Primary Biliary Cholangitis (PBC) a chronic, progressive autoimmune disease afflicting the small bile ducts of the liver represents an ominous challenge in hepatology. Cholestasis ensues with the accumulation of bile acids due to damage to these functional units, leading readily to extensive scarring or cirrhosis. PBC is a devastating disease that can cause severe fatigue, disabling pruritus and ultimately liver failure. The psychological toll of living with a terminal chronic disease is as heavy a weight for visit patients. Although current medicine has achieved some successes, a considerable fraction of the patient population does not respond to frontline chemical treatments. To address this clinical gap, there is an urgent need to determine new regenerative strategies, in particular the use of UC-MSCs capable of modulating effectively the immune system and repairing hepatic tissue. With Stem Cell Therapy Thailand,the goal of the medical professional is to provide a top-notch biological approach to this autoimmune disease within the clinic.
The pathophysiology and clinical manifestations of PBC
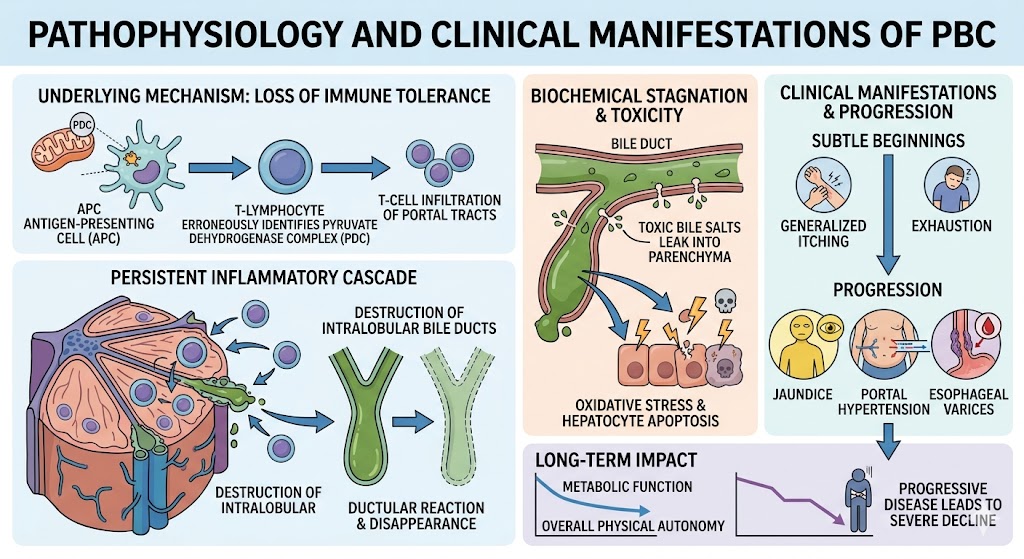
Primary Biliary Cholangitis is initiated by a loss of immune tolerance toward biliary epithelial cells. In particular, the T-lymphocytes of the body mistakenly recognize pyruvate dehydrogenase complex present in the mitochondria of these cells as foreign. This stimulates a chronic inflammatory cascade leading to T-cell infiltration in the portal tracts and destruction of the intralobular bile ducts. When the ducts go away, it causes the liver not to be able to move bile properly. This process stops at the biochemical level, promoting spillover of toxic bile salts in the adjacent parenchyma inducing oxidative stress and hepatocyte apoptosis. Initial clinical symptoms are usually nonspecific and consist of generalized pruritus and fatigue, eventually leading to jaundice, portal hypertension and esophageal varices. However the long-term consequence on life is high, with the progressive aspect of the illness generally inducing a drop in metabolic operate and bodily independence.
