Chronic kidney disease (CKD) is a progressive disorder characterized by the decline of the kidneys’ ability to filter metabolic waste, regulate fluid and maintain overall homeostasis. As the disease progresses, patients can feel fatigued and experience swelling, high blood pressure and even require dialysis in severe cases.
Standard treatments are focused on slowing disease progression and controlling complications. But they do not directly restore damaged kidney tissue. This has been associated with increasing interest in regenerative strategies, including umbilical cord–derived mesenchymal stem cells (UC-MSCs), as a supportive intervention in kidney health.
Why Kidney Disease Is Difficult to Reverse
Kidney disease is also challenging to treat because the kidneys have very low regenerative capacity after significant damage has been done.
Principal factors contributing in CKD progression include:
- Chronic inflammation, which leads to persistent damage of tissues
- Fibrosis (scarring), which reduces functional kidney tissue
- Functional nephron loss with reduced filtering ability
- Decreased blood flow, which compromises oxygen transport
- Oxidative stress, causing cellular injury
These processes form a cycle of harm that becomes difficult, if not impossible to undo as time goes by.
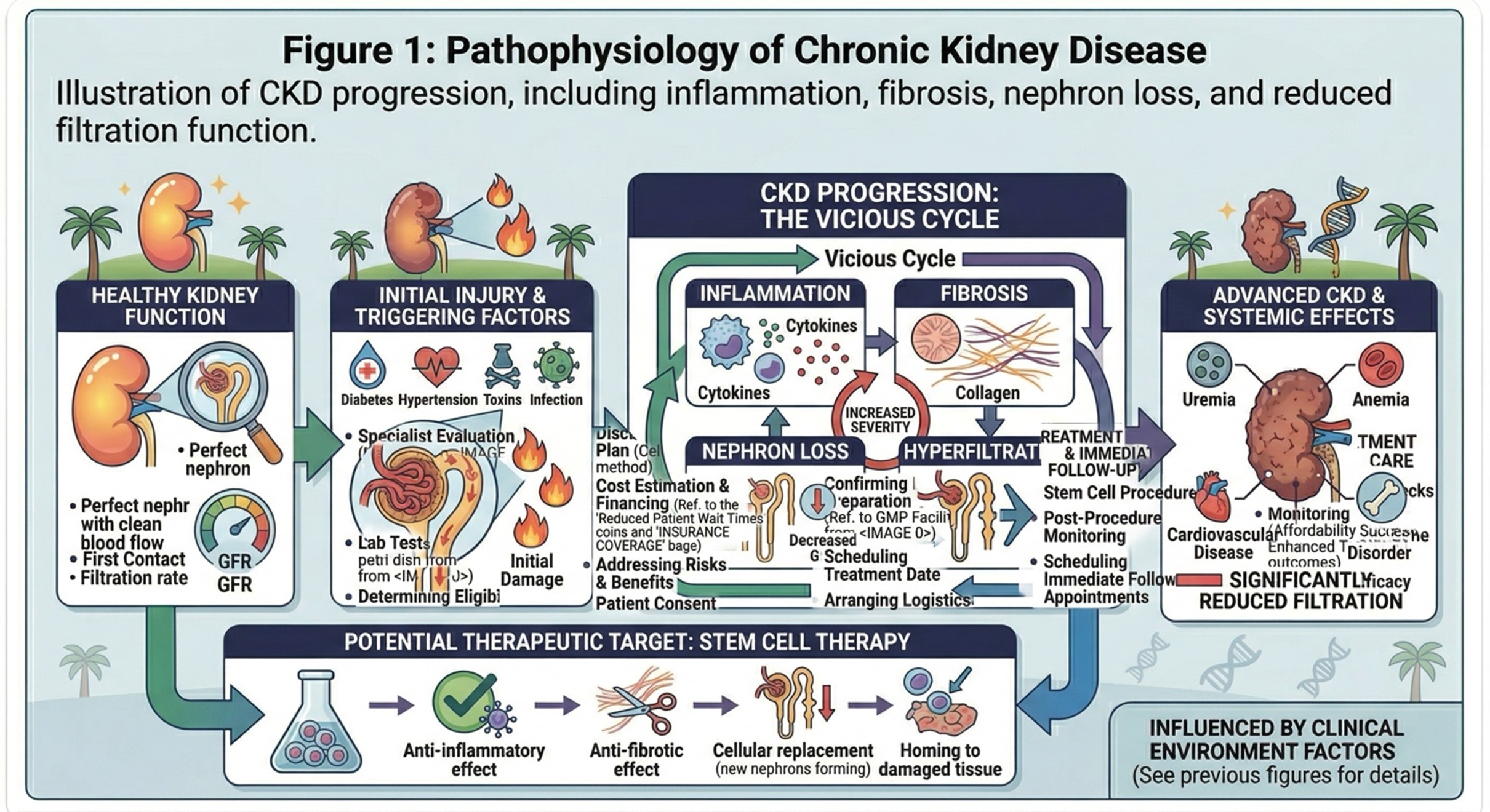
Illustration of CKD progression, including inflammation, fibrosis, nephron loss, and reduced filtration function.
Limitations of Conventional Treatment
The current management strategies of CKD are aimed at symptom control and limiting progression.
Common approaches include:
- Blood pressure and glucose control
- Medications that minimize protein loss through urine
- Dietary modifications
- Dialysis in advanced stages
- Although these treatments are vital, they have their limits:
- Do not regenerate injured kidney tissue
- Progression may continue despite treatment
- Long-term dependency on supportive therapies
- Dialysis impacts quality of life
This emphasizes the need of potentially biological mechanisms that could support kidney tissue.
How UC-MSC Stem Cells May Help
In addition, studies on human UC-MSCs in our laboratory focus more on their potential to secrete paracrine factors to help with tissue repair rather than directly replace kidney cells.
