In regenerative medicine Thailand discussions, few topics attract as much curiosity as Osteoarthritis. That is not surprising. Osteoarthritis is one of the most common causes of long-term joint pain, stiffness, and loss of mobility, especially in the knee and hip. Higher-quality clinical practice guidelines still consistently place exercise, education, and weight management at the center of care, but interest in biologic and regenerative strategies continues to grow because many patients want options that do more than temporarily reduce symptoms. In Thailand, that interest is also easy to understand in the context of an aging population and local studies showing a meaningful osteoarthritis burden among Thai adults.
It is important to start by saying regenerative medicine in Thailand should not be framed as some kind of journey around evidence-based osteoarthritis care. The emerging scientific literature rather indicates otherwise. While current nice guidance says intra-articular stem cell injections for osteoarthritis are still experimental and not to be used outside research, the American College of Rheumatology guideline as well have absolutely recommended against them for knee and hip OA due to heterogeneity and lack standardization. That doesn’t mean the field is without meaning. It does mean the field is also still immature, and therefore the most responsible way to talk about Osteoarthritis and regenerative medicine is really to do so is twofold, differentiating between established care from emerging care.
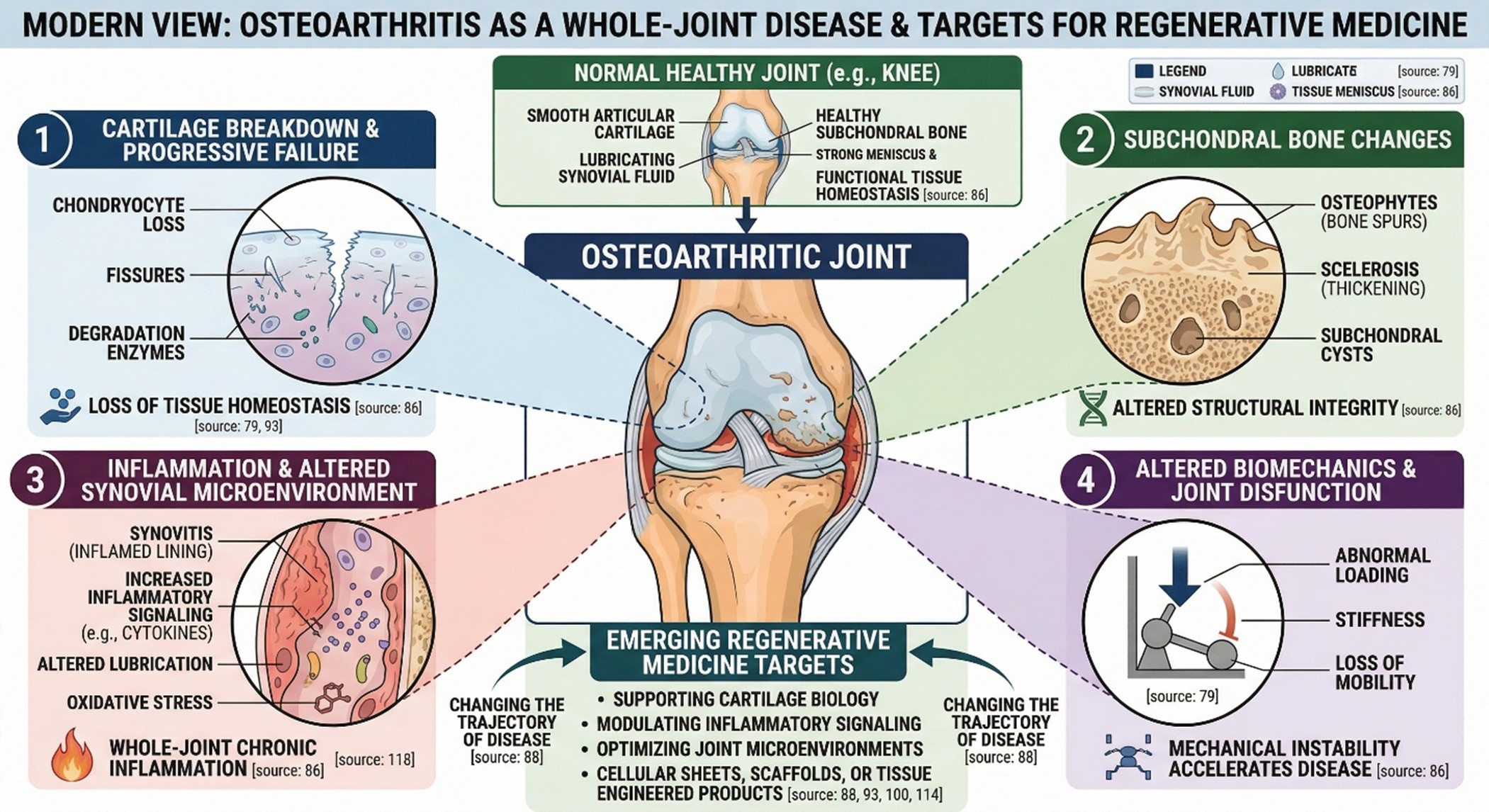
That distinction matters because osteoarthritis is not only “wear and tear.” It is now understood as a whole-joint disease involving cartilage breakdown, subchondral bone changes, inflammation, altered biomechanics, and progressive failure of tissue homeostasis. This more modern view is exactly why regenerative approaches are attractive. Researchers are not just trying to mask pain; they are asking whether cartilage biology, inflammatory signaling, or joint microenvironments can be supported in ways that change the trajectory of disease. Reviews published in 2024 and 2025 suggest that mesenchymal stromal or stem cell-based therapies may improve pain and function in some patients with knee osteoarthritis, but they also repeatedly highlight a familiar problem: study protocols remain highly variable. Cell source, dose, preparation, delivery, and patient selection still differ enough across trials that strong universal conclusions remain difficult.
