Realizing Hearing Loss as a Biological and Basically Successful Condition
Deafness is not just a problem of sound pressure level. It influences communication and social confidence, balance, emotional status and daily autonomy. More than 1.5 billion people have some hearing loss today, and the figure will rise to nearly 2.5 billion by 2050, according to the World Health Organization (WHO). This high burden places a great number of patients in search for novel medical solutions, including UC-MSC Thailand, hearing loss stem cell therapy and other types of regenerative medicine techniques focusing on more auditory system assistance.
Sensorineural hearing loss is particularly relevant within the field of regenerative medicine from all types of hearing loss. This happens when the hair cells in the inner ear get damaged due to aging, due to exposure to loud noises, due to infection or inflammation of the ear organ, because of ototoxic medication that affect hearing loss, genetic factors affecting function and structure of cochlea with age along with trauma or metabolic stress affecting cellular components required for hearing. One of the main reasons that permanent hearing loss is permanent in humans (and other mammals) is because damaged cochlear hair cells do not regenerate naturally.
Hearing Loss Treatment using UC-MSC Thailand
Many potential patients are searching UC-MSC Thailand when looking at medically supervised regenerative programs. Umbilical cord-derived mesenchymal stem/stromal cells (UC-MSCs), which are a population of multipotent cells, are considered with buzz due to their ability in releasing bioactive molecules that modulate inflammation, redox balance, immune system regulation and promotions to blood vessel development and tissue repair signaling.
For the audience of hearing loss treatments, UC-MSCs should not be referred to as a treatment guaranteed to improve or even restore hearing. The field remains investigational. Nevertheless, the scientific interest is understandable потому что versatile sensorineural hearing loss (SNHL) of one or another aetiology manifested cellular stress, inflammatory injury, mitochondrial dysfunction, microvascular compromise with degeneration of delicate inner ear structures.
Given the evidence, a responsible discussion of UC-MSC Thailand for treatment of hearing loss should provide biological justification, subject selection criteria, safety data from clinical trials or credible studies and realistic expectations rather than miracle stories.
UC-MSCs Potential Mechanisms of Support to the Auditory Microenvironment
UC-MSCs are not primarily considered as simply “becoming new ears” or directly replacing all damaged cochlear hair cells. A more scientific explanation is derived from what we know about paracrine signaling. This suggests that UC-MSCs can release growth factors, cytokines, extracellular vesicles and other signaling molecules to communicate with surrounding tissues.
In hearing loss research, mechanisms associated with stem cells are being investigated for potential influence on:
inflammatory modulation
oxidative stress reduction
cochlear cell survival signaling
vascular and microcirculatory support
neural protection
tissue repair communication
inner ear microenvironment stability
These mechanisms are scientifically interesting but are still under study. A systematic review in 2025 on cellular therapy for sensorineural hearing loss based on available studies showed mixed results: Several included studies reported improvements in hearing threshold while others did not demonstrate unambiguous improvement. It shows the promise and also reflects some of the uncertainty in the field.
Current research direction of stem cell therapy for hearing loss
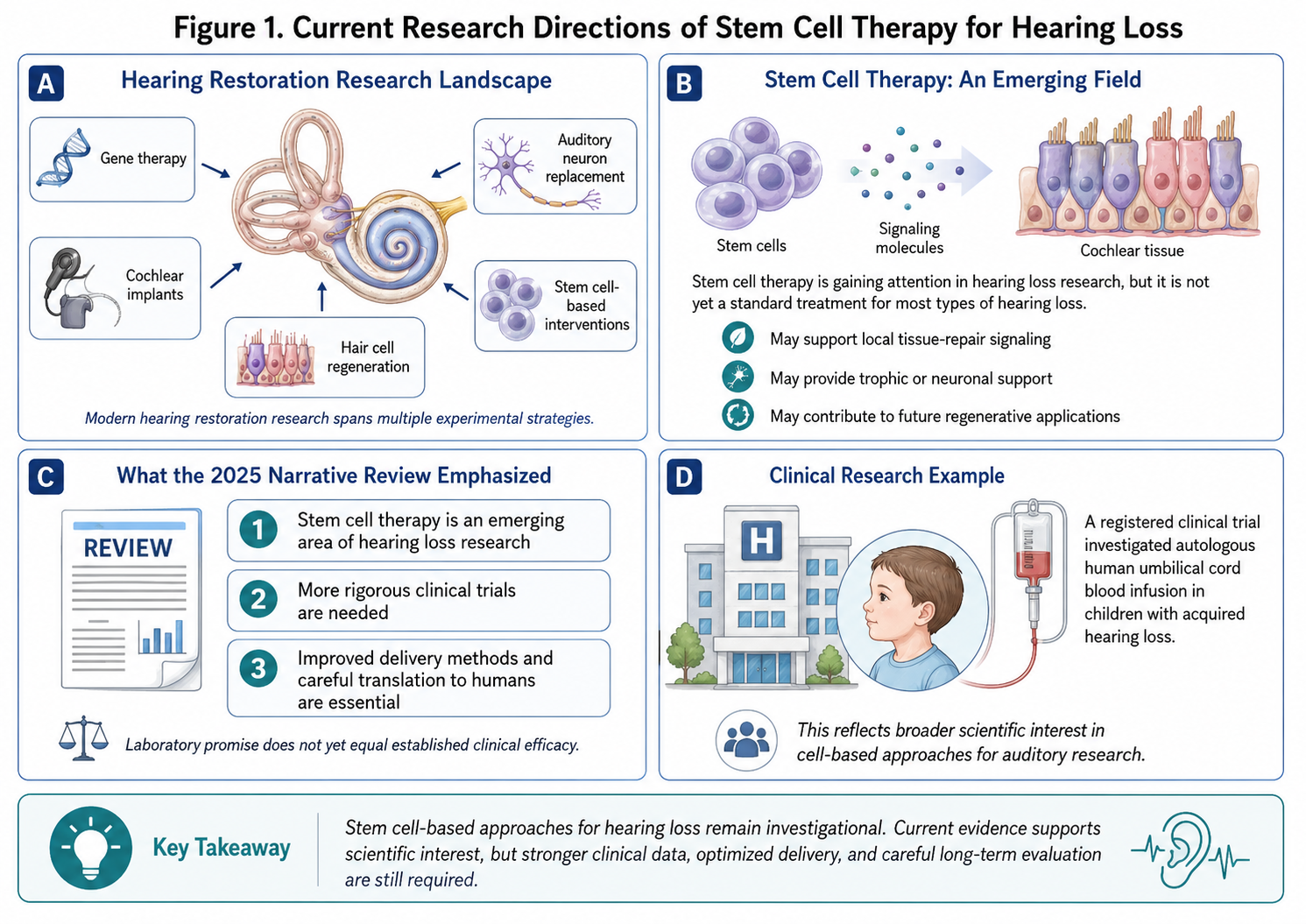
Experimental therapies for hearing restoration nowadays range from local delivery of gene therapy, cochlear implants, hair cell regeneration, auditory neuron replacement and interventions using stem cells. An area that is gaining attention is the role of stem cells in hearing loss; however, many stem cell therapies are not yet standard treatments for most types of hearing loss.
