Emerging novel regenerative strategies for Alzheimer disease using cell based therapy in Southeast Asia
Alzheimer s disease (AD) is one of the most prevelant neurodegenerative disorder and a major global health challenge. It gradually impacts memory, cognitive function, behaviour, communication and eventual functional independence with a tremendous burden to patients as well as families and healthcare systems. Over time, people with the disease need more help, and caregivers are under emotional, financial, and social stress. These realities have prompted interest in treatments that go beyond symptomatic relief and examine the possibility of regenerative medinice to provide biological modalities directed at neurodegenerative processes.
Pharmacological therapies are able to alleviate some symptoms in a narrow range of patients, but they neither stop neuronal loss nor restore already occurred structural damage. Regenerative medicine is therefore a focus of interest within Alzheimer’s disease research, especially the use of approaches with stem cells that may potentially modify inflammation as well as cellular signalling and neural repair pathways.
The Pathology of Alzheimer’s Disease
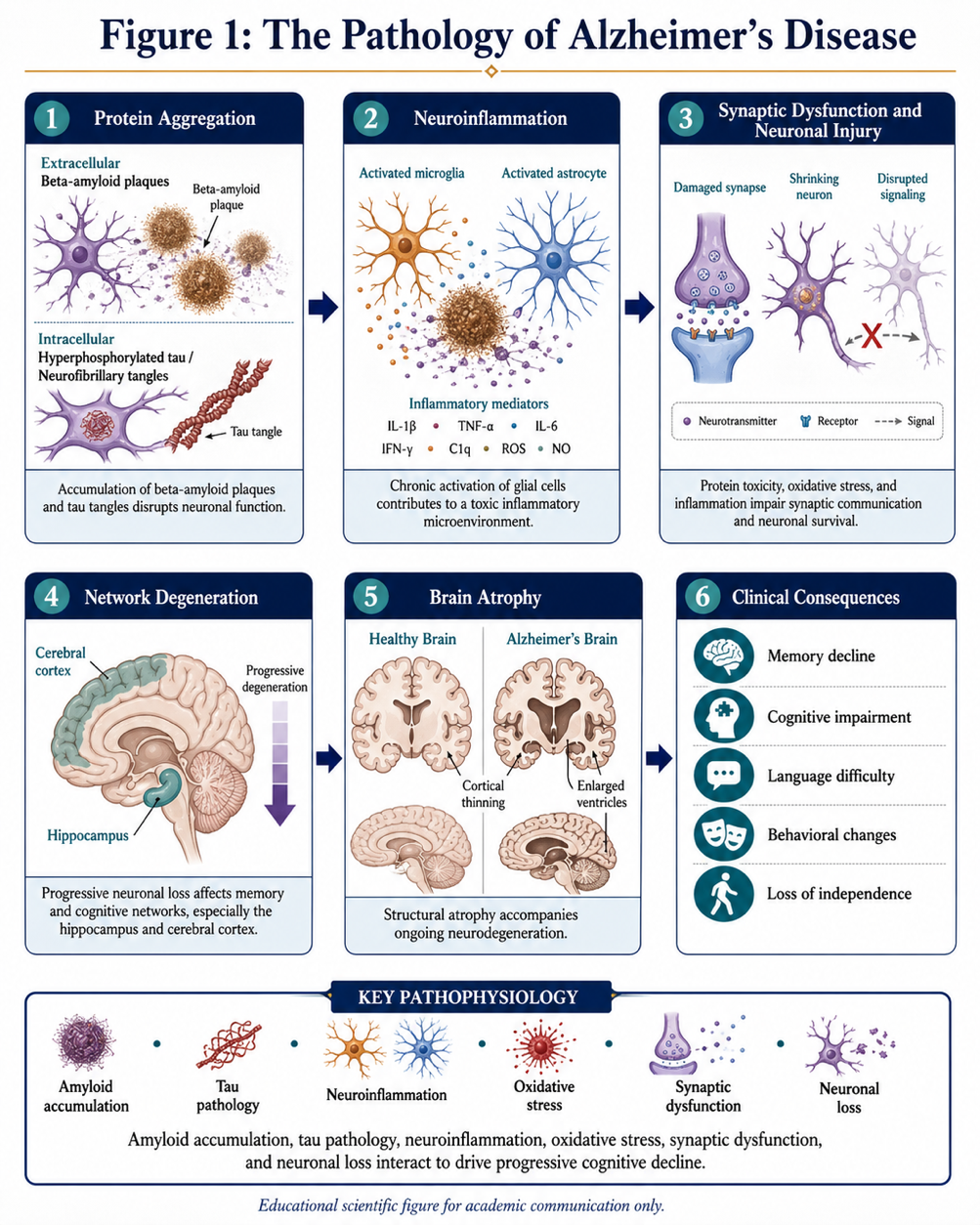
Alzheimer’s disease is an insidious, progressive atrophy and dysfunction of the structural components of the brain. In its pathology, the accumulation of extracellular beta-amyloid plaques and intracellular neurofibrillary tangles (NFT) containing hyperphosphorylated tau protein aggregates is often associated. This eventually results in pathological processes that result in synaptic damage, neuronal injury, network disconnection and progressive loss of brain volume.
