Comprehending Type 1 Diabetes More Than Just Blood Glucose Control
Type 1 diabetes: an autoimmune disorder in which the insulinsynthesizing beta cells of the pancreas are attacked by immune system. In general, when beta-cell function deteriorates, then the body cannot secrete adequate amounts of insulin to maintain blood-glucose homeostasis. This is why insulin therapy continues to be the mainstay of treatment for type 1 diabetes.
But, quite a few patients are still looking for other supportive means particularly whilst having fluctuating blood sugar, lengthy-term insulin reliance, fatigue, metabolic strain or worried about excessive risk of future complications. For this reason, UC-MSC Thailand has become an increasingly searched topic by patients investigating stem cell and regenerative therapy for type 1 diabetes.
Umbilical Cord-Derived Mesenchymal Stem/Stromal Cells (UC-MSCs) UC-MSCs are being studied for their potential involvement in immune regulation, inflammation balance, cellular repair signaling, and pancreatic microenvironment support. However, this field requires cautious talk. Finally, UC-MSCs should not be advertised as a type 1 diabetes cure or insulin substitute.
The Case for UC-MSC Thailand in T1D
Thailand has earned its rightful place among the destinations of those seeking out travel for medical facilities, wellness medicine, hospital-based expert geriatric and regenerative programs stemming up, supported by essential biomedical laboratory work. This is part of the reason why international patients with an interest in advanced supportive care are turning to UC-MSC Thailand.
In the case of type 1 diabetes, UC-MSCs are mainly investigated for their potential immunomodulatory and anti-inflammatory capacities. Stemming immune mediated betacell destruction, pre-clinical trials are initiating to identify potential value of mesenchymal stem/stromal cells in maintaining a more tolerogenic state.
Your aim is not genuinely to replace the pancreas. More precisely, it is likely that UC-MSCs communicate with neighboring tissues using biological signaling. This could aid the survival of cells, decrease inflammatory strain and enhance tissue milieu in definitive cohorts.
T1D searching how UC-MSCs May work in Type 1 Diabetes
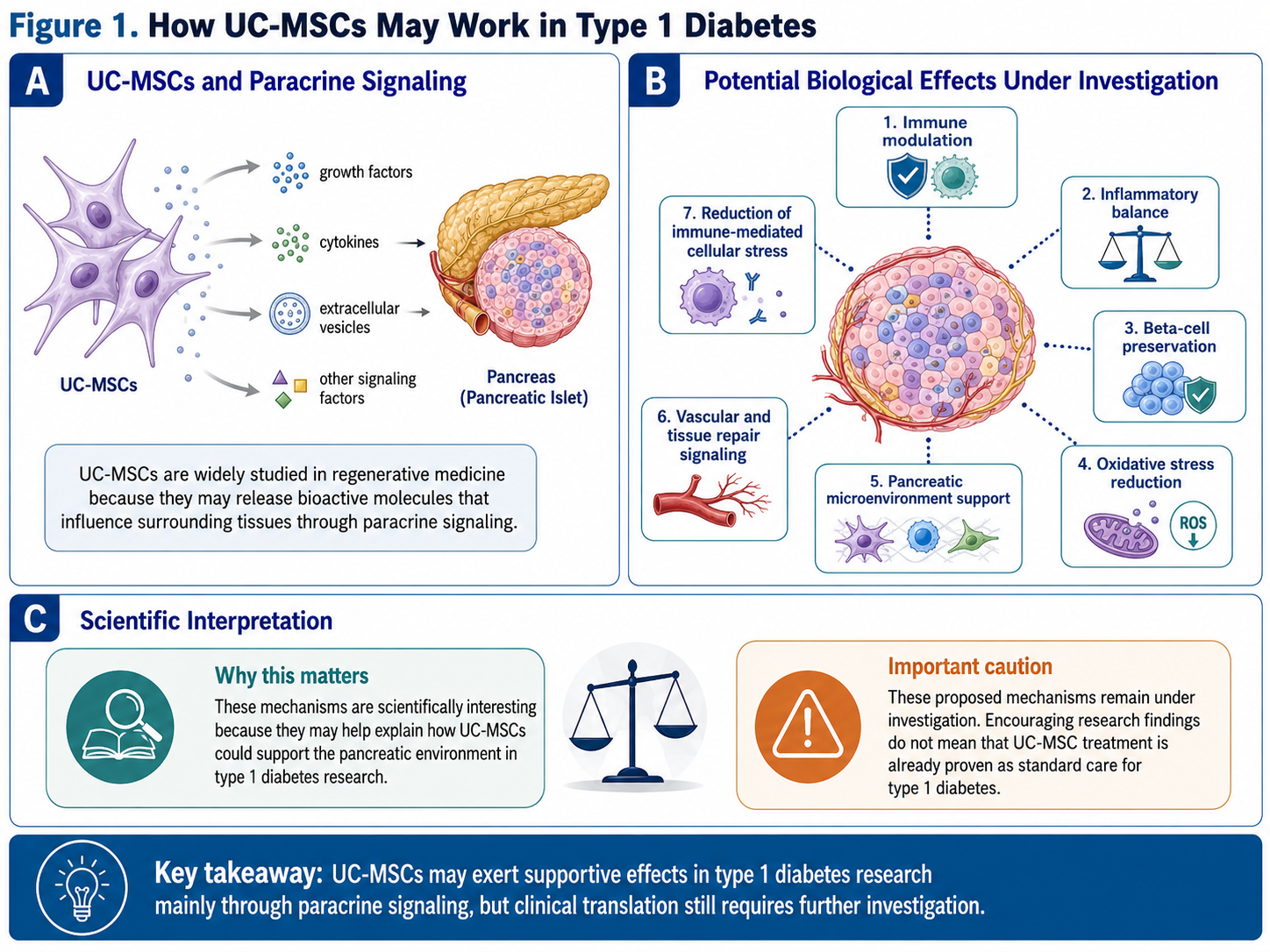
The potential of UC-MSCs to release numerous bioactive molecules, including growth factors, cytokines, extracellular vesicles, and other signaling factors make this type of cells widely discussed in regenerative medicine. Paracrine signaling is the process that takes place here.
