- When Multiple Sclerosis Stops Feeling Like a Simple Diagnosis
Multiple sclerosis usually isn’t limited to just a few symptoms that seem strange and disorganized. Major in-patients may experience blurring when they look down from their computer screens to talk to others who share their textbooks or check each other pre-harvest conditions. Facebook recently disclosed that, in one group, it has deleted over 100 pages used by spammers who merely repurpose material from other sources without credit or attribution. Over time, diagnostic uncertainty becomes a heavy burden. Not just the label for a neurological problem patients carry throughout their lives, it starts to plague them on a daily basis–trying and trying again to keep up energy, keep upright and balanced instead of slumping over the next puff from an air conditioner or heating duct vent but allowing themselves liberally to spill over phone books they carry in their pockets just in case they’re ever sick of simply taking off their shoes on public transport. This is why people with multiple sclerosis often start by treatment of their symptoms, but end up looking for root causes. Here, as search volume on “stem cell clinic” and “stem cell therapy for MS” both grow, that is exactly where America’s largest philanthropy focused on the disease does not name them as a form of hero. The National Multiple Sclerosis Society states that MS is a disease in which the immune system attacks the central nervous system, causing damage to myelin Sheath. And stem cell techniques are being studied in order to “reprogram” the immune system or potentially repair damaged tissue.
For many patients, the search for alternatives is not about rejecting standard medicine. It is about reaching the point where standard care feels incomplete. Modern disease-modifying therapies have changed MS care dramatically, but they do not erase the emotional reality of living with relapses, MRI changes, progression risk, or the fear of what comes next. That is why a phrase like stem cell therapy for MS carries so much