Parkinson’s disease is one of those conditions where patients and families often live between two worlds. One world is the daily reality: tremor, stiffness, slow movement, balance changes, sleep problems, fatigue, anxiety, constipation, and the gradual uncertainty of what tomorrow may look like. The other world is the future of medicine, where researchers are exploring whether cell-based science may one day change how Parkinson’s is treated.
This is why searches for the best stem cell clinic and stem cell Parkinson’s programs are increasing. Patients are not only asking for symptom control. Many are asking whether regenerative medicine can support the brain environment, protect remaining function, or even replace the dopamine-producing neurons lost in Parkinson’s disease.
That last idea is where the keyword iPS cells replace dopamine neurons becomes important. It sounds futuristic, but it is no longer only a theory. Parkinson’s disease involves the progressive loss of dopamine-producing neurons, especially in brain regions related to movement control, and recent clinical research is testing transplanted stem-cell-derived dopamine neuron progenitors as a form of cell replacement therapy.
The Real Question Patients Are Asking
Most patients who search for stem cell Parkinson’s are not looking for complicated scientific language. They usually want to know one thing:
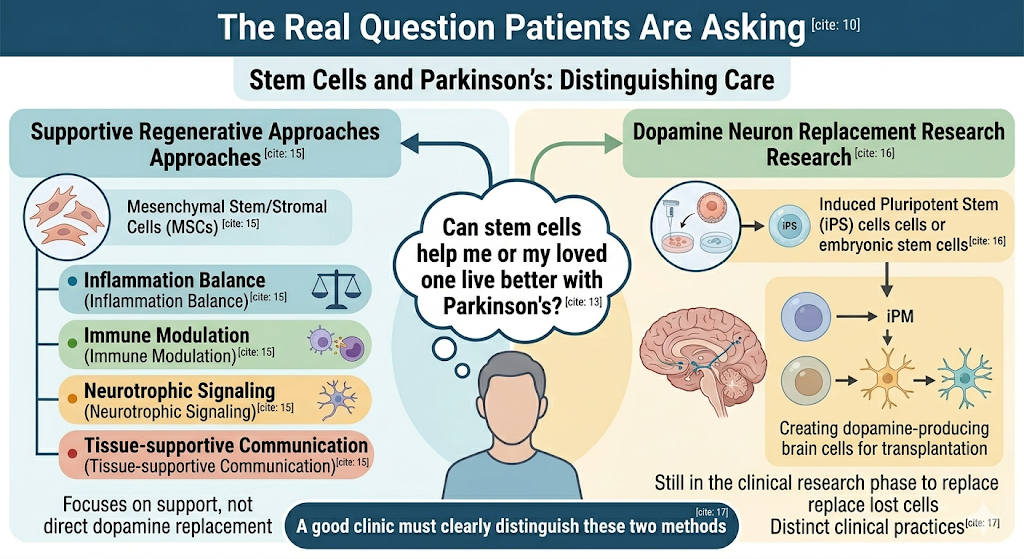
Can stem cells help me or my loved one live better with Parkinson’s?
The honest answer is layered.
Such supportive regenerative approaches usually include mesenchymal stem/stromal cells (MSCs) and encompass a variety of mechanisms, including inflammation balance, immune modulation, neurotrophic signaling, and tissue-supportive communication. Afterwards, there is a more specific domain: replacement of dopamine neurons, where working with either embryonic stem cells or induced pluripotent stem (iPS) cells to make transplanted dopamine-producing brain cells.
These two practices should not be made. A good stem cell clinic should make that distinction clear.
Parkinson’s is commonly recognized by tremor, stiffness, and slow movement. But the disease is much broader. It can affect sleep, mood, digestion, cognition, voice, swallowing, walking, and independence. The Parkinson’s Foundation describes Parkinson’s as a progressive brain disorder that damages dopamine-producing neurons and can cause both motor and non-motor symptoms.