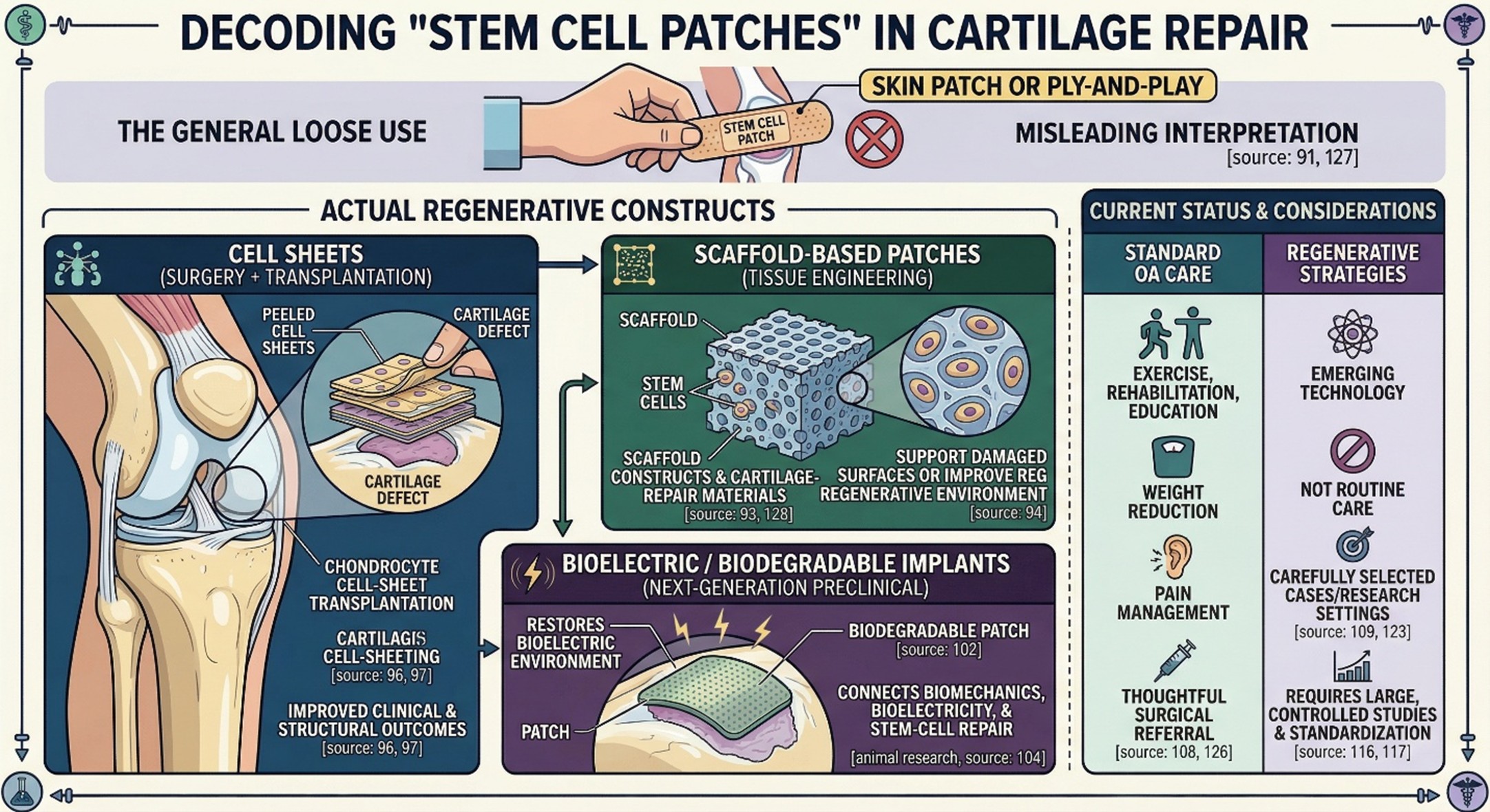
This is where the article needs a second layer, because the phrase stem cell patches is often used loosely online. actual scientific articles naturally didn’t mean an easy plug-and-play product, like one poured onto cells. Instead, the term was more likely to apply to cells sheets, scaffold-based cartilage patches, or tissue engineered products designed to support cartilage repair. It didn’t, in other words, usually mean the skin patch or such What makes sense true for people on the internet put in an artificial structure surgically planted or lately invented on to help repair damaged cartilage surfaces or improve the regenerative environment inside a joint. This is a subtle distinction, but it will loom large in how credible regenerative medicine Bang Khen content seems when read over by an expert reviewer or you tweak your own style template to the satisfaction of a peer.
