Why this topic needs a careful explanation
- CKD makes people search for regenerative answers fast
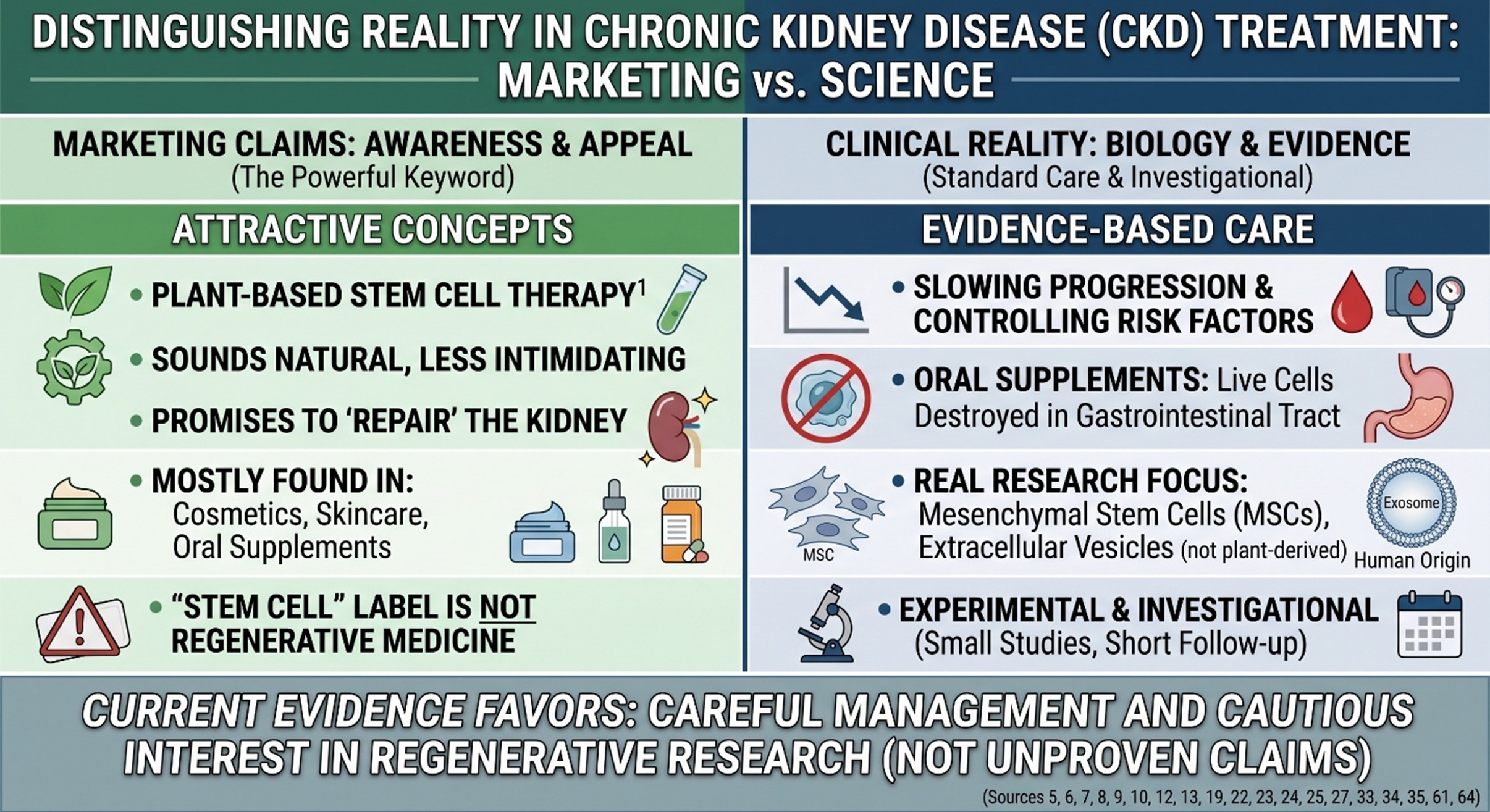
When people start reading about CKD, they often do so after hearing words like “scarring,” “declining kidney function,” or “progression.” That tends to push the search in a very human direction: is there anything beyond routine management that might actually help repair the kidney? That is one reason phrases like Plant-Based Stem Cell Therapy attract attention so quickly. They sound advanced, natural, and less intimidating than conventional renal medicine. But CKD is not a condition where language should get ahead of the biology. Chronic kidney disease means the kidneys are damaged or structurally abnormal and cannot filter blood the way they should, and current evidence-based care still focuses on slowing progression, controlling risk factors, and preserving function for as long as possible.
- The keyword is powerful, but the science behind it is uneven.