These cells secrete bioactive molecules like growth factors, cytokines and extracellular vesicles that could potentially modulate the kidney milieu.
Potential supportive mechanisms include:
- Anti-inflammatory effects
- Assisting in the reduction of chronic inflammation in kidney tissue
- Anti-fibrotic activity
- Can potentially slow down or modulate scarring processes
- Improved microcirculation
- Enabling blood flow aids in protecting kidney structures
- Cellular signaling support
- Enhancing communication between kidney cells
- Reduction of oxidative stress
Limiting further cellular damage
These mechanisms can drive a more friendlier environment for persistence of the renal reserve.
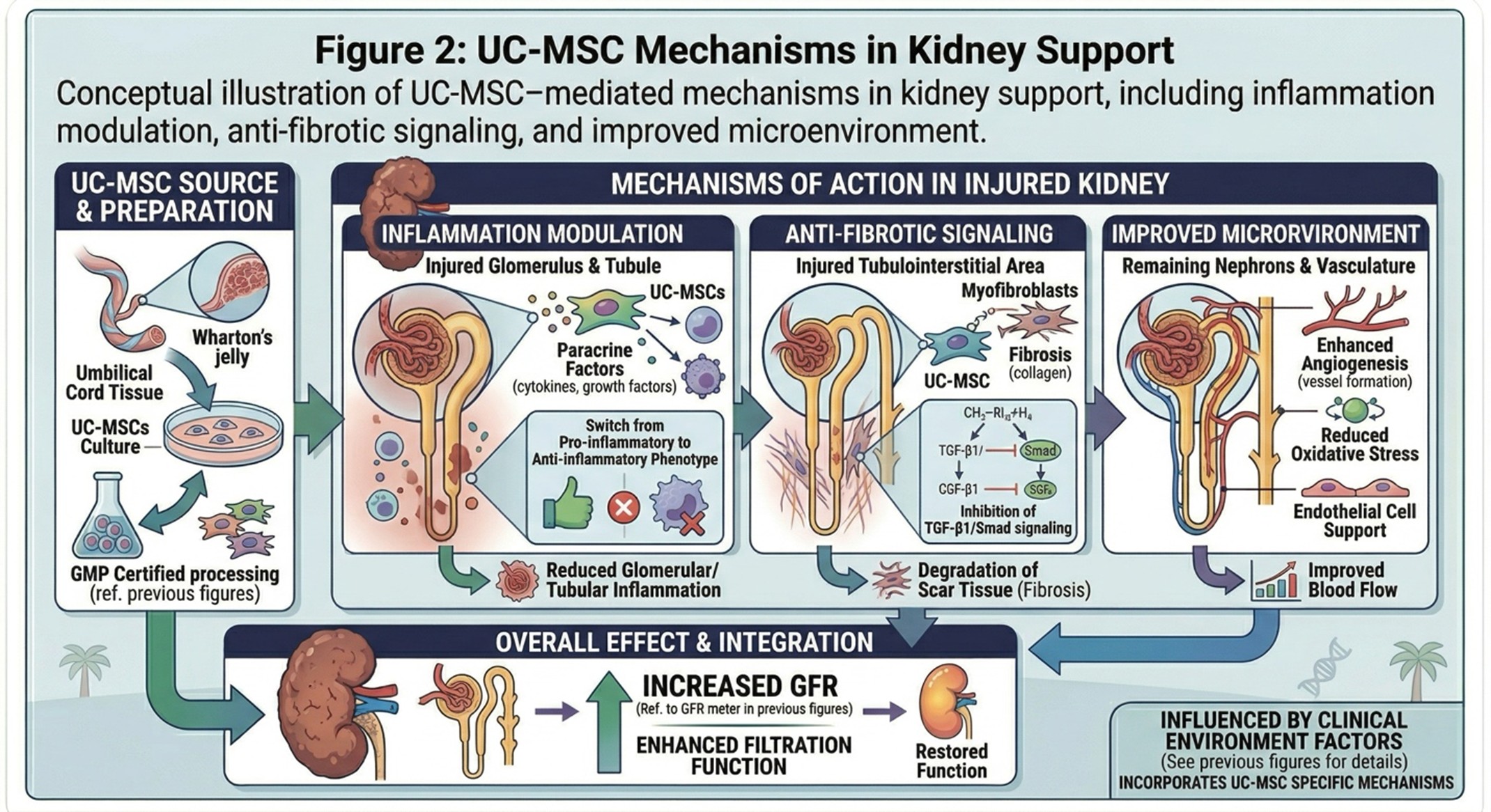
Conceptual illustration of UC-MSC–mediated mechanisms in kidney support, including inflammation modulation, anti-fibrotic signaling, and improved microenvironment.
What Patients May Experience
Also, Set realistic expectations for this topic. The therapy is not a cure for kidney disease, but rather may serve as a supportive approach.
Some patients may aim for:
- Stabilization of kidney function
- Slower progression of disease
- In some instances, improvement in specific clinical markers
- Better overall well-being
Outcomes vary depending on:
Stage of kidney disease
Underlying cause (e.g., diabetes, hypertension)
Overall health condition
- Treatment protocol and follow-up care
Conclusion
Common pathological features of CKD include inflammation, fibrosis, and progressive loss of function. Conventional treatments, while necessary, do not cure a sick tissue.
UC-MSC stem cell therapy is an innovative regenerative approach to support the kidney environment with inflammation control, anti-fibrotic signaling and enhanced cellular communication.
Though still investigational, this strategy reflects a wider shift toward biologically informed approaches in chronic disease management. The goal for many patients is to preserve whatever kidney function remains, slow the progression of disease and improve quality of life.

