Chronic Kidney Disease (CKD) is a progressive issue which sees a gradual decline in renal function and which in turn leads to end stage renal disease (ESRD). At present treatment options mainly put forth to stop disease progress and to manage complications but do not reverse the base tissue damage. In the field of regenerative medicine recent progress has reported the role of mesenchymal stem cells (MSCs) which include umbilical cord derived MSCs (UC-MSCs) in terms of their ability to modulate inflammation and support renal repair. Also Thailand has become a region wide hub for stem cell based therapies which it does via its specialized clinical infrastructure and integrated care models. In this article we review the pathophysiology of CKD, the flaws of current treatment practices and also we look at the role of stem cell therapy in Thailand which is put forth as an investigative approach to support kidney function.
- Introduction
Chronic Kidney Disease (CKD) is a large scale health issue which affects many around the world. This condition which sees a progressive decline in glomerular filtration rate (GFR) and also reports of kidney structure damage is very much so a global issue. Also of note is that CKD brings about great morbidity and mortality which in large part is a result of cardiovascular issues and progress to end stage renal disease. Presently available treatments which include blood pressure control, glycemic management, and use of renin–angiotensin system inhibitors do improve disease progression. But they do not reverse renal damage. Given the kidney’s low ability to regenerate, we see growing interest in which therapeutic options may support tissue repair and which may also modify disease progression. In Thailand which is home to some specialized treatment centers, stem cell based approaches are at the fore of this field.
- Pathophysiology of Chronic Kidney Disease
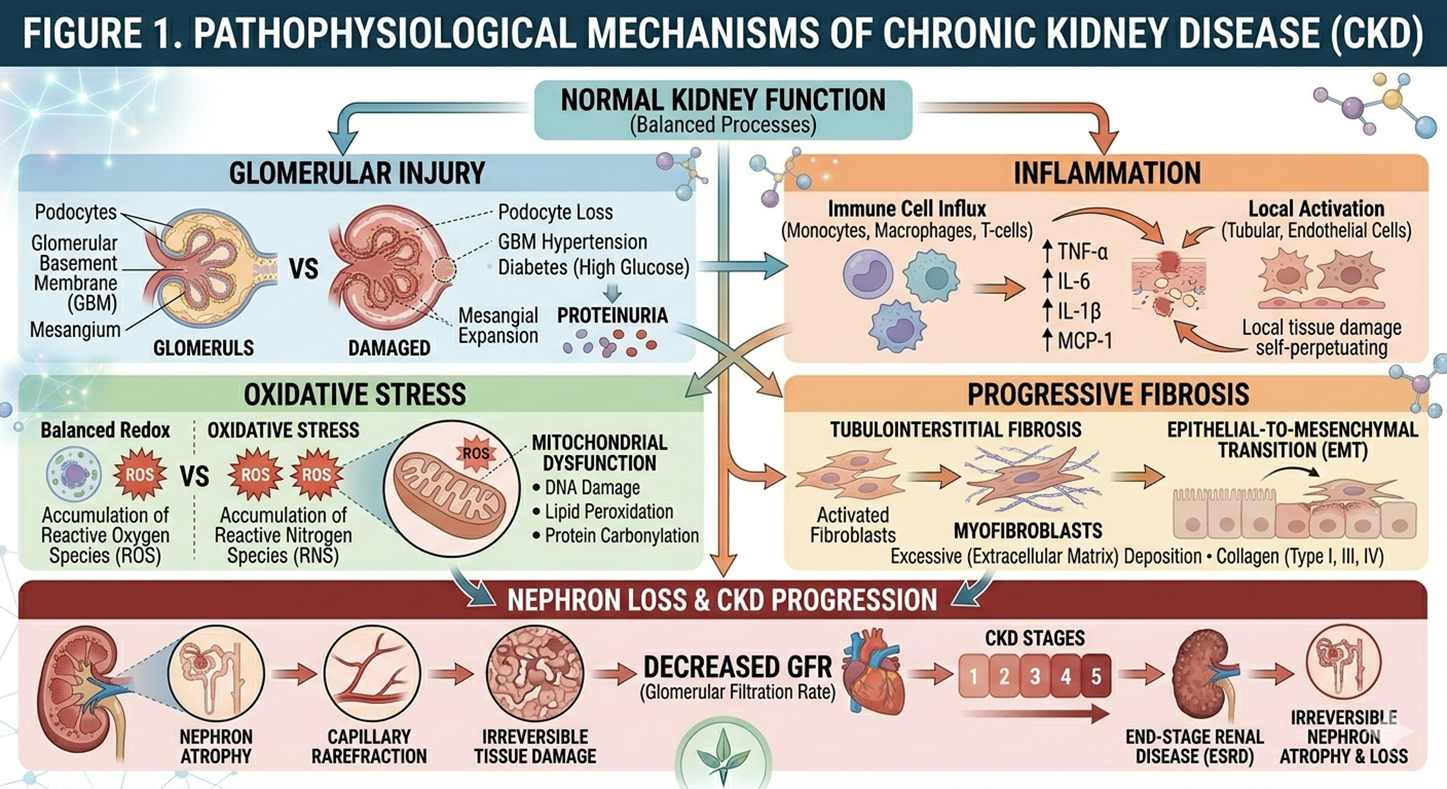
CKD is a result of a complex interaction of hemodynamic, inflammatory, and fibrotic processes which lead to gradual nephron loss.
- Renal injury to the glomeruli
At first damage presents in the glomerulus which in turn causes proteinuria and impaired filtration.
- Tubular interstitial fibrosis
Chronic injury causes the build up of extracellular matrix elements which in turn leads to fibrosis and tissue function loss.
- Swelling