However, this is also a reason why people need to spend some effort to unpack Plant-Based Stem Cell Therapy. In the serious kidney literature, cell therapy for CKD research activity is mostly focused on mesenchymal stem/stromal cells and extracellular vesicles, tissue engineering-related regenerative platforms, etc. These are not plant-derived stem cells that you normally use in standard renal treatment programs. Recent reviews of CKD stem cell research describe it as promising but still limited by small study sizes, short follow-up, and inconsistent protocols. So the real question is whether regenerative medicine is interesting in kidney disease at all. Whether this phrase describes something scientifically established in CKD, or only in rare instances and under certain conditions. For the moment, it cannot.
What “Plant-Based Stem Cell Therapy” usually means
- In published literature, plant stem cells are mostly discussed outside of kidney medicine.
Plant-Based Stem Cell Therapy is most commonly found in the cosmetics, skin care products, and plant cell culture technology-related literature, or can be part of a food source (e.g., phytochemicals). Plans to utilize plant stem cells for potential applications are exactly the domain of Applications of Plant Stem Cells. This review will focus on: extracts – plant cell cultures; all kinds of cosmetic use, rather than curing therapies for chronic kidney disease. That’s important because plant-based stem cell therapy sounds like a recognized category of treatment for chronic kidney disease, even when most frequently it is a more likely term marketing people would use rather than one used in actual practice by nephrologists. And for CKD, this distinction is not trivial. It is the difference between a concept that sounds rejuvenating and a treatment pathway that is actually backed by clinical data from the kidney.
- “Stem cell” on a supplement label is not the same thing as regenerative medicine.
A second problem is that some products use “stem cell” language in ways that sound much more medical than the evidence justifies. Singapore’s Health Sciences Authority states that claims that oral supplements contain live stem cells are false and not scientifically plausible, explaining that viable stem cells require very cold storage and would be destroyed in the gastrointestinal tract if consumed orally. The same advisory also notes that regenerative medicine products intended to treat disease are generally experimental, and products used for such purposes are usually formulated as injections or infusions and require rigorous clinical testing. So when Plant-Based Stem Cell Therapy is presented like a ready-made oral fix for CKD, that should raise scientific questions immediately.
Where real stem cell science in CKD actually stands
- The main investigational field is mesenchymal stem cells, not plant-derived stem cells
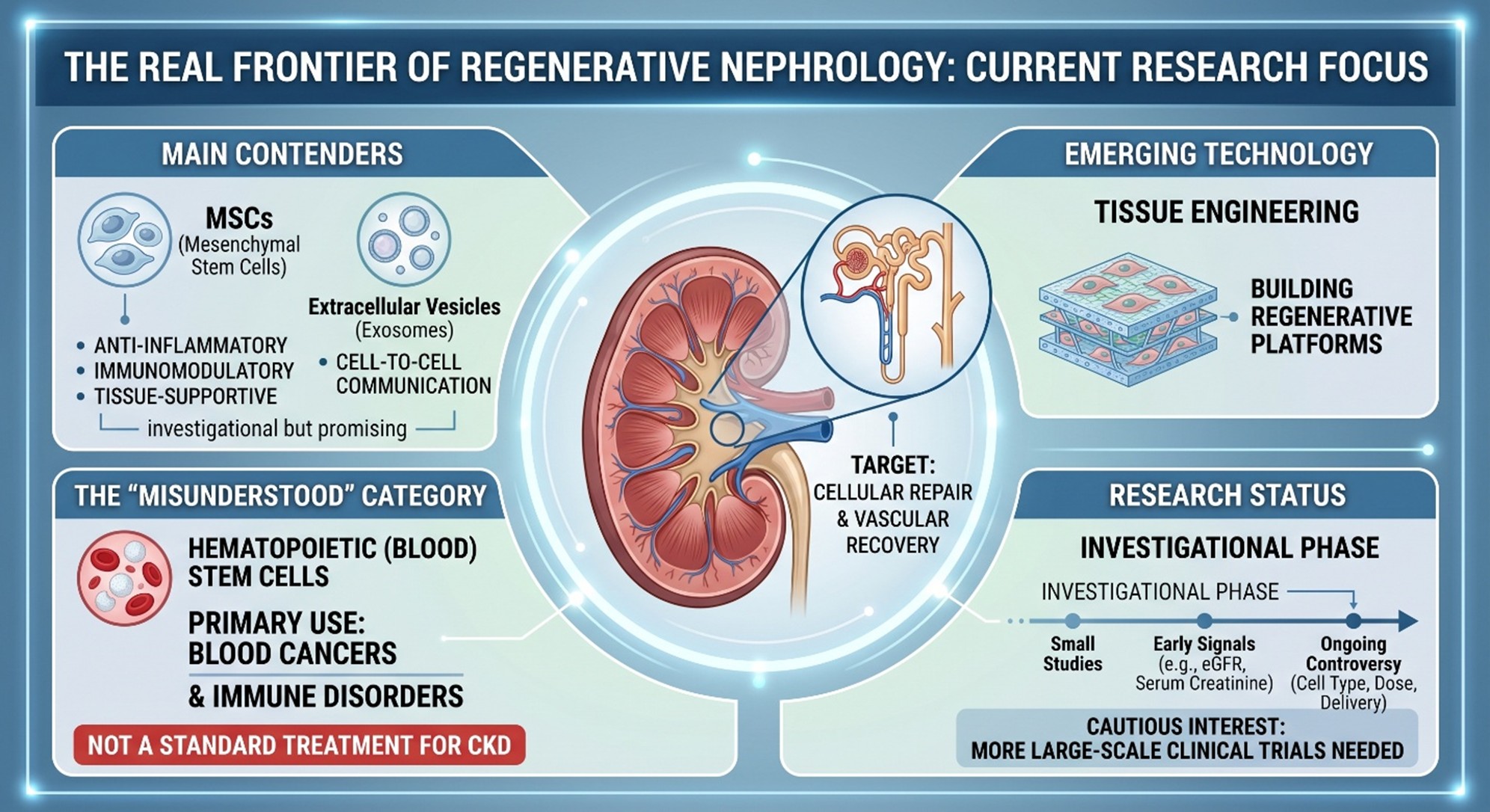
If we move away from marketing language and into actual kidney research, the field looks very different. Reviews from 2024 and 2025 describe mesenchymal stem/stromal cells as one of the main experimental cell types being studied in renal disease because of their anti-inflammatory, immunomodulatory, and tissue-supportive effects. The clinical landscape review from 2025 similarly found that CKD stem cell trials remain heavily centered on MSC-based strategies, while also emphasizing that the human evidence is still early and methodologically limited. In other words, real regenerative nephrology does exist—but it is not primarily a story about Plant-Based Stem Cell Therapy.
- Some early signals exist, but the field is still investigational.