emotional force. It sounds less like symptom management and more like the possibility of resetting the story. Scientifically, that hope is not coming from nowhere. The National Multiple Sclerosis Society says the stem cell approach currently used in MS is autologous hematopoietic stem cell transplantation, or aHSCT, while other types of stem cell approaches remain under investigation.
- Why Stem Cell Therapy for MS Has Become Such a Strong Search Topic
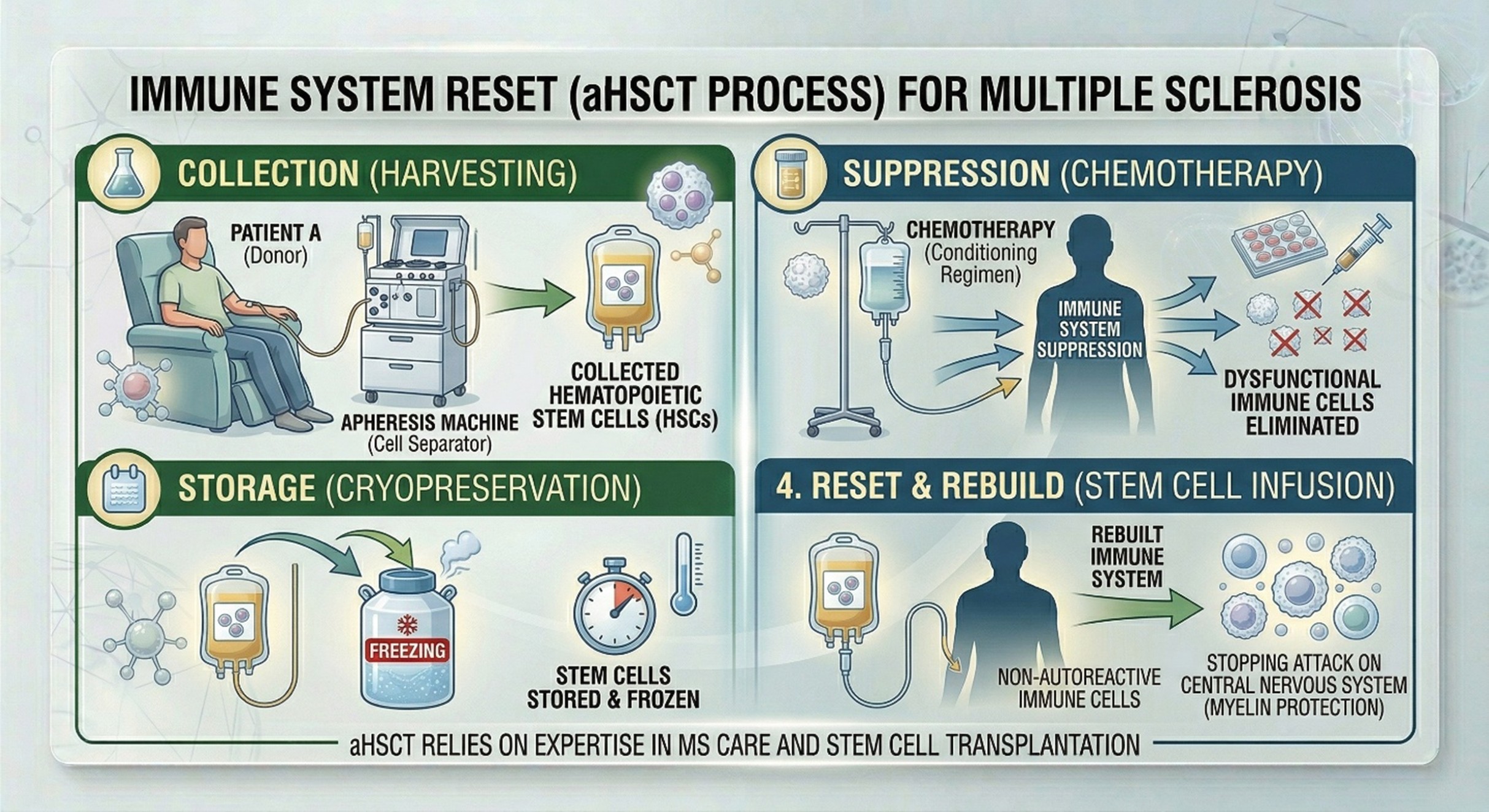
The reason stem cell therapy for MS keeps attracting attention is that it offers something conventional treatment does not always promise: the possibility of changing the immune trajectory of the disease more dramatically. In aHSCT, the patient’s own blood-forming stem cells are collected, the immune system is suppressed with chemotherapy, and then the stem cells are returned to rebuild the immune system. The idea is not to “regrow a new brain” but to reset the inflammatory immune activity driving some forms of multiple sclerosis. That is why the strongest clinical conversation around stem cell therapy in MS is still centered on aHSCT, not on generic marketing language from any random stem cell clinic.
At the same time, stem cell strategies for multiple sclerosis aren’t all alike. In addition to aHSCT, researchers have also investigated mesenchymal stem cells, neural stem cells and cell-derived neural progenitor transplantation. These approaches are interesting for different reasons: immunomodulation, neuroprotection, or maybe even the potential for structural regeneration. A 2025 systematic review of mesenchymal stem cells in MS found signs of neuroprotection, reduced lesion activity in some studies, increased disability scores for some patients, and yet also emphasized how uncertain their long-term efficacy remains as different treatment protocols received wide notice. This is why stem cell treatment for MS is both a genuine scientific topic and a dangerous cheating phrase. The science is active, but neither the field speaks with one voice.