Inflammation is a key player in the progression of disease and damage to tissues.
- Oxidation Stress
Increased free radical activity causes cellular injury and also aggravates fibrotic processes.
- Endothelial Insufficiency
Renal microvascular injury which in turn causes reduced oxygen delivery and more tissue damage.
These processes develop a progressive course of injury which in the end results in permanent loss of kidney function.
- Limitations of Conventional Treatment Approaches
Standard treatment of CKD is to slow disease progress and manage complications like hypertension, anemia, and electrolyte imbalance. Though these are very important measures what they do not do is to repair the actual kidney structure.
In later stages patients will see dialysis or kidney transplant as treatment options. Dialysis which is life sustaining does not however fully replace kidney function. Transplant which has better results is in short supply and requires a lifetime of immunosuppressant therapy.
Presently it is the case that we do not have at our disposal treatments which are able to regenerate damaged nephrons or to reverse fibrosis which in turn highlights the need for other approaches.
- Mesenchymal Stem Cells in Renal Regeneration
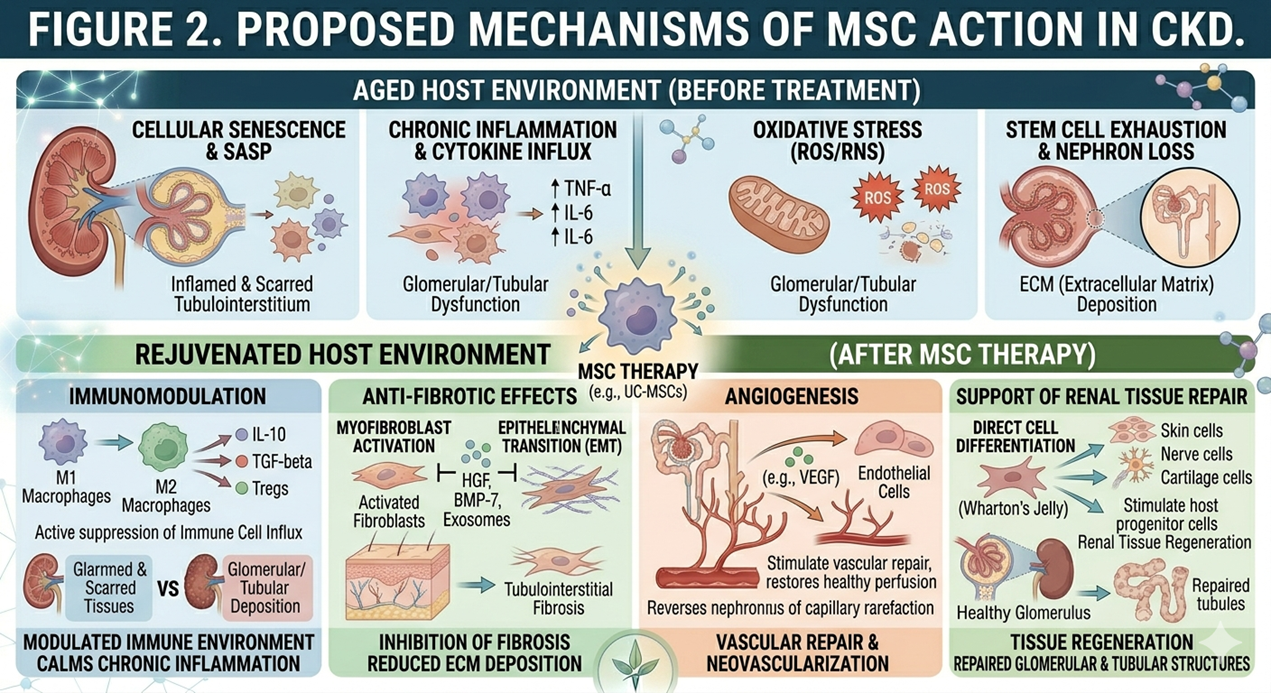
Mesenchymal stem cells (MSCs) which include those from the umbilical cord tissue (UC-MSCs) are a focus of study for what they do in renal repair. Instead of differentiating into kidney cells themselves, it is the idea that they affect change through paracrine signaling which in turn modifies the local microenvironment.
Proposed Mechanisms
- Immunoregulation : MSCs play a role in modulating immune responses and in the reduction of chronic inflammation within renal tissue.
- Fibrosis reducing effects : MSC derived factors may also suppress development of fibrosis and accumulation of extracellular matrix.
- Tumor neovascularization : Promotion of neovascularization may improve renal perfusion and oxygenation.
- Reduction in Oxidative Stress : MSC signaling may reduce the level of oxidative damage.
- Tissue Regeneration : Paracrine agents may support the survival and function of affected renal cells.
In preclinical studies we see that MSCs may play in the role of reducing inflammation and fibrosis in cases of kidney injury which reports that these findings, however the clinical picture is still very much in development.
- Clinical Applications and Thailand as a Medical Hub
