Huntington’s Disease and Natural Cellular Regeneration
Introduction To the Genetic Crisis
A neurodegenerative disorder associated with a genetic mutation; Huntington’s Disease is a disease which is characterized by progressively ceaseless and involuntary degradation of brain tissue. A clinic-psychiatric disorder of motor control, patients with Huntington’s Disease face severe and detrimental changes to their quality of life, experiencing dystonic movements coupled with uncontrollable outbursts, and may also present severe psychiatric disorders. While conventional symptom management is a healthcare disaster, patients and their families experience even greater despair and suffering, worsening the highly emotive and psychologically impacting symptoms of the disease. While researchers have concentrated on cellular degeneration in order to stop or even reverse the disease’s physiological deterioration, the use of Natural Cellular Regeneration to control neurodegeneration is the only viable and rational approach to controlling the devastation of the disease.
Mechanism of the Illness
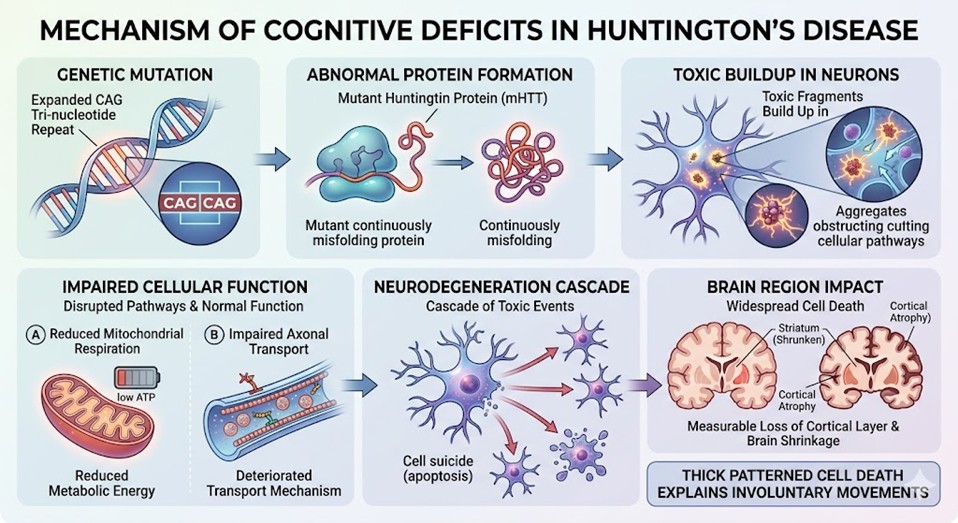
The cognitive deficits from Huntington’s Disease are due to an expanded CAG tri-nucleotide repeat in the sequence of the HTT gene. This mutation leads to the development of an abnormal huntingtin protein that misfolds all the time. Toxic protein fragments build up in the cell and neurons. They encroach on the normal cellular function on the pathways. The cell diminishes the activity of mitochondrial cellular respiration and reduces the formation of the metabolic energy the cell needs to survive. Other points of cellular function that comprise the axonal transport mechanism in the cell deteriorate. This sets off the cascade of toxic events that leads to the long and wide spread of cell suicide in the striatum as it spreads to the outer layer of the brain. The thick patterned cell death explains the chopped repetitive movements involuntarily. The specific disease mechanism of Huntington’s Disease is due to the measurable loss of cortical layer and the shrinking of the brain. It is to this extent of intricate cellular damage that the scientists interested in cell restoration techniques will look to the pathway of the Natural Cellular Regeneration as the biological pathway to the cellular restoration that will reverse the damage.