This matters because any stem cell Parkinson’s discussion should not focus only on one symptom. A good care plan needs to consider the whole patient: neurological stage, medication response, mobility, rehabilitation needs, sleep quality, nutritional status, mood, and daily function.
Why Dopamine Neurons Matter So Much
Dopamine is a neurotransmitter that plays an important role in movement, motivation, and many functions of the brain and body. Dopaminergic neurons are selectively lost in Parkinson’s disease. Existing drugs, including levodopa, can partly compensate for the lack of dopamine activity but do not restore all lost cells.
This is where the concept of iPS cells superseding dopamine neurons becomes relevant to science. iPS cells are reprogrammed adult cells with a stem-cell-like state. Researchers can then encourage them to become progenitor cells that give rise to dopamine neurons. These cells are then implanted into defined brain regions that have lost dopamine neurons.
A Different Kind of Stem Cell Parkinson’s Research
And, as multiplex PD programs will not be similar to a standard IV regenerative program. There is sophisticated neurosurgical research in the replacement of dopamine neurons. It includes cell manufacturing, brain transplanting, immune monitoring, and safety tracking, as well as imaging and long-term follow-up.
In a publication in Nature (2025), results from an iPS-cell-based Phase I/II trial using dopaminergic cells were reported for Parkinson´s disease. Researchers at Kyoto University’s Center for iPS Cell Research and Application also characterized the work as a clinical trial with dopamine neurons produced from induced pluripotent stem cells (iPS) [life sciences; gene therapy]
This is why the phrase iPS cells replace dopamine neurons should be treated as a research concept, not just marketing buzz words.
The New Research Timeline Patients Should Know
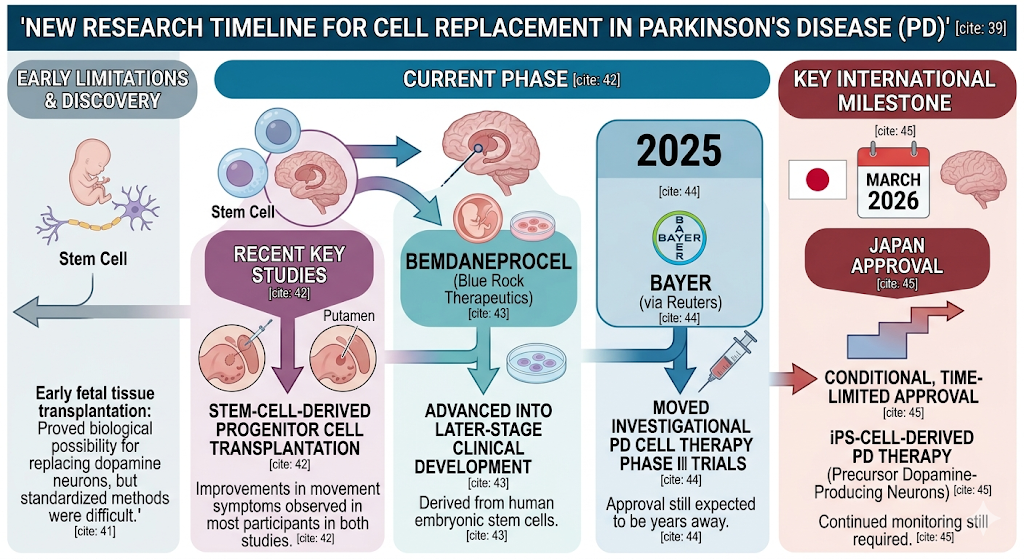
For many years, cell replacement in Parkinson’s was limited by ethical, technical, and safety challenges. Early fetal tissue transplantation showed that replacing dopamine neurons might be biologically possible, but the method was difficult to standardize.
Now the field is moving into a new phase. The Parkinson’s Foundation reported that two recent studies transplanted stem-cell-derived progenitor cells into the putamen, a brain region involved in movement, and both studies observed improvement in movement symptoms in most participants.
