Why does this topic need more precision than most articles give it
- Crohn’s disease is already a regeneration problem, but not in the simple way people imagine
When people search Natural Cellular Regeneration in relation to Crohn’s disease, they are usually reacting to the same hard reality: Crohn’s is chronic, inflammatory, and often unpredictable. It can affect any part of the digestive tract from the mouth to the anus, and over time it may lead to complications such as fistulas, abscesses, obstruction, malnutrition, and repeated flares that interrupt normal tissue repair. That is why regenerative language becomes so attractive. But in Crohn’s disease, regeneration is not just about “growing new tissue.” It is about trying to calm immune-driven injury while also helping damaged tissue heal in a hostile inflammatory environment.
That distinction matters because Natural Cellular Regeneration is not a formal Crohn’s treatment category. It is better understood as a framework for thinking about whether cell-based therapies can restore some balance to a system that keeps injuring itself. In the stem-cell literature, the interest is not only that cells might replace damaged tissue directly. It is also possible that they may exert immunomodulatory, anti-inflammatory, and wound-healing effects that could support mucosal or fistula repair. That is a much more accurate and much more interesting way to frame the topic.
- The strongest evidence is not spread evenly across the disease
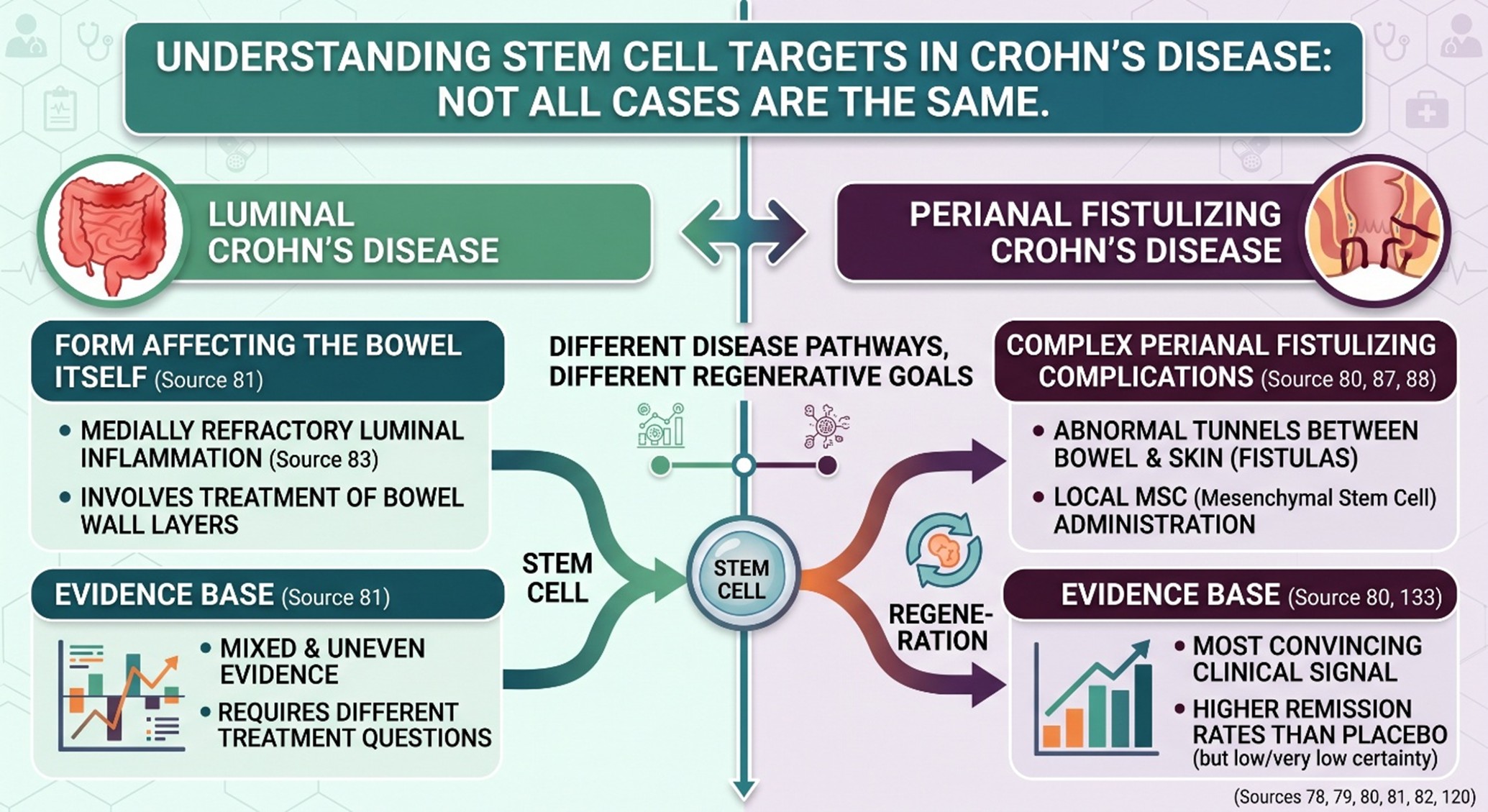
One of the biggest mistakes in online writing is treating all Crohn’s disease stem-cell research as one thing. It is not. The most convincing clinical signal has been in complex perianal fistulizing Crohn’s disease, where local mesenchymal stem/stromal cell approaches have been studied as a way to promote fistula healing while reducing damage to the sphincter. By contrast, luminal Crohn’s disease, the form affecting the bowel itself, has a more mixed evidence base and involves very different treatment questions.
That difference gives the article its first real layer. If someone says stem cells “work in Crohn’s,” the immediate follow-up should be: which Crohn’s problem? A patient with chronic perianal fistulas is not facing the same biological challenge as someone with medically refractory luminal inflammation. The literature increasingly reflects that split, and good SEO writing should too.
