Type 2 diabetes is more than just a blood-sugar disease. Untreated of course, it can lead to the destruction of heart, blood vessels. kidneys, nerves eyes in the long run. What happens about eight years later is subtle in many, and some might only have mild symptoms at beginning, but would notice their thirst gradually increasing greater than urinating frequently fatigue or blurred vision. Because early signs are often mild and only become clear as complications develop later by which time all has gone wrong.
How Type 2 Diabetes Affects the Body
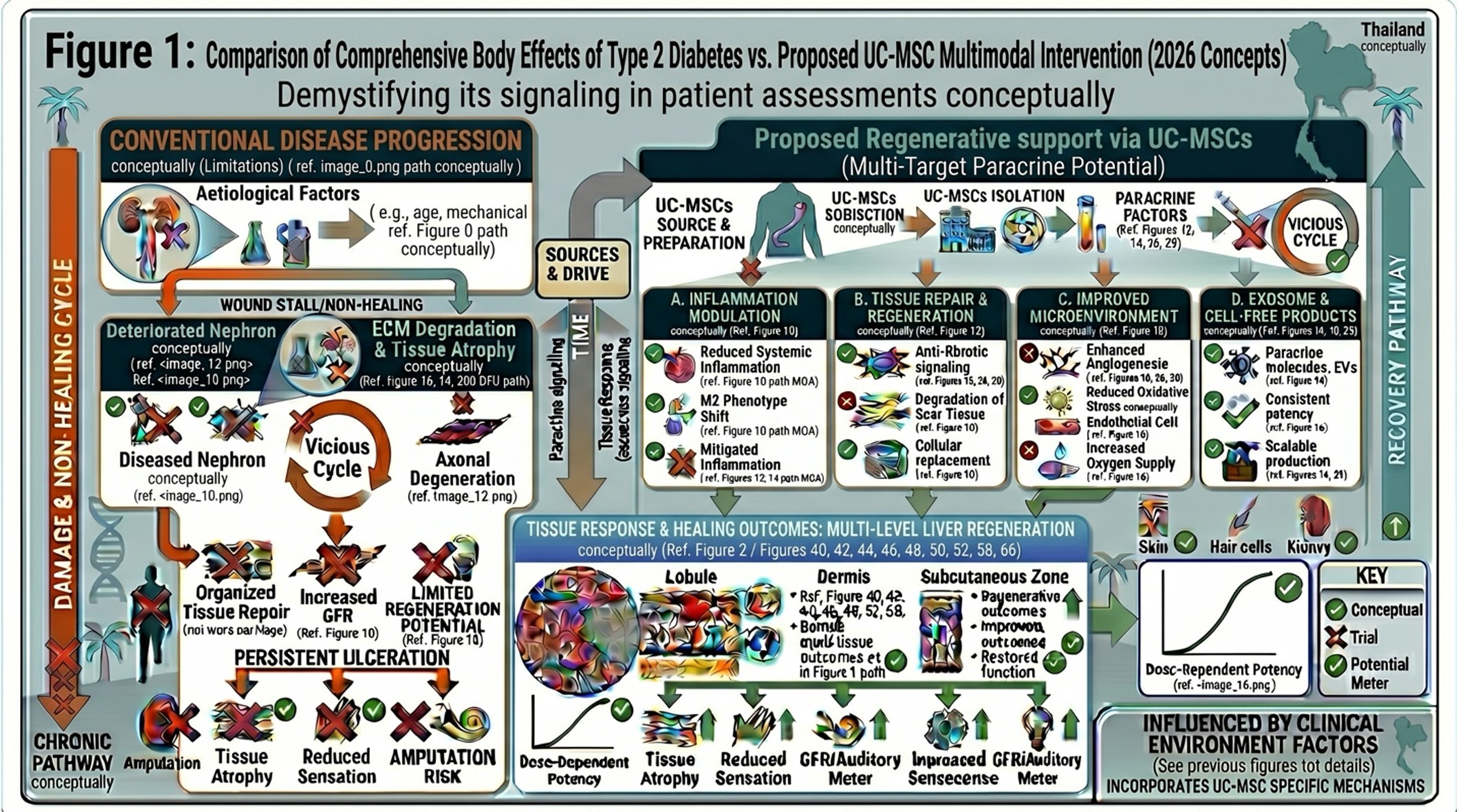
In type 2 diabetes, the body either doesn’t use insulin properly or produces enough of it. Insulin is a hormone that allows glucose to move from the blood into cells to be used for energy. When the action of insulin no longer works, glucose remains in the blood, causing injury to several organs and tissues over time. While insulin resistance forms a part, and an important part at that of the pathology of diabetes — something almost everyone misses entirely. Another aspect of the pathophysiology is chronic destruction or loss of pancreatic beta cells that produce insulin.