One narrative review from 2025 characterized stem cell therapy as an emerging area of research into hearing loss, particularly because different diseased cells might mediate local tissue-repair signaling, provide support for neurons, or serve roles in future regenerative applications. Simultaneously, the review stressed the importance of more rigorous clinical trials, improved delivery methods, and caution in translating laboratory data to humans.
The clinical research has also investigated umbilical cord blood-derived approaches. A registered clinical trial of autologous human umbilical cord blood infusion in children with acquired hearing loss reflects the broader scientific interest in other cell types for auditory research.
Figure 1: Overview of current research directions in stem cell therapy for hearing loss. Stem cell-based approaches are being investigated alongside gene therapy, cochlear implants, hair cell regeneration, and auditory neuron replacement, but they are not yet standard treatment options.
Explaining Thailand‘s Appeal/interest in Regenerative Hearing Programs
Directly or indirectly, Thailand is synonymous with global healthcare tourism and hospital-centred medical services, healing arts, wellness medicine and lab-augmented regeneration. That’s also why UC-MSC Thailand is at the top of your patient searches for stem cell therapy, they see doctors for hearing loss treatment and supportive regenerative programs.
Location, however, should not be the only consideration in choosing care. For hearing loss, the precision of diagnosis is critical. Your program should start with a thorough hearing test — not just an eval. These can be pure tone audiometry, speech discrimination testing, tympanometry, otoacoustic emissions, auditory brainstem response testing (in both cases when appropriate), medication history and noise exposure history assessment or even imaging if necessary and ENT evaluation.
What patients should always ask before consider UC-MSC Thailand
Patients explore UC-MSC Thailand to treat hearing loss I will just give you some perspective: one question that patients should ask as they consider their options when an ear infection does not go.
What kind of hearing impairment am I suffering from?
Sensorineural, conductive, mixed, sudden, presbyacusis (age-related), noise-induced or hereditary?
Then is it a stable loss, or is the hearing changing and progressive?
Shall we go with hearing aids, cochlear implants, medication or surgery?
What cell source is this?
Sterility, viability, identity and quality-control tests are performed.
What outcomes are realistically measurable?
Which follow-ups will be used for hearing tests?
These two questions should distinguish a medical program from marketing specifications.
Framing UC-MSCs for Hearing Loss
As far as UC-MSCs in hearing loss the most appropriate description are as a supportive investigational regenerative treatment. You should not label it as guaranteed restoration of hearing. They may instead be seen through a broader medical lens, where the focus is inflammatory homeostasis, senolysis and cellular stress reduction, vascular support as well as control of the auditory microenvironment by UC-MSCs.
Regenerative care for some may be an adjunct to routine hearing care as well as standard audiology, rehabilitation, hearing protection, hearing aids or cochlear implant assessment. Presenting stem cells as a pluck-it-off-the-shelf, stand-alone product is less scientifically sound than from an integrated model standpoint.
Conclusion
UC-MSC Thailand and stem cell therapy for hearing loss treatment is becoming more pronounced with the direction of regenerative medicine. The interest is justified because although many types of hearing loss are reversible, sensorineural hearing loss (SNHL) due to damaged or missing human cochlear hair cells has low spontaneous regenerative capacity. UC-MSCs are believed to exhibit paracrine, anti-inflammatory, immunomodulatory, vascular supporting and tissue signaling activities.
Meanwhile, the evidence is still developing. The currently investigated scientific potential is certainly exciting, but clinical outcomes show mixed results and no responsible provider should say that UC-MSCs are a cure for hearing loss. ConclusionsFor patients considering UC-MSC Thailand, the optimum approach includes careful diagnosis, ENT and audiology evaluation, patient education on cell quality standards, realistic expectations and structured followup.