Figure 1: The Pathophysiology and Clinical Manifestations of PBC
2.Conventional Treatment Modalities and Constraints
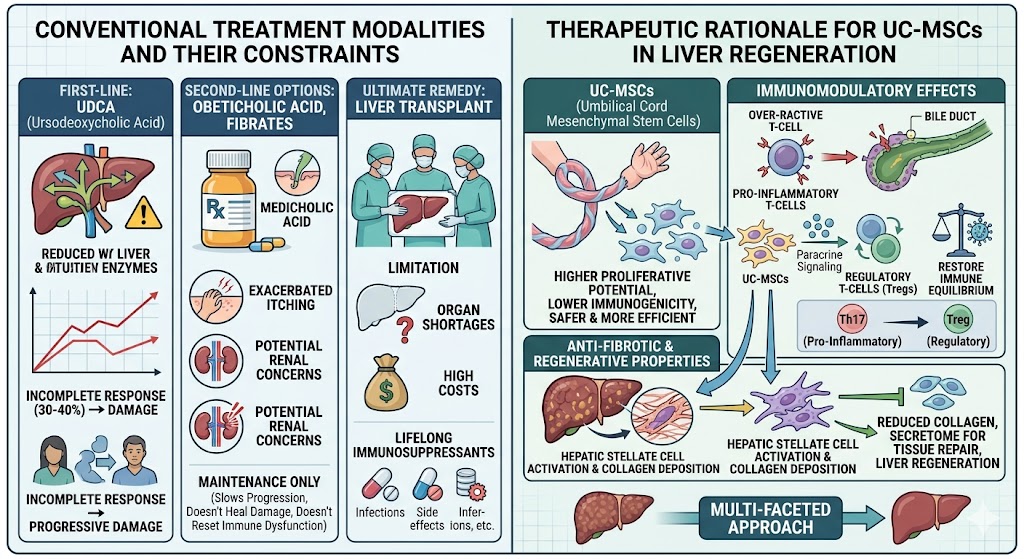
For decades, the standard approach to managing PBC has relied heavily on Ursodeoxycholic Acid (UDCA), which aims to improve bile flow and reduce liver enzyme levels. While UDCA is effective for many, approximately 30% to 40% of patients show an incomplete biochemical response, meaning their liver damage continues to progress despite treatment. Second-line options like Obet cholic Acid or fibrates have emerged, yet they often come with side effects such as exacerbated itching or potential renal concerns. Furthermore, these pharmacological agents are largely maintenance therapies; they slow the progression but do not heal the existing fibrotic damage or reset the underlying immune dysfunction. In the most critical cases, the only remaining option is a liver transplant. However, transplants are limited by organ shortages, high costs, and the lifelong requirement for immunosuppressive drugs, which carry their own set of risks and complications.
3.The Therapeutic Rationale for UC-MSCs in Liver Regeneration
The transition toward using UC-MSCs, or Umbilical Cord-derived Mesenchymal Stem Cells, marks a significant shift from symptom management to biological modulation. These cells are uniquely suited for treating PBC due to their potent immunomodulatory and anti-fibrotic properties. When administered, UC-MSCs exert their influence through paracrine signaling, releasing cytokines and growth factors that suppress the overactive T-cell response responsible for bile duct destruction. Specifically, they promote the conversion of pro-inflammatory Th17 cells into regulatory T-cells (Tregs), which help restore immune equilibrium. Additionally, UC-MSCs can inhibit the activation of hepatic stellate cells, the primary drivers of liver scarring. By reducing collagen deposition and stimulating the secretome for tissue repair, Stem Cell Therapy Thailand provides a multi-faceted approach that addresses both the autoimmune cause and the structural damage of the liver. Unlike bone marrow-derived cells, those sourced from the umbilical cord are more primitive, have higher proliferative potential, and possess lower immunogenicity, making them a safer and more efficient choice for systemic infusion.
Figure 2: Conventional and Therapeutic Rationale for UC-MSCs in Liver Regeneration
4.The Future Landscape of MSCs Research in Thailand
The outlook for utilizing MSCs to combat liver disease in Thailand is exceptionally promising. The country has established itself as a regional hub for advanced biotechnology, supported by a robust infrastructure of specialized medical facilities and research institutes. Thailand is particularly well-positioned for this advancement because of its stringent yet progressive regulatory frameworks that ensure patient safety while encouraging scientific innovation. The integration of Stem Cell Therapy Thailand into the broader medical tourism and healthcare sector allows for more accessible specialized care. Looking ahead, the focus is shifting toward off-the-shelf cellular products that can be standardized for PBC patients nationwide. The combination of expert hepatologists and cutting-edge cellular laboratories makes the nation an ideal environment for clinical trials that could eventually establish new protocols for regenerative hepatology on a global scale.
In summary, Primary Biliary Cholangitis remains a high-stakes medical condition that demands more than just traditional chemical management. The destructive cycle of autoimmunity and cholestasis requires a solution that can actually modify the disease environment. The application of UC-MSCs offers a sophisticated biological bridge, providing the immunomodulatory power necessary to halt ductal destruction and the regenerative capacity to address fibrosis. As the medical community in Thailand continues to refine these protocols, the synergy between advanced cell biology and clinical practice grows stronger. Ultimately, the adoption of Stem Cell Therapy Thailand represents a significant leap forward in improving the quality of life and long-term prognosis for those living with PBC, moving us closer to a future where chronic liver failure is no longer an inevitability but a manageable and reversible condition.