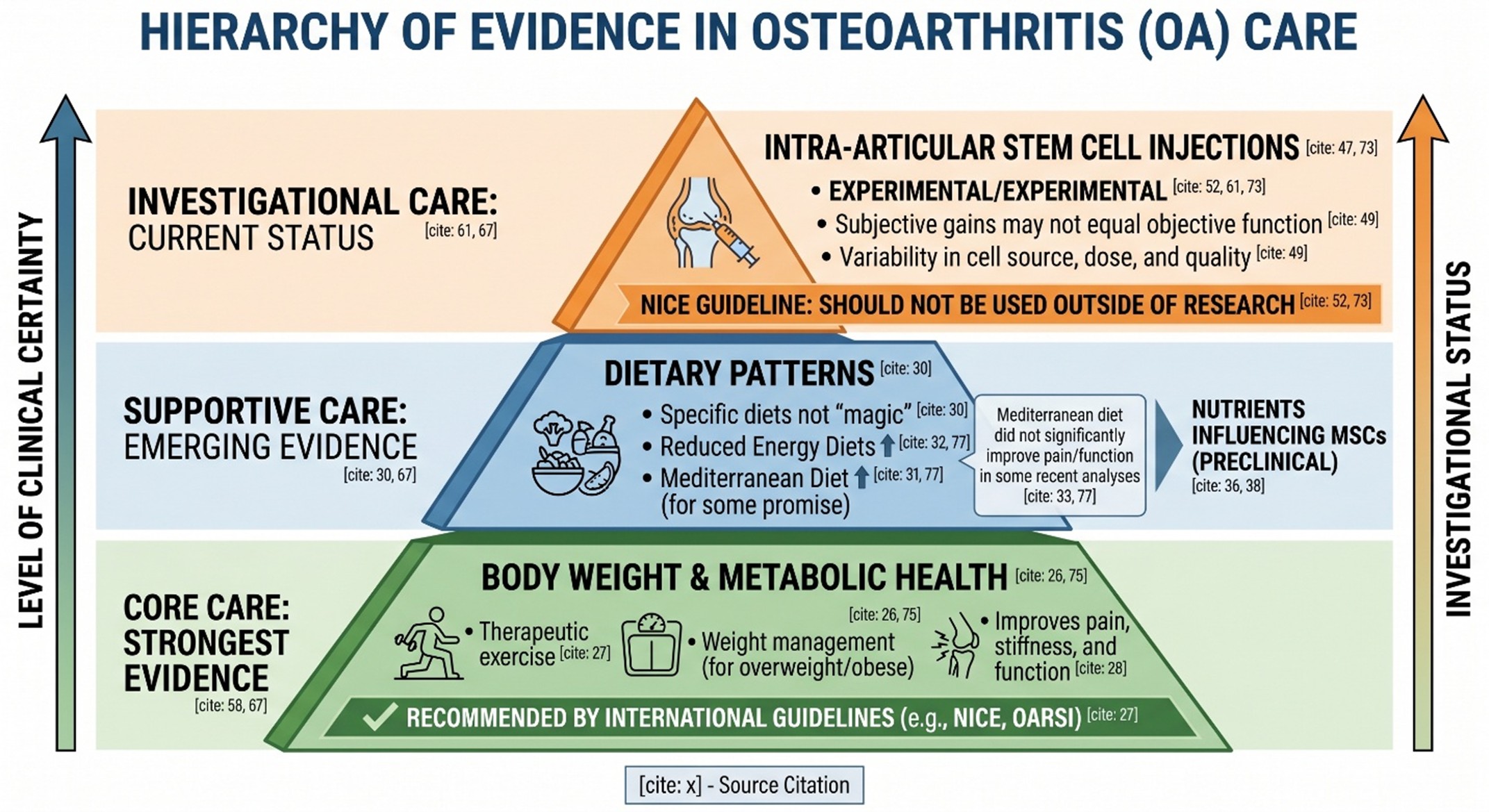
The most credible nutrition message in OA is still the least glamorous one: body weight, metabolic health, and inflammatory load matter. The NICE guideline recommends therapeutic exercise and weight management as core parts of osteoarthritis care, and OARSI-linked reviews continue to note that weight management is widely recommended across international guidelines for knee OA. For patients who are overweight or obese, weight loss helps with pain, stiffness, and function. That is not “anti-aging” in the influencer sense, but it is anti-decline in a very practical clinical sense.
- Specific dietary patterns may help, but they are not magic.
