Clinical Uses of Plant-Based Stem Cell Therapy for Treatment of Chronic Diabetic Wounds
The global increase of metabolic disorders has led to an alarming number of non-healing ulcerations known as Diabetic Wounds. These wounds indicate systemic failure of the body’s integrated healing processes. Chronic hyperglycemia creates an adverse metabolic environment for all cell activities, resulting in a chronic state of impaired healing, which can last for years. This clinical condition is severe, often resulting in deep tissue necrosis and the eventual need for lower limb amputation. Physically devastating, a patient may suffer chronic pain and a considerable emotional burden. Because traditional medical approaches have proven to be fundamentally insufficient in addressing cellular exhaustion, there is an urgent need for advanced regenerative therapies. Plant-Based Stem Cell Therapy offers a sophisticated solution by providing unique bioactive signaling molecules that can effectively ‘turn on’ the dormant biological pathways for complete tissue closure.
- fundamental pathophysiology of chronic Diabetic Wounds
The fundamental pathophysiology of chronic ulceration involves a multifaceted breakdown of the inflammatory and proliferative stages of skin healing. With a healthy individual, an injury triggers a prompt response by macrophages to clear cellular debris. For the individual with persistent hyperglycemia, the site of the injury becomes stuck in a chronic inflammatory cycle. The Diabetic Wounds microenvironment is filled with damaging inflammatory cytokines and reactive oxygen species that severely damage the DNA and cell membranes. Additionally, the local blood micro vessels undergo microvascular changes which further exacerbate the inefficient delivery of critical oxygen. Localized hypoxia primarily restrains the action of fibroblasts in synthesizing collagen which is critical for the structural integrity of skin. On the other hand, the injury remains open which greatly increases the risk for developing a bacterial biofilm while also being unresponsive to the body’s own restorative signals. This creates a bad environment due to the fact that this is where cell death is greater than the formation of new tissue.
- standard therapy methods and Limitations on Diabetic Wounds
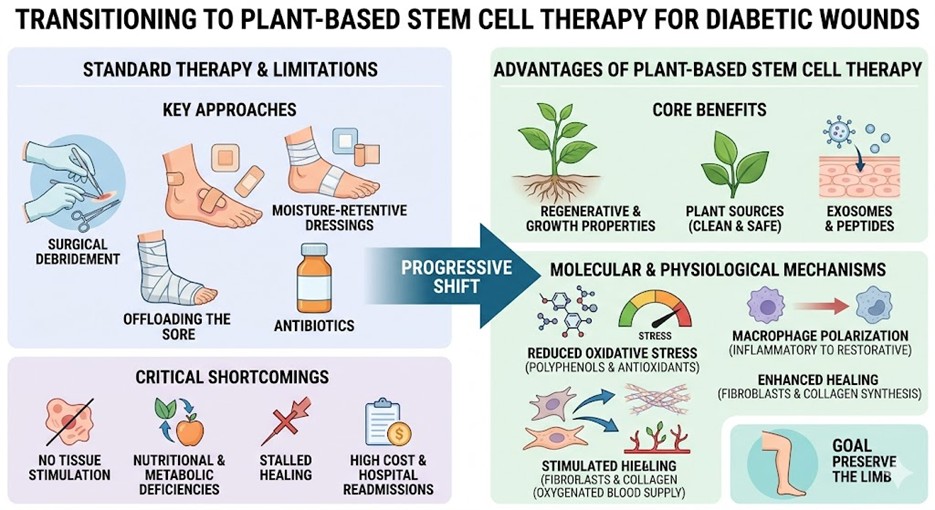
From the outset, the management of these complex conditions has relied on standard therapy methods that focus on care in a more active sense. Surgical debridement to remove dead tissue and leave a clean bed for new tissue and moisture-retentive dressings (collagens and hydrocolloids) are the main constructive therapies for the management of these complex and chronic Diabetic Wounds. Offloading the sore and administering antibiotics are also used to reduce the risk of infection. Despite the arduous efforts of the healthcare professionals, the limitations of their methods are enormous. For example, standard dressings do not stimulate healing as do bioengineered tissues, and they do not address the underlying tissue nutritional and metabolic deficiencies at the cellular level. As a result, many patients suffer extended periods of time in a state of chronic wound, only to witness the Diabetic Wounds healing process come to a complete standstill. The cost of chronic Diabetic Wounds care is enormous and the inability to ever achieve complete closure of the Diabetic Wounds, often results in repeated admissions to hospital. The inability to demonstrate the effectiveness of the therapy is the justification for a progressive shift to modern therapies in regenerative medicine in the hope to preserve the limb for a prolonged period.
3.The innovative application of Plant-Based Stem Cell Therapy
The transition to Plant-Based Stem Cell Therapy is based on the unique regenerative and growth properties of plant cells due to the fact that they are able to survive and rejuvenate in extreme conditions. Plant sources, as opposed to cell sources of animals which may carry immunological risks, also offer a clean and safe source of regenerative signals. The process involves the use of specific exosomes and peptides that interact with human skin cells. The phytochemical signals reduce the high oxidative stress of Diabetic Wounds due to the high number of polyphenols and natural antioxidants. At the molecular level, these agents stimulate macrophage polarization from a pathologically destructive inflammatory process to one that is restorative. This change in process enhances healing by enabling the rapid influx of new fibroblasts and better collagen synthesis. The botanical extracts also stimulate angiogenesis to ensuring that the newly formed tissue is adequately supplied with oxygenated blood.
- New regenerative Diabetic Wounds medicine approaches in Thailand
The domain of advanced medicine is rapidly changing with a clear worldwide preference for the application of integrated biotechnology in this region. With a focus on the clinical aspects of metabolic health, Thailand has one of the best systems in the region. This high burden of diabetes in this region ensures that there is a good opportunity for the application of new regenerative Diabetic Wounds medicine approaches in Thailand. In addition to the highly qualified personnel, the good regulatory framework in Thailand for the application of advanced biotechnology ensures that people from anywhere in the world can access Plant-Based Stem Cell Therapy with a high level of safety. The focus of state-of-the-art dedicated research centers for advanced extraction techniques to this area ensures that the quality of Plant-Based Stem Cell Therapy is maintained at the highest level. This ensures that the application of modern regenerative medicine is not only possible but highly effective for those at ongoing risk of limb loss.
In summary, protective measures for chronic metabolic ulcers must evolve into active biological solutions. Addressable proprietary technology that diverts the ill-defined, but clearly mapped, pathways of the bottom-up molecular framework of Diabetic Wounds is revolutionary. It equips today’s physician with the means to achieve closure. Plant-Based Stem Cell Therapy is the first integrative pathway of the Plant Kingdom and modern molecular biology targeted at stimulating cell regeneration. As these therapies develop, clinical outcomes for patients will improve, especially in medically innovative countries like Thailand. The aim is to achieve the restoration of the integument and with it, the patient’s functional and physiological well-being, free from the burdens of chronic Diabetic Wounds sequelae. The advancement of these therapies will not only save limbs, but also honor the humanity that chronic illness consumes.