Mechanisms of UC-MSC for type 1 diabetes recherche could also affect:
Immune modulation
Inflammatory balance
Beta-cell preservation
Oxidative stress reduction
Pancreatic microenvironment support
Vascular and tissue repair signaling
Reduction of immune-mediated cellular stress
These mechanisms are scientifically interesting, but they have yet to be fully investigated. Patients should understand that just because Rand’s stood-in for my doctor is encouraging research, it’s not the same as saying a treatment has already been proven to be standard care.
Figure 1: Proposed mechanisms of UC-MSCs in type 1 diabetes research, focusing on paracrine signaling, immune modulation, inflammatory balance, beta-cell preservation, oxidative stress reduction, and pancreatic microenvironment support.
Patient Progress: Blood Tests Beautiful OG by The Continue Reading
Sometimes, a patient will tell you that their lab tests after a regenerative support program are almost encouraging. In one case, a patient declared her diabetes blood test to be “wonderful,” and she wished salt away insulin injections.
A pivotal moment that calls for the best of caution and hope
Better blood test results pass with the likelihood of better glucose control better insulin sensitivity lifestyle adjustment reduce inflammatory burden more and better nutrition or broader improvement consistent metabolic stability. But in type 1 diabetes, favorable blood tests do not guarantee the body can safely internally produce sufficient amounts of insulin.
The safest message is:
Positive results are encouraging, however insulin should never be tapered without an endocrinologist’s go ahead.
It is also dangerous to stop the use of insulin too fast. Without sufficient insulin in the body, blood glucose can soon soar and ketones accumulate. This can put higher risk of a rare but serious medical emergency known as diabetic ketoacidosis.
Before considering lowering insulin, what you may want to check for?
Any insulin adjustment should not only be at the discretion of an appropriately skilled diabetes provider. Multiple markers may need to be evaluated by the doctor, and it may not involve just a single blood test result.
Important assessments may include:
HbA1c
Fasting blood glucose
Post-meal blood glucose
C-peptide level
Insulin requirement
Continuous glucose monitoring data
Frequency of hypoglycemia
Ketone risk
Kidney function
Liver function
Body weight and nutrition status
Diabetes duration and autoantibody status
Insulin reduction (if indicated) should ideally be done in a staged way and with monitoring. Not to stop insulin quickly but maintaining safe and stable blood glucose control.
The Right Way to UC-MSC Thailand for Type 1 Diabetes
A legally and ethically conducted UC-MSC Thailand program for type 1 diabetes should be medically supervised Study design and has to be carefully planned. It must not be presented as an isolated treatment or a guaranteed method for eliminating insulin use.
A more fitting framework might consist of:
Medical Assessment
Patients should have a complete assessment of diabetes history, use of insulin, glucose control, complications (if any), medications / and lifestyle habits and laboratory tests in the past.
Laboratory Monitoring
This can include testing for HbA1c, fasting glucose, C-peptide, kidney function tests, liver function tests (LFTs), lipid profile and inflammatory markers / other metabolic indicators.
UC-MSC Supportive Program
In a nutshell, we could interpret UC-MSCs and adopt them as an adjunct regenerative remedy considering that they tailor the immune homeostasis, modulates inflammation and signs to cells.
Endocrinology Follow-Up
Continue follow-up with Diabetes Specialist (especially if blood sugar is starting to improve)
Safe Insulin Adjustment
Physician recommendations for any insulin reduction should be followed closely with glucose measurements.
The role of UC-MSC support in type 1 diabetes should not therefore be described as “curing diabetes” or even no longer needing insulin. Here is a more medically responsible message:
UC-MSCs are being investigated as a potential regenerative strategy to help modulate immune homeostasis, inflammatory cytokine network, and pancreatic microenvironment support in select patients with diabetes.
Conclusion
UC-MSC Thailand and type 1 diabetes therapy are emerging issues in regenerative medicine. Type number is an explanation because it is a chronic, autoimmune disease that prevented insulin production to the sweetener of blood glucose and thus very much decreased quality of life.
UC-MSCs can act as immunomodulators, anti-inflammatories and tissue supportive signallers, which is why they are currently being tested. Such mechanisms may be of interest to type 1 diabetes biologists, particularly with respect to immune regulation and beta-cell preservation. On the other hand, this is still an evolving area and UC-MSCs should not yet be considered a panacea or alternative to insulin.
In itself it is good news if the blood tests of a patient turn out well. But anyways, insulin is not a drug that you should stop immediately. The next right step is to review medical, HbA1c, glucose trends, C-peptide, insulin requirement and ketone risk. Insulin may be adjusted slowly under supervision If the endocrinologist believes it to be safe.
The best way to compete in the modern regenerative medicine era is not to outright overreach. It is about balancing scientific advancement, prudence, safety for patients and GPs, and realistic expectations.