Beyond Conventional Kidney Care: Stem Cell Therapy in Thailand
Their KOOB-05 research team report that acute kidney injury (AKI) and chronic kidney disease (CKD) are among the most important health problems on Earth. Standard medical therapy primarily influences conditions by slowing the progression of disease and between written etiquette, but not overall policy implementation.
Regenerative medicine represents a new concept for treating kidney diseases that has only surfaced over the past five years. One of those is a novel, sophisticated method using MSCs, UC-MSC stem cells specifically sourced from umbilical cord tissue. These cells have TOE biological properties that enable tissue repair, modulation of immune function and inflammation, and promotion of healing in injured organs.
Activity mechanisms underlying the involvement of stem cells in kidney repair
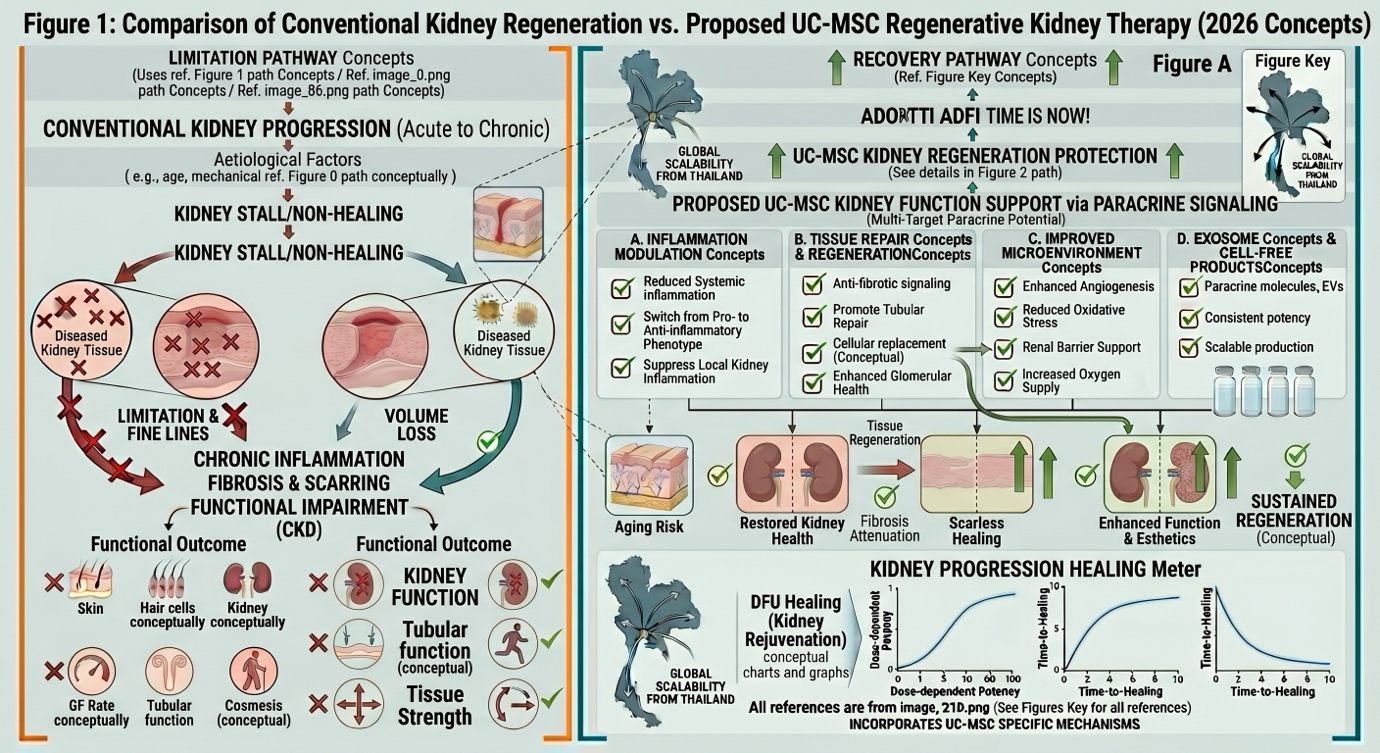
Figure 1: Comprehensive Comparison of Conventional Kidney Progression vs. UC-MSC Regenerative Therapy (2026 Concepts), highlighting paracrine signaling mechanisms in attenuating inflammation, promoting tubular repair, and restoring Glomerular Filtration Rate (GFR)
Regulates Immune System: Stem cells help downregulate these immune responses by producing signaling molecules that suppress excessive immune activity. They have the capacity to influence immune cells, such as T lymphocytes and macrophages, directing them towards a non-inflammatory profile. Not only do stem cells directly benefit the kidney, but by slowing down immune reactions responsible for subsequent injury, they can also enhance the efficiency of native kidney self-repair processes.