Interestingly, there is real science behind this area. In npj Regenerative Medicine, researchers reported that combined surgery plus autologous chondrocyte cell-sheet transplantation improved clinical and structural outcomes in a small osteoarthritis series, although the treatment package included multiple steps and the study was not designed to isolate the exact effect of the sheet alone. A later report on allogeneic polydactyly-derived chondrocyte cell sheets also described encouraging findings in a small longitudinal series of knee osteoarthritis patients with cartilage defects. These are not large definitive trials, and they are not proof that stem cell patches have become routine care. But they do show that patch-like regenerative constructs are not just a marketing phrase; they are a real branch of cartilage repair research.
At the same time, not every “patch” headline translates into clinical reality. Some of the most exciting developments remain preclinical. A 2025 study described a biodegradable implantable patch designed to restore the bioelectric environment of osteoarthritic tissue and promote cartilage regeneration in a rat model. That kind of work is scientifically exciting because it connects biomechanics, bioelectricity, and stem-cell-responsive tissue repair in a way that feels genuinely next-generation. But it is still animal research. For a human reader interested in Osteoarthritis, the key message is that regenerative design is advancing quickly, but not every elegant laboratory result is ready for everyday clinical use.
So where does that leave regenerative medicine Thailand today? In a realistic sense, it sits in a middle space. The field is too active to dismiss, but not mature enough to exaggerate. For patients with osteoarthritis, standard non-surgical care still matters enormously: exercise, rehabilitation, education, weight reduction where appropriate, pain management, and thoughtful surgical referral when needed remain the backbone of treatment. Regenerative strategies may become relevant in carefully selected cases, especially in research settings, cartilage-defect repair strategies, or future joint-preservation pathways. But the strongest current evidence does not support replacing core osteoarthritis care with stem-cell branding alone.
This is also why the best writing on stem cell patches should sound honest, not breathless. People with osteoarthritis are usually not looking for abstract science. They are looking for a reason to believe that the next option might preserve movement, reduce pain, and delay decline. That human instinct is understandable. Therefore, the most reliable theory is that the regeneration therapy patches be incorporated into repair materials and machinery for cartilage tissue construction, rather than considered a complete method of tackling osteoarthritis. But there is hope in clinical trials, more experimental studies are underway and products are being introduced across surgery. However, large controlled studies are urgently needed; standardized techniques need to be developed; and longer-term follow-up is required if the field is to advance beyond what we now know.
The deeper reason this topic keeps growing is simple: osteoarthritis is painfully common, biologically complex, and frustratingly persistent. That makes it a natural target for regenerative thinking. But in serious medicine, hope works best when it is tethered to evidence. For now, the most accurate way to understand regenerative medicine Thailand and Osteoarthritis is this: the science is moving, the engineering is getting smarter, and stem cell patches are becoming more scientifically meaningful as part of cartilage-repair research, but the field still belongs to careful interpretation rather than sweeping promises.
FAQ
Are stem cell patches already a standard treatment for osteoarthritis?
No. In current evidence, patch-like regenerative constructs are still better understood as emerging cartilage-repair technologies rather than standard routine osteoarthritis care.
Do stem cell therapies help osteoarthritis symptoms at all?
Some recent reviews and meta-analyses suggest improvements in pain and function in selected knee osteoarthritis studies, but results remain heterogeneous and methods are not yet standardized.
Why do so many osteoarthritis guidelines still emphasize exercise and weight management?
Because across high-quality guidelines, those remain the most consistently recommended non-surgical foundations of care.
What does “stem cell patches” usually mean in the literature?
Usually not a skin patch. It more often refers to cell sheets, scaffold constructs, or implanted cartilage-repair materials used in tissue engineering and regenerative orthopedics.