Natural Cellular Regeneration in perianal Crohn’s disease
- Why fistulas became the most important testing ground
Perianal fistulas are one of the most difficult complications of Crohn’s disease. They are abnormal tunnels that can become infected, recur, and significantly affect quality of life. Because surgery alone can be difficult and may risk continence depending on anatomy, regenerative approaches have drawn particular interest here. The 2024 ECCO surgical therapeutics guideline states that, in complex perianal fistulae, stem cells can be an alternative in selected cases, especially when fistula anatomy is challenging.
This is where Natural Cellular Regeneration becomes concrete rather than abstract. In fistulizing disease, the goal is not to regenerate an entire intestine. It is to support local healing of a chronically inflamed tract. A meta-analysis from the year 2025 that looked at MSC-based therapies for perianal fistulizing Crohn’s disease included 596 patients from 25 studies, and looked at three-, six-, and twelve-month remission rates. Contrasted with placebo in randomized trials, MSC-based therapy showed a significantly higher remission rate at both three and six months, but the evidence was judged low to very low for certainty. A meta-analysis of adipose-derived stem cell therapies for complex anal fistula from the year 2025, which encompasses 1,056 patients from five randomized trials, yielded better long-term and short-term clinical outcomes than conventional control groups. That is not to say it is over, but it does point up why the clinical area where stem-cell treatments for Crohn’s fistula repair is most at home.
- Why the darvadstrocel story matters
The darvadstrocel story is important because it shows how serious this field has become, and how disciplined interpretation still needs to be. Early trials helped establish allogeneic adipose-derived MSCs as a credible option for complex Crohn’s perianal fistulas. But in December 2024, the European Medicines Agency announced that Alofisel had been withdrawn from the EU market because the available data were considered insufficient to confirm benefit, and no new patients were to be treated after 13 December 2024. That is one of the clearest reminders that regenerative medicine can be promising and still face major evidence hurdles.
