Autism Spectrum Disorder, a type of neuron development disorder has seen an exponential increase in global prevalence over the past decade. At its core, this disorder is defined by persistent difficulties with social communication, repetitive patterns of behavior and restricted interests. But beyond behaviour, patients suffer a very pronounced physiological effect. The same cellular dysfunction may underlie systemic inflammation, immune dysregulation, and oxidative stress in individuals. These can vary from mild social difficulties to total non-verbal status, requiring a lifetime of care. The impact not only of this disorder but also on the future earnings potential and educational trajectory of the child perpetuates huge emotional and financial burdens for families.
1.Pathophysiology and Neural Mechanisms of Autism
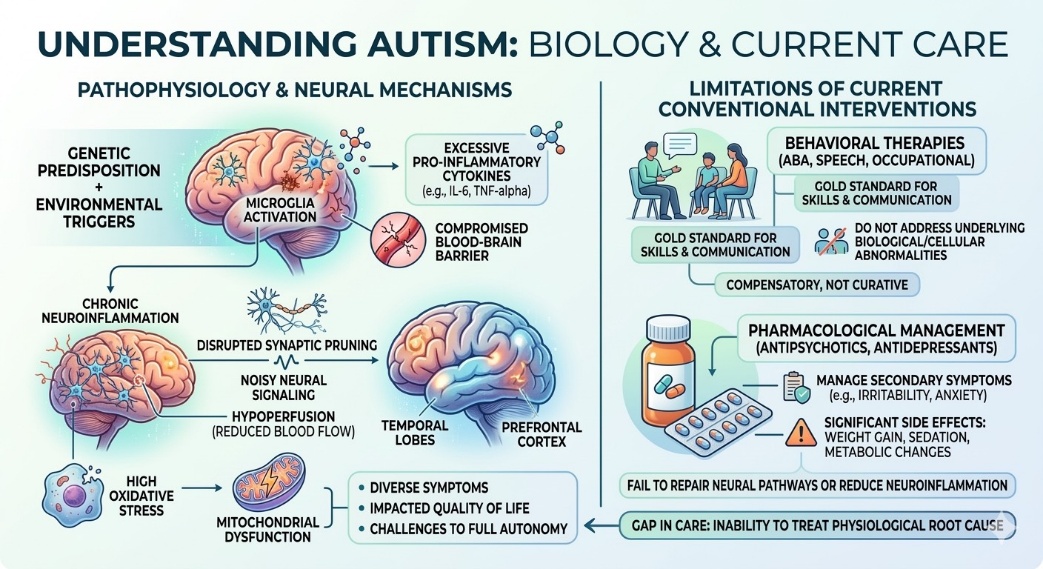
The Pathophysiology of Autism involve a sophisticated interplay between genetic predisposition and environmental triggers. Research indicates that the core of the issue often lies in neuroinflammation and a compromised blood-brain barrier. Specifically, the activation of microglia—the resident immune cells of the brain—leads to the excessive release of pro-inflammatory cytokines such as IL-6 and TNF-α. This chronic inflammatory state disrupts synaptic pruning, a vital process where the brain removes unnecessary neural connections to improve efficiency. When this process fails, it results in noisy neural signaling, which manifests as sensory sensitivities and social processing delays.
Furthermore, many Autism patients exhibit hypoperfusion, or reduced blood flow, to specific regions of the brain like the temporal lobes and the prefrontal cortex. This lack of oxygen and nutrients contributes to neuronal dysfunction. The cellular environment is further damaged by high levels of oxidative stress, where the body cannot effectively neutralize free radicals, leading to mitochondrial dysfunction. This cascade of biological failures explains why the symptoms are so diverse and why they significantly impact the quality of life, often preventing individuals from achieving full autonomy in adulthood.
2.Limitations of Current Conventional Interventions
Currently, the medical Autism community relies heavily on a combination of behavioral therapies and pharmacological management. Applied Behavior Analysis (ABA), speech therapy, and occupational therapy are the gold standards for improving social skills and communication. While these methods are essential for developmental progress, they do not address the underlying biological or cellular abnormalities. They are essentially compensatory strategies rather than curative measures.
Pharmacological Autism treatments, such as antipsychotics or antidepressants, are often prescribed to manage secondary symptoms like irritability, aggression, or anxiety. However, these medications come with a heavy toll of side effects, including significant weight gain, sedation, and metabolic changes. More importantly, these drugs fail to repair the neural pathways or reduce the neuroinflammation that causes the behavioral issues in the first place. This gap in medical care—the inability to treat the physiological root cause—has led researchers to explore more regenerative approaches likes Stem Cell Therapy that can modify the disease environment at a molecular level.
