Osteoarthritis (OA) is a common degenerative joint disease that has a substantial impact on quality of life. For patients, that can mean ongoing pain, stiffness and progressive diminished mobility that can thwart the most mundane of day-to-day activities. As the disease progresses, most people become more reliant on medications or assistance for simple mobility.
Given the burden of osteoarthritis in society, current treatment strategies are mainly targeted towards symptom alleviation instead of reversing the biological processes behind this condition. Pain management techniques can provide short-term relief, but they do not heal damaged cartilage or remedy joint degeneration. This limitation has motivated interest in more robust therapeutic modalities.
Recently, regenerative medicine has played an important role in the clinical as well as research aspect where Thailand stem cell therapy: The use of umbilical cord–derived mesenchymal stem cells (UC-MSCs) and growth factor support has gained much attention. As opposed to solely treating symptoms, these therapies are meant to work at a cellular level by complementing the joint environment.
Pathophysiology of Osteoarthritis
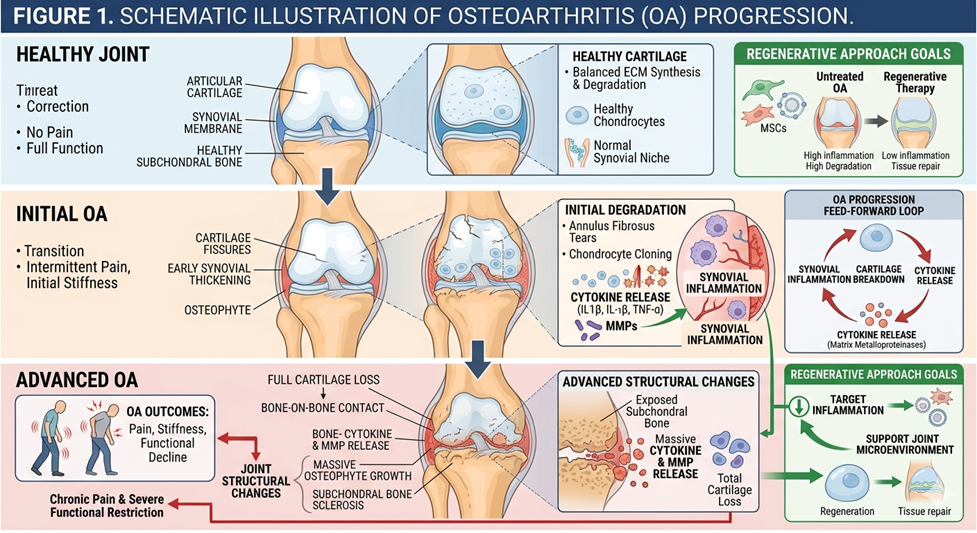
Understanding osteoarthritis itself first requires an understanding of the underlying biological processes. The disease generally begins with destruction of articular cartilage, the smooth tissue that cushions joints and enables bones to move freely.
This damage may result from:
- Repetitive mechanical stress
- Aging-related cellular decline
- Genetic predisposition
- Previous injury
Over time, the cartilage may erode and tiny particles are released into the joint space. These remnants can prompt an immune reaction in the synovial membrane, resulting in macrophage activation and inflammatory cytokine production.
This inflammatory cascade contributes to:
- Continued cartilage degradation
- Breakdown of extracellular matrix
- Increased joint inflammation
- Impaired natural repair mechanisms
Over time, as the protective cartilage layer erodes, bones may begin to make direct contact. This results in increased friction, leading to pain, stiffness, and structural changes within the joint, including the formation of osteophytes (bone spurs). Chronic pain associated with osteoarthritis can also contribute to secondary complications such as sleep disturbances, reduced physical activity, and emotional stress. Importantly, once cartilage is significantly damaged, the body has limited ability to regenerate it naturally.
Limitations of Conventional Osteoarthritis Treatments
Conventional treatments for osteoarthritis focus on alleviating symptoms rather than repairing joint structure.
Common approaches include:
- Non-steroidal anti-inflammatory drugs (NSAIDs) for the analgesic management
- Corticosteroid injections to reduce inflammation
- Physical therapy to enhance strength and range of motion
- Joint replacement surgery in advanced stages
Although these techniques will provide symptomatic relief in the short term, they come with certain limitations:
- Prolonged Use of NSAIDs Could Lead to Gastrointestinal and Renal Complications
- Repeated steroids may jeopardize cartilage integrity
- Physio does not recreate the tissue which was damaged
- Surgery carries risk and recovery time and potential for long-term complications
These limitations underscore the need for therapies that target the underlying biological processes of osteoarthritis, rather than just help manage their end symptoms.
Cellular Mechanisms of Regenerative Therapy
MSCs themselves potentially offer a biologically based treatment system. These cells are studied for their acute ability to communicate with damaged tissue by paracrine signaling instead of direct tissue replacement.
