Stem Cell Therapy for Diabetes Mellitus Type 2 at Stem Cell Clinic Thailand
1.Introduction and the Urgency for Novel Intervention
Diabetes Mellitus Type 2 has emerged as a primary global health crisis that places an immense burden on modern medical infrastructure. This metabolic condition is characterized by chronic hyperglycemia resulting from a combination of insulin resistance and the progressive failure of pancreatic β-cells. While lifestyle modifications and oral medications serve as the initial line of defense, the degenerative nature of the disease often leads to long-term systemic damage. Patients frequently face debilitating complications such as nephropathy, neuropathy, and cardiovascular diseases which severely diminish quality of life. The necessity for a novel therapeutic approach arises because current pharmacological interventions merely manage symptoms rather than addressing the underlying cellular degradation. Emerging research suggests that advanced regenerative medicine, particularly through a specialized Stem Cell Clinic Thailand, offers a transformative path by targeting the root causes of metabolic dysfunction rather than just masking high glucose levels.
2.Pathophysiology of Diabetes Mellitus Type 2
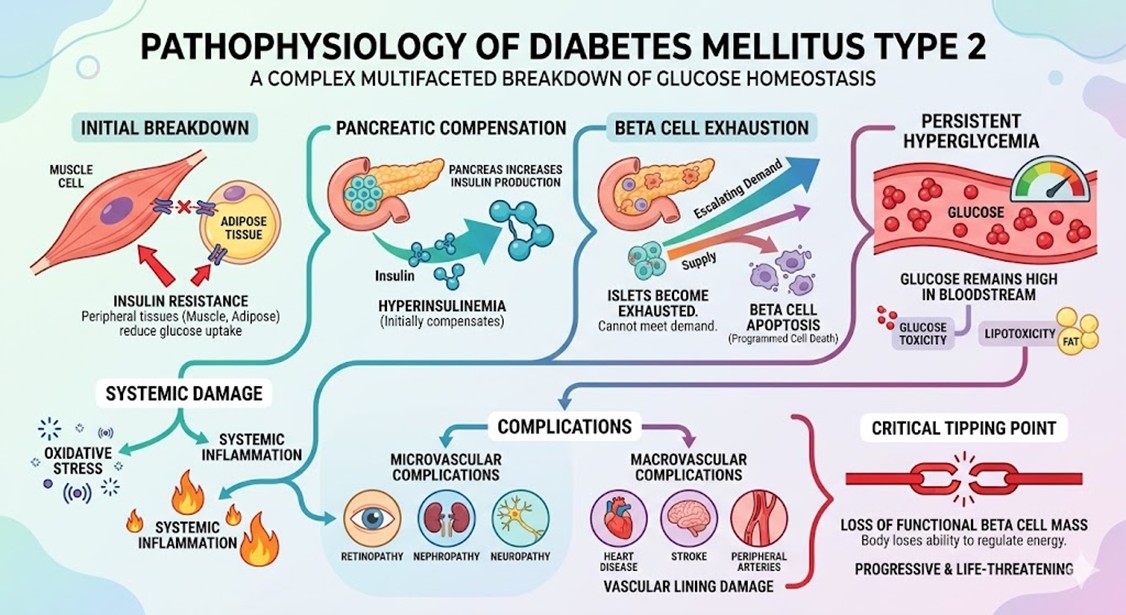
The pathophysiology of Diabetes Mellitus Type 2 is complex and involves a multifaceted breakdown of glucose homeostasis. Initially, the body develops resistance to insulin, a hormone vital for glucose uptake in peripheral tissues like muscles and adipose tissue. To compensate, the pancreas increases insulin production, leading to hyperinsulinemia. However, over time, the pancreatic islets become exhausted and cannot meet the escalating demand. This leads to glucose toxicity and lipotoxicity, which further accelerate β-cells apoptosis or programmed cell death. As the concentration of glucose in the bloodstream remains persistently high, it triggers oxidative stress and systemic inflammation. These biological processes damage the vascular lining, leading to the microvascular and macrovascular complications that define the severity of the disease. The loss of functional β-cells mass is the critical tipping point where the body loses its innate ability to regulate energy, making the condition a progressive and life-threatening struggle for millions.