Thailand has emerged as a leading player in the field of regenerative medicine which reports an array of advanced stem cell based therapies from our specialized clinics. We have state of the art laboratory infrastructure and we are committed to upholding international standards in cell processing and quality control. In clinical practice MSCs are introduced into the body systemically which is usually via intravenous injection. We aim to modulate systemic inflammation and support renal function. Early reports of which some patients had seen stabilization of renal parameters or improvement in inflammatory markers. Also Thailand is a destination for emergent regenerative therapies in which the medical expertise, technological resources, and patient centered care play a key role.
- Future Perspectives
This shift toward regenerative strategies aimed at altering progression, rather than simply treating symptoms is reflected in the use of MSC-based therapies to treat CKD.
Future research priorities include:
- Characterizing molecular mechanisms of MSC function in kidney tissue
- Identifying optimal dosing and routes of administration
- Evaluating long-term safety and efficacy
- Prioritisation of patient populations with highest likelihood of benefit
- Cell-free strategies like exosome-based therapies are also under investigation as a promising alternative.
Large-scale randomized controlled trials are required to establish the clinical utility of these therapies.
Conclusion
Chronic Kidney Disease, despite treatment advances, is persistent and progressive with few available therapies to reverse kidney tissue damage. Conventional non-biologic therapies slow disease progression but do not restore renal structure or function. First, stem cell–based approaches, especially those involving mesenchymal stem cells or bone marrow–derived progenitors, represent a promising strategy to modulate inflammatory responses and fibrosis and to promote tissue regeneration. Meanwhile, clinical applications in Thailand illustrate the increasing interest in regenerative strategies. Nonetheless, these therapies should be seen as investigational; further studies are needed to clarify their position in routine clinical practice. It will continue to evolve and play a potentially transformative role in the future advances related to novel approaches in CKD management through regenerative medicine.