Figure 1: Understanding Biology and Current Care of Autism
3.The Role of UC-MSCs in Stem Cell Therapy
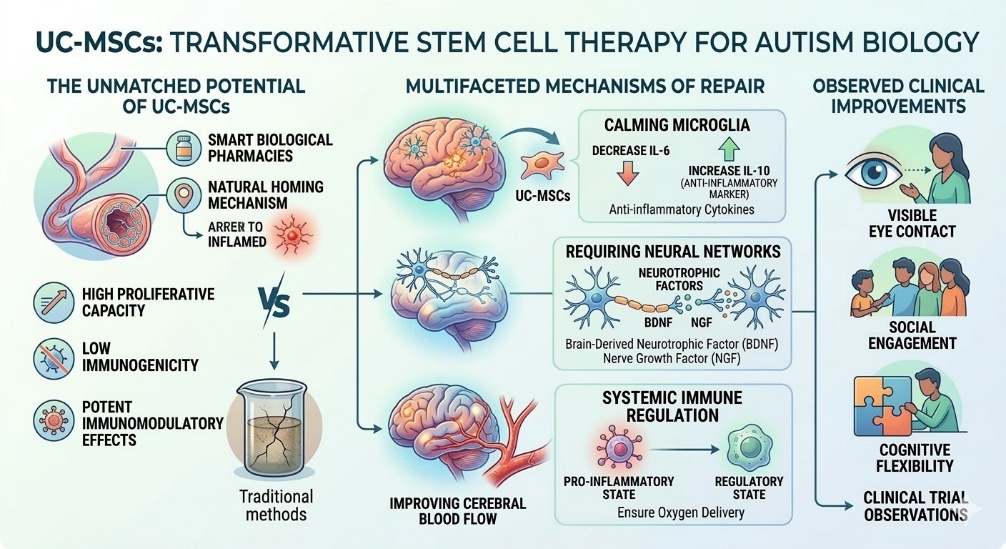
This is where Stem Cell Therapy using UC-MSCs offers a transformative potential. Unlike Autism traditional methods, these cells act as biological pharmacies. When introduced into the body, they exhibit a natural homing mechanism, migrating toward areas of inflammation and tissue damage. The primary reason for utilizing UC-MSCs over other sources is their high proliferative capacity, low immunogenicity, and potent immunomodulatory effects.
The mechanism of through UC-MSCs cells work is multifaceted. First, they secrete anti-inflammatory cytokines that reduced the overactive microglia in the brain. By reducing the levels of IL-6 and increasing anti-inflammatory markers like IL-10, they create a more hospitable environment for neural repair. Second, they release neurotrophic factors such as Brain-Derived Neurotrophic Factor (BDNF) and Nerve Growth Factor (NGF). These proteins are crucial for supporting the survival of existing neurons and encouraging the formation of new synaptic connections, effectively rewiring the brain’s communication networks.
Additionally, UC-MSCs promote angiogenesis, which is the formation of new blood vessels. This improves blood flow to the hypo-perfused areas of the brain, ensuring that neurons receive the necessary oxygen to function correctly. The cells also assist in regulating the immune system, shifting it from a pro-inflammatory state to a regulatory state. This systemic reset is what allows for the visible improvements in eye contact, social engagement, and cognitive flexibility observed in clinical trials.
Figure 2: Transformative Stem Cell Therapy for Autism
4.Future Prospects and the Strategic Importance of Thailand
The outlook for Autism treatment in Thailand is exceptionally promising. The country has positioned itself as a global hub for regenerative medicine, blending advanced laboratory technology with a highly regulated medical framework. Stem Cell Therapy is no longer a distant hope but a tangible reality in Thai clinical settings. The reason Thailand stands out is its rigorous adherence to international processing standards for UC-MSCs, ensuring that the cells are pure, potent, and safe for pediatric use.
Thailand also offers a unique ecosystem where academic research and clinical application coexist seamlessly. The government has invested heavily in biotechnology, fostering an environment where medical professionals are specifically trained in the nuances of cell transplantation. For families seeking help for Autism, Thailand provides a compassionate yet scientifically robust destination. The integration of traditional Thai care values with cutting-edge cellular science makes it a preferred choice for international patients. As more long-term data emerges, the goal is to standardize these protocols, making regenerative treatments a primary option rather than a last resort.
To sum up, there is a huge shift in paradigm of treatment or intervention from purely behavioral management to cellular level. Although first line therapies offer much needed relief, they do not reverse the neuroinflammatory and oxidative damage that the disorder has already caused. UC-MSCs when translated through Stem Cell Therapy provides intervention to these fundamental biological limitations through immune modulation and neuroprotection. Much of this innovation is still driven from Thailand which continues to offer hope through scientific excellence and its long held commitment to improving the lives of those individuals affected by this complex condition. With further exploration and clinical refinement, the opportunity to profoundly increase patients’ functional independence is nearer than before.