Chronic ulcerative wounds most commonly develop when the body is no longer able to efficiently heal bruised tissue due to malfunctioning internal devices. Patients often suffer from long-term pain, repeated infections, limited mobility and in extreme cases limb amputation.
Regenerative medicine was recently an emerging discipline in chronic wound care. One of the most promising developments is stem cell therapy, one of which using mesenchymal stem cells from umbilical cord tissue (UC-MSCs). Regenerative therapies target not merely to manage symptoms, but to engage the body’s normal mechanisms of self-repair and tissue such that healed tissues are structurally and functionality closer to native than synthetic or exogenous. This change, from supportive nature towards biological regrowth, is changing the treatment paradigm for chronic ulcers by clinicians.
How Stem Cells Help in Tissue Repair
Stem cells ultimately confer their few benefits, at least in regards of the wound healing mechanism via one of two mechanisms. The first form of direct organ regeneration. Stem cells are able to differentiate into the specialized and differentiated cells required to reconstitute damaged structures (e.g., skin, connective tissue, or cells lining blood vessels). These fresh cells repair the integrity of the injured area.
The second mechanism is related to paracrine signaling. Stem cells secrete a wide range of bioactive molecules and factors to impact adjacent cells (including growth factors, cytokines and chemokines). These signaling molecules provoke neighboring tissues to engage in repair, control inflammation and boost immune reaction. And even without permanently integrating into the tissue, the molecules that stem cells secrete may work wonders to speed healing.
How Stem Cell Therapy Aids the Healing of Ulcers
Regenerating Damaged Tissue: Stem cells can differentiate into all types of skin-related cells. This encompasses fibroblasts (which create connective tissue components including collagen), keratinocytes (which make up the skin’s outer protective layer), and endothelial cells, which can help form new blood vessels. These essential cell types provided by stem cells then rebuild the inside of ulcerated tissue outward.
Enhancing Blood Supply: Stem cells release growth factors, including vascular endothelial growth factor (VEGF), that stimulate the generation of new capillaries. Simplifying angiogenesis process enhance blood flow in degenerative site and aestablish quick recovery time.
Decrease Chronic Inflammation: Through the production of anti-inflammatory molecules like cytokines (interleukin-10 and also transforming growth factor beta) by stem cells. These compounds also regulate the hyper-inflammatory phase and push the wound environment from a damaging phase to a tissue repair stage.
Immune Maintenance: Macrophages and T lymphocytes also interact with stem cells. By such interactions they regulate immune exertion, enhancing the body’s ability to clear infection but preventing damaging over-activity that would otherwise prevent healing.
Revitalizing the local repair mechanisms: The signaling molecules from stem cells can stimulate nearby skin and connective tissue cells. They then release signals that promote the local cells to divide, move towards the area of damage and help to rebuild tissue. Thus, stem cells play a role of biological conductors directing the entire healing process.
Putative Antimicrobial Properties: Certain studies imply that stem cells have antimicrobial peptides that could be active against particular pathogens. These properties can inhibit infections and promote more rapid healing of wounds.
A : Stem cells may assist in ulcer healing through enhancement of tissue repair and stimulates improvements in local circulation, reduction in inflammation, balancing the immune system or by activating regenerative processes.
