Type 2 diabetes mellitus (T2DM) is an extensively studied, common metabolic disease which affects millions of people worldwide and is still increasing at an alarming pace across all ages. While blood glucose is often well controlled with recent medical treatments, there are no direct actions at the cellular level and disease progression is not being halted.
Type 2 diabetes management has recently begun to change direction in using regenerative medicine. Among these, stem cell therapy with umbilical cord–derived mesenchymal stem cells (UC-MSCs) in particular is one of the best approaches. This new treatment restores pancreatic function, determines insulin sensitivity and has potential to modify the disease course as opposed to simply controlling its manifestations.
Revolutionized Diabetes Care with Stem Cell Therapy
Restoration of Insulin-Producing Cells
Under specific lab conditions, stem cells can turn into insulin-producing beta-cells. These cells had the ability to sense local glucose levels and secrete insulin, just like pancreatic beta-cells do under physiological conditions. This regenerative capacity gives hope to replenish the depleted insulin resources of the body.
Protection of Remaining Pancreatic Function
Stem Cells Release Other Growth Factors and Signalling Molecules that Maintain Friendliness in the Pancreas This particular state reduces the stress of cells, optimises the damage due to oxidative mechanisms and protects ongoing islet β-cells a loss of further relapse. Stem cell therapy works by preserving function in existing beta cells, which could potentially prevent the progression of diabetes too.
Decrease Inflammation and Oxidative Stress
Stem cells are still considered an amazing source of drugs due to their immunomodulatory and anti-inflammatory features. Mesenchymal Stem Cells (MSCs) release bioactive factors such as cytokines, that help modulate immune cell activity and decrease tissue damage by excess inflammatory responses. By reducing inflammation, it not only protects the pancreas but also increases cellular sensitivity to insulin (Shaw et al., 2010).
Enhancement of Insulin Sensitivity
So, this finding could help improve the way in which the tissue responds to insulin via stem cell therapy. Insulin resistance is defined as decreased responsiveness of insulin sensitive tissues (skeletal muscle, liver and adipose tissue) to effects from circulating insulin: one of the hallmarks of T2DM and crucial for glucose homeostasis. Stem cells have the potential to improve mitochondrial function in these tissues, as well as reducing inflammatory markers known to impair both glucose uptake and utilization. The synergistic improvement of insulin secretion and sensitivity represents a complete diabetes remedy that stem cell therapy can offer.
A : Stem cells restore insulin production, protect pancreatic cells from damage and modulate inflammation to improve glucose control by inducing insulin sensitivity.
IV: Evidence from Clinical Studies for Type 2 Diabetes and Stem Cell Therapy
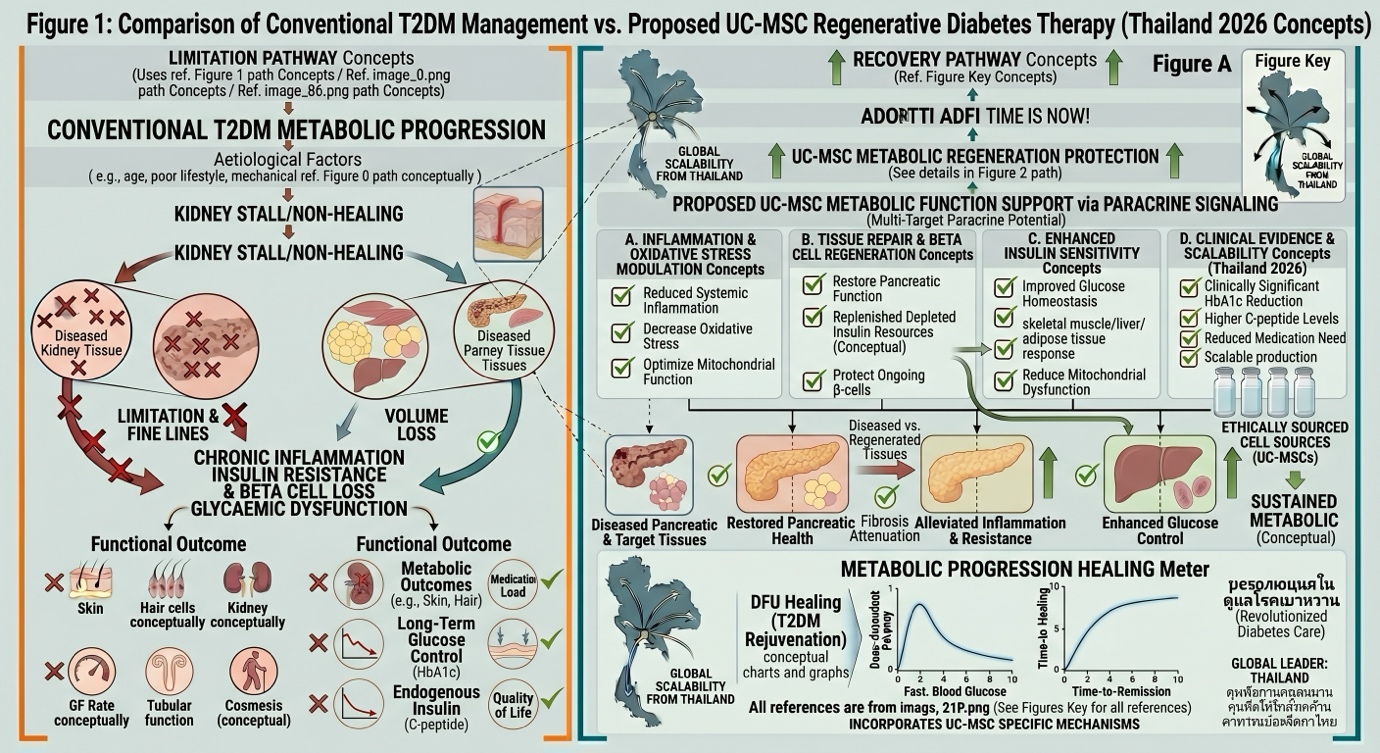
Outcomes from Stem Cell-Based Studies
Widespread improvements in associated metabolic markers have been reported with clinically significant reduction in glycated haemoglobin (HbA1c), a biomarker of long-term glycaemic control. Lower fasting blood glucose and higher C-peptide levels—a marker of endogenous insulin production—have also been demonstrated in patients. This meant for many, fewer insulin injections or oral glynase.
Stem Cell Therapy Subgroup Findings
Patients experience durable effects on glucose homeostasis, and even increase in pancreatic performance. Some went off insulin for months and even years at a time. Results like these suggest that stem cell therapy could have a fundamental impact on the disease.