Why researchers persist There are still four randomized trials, all of which are not of that same time period, and these The first evidence that stem cells may help diabetic kidney disease came from a 2025 systematic review and Medi-analysis in which 5 people ended up in hospital as a result yet one study found stem cell therapy beneficial for eGFR (measured by urine test) and serum creatinine levels and even lowered microalbuminuria without significantly more harm than other possible options (e.g. low-dose atorvastatin)The paper also drew attention to the fact that there is an ongoing controversy about which cell type, how grown Dose, from where and to deliver route it wanted for therapy That kind of nuance is exactly what this topic needs There may be a signal, but a signal does not equal a standard of care. For CKD, the regenerative frontier is still under construction
- Blood stem cells usually mean hematopoietic stem cells
The secondary keyword blood stem cell has a precise meaning in mainstream medicine. The U.S. National Cancer Institute defines a hematopoietic stem cell as an immature cell that can develop into all types of blood cells and notes that it is also called a blood stem cell. That is useful because it keeps the terminology honest. A blood stem cell is not the same thing as a kidney-specific regenerative cell product, and it should not be casually blended into every CKD discussion as though the categories were interchangeable.
- Blood stem cell therapy is not a standard treatment for CKD.
This is where confusion often starts online. Hematopoietic stem cell transplantation is a real and important therapy in blood cancers and some immune disorders, but it is not a standard treatment for chronic kidney disease. In fact, recent kidney literature describes CKD as a known complication after hematopoietic stem cell transplantation in some patients. So while blood stem cells are a legitimate medical term, it does not currently function as routine regenerative therapy for native CKD in the way some readers might assume.
- There is also research on blood-derived repair cells, but that is still a different discussion.
A more subtle scientific point is that some blood- or bone-marrow-derived progenitor cells have been studied in kidney and cardio-renal disease, especially around endothelial injury and vascular repair. That work is scientifically interesting, and it helps explain why blood stem cells sometimes appear in regenerative kidney writing. But it is still research territory, not a settled clinical solution for CKD. It belongs in the “emerging mechanisms” category, not in the “established therapy” category.
What honest CKD care still looks like
- Evidence-based CKD care remains the foundation
This part is easy to overlook when regenerative keywords dominate the page, but it is probably the most important. KDIGO’s 2024 guideline remains the current global standard for CKD evaluation and management, and NIDDK continues to emphasize measures like blood pressure control, glucose control in diabetes, medication review, monitoring GFR and urine albumin, nutrition planning, physical activity, and avoiding kidney-harming drugs such as some NSAIDs. That means the most credible way to talk about Plant-Based Stem Cell Therapy and CKD is not as a replacement for standard care, but as a keyword that needs to be placed against the reality of what actually helps protect kidney function today.
The most honest conclusion
- A strong keyword, but not a strong clinical category
The most honest reading is to say: Plant-Based Stem Cell Therapy may be a strong phrase in search engine optimization, but it’s not yet a well-established clinical category for treating chronic kidney disease. In current kidney science, the real regenerative action is in MSCs, exosomes, and tissue engineering, as well as other experimental cell-based therapies. Meanwhile, blood stem cells have a clear medical meaning, but they shouldn’t be taken as an abbreviation for a proven therapy to cure CKD from now on. For now, the current evidence is in favor of careful management and cautious interest in regenerative research on CKD, not wild claims that plant-based stem cell products have already changed kidney medicine.