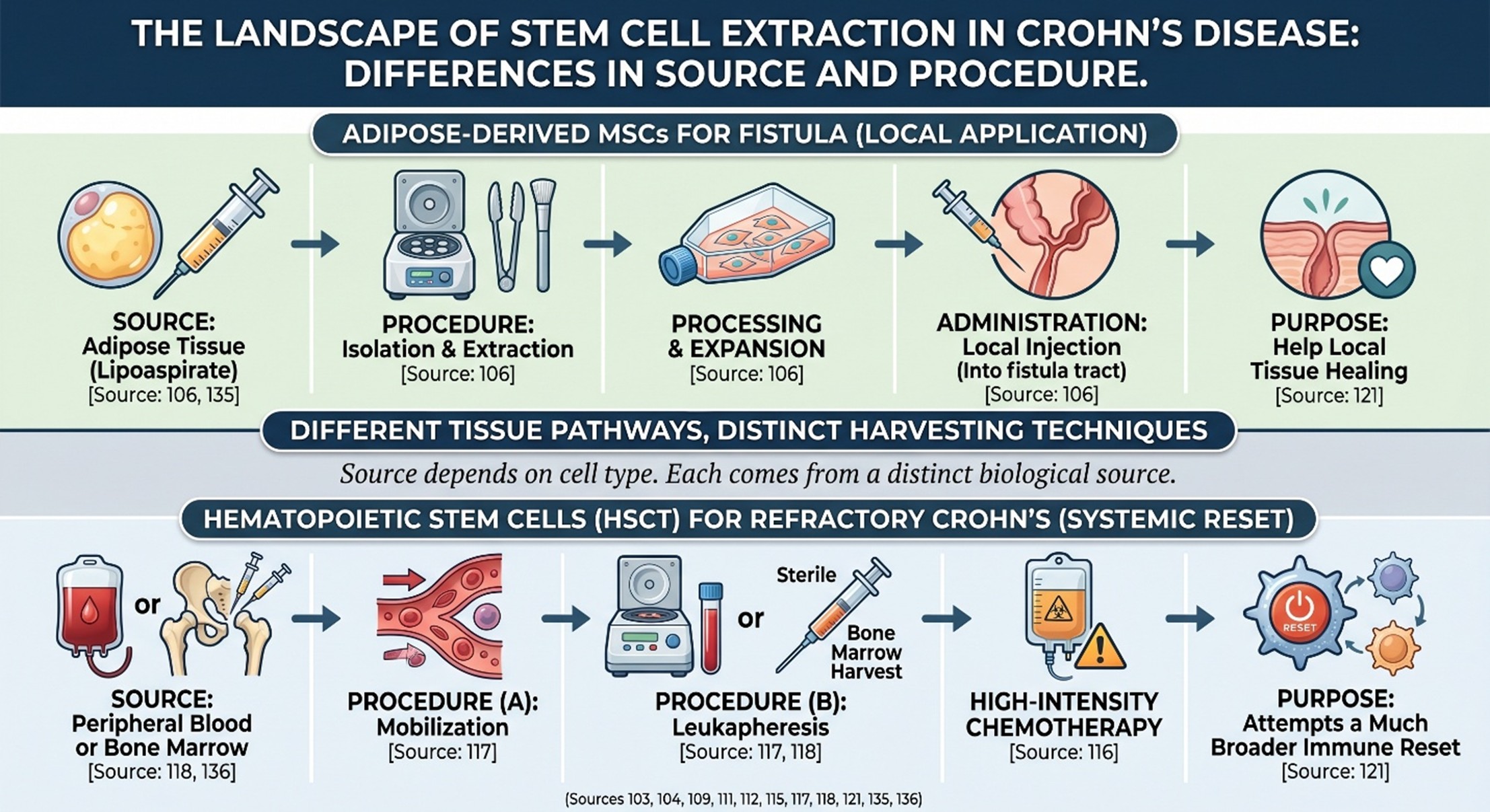
- Stem cell extraction is source-dependent, not a universal procedure.
The keyword stem cell extraction sounds simple, but in real medicine, it depends entirely on the kind of stem cell being discussed. In Crohn’s perianal fistula research, many studies focus on adipose-derived mesenchymal stem cells. These are obtained through isolation and extraction from adipose tissue, often from lipoaspirate, and then processed or expanded before local administration. In other words, the extraction method is tied to the tissue source and manufacturing pathway, not just to the word “stem cell.”