Alongside protein aggregation, neuroinflammation has recently gained attention to be a key component in the progression of the disease. Increased numbers of activated microglia and astrocytes might establish a low-grade, chronic inflammatory milieu that adds to the neuronal stress in a bidirectional manner. Oxidative damage, defect in mitochondrial functioning, contribution of vascular factors and the disruption of intercellular communication may aggravate the neurodegenerative cascade.
These processes progressively lead to disruption of the structural and functional integrity of neural circuits important for memory, executive function, language, and activities of daily living. The outcome does not only of individual cognitive deficit but a gradual crumbling of the coordinated operations of the brain at cellular and systems levels. That’s important for the design of targeted mechanisms—not only biologically based but in fact much beyond that.
Figure 1: The Pathology of Alzheimer’s Disease
Traditional Medical Interventions
Conventional treatments for Alzheimer’s disease targeted the symptoms. Cholinesterase inhibitors and N-methyl-d-aspartate receptor antagonists are intended to facilitate neurotransmission and may offer transient stabilization or slight symptomatic relief in some patients. However, they do not in essence counteract neuronal degeneration or reclaim lost neural networks.
One of the constraints for traditional pharmacologic methods is that their impacts might diminish as the disorder progresses and therefore the neuronal substrate remains to degrade. Moreover, side effects like gastrointestinal symptoms, dizziness, cardiovascular complications and minimization of tolerability level could restrict the applicability of these drugs among patients.
Therefore, although conventional therapies are still a critical part of current therapy for Alzheimer’s disease (AD) for symptomatic control and multidisciplinary support, they do not cover all pathological structural, inflammatory, and degenerative components of the disease. This limitation has been a main driving reason for the rising curiosity in regenerative medication, both as adjuvant or exploratory treatment.
Regenerative Medicine for Alzheimer’s Disease
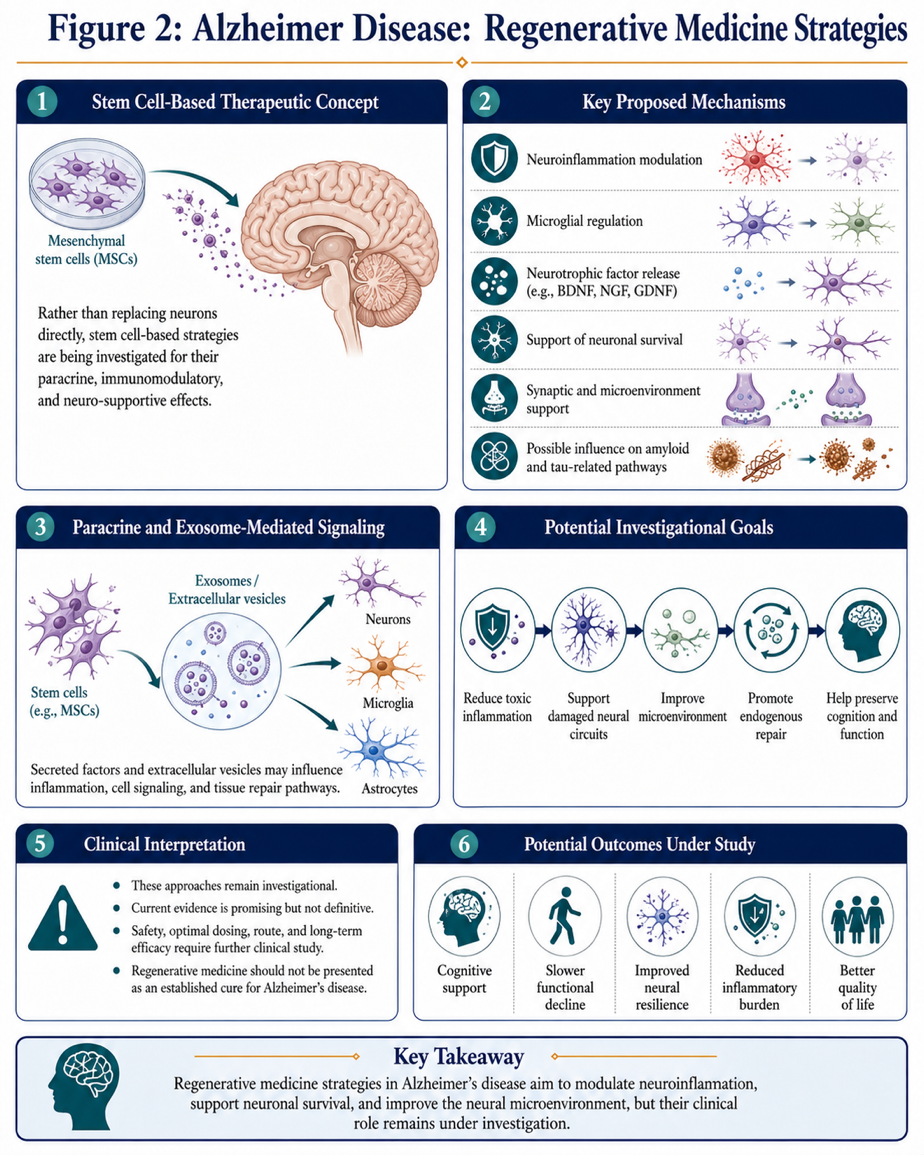
Unlike the previous approaches, regenerative medicine offers a unique framework to thinking about therapy in neurodegeneration by emphasizing not simply reparative properties but the biological milieu of nerve degeneration. This suggests that stem cell-based approaches might have immunomodulatory, anti-inflammatory, trophic and/or reparative properties rather than simply targeting neurotransmitters.
In particular, due to their potential for paracrine effects mediated by the secretion of bioactive molecules (eg cytokines, growth factors and extracellular vesicles), Umbilicle cord-derived mesenchymal stem cells (UC-MSCs) have become of great interest in neurodegeneration research. These soluble factors may regulate neuroinflammation, alter microglial activity, protect neurons and ameliorate the neural microenvironment. Additionally, signalling from transplant derived stem cells have also been investigated in experimental whole animal studies for potential involvement in stimulating endogenous repair processes, as well as synaptic plasticity that may regulate pathways relating to amyloid and tau-related pathology.