A further layer is added by recent nutrition reviews. An updated report on the Mediterranean diet and osteoarthritis in 2024 found that some observational studies have found a greater adherence to be associated with less OA risk and less severe symptoms, and a few intervention studies show improvements in pain, function, and quality of life. Also in 2025, a nutrition meta-analysis showed that when weighted by the study type, while dietary interventions as a whole can improve pain, physical function, and help manage weight management in OA, reduced energy diets appeared to work better than the specific named diets evaluated with metrology/how much does it cost money and effort wise; furthermore the Mediterranean diet itself did not change in this analysis functionally significant pain levels at one year follow-up were nonetheless statistically indistinguishable between the two groups. This kind of nuance is exactly what the topic needs: Nutrition matters, but not all stylish diets yield equal clinical backgrounds.
The “stem cell” part of Anti-Aging Stem Cell Nutrition
- Some nutrients may influence stem-cell behavior, but mostly in preclinical research.
This is where online content often gets slippery. There is real scientific interest in whether natural products or bioactive compounds can improve mesenchymal stem cell survival, reduce senescence, or enhance cartilage-repair signaling. Reviews published in 2025 discuss synergistic effects of natural products with MSCs in OA models, and other papers describe bioactive compounds that may regulate MSC behavior or reduce senescence-related dysfunction. But this work is still largely preclinical or translational. It does not mean that a supplement marketed as Anti-Aging Stem Cell Nutrition has already become a validated OA treatment.
- That is the key difference between mechanism and medicine.
Mechanism asks, “In practice, will this compound affect stem-cell biology, cartilage inflammation?” Medicine asks, “Do real patients feel better after this?” It’s not the same question. The way people usually put it is like this: ‘It makes perfect sense to be concerned about nutrition when your knee deteriorates, but it is intellectually dishonest to treat nutritional solutions for OA as if they had already been identified.’
Where does stem cell therapy for a bad knee stand today
- The field is active, but still not routine care
Now, to the phrase people actually search: stem cell therapy for a bad knee. In research terms, this usually means intra-articular mesenchymal stem/stromal cell-based injections for knee osteoarthritis. Recent systematic reviews and meta-analyses suggest these injections may improve subjective pain and symptoms in some patients, and some 2025 analyses report improvements in pain and function, especially in unoperated knee OA. But the same literature also notes variability in cell source, dose, comparators, and trial quality, and some reviews say subjective gains do not consistently translate into better objective knee function.
- Guidelines remain more cautious than marketing.
That is why guidelines still sound more restrained than websites do. NICE states that although some very small studies suggested potential benefit, intra-articular stem cell injections for OA are experimental and should not be used outside of research. That single point is probably the most important reality check in the whole article. It does not mean the science is empty. It means the science is still maturing, and OA patients deserve that distinction to be stated clearly.
The most grounded way to connect anti-aging, nutrition, and bad knees
- The smartest model is layered, not all-or-nothing
The bottom line – and the start-point for Anti-Aging Stem Cell Nutrition – is to support joint biology in aging, rather than seeking miraculous treatments. For osteoarthritis (OA), that means attending to the most important things first: the things with the strongest evidence, exercise, weight management, symptom-guided medical care, and realistic expectations. Nutrition becomes important because it can modify weight, inflammation, and metabolic stress. Stem-cell science becomes relevant because OA is a disease in part due to failed repair—a joint that is aging. But stem cell therapy for a bad knee remains investigational, and nutrition remains supportive rather than curative.
The honest conclusion
The most honest conclusion is not anti-stem-cell and not anti-nutrition. It is simply more disciplined. OA is strongly linked to aging biology, and that makes the idea behind Anti-Aging Stem Cell Nutrition scientifically interesting. Nutrition can absolutely matter, especially in terms of weight, metabolic health, and inflammatory burden. Stem-cell therapy for a bad knee has produced promising but still inconsistent clinical signals. For now, the strongest evidence supports building a healthier joint environment first and treating stem-cell injections as an evolving research area rather than a settled answer.
Frequently Asked Questions
1) What does “Anti-Aging Stem Cell Nutrition” really mean in OA?
It is best understood as a way of talking about how diet, metabolic health, inflammation, and aging biology may affect the joint environment and stem-cell-related repair capacity. It is not a formal guideline-approved OA treatment category.
2) Is stem cell therapy for a bad knee already a standard treatment?
No. NICE says intra-articular stem cell injections for osteoarthritis are experimental and should not be used outside of research.
3) Can nutrition actually help osteoarthritis?
Yes, especially through weight management and broader metabolic health. Guidelines and reviews continue to support exercise plus weight-management strategies, and weight loss in people with OA and overweight or obesity helps pain, stiffness, and function.
4) Does the Mediterranean diet cure OA?
No. Some observational and intervention data are promising, but newer meta-analytic work suggests reduced-energy diets may be more consistently helpful than any single branded diet pattern, and Mediterranean-diet effects on pain and function were not significant in one 2025 meta-analysis.
5) Why do people connect OA with anti-aging at all?
Aging is a major driver of OA biology. Recent reviews describe osteoarthritis as linked to senescent cells, immune imbalance, and stem cell exhaustion, which makes aging biology central to the disease rather than peripheral to it.