Negatives of Traditional Pharmacological Treatments
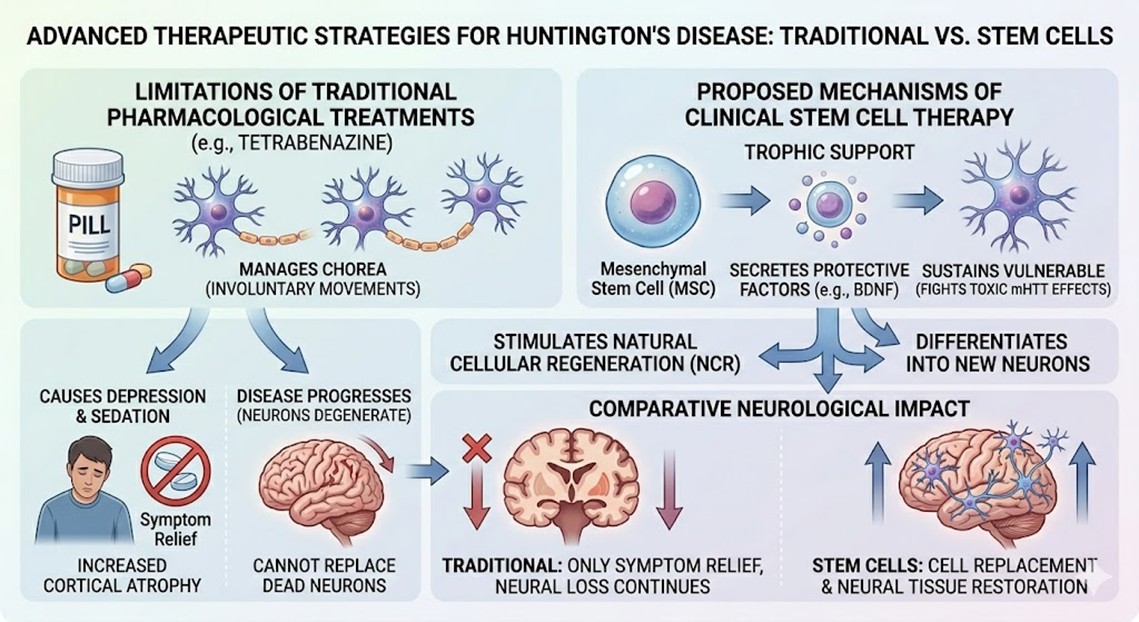
In the past, medical doctors in the world would rely on many of the traditional and historic pharmacological treatments to try to manage Huntington’s Disease and all of the chorea movements that are caused due to the disease. Tetrabenazine has and is continuing to be one of the most prescribed treatments to manage the involuntary motor fluctuations that occur. Yet these historic treatments are not stopping the disease from progressing and making the neurons degenerative. The patients also end up receiving a lot of the traditional and historic pharmacological treatments and end up receiving a lot of depression and sedation. The patients also end up having their brain undergo a lot more atrophy. None of the drugs that currently exist in the world are able to accomplish the goal of having the neurons that die be able to be replaced, or to restore the neurons in the networks that are used. This has led to one of the most essential driven switches toward dynamic biological pathways that are needed throughout clinical settings to achieve much of the Natural Cellular Regeneration that is needed in the structures of the neurons.
Proposed Mechanisms for the Clinical Use of Stem Cells
Stem cell therapies are the only proven way to encourage the growth of new neurons in the brain, a process termed neurogenesis. Mesenchymal stem cells (MSCs), for example, provide trophic support to the dying striatum. The implanted MSCs secrete protective brain-derived neurotropic factors (BDNF) to sustain vulnerable neurons from the toxic effects of mutant huntingtin. More importantly, these cellular therapies stimulate Natural Cellular Regeneration (NCR) by differentiating directly into new, functionally striatal projection neurons. These new projection neurons re-establish synaptic links within the ailing basal ganglia circuitry. This treatment approach tackles the primary pathogenic genetic abnormality of Huntington’s Disease at the cellular and molecular level. Stem cell therapy, by directly replacing lost neural tissue, rather than addressing only the surface symptoms, transforms the prognosis for the affected individuals.
Anticipated Developments in the Thai Medical System
The Southeast Asian region has recently developed strategically as the world’s primary destination for international medicine and the latest biotechnological therapies. The Thai Government’s positive regulatory environment has made it the main regional leader in innovative stem cell research. The first-rate medical facilities in Thailand have specialized, and world-class laboratories, which, are expected to deliver the first effective protocols for neurological regeneration. Due to the affordability of the latest medical technologies and the combination of medical excellence and engineering, international patients are encouraged to seek treatment. At this moment, the geographical region has the best prognosis for the management of Huntington’s Disease. Many clinical research studies are underway, which are aimed at the global clinical application of Natural Cellular Regeneration.
The complex genetics of Huntington’s Disease are likely going to be fatal for those afflicted until an entirely new kind of biological intervention is developed. Standard, synthetic, drugs, even those in clinical trials, have not been able to stop the progression of brain atrophy. In contrast, the new regenerative technologies under development are expected to have the first disease-modifying therapeutic effect. Natural Cellular Regeneration, in addition to establishing new, resilient, neural networks, will also replace lost, injured, or diseased neurons. These advances will provide hope to many families of patients with this terrible, worldwide, degenerative brain disease. As long as the regional funding initiatives continue, these commercialized, breakthrough, cellular therapies will be available to patients in the near future as opposed to the distant future.

