Type 1 diabetes mellitus (T1DM) is a chronic autoimmune disease in which the body’s immune system mistakenly attacks and destroys the insulin-producing beta (β) cells located in the pancreas.
For most individuals living with Type 1 diabetes, treatment relies on lifelong insulin replacement through daily injections or insulin pumps. Although these therapies help regulate blood glucose levels, they do not repair the damaged pancreas or address the autoimmune process that caused the disease in the first place.
Recent developments in regenerative medicine have introduced new possibilities for treating autoimmune diseases such as Type 1 diabetes. Among these emerging approaches is stem cell therapy, particularly treatments involving umbilical cord–derived mesenchymal stem cells (UC-MSCs). These specialized cells possess regenerative and immune-regulating properties that may help restore pancreatic function while simultaneously reducing the autoimmune activity responsible for β-cell destruction.
The Objectives of Regenerative Therapy in Type 1 Diabetes
Stem cell therapy for Type 1 diabetes aims to go beyond simple blood glucose management. Instead, the goal is to repair or regenerate pancreatic tissue and restore the body’s natural ability to produce insulin. Achieving this requires addressing multiple aspects of the disease simultaneously.
The first objective involves regenerating or replacing damaged β-cells. Because insulin-producing cells are essential for maintaining normal glucose levels, restoring a healthy population of these cells is critical. Stem cells may support this process by stimulating new cell growth or by differentiating into insulin-producing cells.
The second objective focuses on regulating the immune system. Since Type 1 diabetes is caused by an autoimmune attack, it is essential to calm or reprogram immune responses that target β-cells. Effective immune modulation can help prevent newly regenerated cells from being destroyed again.
The third goal is to improve the pancreatic microenvironment. A supportive tissue environment is necessary for cell survival and regeneration. This includes improving blood flow to pancreatic tissues, reducing inflammation, and ensuring that newly formed cells receive adequate nutrients and oxygen.
By addressing these three components—cell regeneration, immune balance, and tissue support—regenerative therapies aim to restore pancreatic function rather than simply compensate for its loss.
Mechanisms of Stem Cell Therapy in Type 1 Diabetes
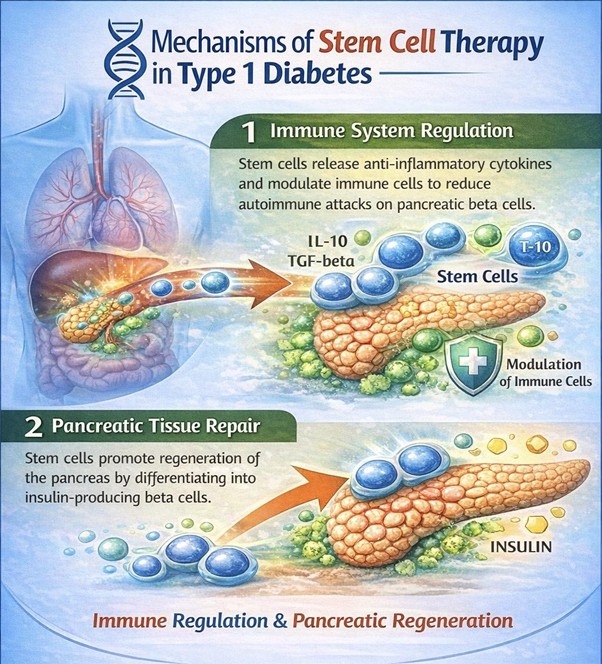
Immune System Regulation: Stem cells help rebalance immune function by promoting regulatory pathways that reduce destructive immune activity.
They encourage the expansion of regulatory T cells, which suppress autoimmune reactions and maintain immune tolerance. At the same time, they inhibit the activation of inflammatory T helper cells and cytotoxic lymphocytes that specifically target pancreatic β-cells.
Stem cells also release immunomodulatory molecules such as cytokines and transforming growth factor beta (TGF-β). These substances reduce excessive immune activation and help restore a balanced immune environment.
Pancreatic Tissue Repair: Stem cells support the regeneration and survival of pancreatic cells. Much of this effect occurs through paracrine signaling, a process in which stem cells release biologically active molecules that influence nearby tissues.
These signaling molecules can stimulate existing β-cells to survive and function more effectively. They may also activate dormant precursor cells within the pancreas, encouraging them to develop into insulin-producing cells.
Stem cells also contribute to improved vascular health by stimulating the formation of new blood vessels. Increased circulation enhances oxygen and nutrient delivery to pancreatic tissues, supporting the regeneration process.
By reducing local inflammation and oxidative stress, stem cell therapy helps create a healthier environment that allows pancreatic cells to recover and maintain their function over time.
Clinical Use of Stem Cell Therapy in Thailand
Thailand has become an increasingly recognized center for regenerative medicine and advanced medical treatments. The country offers modern healthcare facilities, experienced medical specialists, and laboratories that follow strict international standards for stem cell processing.
Stem cell therapy in Thailand typically begins with the ethical sourcing of umbilical cord tissue from voluntary donors. The collected cells are isolated, purified, and expanded in specialized laboratories operating under Good Manufacturing Practice (GMP) conditions. These strict protocols ensure that the cells meet safety and quality standards before being used in medical procedures.
Patients undergoing treatment are carefully monitored through laboratory testing and medical evaluations. Physicians may measure C-peptide levels to assess natural insulin production, track HbA1c values to monitor long-term glucose control, and analyze immune markers to evaluate changes in immune activity.
Regenerative treatment programs in Thailand often integrate supportive therapies as well. Nutritional counseling, lifestyle guidance, and metabolic monitoring are commonly included to help patients maintain overall health and improve treatment outcomes.
Potential Benefits of Stem Cell Therapy for Type 1 Diabetes
Stem cell therapy offers several potential advantages compared with conventional diabetes treatments. One key benefit is the possibility of restoring natural insulin production, which could reduce reliance on daily insulin injections.
Another important advantage is that stem cell therapy targets the underlying causes of the disease. By addressing both immune dysfunction and pancreatic damage, it aims to treat the root mechanisms of Type 1 diabetes rather than focusing only on symptom control.
Clinical studies involving stem cells have generally demonstrated strong safety profiles when procedures are performed in controlled medical environments. Additionally, because umbilical cords provide a sustainable and ethically sourced supply of stem cells, the therapy can be developed without invasive collection methods.
Conclusion
Stem cell therapy represents a promising advancement in the treatment of Type 1 diabetes. By combining immune regulation with regenerative capabilities, this approach seeks to rebuild the population of insulin-producing β-cells and restore balance within the immune system.
Thailand has emerged as an important hub for the development and application of these therapies, supported by advanced medical infrastructure and growing expertise in regenerative medicine. Stem cell–based interventions may one day transform the management of Type 1 diabetes.
Rather than focusing solely on controlling blood sugar, regenerative medicine aims to repair the body’s natural systems and restore metabolic harmony—offering new hope for individuals living with this lifelong condition.