Blue Rock Therapeutics’ bemdaneprocel, derived from human embryonic stem cells, has also advanced into later-stage clinical development. Reuters reported in 2025 that Bayer moved the investigational Parkinson’s cell therapy into Phase III trials, while noting that approval was still expected to be years away.
Japan has also become an important country to watch. In March 2026, Japan granted conditional, time-limited approval for an iPS-cell-derived Parkinson’s therapy involving precursor dopamine-producing neurons, with continued monitoring still required.
What the Best Stem Cell Clinic Should Say Honestly
The best stem cell clinic should not make Parkinson’s sound easy. It should not say that stem cells can cure Parkinson’s, stop all symptoms, or reverse the disease permanently. That would not be scientifically responsible.
Instead, the clinic should explain that stem cell Parkinson’s care exists in different categories.
Supportive Regenerative Care
This may involve cells such as UC-MSCs or MSC-based approaches being explored for immune modulation, inflammation balance, and neurotrophic support. These are usually discussed as supportive or investigational, not as proven dopamine neuron replacement.
Dopamine Neuron Replacement Research
This includes advanced products made from embryonic stem cells or iPS cells. This is where iPS cells replace dopamine neurons becomes relevant. These therapies are designed to replace lost dopamine-producing cells, but they require complex clinical trial systems and long-term safety monitoring.
Standard Parkinson’s Care
Medication, neurologist follow-up, physiotherapy, occupational therapy, speech therapy, exercise, sleep management, nutrition, and fall prevention remain essential. A responsible best stem cell clinic should never tell patients to abandon standard neurological care.
How to Judge a Stem Cell Parkinson’s Program
Patients often compare clinics by price, location, or testimonials. That is understandable, but it is not enough. Parkinson’s is a serious neurological disease. Choosing the best stem cell clinic requires deeper questions.
Does the clinic separate support from replacement?
A clinic should clearly explain whether it is offering supportive regenerative care or discussing true dopamine neuron replacement research. If a clinic uses the phrase iPS cells replace dopamine neurons but is only providing a general infusion, that should raise questions.
Is there a neurological assessment?
Parkinson’s treatment should involve proper staging, medication review, motor and non-motor symptom evaluation, imaging history, and neurologist input when possible.
Are expectations realistic?
A good clinic may discuss possible support for quality of life, inflammation balance, recovery environment, or functional goals. It should not promise that a patient will stop medication or regain all lost movement.
Is cell quality explained?
The best stem cell clinic should be transparent about cell source, laboratory standards, sterility testing, viability, identity testing, route of administration, and follow-up.
Is rehabilitation included?
For Parkinson’s, movement training matters. Exercise and rehabilitation can support balance, strength, gait, flexibility, and confidence. Regenerative care should fit into this larger plan.
Why “Best” Should Mean Safe, Not Loud
The phrase best stem cell clinic is powerful for SEO, but medically, “best” should not mean the clinic with the boldest claims. It should mean the clinic with the strongest safety culture, clearest explanation, careful patient selection, and honest communication.
In Parkinson’s, hope is important. But hope should not be built on shortcuts. The real progress in stem cell Parkinson’s science is happening through careful trials, regulated manufacturing, neurosurgical precision, and long-term observation.
Conclusion: A More Mature View of Stem Cell Parkinson’s Care
The Parkinson’s medicine of tomorrow could look radically different from the past. Regenerative strategies with supportive potential may further investigate inflammation modulation, immune signaling, and neuroprotective pathways. Simultaneously, dopamine neuron replacement has stacked up as arguably one of the most exciting frontiers in all things stem cell research now that scientists can examine more directly whether iPS cells do indeed replace dopamine neurons and test if their newborn counterparts reasonably match idealized striatal targets.
As for those patients in search of the best stem cell clinic, it is important not to run after the flashiest promise. It’s to identify a medical team that can articulate the distinction between supportive care, exploratory research, and bona fide cellular replacement science.
Parkinson’s disease is complex. Good care by definition must be as thoughtful: neurologist-guided, safety-beaming, patient-centered, and open to advances—not exaggerated posturing regarding what science has not yet established.