Long-Term Observations
Follow-up studies elsewhere in northeast Asia have likewise shown the long-lasting effects of stem cell therapy. Several patient groups have been described in literature to achieve glycemic control at two or even three years after the introduction of a range of diabetes therapies. This also includes some studies where dozens / hundreds of people ceased all insulin for long periods, While further large-scale investigations are necessary, these data reinforce the promise of regenerative therapies to provide durable effects.
Advantages of Stem Cell Treatment in Comparison to Standard Diabetes Treatments
● Regeneration Therapy: This approach goes beyond blood sugar control and addresses damaged tissues to restore physiological homeostasis.
● Reduced Medication Requirement: Improved insulin sensitivity and pancreatic output could lead to patients being able to gradually wean off their medications.
● Good safety profile: The current evidence indicates that stem cell therapy is very well tolerated, with a much lower incidence of adverse events than prolonged use of drugs.
● Enhanced Quality of Life: Metabolite control and reduced treatment burden can substantially impact day-to-day functioning and quality of life.
● Potential for Disease Modification: Unlike conventional therapies, Stem Cell Therapy not only aims to alleviate the symptoms of T2DM but also addresses the underlying pathological mechanisms responsible for T2DM, potentially delaying or even preventing disease progression.
Type 2 Diabetes and the Regenerative Medicine Leader: Thailand
● Modern Medical Facilities – Many hospitals and laboratories are equipped with state of the art machinery and work on quality standards of stem cell processing.
● Ethically Source Required Cell Sources – By using stem cells obtained from umbilical cord tissue donors, the cell sources are more ethical and biological quality is better.
● Costly Specialists – The medical team in Thailand is often internationally trained and has worked with stem cell-based therapies.
● Affordable – Therapy offering the therapy at a very low cost in comparison to Western Nation it is an economical thing to do without cutting the quality.
● Integrated Care Programs – Lifestyle strategies are a standard component of Treatment plans to improve long term outcomes including nutrition, exercise and metabolic management.
In conclusion: a new line on diabetes management
Stem cell therapy is a game changer for the Type 2 diabetic patient. This is the first time that this disease mechanism targeting approach—specifically the prevention and treatment of these key facets of metabolic dysfunction, each of which contribute uniquely to underlying inflammation, insulin resistance and beta cell dysfunction—has been shown to have potential for restoring metabolic health rather than simply controlling symptoms. In addition, it may lead to chronic disease modification by improving glycemic control in this manner.
Regenerative medicine will never be a panacea, but as our understanding of regeneration continues to ana-tomize and unfold themselves in front of us, it becomes more relevant; Modern diabetes care will inevitably require an ever-increasing toolbox. Thailand, with its sophisticated healthcare system and zero tolerance for non-innovation, is on the path of implementing these changes. If one wishes to avoid conventional treatments, you and should possibly consider arising stem cell treatment since it presents a next-generation alternative which could change the triangular of living with Kind 2 diabetic situations because that is them.