Why Beta Cells Matter
The pancreatic islets contain insulin-producing (or β-) cells. These cells learn to cope, but over time, for many people with type 2 diabetes, this stress leads to less effective or even exhausted insulin-producing cells. More accurately, that some patients will be able to manage diabetes for years with diet and oral therapies while others will probably require injectable or insulin therapy soon afterward. At our level of understanding, regenerative medicine investigators are also interested in whether cell-based strategies could protect beta-cells from injury and replace or restore beta-cell function sooner rather than later.
All You Need To Know About Stem Cell Therapy
Stem cell research in relation to diabetes is really looking at two broad concepts. The first one is whether other cell-based therapies might also have a paracrine effect on inflammation, metabolic milieu and pancreas. The latter is whether new cell-engineering approaches could generate insulin-producing cells to serve as transplants or replacements. These concepts are scientifically significant, and they merit careful introduction. In its present form stem cell derived islets and beta-cells are the most promising area of type 1 diabetes research with preliminary data being collected however there can be meant for small subsets of patients with type 2 diabetes, so in this case nano therapeutics may play a direct role as expected they will not provide explicit clinical “cures” to all actions or indeed every patient.
What the Evidence Right Now Does and Doesn’t
This is the part that matters most to readers. Although it seems like some early studies and reviews suggest possible metabolic benefits in selected patients or reduced insulin requirements, of cell-based strategies seem compelling these data are not yet convincing enough to introduce stem cell therapy into standard practice for type 2 diabetes. Despite mechanistic studies and pilot trials aiming to replicate our previous findings, a definitive and reproducible control of glycemia is still likely lacking across studies, although retrospective data from recent systematic reviews indicate reduced fasting insulin requirements after investigational stem cell treatment in some people with type 2 diabetes. At least some things with the field are promising, but it’s still a work in progress on a lot of things.
Careful Patients Need
Since even that requires brain surgery and diabetes is a dangerous health condition, a thousand hyperboles could not mitigate any clinic talking regenerative cure. The FDA advises consumers to be cautious about advertisements for regenerative medicine products, which are marketed more broadly across a wide range of diseases unless quality, safety, purity and potency has been properly established through established routes regulatory. Additional ISSCR recommendations for patients include asking about the evidence supporting a treatment, how it is overseen and whether it is performed as part of an ethically reviewed clinical programme.
Conclusions: Diabetes stem cell therapy should be considered as an invasive medical treatment and never a simple exit case to bypass meticulous endocrine armamentarium.
What a Real Assessment Is Made of
For patients even entering the treatment threshold, a medical assessment is required. In practice, that typically includes glucose control history, HbA1c level, fasting plasma glucose level, renal function (eGFR), blood pressure and lipids/medication use as well as diabetes complication screening of the eye and nerve at a minimum, heart or foot. An evidence-based appraisal also should recognize if nonetiological syndromes are closely insulin resistant, impaired insulin secretion, metabolic derangement due to obesity or advanced organ injury. This step matters because not everyone with type 2 diabetes is at the same stage of disease (or needs the same treatment).
Lifestyle and Standard of Care Remain Essential
Regenerative medicine for type 2 diabetes has to be framed within the context of lifestyle and medical management. This is also consistent with WHO (3) and NIDDK (4) recommendations of dietary advices, physical activity, weight and obesity management (and prevention), avoidance of tobacco use as well as appropriate medical follow-up for the primary or secondary prevention or delay of type 2 diabetes mellitus (T2DM) and its complications. We can ill-afford unmoved by them as “basic”, they continue to be the most evidence-based treatment tools which patients can use. Like any treatment the high-end therapy fit — if offered or considered for other causes of diabetes like this ought to be at best deployed in the context of medical care being delivered carefully and coordinated.
Conclusion
Stem cell therapy for type 2 diabetes, a disease marked by both concurrent insulin resistance and progressive relative beta-cell decopensation, is appealing. Although, in principle, some cell-based approaches might maintain or even improve insulin-producing function, there is at present no evidence to recommend that these therapies can be characterised as standard-practice cures. Search for evidence-based hopes and tread cautiously, the reality remains that decent diabetes care has always begun with diagnosis and monitoring! Lifestyle management endocrinologist supervision.