- What Current Research Actually Suggests
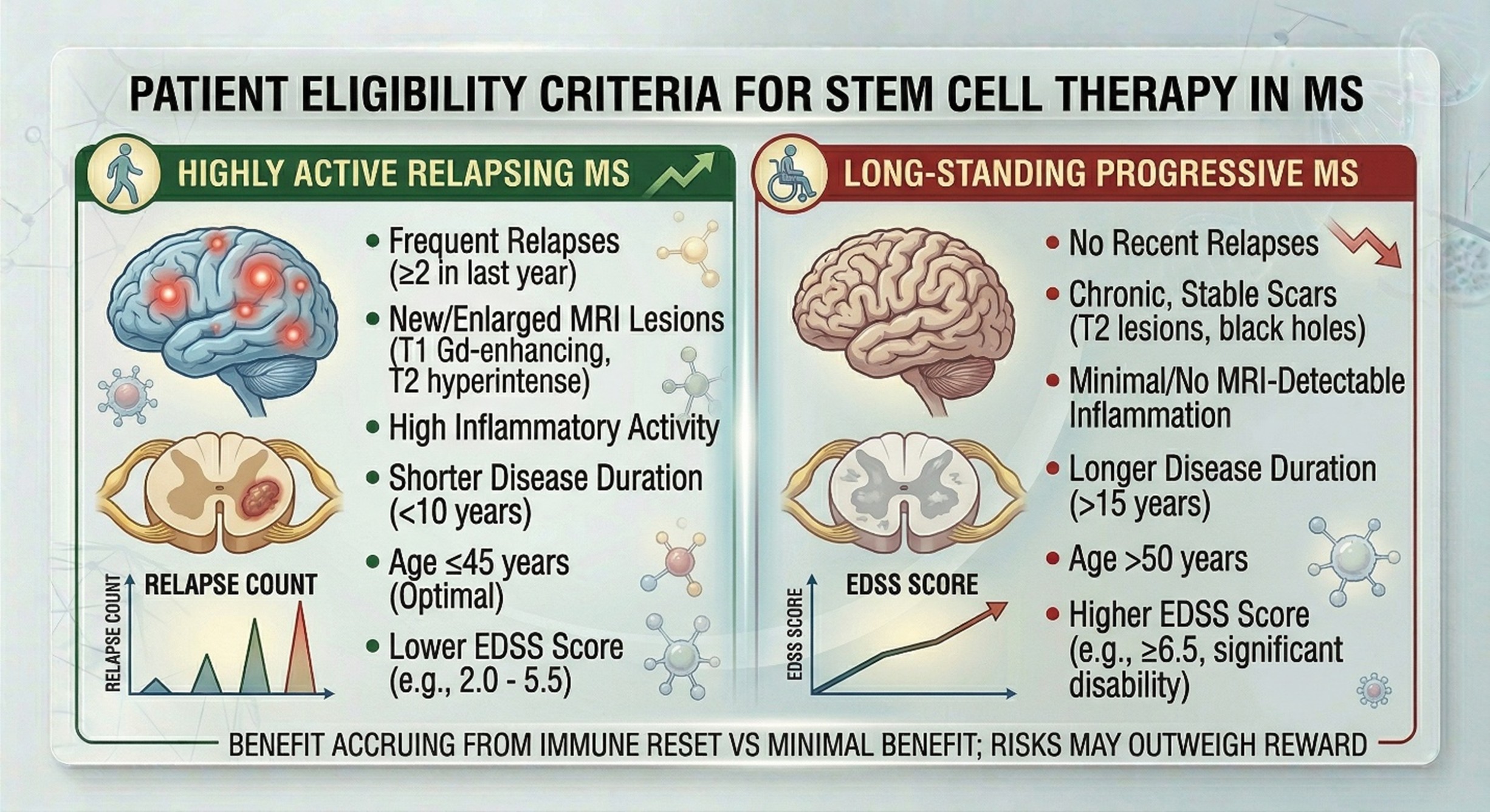
The most clinically grounded stem cell option for multiple sclerosis today is still aHSCT, especially for selected people with highly active relapsing disease. MS Society UK says people are most likely to benefit if they have highly active relapsing MS, because the treatment targets the inflammatory immune activity driving relapses and new lesions. A 2025 review in Nature Reviews Neurology also noted that because of high risk and low or no benefit, aHSCT is not recommended for people with long-standing, advanced forms of MS with substantial disability and little active inflammation. That is an important detail, because it shifts the conversation away from “anyone with MS should try stem cells” toward “the right patient, at the right stage, in the right setting.”