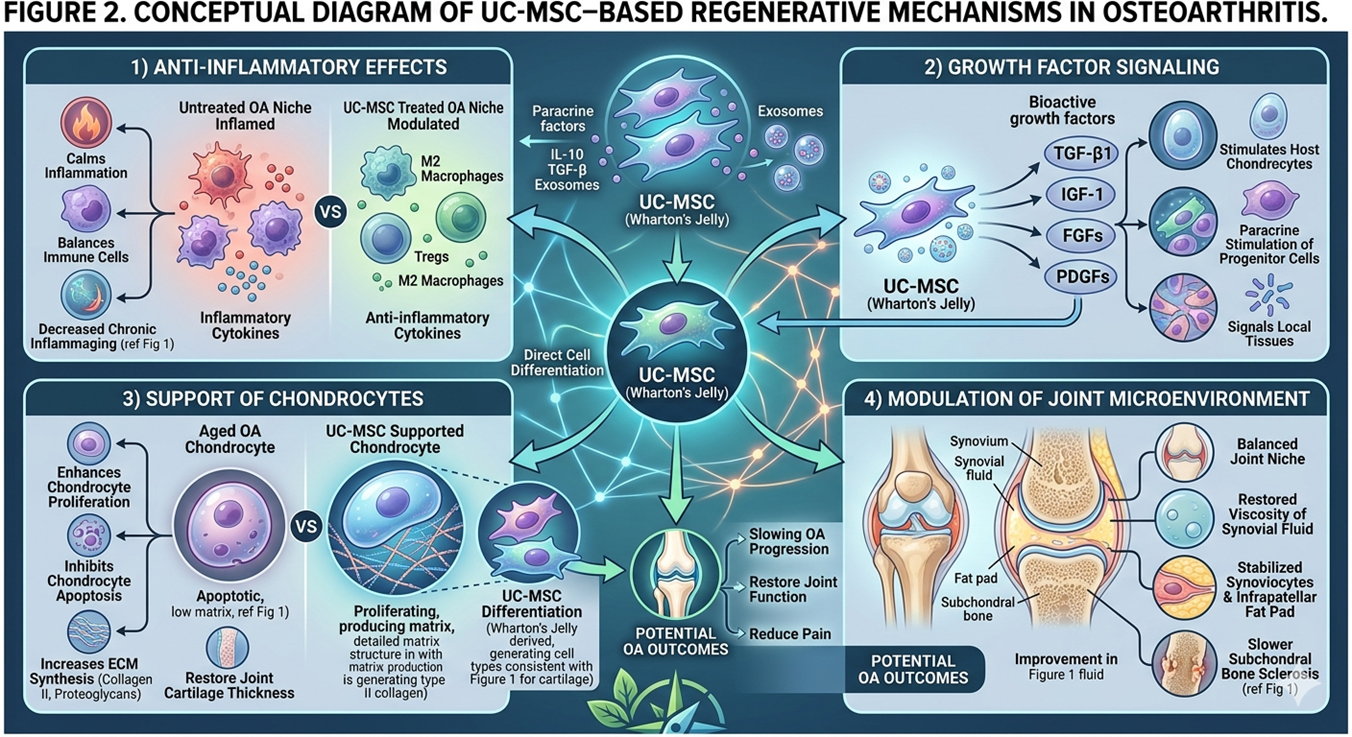
UC-MSCs, when exposed to the joint environment, may influence several mechanisms:
- Immunomodulation: Modulating proinflammatory responses in the joint
- Secretion of growth factors: That support cellular communication and repair processes
- Chondrocyte support: Modulation of cartilage-producing cell activity
- Regulating the components of the extracellular matrix: targeting structural elements of joint tissue
- Environment joint optimization: make microenvironment more balanced
This is largely mediated by growth factors; proteins that are involved in paracrine signaling pathways affecting cell behavior, tissue repair and the control of inflammation.
Moreover, MSCs were found to home toward sites of tissue injury a phenomenon commonly referred to as “homing” This may provide some degree of targeting to the site of interest where their effects can be felt locally.
Latest News from Thailand and Southeast Asia
Fortunately, Thailand and Southeast Asia have gradually established themselves as a powerhouse in regenerative medicine. The region has a combination of strong medical infrastructure, laboratory capabilities, and advancing expertise in cellular therapies.
Key contributing factors include:
- Establishment of specialized centers for regenerative medicine
- Failure to invest in biotechnology and laboratory systems
- Growing regulatory frameworks championing medical innovation
- Integration of personalized treatment planning
Thailand’s healthcare system also receives support from international patients, widening its access for patients requiring advanced treatment options.
Moreover, treatment plans are more frequently being customized to the profile of each patient in order to promote overall effectiveness and support natural bodily defenses.
Conclusion
Osteoarthritis is a degenerative disorder characterized by cartilage degradation, inflammation, and failed tissue regeneration. Conventional treatments offer significant symptom relief, but are not structurally restorative at the joint level.
Regenerative medication focusing on supporting the joint at cell level with stem cell therapy in Thailand using UC-MSCs and growth factors is a potential platform to offer real promise. These approaches are designed to enhance existing therapies and improve functional outcomes through the modulation of inflammation and the joint microenvironment.
Though these treatments are still investigational and results will vary, they demonstrate a wider transition toward biologically-informed approaches to the treatment of osteoarthritis.

