Chronic kidney disease (CKD) is a progressive condition with high prevalence worldwide. As the kidneys fail, patients can become fatigued and retain fluid as well as metabolically imbalanced effects so debilitating that they have a major impact on quality of life. Conventional treatments are designed to slow the disease down, but they do not directly repair damaged kidney tissue.
The field of regenerative medicine, which incorporates the application of umbilical cord (UC)-derived mesenchymal stem cells (MSC), has recently emerged as a potential supportive therapy. This essay will aim to explain why kidney disease is a challenging entity to reverse and in what ways UC-MSC stem cell therapy may help support the function of your kidneys.
1: Why Kidney Disease Is Difficult to Improve
The limited regenerative capacity of kidney tissue is a major reason kidney disease is so difficult to treat. Unlike some other organs, the kidneys have a limited capacity to repair themselves after irreversible damage has occurred. There are multiple biological factors involved in disease progression.
First of all, chronic inflammation is central to continuous tissue damage. This chronic state of inflammation may slowly damage the architecture and function of the kidney.
Second, fibrosis or scarring accumulates over time and replaces healthy tissue with non-functional tissue. Fibrosis is hard to reverse once it has happened.
Also, diminished blood supply in the kidneys reduces oxygen and nutrient delivery, further compromising cellular function. Oxidative stress further causes injury to cells, furthering the decline in kidney function. These factors together form a cycle through which damage does not abate even with standard treatment.
2: Limitations of Conventional Treatment
CKD is been mainly treated by current therapies focused on symptom management and disease progression delay. These are blood pressure control, blood sugar regulation, dietary modification and dialysis in advanced stage.
These techniques are crucial, but come with limitations. They do not rebuild damaged kidney tissue, and patients can continue to see a gradual decline over time. In many cases, treatment becomes increasingly reliant on long-term management rather than recovery.
This is another reason why we need new therapies that target the disease in its underlying biology and especially those that promote tissue repair and cellular function.
3: How UC-MSC Stem Cell Therapy May Help
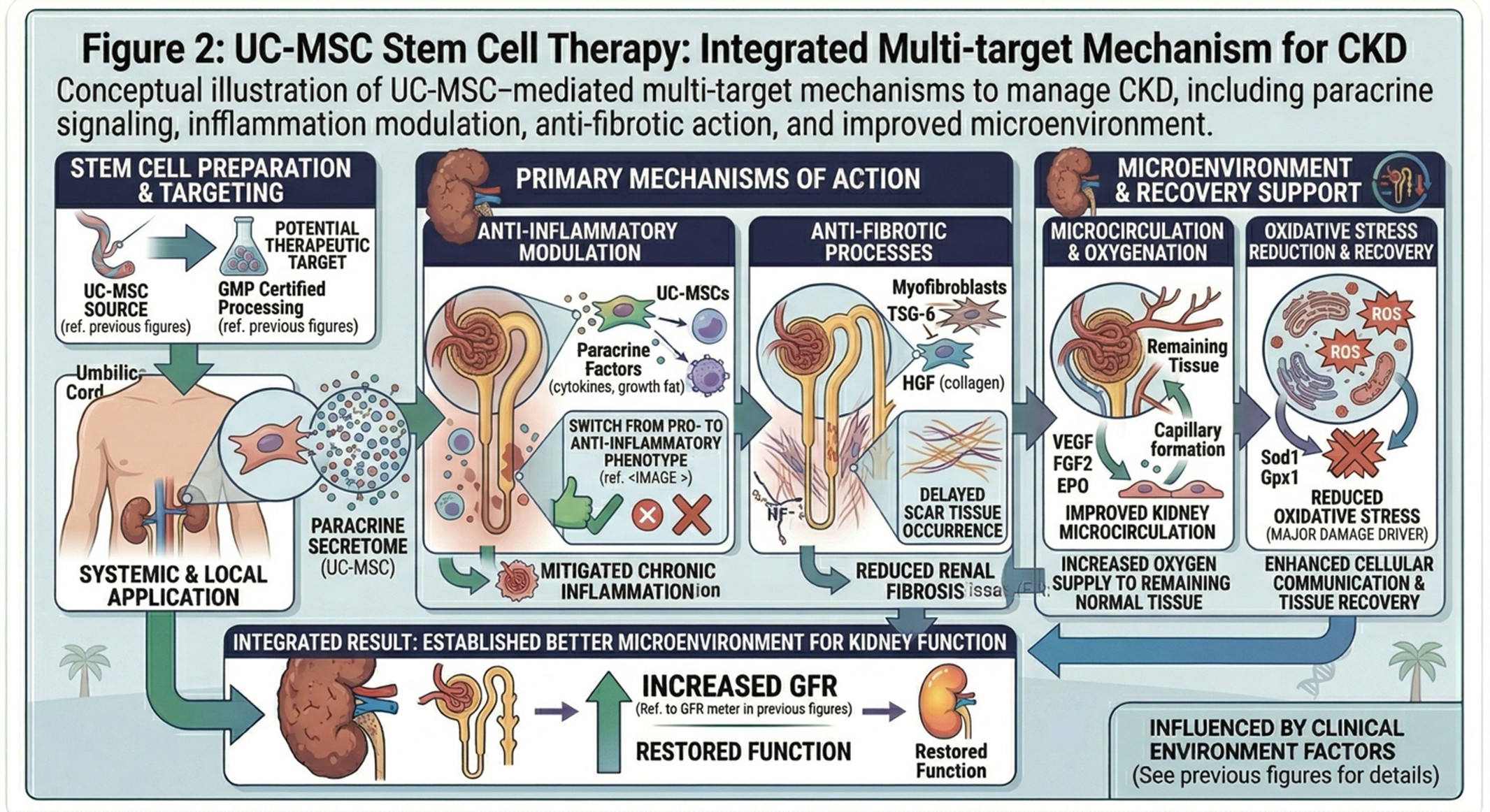
UC-MSC stem cell therapy manages this issue differently, it concentrates on enabling the kidney’s interior environment. Instead of replacing kidney cells directly, these stem cells are thought to communicate via paracrine signaling, where they release bioactive molecules that affect tissues in their intermediary milieu.
There are a number of potential mechanisms being explored. In addition, UC-MSCs was found to modulate the inflammatory process, thus, mitigating CKD-associated chronic inflammatory state. They may also help anti-fibrotic processes, possibly delaying the occurrence of scar tissue. These cells also release growth factors, enhancing cellular communication and tissue recovery.
Additionally, UC-MSCs might improve kidney microcirculation to supply more oxygen and support the remaining normal tissue. They might also reduce oxidative stress, a major driver of cellular damage.
While the mechanisms are still being studied, it potentially indicates that stem cell therapy could establish a better microenvironment for the kidney to function.
Conclusion
When it comes to chronic kidney disease, improvement is complicated by factors including inflammation, fibrosis, reduced perfusion and limited regenerative capacity. Conventional treatments are effective in controlling the condition but do not repair damaged tissue.
Therapies that focus on regenerative approaches, such as UC-MSC stem cell therapy, which support the kidney environment through pathways related to inflammation control, cellular signaling, and tissue support. Although this treatment is still experimental and results will vary, it is a hopeful step forward in the treatment of chronic kidney disease.
For many patients, the goal is not complete reversal, but stabilization, improved function, and a better quality of life.