That more selective view is one reason a serious stem cell clinic discussion should sound different from a sales pitch. In real medicine, the question is not whether stem cells sound exciting. The question is whether the patient’s pattern of multiple sclerosis matches the biology the treatment is most likely to influence. A person with aggressive inflammatory relapsing disease is not in the same clinical position as someone with long-standing progressive disability and little active inflammation. This is why clinicians and consensus papers keep returning to patient selection, timing, and disease phenotype as the heart of the conversation around stem cell therapy for MS.
- What a Stem Cell Clinic Should Help a Person With Multiple Sclerosis Understand
A credible stem cell clinic for multiple sclerosis should do more than repeat the phrase stem cell therapy for MS. It should help patients understand which stem cell approach is actually being discussed, whether the goal is immune reset or experimental repair, what evidence exists for that specific approach, and what level of uncertainty remains. The National Multiple Sclerosis Society says aHSCT for MS should take place at centers with expertise in both MS care and stem cell transplantation, and its materials emphasize multidisciplinary transplant teams with neurology and hematology expertise. In other words, a serious stem cell clinic should look more like a coordinated medical program than a wellness brand using research language.
This is meaningful because when people search for a stem cell clinic, emotional appeal often plays a big role in their decisions. They are often out of energy, so they are drawn to any treatment, even if it is not up to date, yet much less definitive. Anyone taken in by weak but impressive words can easily come away with their brain eaten. The more powerful hospitals will be those that explain not only possible benefits but also intensity, risk, eligibility, and follow-up. And what does success really mean in multiple sclerosis? UCLH and Sheffield Teaching Hospitals say that aHSCT is an ‘intensive’ treatment involving chemotherapy, not merely an upgrade into being able to walk away from hospital as an outpatient. And with risks that are well defined rather than unknown.
- Why Caution Still Matters
Despite the excitement around stem cell therapy for MS, the regulatory message remains very clear. The FDA says regenerative medicine therapies have not been approved to treat neurological disorders such as multiple sclerosis and warns that patients offered such products outside legitimate regulatory pathways may be exposed to serious risks, including infection, unwanted immune reactions, neurological events, and treatment failure. The FDA also explicitly says that being listed on ClinicalTrials.gov does not mean a product is legally marketed or proven effective. That makes caution part of good medical judgment, not negativity.
This is also why the phrase ‘stem cell clinic‘ should be used in MS content only cautiously. This is a powerful search term, but it gives the false impression that all clinics providing stem cell-related care for multiple sclerosis are working from the same level of evidence. They aren’t. Some programs are closely tied to academic transplant frameworks and have formal eligibility criteria. Others may be using the language of regenerative medicine, yet without that same level of transparency and oversight. And for someone considering stem cell therapy for MS, the distinction matters as much as their treatment actually does.
The Real Reason This Topic Keeps Growing
What makes this subject so compelling is that it sits exactly where modern medicine is most emotionally charged: between hope and proof. Multiple sclerosis is a life-changing disease. Stem cell therapy for MS is not fantasy; it is a real area of clinical research and, in the case of aHSCT, a real treatment option for selected patients in the right setting. But it is also not a blank check for every stem cell clinic to imply universal benefit. That tension is precisely why the topic keeps growing online. People want an option that feels bigger than maintenance. Science is starting to offer pieces of that story. But the full story still requires careful selection, expert centers, and honesty about limits.
The most useful takeaway for a person searching today is not “stem cells are the answer” or “stem cells are hype.” It is more human than that. If you are living with multiple sclerosis, looking into a stem cell clinic may be reasonable when it comes from a serious desire to understand all legitimate options. But the best next step is not the loudest promise. It is a medically grounded evaluation of whether stem cell therapy for MS fits the type, stage, and activity of the disease you actually have. That is what turns a search term into a real treatment conversation.