What is important, however, is to describe these approaches with caution. Stem cell therapy for AD is still an investigational treatment rather than part of established care. Although animal studies and early clinical results are promising, further rigorously designed clinical research is necessary to establish safety, optimal cell source, dosing strategies, route of administration as well as long-term clinical benefit.
From a scientific standpoint, regenerative medicine may provide real value in that it has the potential to target multiple interrelated disease mechanisms simultaneously — inflammatory mediators, cellular stress and impaired tissue repair. This sets it apart conceptually from therapies that target only neuro-transmitter pathways.
Figure 2: Alzheimer Disease: Regenerative Medicine Strategies
The Future of Regenerative Medicine in Southeast Asia
The increased prominence of Southeast Asia for regenerative and translational medicine especially in Thailand. In light of these developments, with increased interest in cell-based therapy, a growing number of advanced laboratory systems and the presence of medical infrastructure and clinical expertise within the region, this places it as a potential site for future contributions to neurodegenerative disease research.
Thailand is a mix of experienced clinicians, biomedical research capacity and internationally oriented medical services. This environment might provide a climate conducive to the rational growth of regenerative medicine research, but it must be used in conjunction with regulatory oversight, as well as quality control standards and ethical safeguards incorporated into clinical practice. Given these trends, the region should be well-positioned to undertake clinical trials evaluating novel treatments for challenging conditions like AD.
However, it is important that excitement in science be tempered by quality clinical data. The future for regenerative medicine in the treatment of Alzheimer′ s disease will depend on well designed clinical trials, reporting long-term data transparently and realistic interpretation of the outcomes.
Conclusion
Alzheimer’s disease continues to be a neurodegenerative disorder with progressive and devastating symptoms, while therapies available to date are largely symptomatic. While pharmacological treatments can ameliorate, they do not completely stop fundamental neurodegenerative processes. Hence regenerative medicine has therefore emerged as an area of great interest in large part due to the idea that stem cell-based approaches may modulate inflammation, tissue signalling and neuronal supportive pathways.
Although these approaches should not yet be regarded as the final or curative interventions, they are an essential scientific advancement in pursuit of more relevant biologic treatments. Future developments in translational medicine, particularly from emerging biomedical infrastructures such as those seen in parts of Southeast Asia, such as Thailand may also serve to advance these fields. In the end, deep clinical research with great evidence will dictate if regenerative medicine for Alzheimer’s Disease has any long term value.