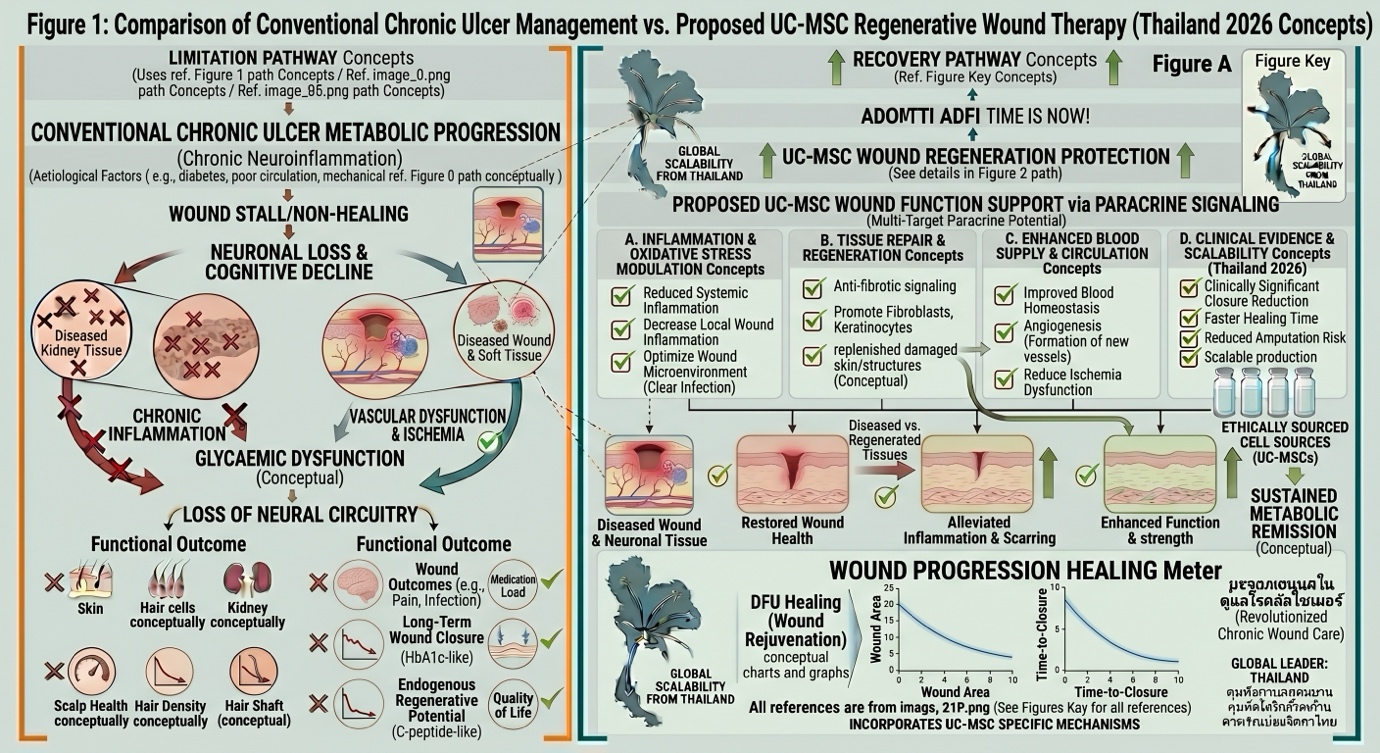
Benefits of Regenerative Stem Cell Therapy
These stem cell-based treatments provide significant advantages over traditional wound treatment.
Promoting full-thickness tissue regeneration is one significant benefit you get. Key advantage of stem cells is that instead of just excising necrotic tissue, they assist in restoring skin and subcutaneous structures. This process can enhance the healing region in terms of function and strength.
Another benefit is reduced scarring. Stem cells play an important role not only in cellular differentiation but also in how organized tissue formation occurs when skin is regenerated, the new skin tends to be relatively more natural and flexible, thereby reducing the formation of fibrotic scars.
Having a speedier recovery diminishes the danger of contamination and different difficulties too. Even more important, wounds close quicker and become less susceptible to invading microorganisms. Regenerated tissue may also be stronger and have greater resistance which would reduce the likelihood of ulcer reformation.
Indeed, in the worst cases, regenerative therapies might even save limbs from amputation by remedying vascular dysfunctions and tissue structure before irreversible damage has occurred.
Research and Clinical Evidence
From the perspective of stem cell therapy for chronic wounds, favorable results were shown with clinical studies. Stem cell treatment has been shown to facilitate quicker wound closure, improve tissue structure, and decrease ulcer size in patients with diabetic foot ulcers and venous leg ulcers in a few early-phase clinical trials.
Higher healing rates in patients receiving regenerative treatments than with comparison to conventional care have been found meta-analyses on stem cell therapy data. Significantly, these studies have also indicated good safety records when stem cellsare given in the appropriate supervised medical setting.
Studies dedicated specifically to pressure ulcers have also shown increased vascularization and regeneration for stem cell therapy, revealing promise in its application among various wound types.
Conclusion
Stem cell therapy is a tremendous advancement in the management of chronic ulcers. While infection control and wound management will continue to be a critical part of treatment, regenerative medicine targets the biological issues that inhibit healing. Stem cells reactivate the body’s natural repair mechanisms by promoting the growth of blood vessels, reduction of inflammation, restoration of tissue structure and regulation of immune responses.
Stem cell based therapies-the near future with ongoing research and advancing clinical techniques, stem cell-based therapies will continue to play a vital role in wound care. These interventions have the ability to hasten healing time, minimize complications, conserve limb and more importantly improve functional outcomes among the chronic ulcerative conditions.