3.Conventional Treatments and Their Inherent Limitations
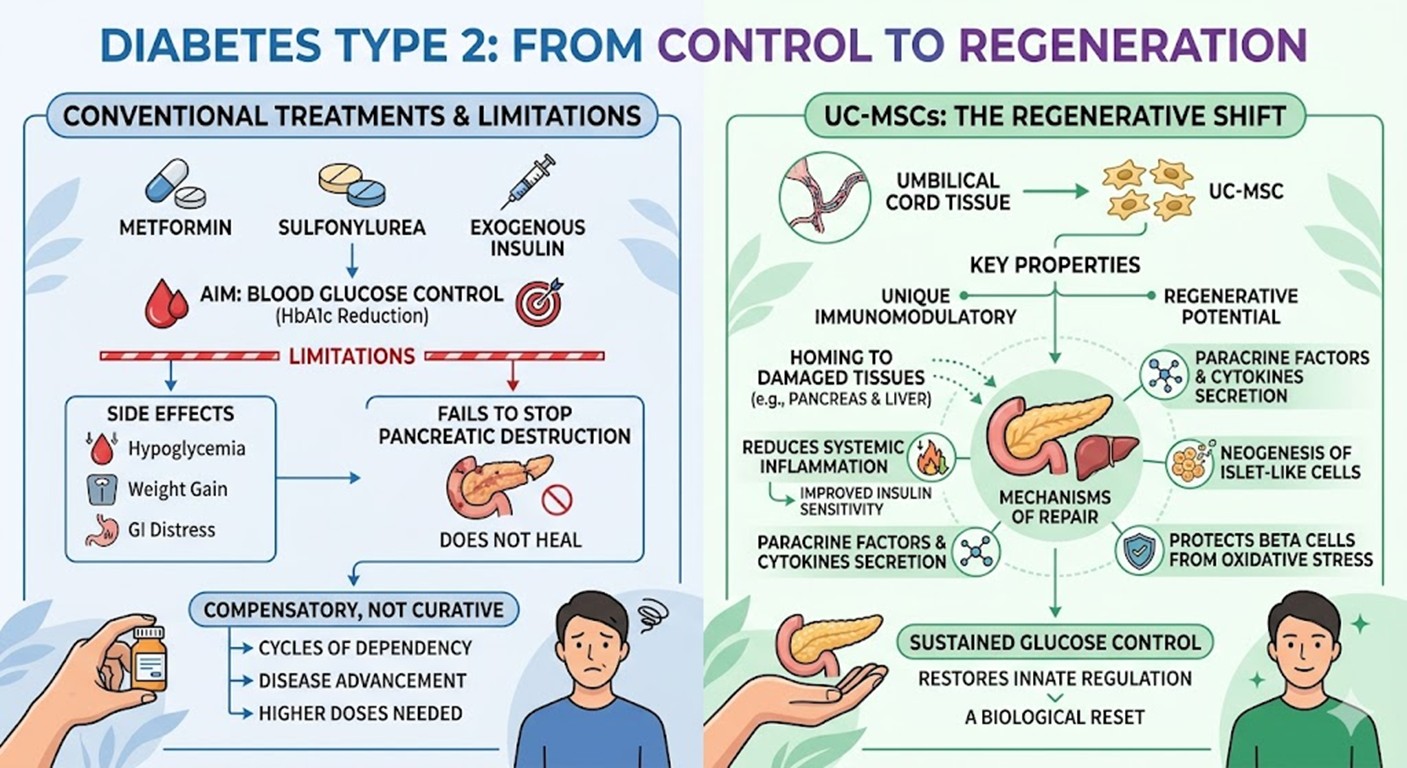
Current standard care for Diabetes Mellitus Type 2 focuses on maintaining blood glucose within a target range. This typically involves a sequence of metformin, sulfonylureas, and eventually exogenous insulin injections. While these methods are effective at lowering HbA1c levels in the short term, they come with significant limitations and side effects. Many patients experience hypoglycemia, weight gain, and gastrointestinal distress. More importantly, traditional medications do not stop the ongoing destruction of the pancreas. They are compensatory rather than curative. As the disease advances, many patients find that their bodies become increasingly unresponsive to these drugs, necessitating higher doses and more frequent monitoring. This creates a cycle of dependency on pharmaceutical products that fails to restore the natural physiological balance of the body. The inherent inability of traditional medicine to regenerate damaged tissues has pushed researchers to look toward cellular therapies.
4.The Role of UC-MSCs in Regenerative Medicine
The shift toward using umbilical cord-derived mesenchymal stem cells, or UC-MSCs, represents a major leap in regenerative science. At a leading Stem Cell Clinic Thailand, this therapy is utilized because of its unique immunomodulatory and regenerative properties. Unlike standard treatments, UC-MSCs have the ability to home in on damaged tissues, such as the pancreas and liver, to initiate repair. The primary mechanism involves the secretion of paracrine factors and cytokines that reduce systemic inflammation, which is a key driver of insulin resistance. Furthermore, these stem cells can promote the neogenesis of islet-like cells and protect existing β-cells from oxidative stress. By modulating the immune system, MSCs help reduce the autoimmune-like inflammatory environment surrounding the pancreatic islets, allowing the body to regain some of its natural insulin-producing capacity. This biological reset targets the metabolic environment at a molecular level, offering a chance for sustained glucose control that pills and injections simply cannot provide.
5.Future Outlook and Thailand as a Medical Hub
Thailand has positioned itself as a premier destination for these advanced biological treatments due to its robust regulatory framework and world-class medical facilities. The future of using MSCs for Diabetes Mellitus Type 2 in the region is incredibly promising, as clinical data continues to demonstrate safety and efficacy. Choosing a Stem Cell Clinic Thailand provides patients access to cutting-edge technology combined with highly skilled medical professionals who specialize in regenerative protocols. The country has invested heavily in biotechnology and specialized laboratories, ensuring that the quality of cultivated cells meets international standards. Moreover, the integration of holistic care with cellular therapy in Thailand offers a comprehensive recovery environment that is difficult to find elsewhere. As global interest in longevity and regenerative medicine grows, Thailand continues to lead the way in making these sophisticated therapies accessible to those who have exhausted traditional options.
In summary, the transition from symptom management to cellular regeneration marks a significant milestone in the fight against Diabetes Mellitus Type 2. While conventional therapies remain the cornerstone of initial care, their limitations in stopping disease progression are evident. The application of mesenchymal stem cells offers a sophisticated biological solution that addresses insulin resistance and β-cells loss through complex immunomodulatory pathways. By visiting a specialized Stem Cell Clinic Thailand, patients can explore a future where their health is not defined by constant medication but by the body’s own enhanced ability to heal. This evolution in medical science promises a more sustainable and effective way to manage metabolic health, potentially halting the complications that have traditionally made this disease so devastating. As research continues to validate these methods, the role of regenerative medicine will undoubtedly become central to modern endocrinology.