This matters as it determines whether or not readers are misled to imagine that all stem-cell therapies have one kind of picking technique. They don’t. Adipose-derived cells, bone-marrow-derived cells, and hematopoietic stem cells each come from distinct biological sources and are harvested differently. Thus, when someone searches for stem cell extraction for Crohn’s disease, what they generally want is not a generalized response, but a kind of hinted understanding about just exactly what sort of cell is being used and for what reason.
A very different world: hematopoietic stem cell transplantation
- This is not the same as local MSC treatment
There is another stem-cell pathway in Crohn’s disease, but it belongs to a different category altogether: autologous hematopoietic stem cell transplantation. This has been studied in refractory Crohn’s disease, especially in people who have failed multiple conventional and biologic therapies. Mechanistically and clinically, this is a much more intensive strategy than local MSC treatment for fistulas. It involves stem-cell collection, high-intensity immunosuppressive therapy, and then reinfusion of collected cells.
Here, stem cell extraction usually refers to the collection of hematopoietic stem cells after mobilization into the bloodstream, followed by leukapheresis. The 2024 EBMT Handbook describes peripheral hematopoietic stem-cell collection by leukapheresis as a well-established process, while bone marrow harvesting remains another possible source, obtained through repeated aspirations from the iliac crests under sterile conditions and anesthesia. That is a very different clinical reality from the local adipose-derived MSC procedures discussed in perianal Crohn’s disease.
The takeaway is simple but important: not all stem-cell strategies in Crohn’s disease are variations of the same idea. One aims to help local tissue healing in fistulas. The other attempts a much broader immune reset in highly selected refractory disease. When articles blur these together, they make the field sound clearer than it really is.
The most honest conclusion
- Crohn’s disease may be one of the better examples of both the promise and the limits of regenerative medicine.
As a matter of fact, if you are looking for a realistic view of natural cellular regeneration in Crohn’s disease, this is probably it: science is sound, logical therapeutics are feasible, and the best thus far clinical evidence lies in complex perianal fistulas treated with a mesenchymal stem/stromal cell approach. On the other hand, the field is still uneven, and even one of its best-known commercial examples lost EU authorization after a confirmatory benefit could not be demonstrated. That makes Crohn’s disease an instructive example of regenerative medicine should be: Considerately, with an eye to detail, and there’s no need to pretend that all stem-cell pathways have already fallen within standard care.
Frequently Asked Questions
1) What does Natural Cellular Regeneration mean in Crohn’s disease?
In this context, it refers to the idea that cell-based therapies may help repair tissue and rebalance inflammation in Crohn’s disease. It is not a formal diagnosis or a guarantee of tissue replacement, but a way of describing regenerative and immunomodulatory treatment strategies being studied in the disease.
2) Where is stem-cell evidence strongest in Crohn’s disease?
The strongest clinical evidence is in complex perianal fistulizing Crohn’s disease, where mesenchymal stem/stromal cell therapies have shown better remission outcomes than placebo or conventional treatment in recent meta-analyses.
3) What does stem cell extraction usually mean here?
It depends on the cell type. For adipose-derived MSCs, it usually means isolating cells from adipose tissue or lipoaspirate. For hematopoietic stem-cell transplantation, it usually means mobilizing blood stem cells and collecting them by leukapheresis, or, in some cases, obtaining them from bone marrow harvest.
4) Is Darvadstrocel still available in the EU for Crohn’s fistulas?
No. EMA announced that Alofisel was withdrawn from the EU market in December 2024 because the available data were considered insufficient to confirm benefit, and no new patients should be treated after 13 December 2024.
5) Is hematopoietic stem-cell transplantation the same as local MSC therapy for fistulas?
No. They are very different approaches. Local MSC therapy is mainly studied for fistula healing, while autologous hematopoietic stem-cell transplantation is a far more intensive strategy studied in highly refractory Crohn’s disease.