Paracrine Signaling and Support of Tissue: The major therapeutic action (away from the importance of stem cells to generate new tissue) is accomplished by signaling molecules released from those cells. Stem cells secrete different types of growth factors, cytokines, and chemokines that influence nearby cells.
These molecules help promote the survival of injured kidney cells, new blood vessels form and oxygen delivery to damaged tissue increases. They also block the programmed cell death that usually takes place after renal injury. This also pushes the native kidney cells to replicate and repair missing or damaged structures.
Stem cells that could differentiate into renal tubular epithelial cells This skill may also cause slight, however purposeful restore of broken nephrons, the small functional devices of the kidney. This reprogramming is not the central process of repair for kidneys, but may be an additional mechanism that drives the normal renal interstitium back toward its anatomical architecture.
Anti-Fibrotic: Stem cells have been able to prevent or further decrease the scar process. These pathways modulate signaling pathways involved in regulating tissue remodeling and inhibit pathways that drive fibrotic collagen production. By inhibiting fibrosis/stromagenesis and fending off the structural derangement of renal parenchyma, stem c ells could also preserve kidney function over the long-term.
Prevention of Oxidative Damage: Stem cells release antioxidant molecules and prime the register war after ever had in the body with intentions that are supported by their own protective systems. All these actions yield beneficial Renal cytoprotective effects against oxidative stress, augmented mitochondrial function and balance enlargement in the aerial organ exploratory equilibrium.
Possible Clinical Benefits Of Stem Cell Therapy: Kidney Disease
Early clinical research and observational studies suggest patient-derived potentially successful advantages of stem cell therapy for kidney disease such as substantial missions in various clinically relevant markers of kidney function.
Glomerular filtration rate (GFR), a parameter that reflects kidney function, indicating the ability of kidneys to filter waste products from blood is one of its most important influences. In contrast to this however some studies showed GFR being stabilized and even increased after stem cell therapy. Another important sign is proteinuria — too much protein in the urine. The reduction of proteinuria was related to the improvement of both functional and structure of renal filtration (lower protein loads suggest more normal glomerular architecture and relatively better renal function).
Although serum creatinine increases and decreases in response to renal function declining, near the recovery of the kidneys it might plateau or decline after treatment. In addition to laboratory improvement, some patients show more energy, less fluid reactivity and better generic health that may indicate higher kidneys function.
Applications Across Different Kidney Disorders
Acute Kidney Injury : Stem Cell therapy could speed recovery of AKI through its anti-inflammatory activity as survivor cells are protected and repair mechanisms activated. Early intervention may also lessen scarring in the long run and lower future issues relevant to chronic kidney disease.
The full set of pathways leading to CKD progression—including inflammation, reduction in the extent of fibrosis and loss of ability of residual renal cells to survive—are potentially modifiable by stem cell therapy. Keeping more functional tissue may delay dialysis or transplant with stem cell therapy.
Kidney Transplantation Support stem cell to elicit immune tolerance against the transplanted kidney. Stem cell therapy may reduce organ rejection by modulating the immune response, potentially permitting a reduction in immunosuppressive drug doses. This approach may enhance allograft longevity with reduced side effects related to drug therapy.

