There is a certain kind of back pain people tend to ignore at first. It is not the dramatic kind that drops you to the floor. It is the kind that begins quietly: stiffness after sitting, pain that gets worse with bending or lifting, and a lower back that seems less forgiving than it used to be. That’s why the symptoms of Degenerative Disc Disease are often not clear. Cleveland Clinic notes that disc degeneration is a natural part of aging, that most people have some degeneration after age 40, and that symptoms often show up as back pain that can worsen with sitting, bending, or lifting rather than as one single catastrophic event.
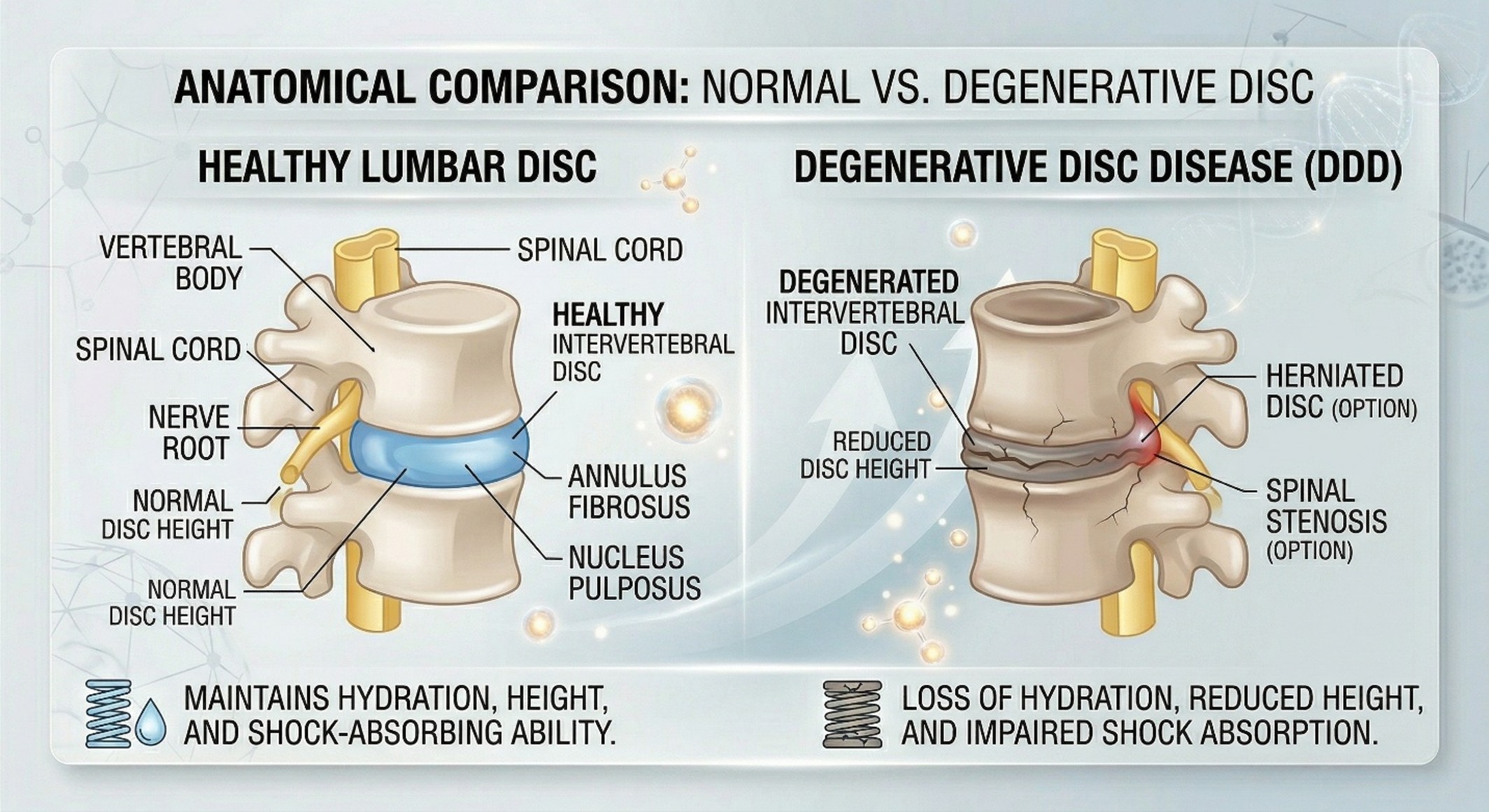
That slow beginning matters because Degenerative Disc Disease is not really a headline-friendly condition. It does not always look affected on day one. But over time, it can become one of the most frustrating forms of chronic back pain because the spinal discs lose hydration, height, and shock-absorbing ability. Cleveland Clinic describes degenerative disc disease as the wearing down of spinal discs over time, sometimes leading to herniation, spinal stenosis, or vertebral instability, while a 2025 review from World Neurosurgery calls degenerative disc disease a significant cause of chronic low back pain and disability.
For years, the usual scenario was predictable: physical therapy, pain relief medications, activity modifications, selected patients receiving injections—most frequently in the lower back and neck zones— and then in those instances that really did necessitate it, surgery. That hasn’t gone away. But the story ‘s verge has shifted. A growing part of the spine world is now posing the question: Can the disc itself be biologically supported, rather than being managed only by mechanics? That’s where regenerative medicine thailand itself becomes a helpful framing keyword. It puts Thailand in a larger global discussion about how the future may bring more biology for chronic spinal pain. The important point to make is that regenerative disc care is still being developed. Current treatments do not reverse degeneration and a review in the World Journal of Neurosurgery 2025, for example, states that bioactive therapies— including cell-based strategies— are still being investigated to try to target the degenerative process itself.
The most interesting update is that this is no longer only a laboratory story. A 2025 PRISMA-compliant systematic review found that preclinical models of stem-cell therapy for degenerative disc disease showed meaningful regenerative signals, including restoration of disc height and extracellular matrix, while human clinical evidence from thirteen low-to-moderate-quality trials showed modest but statistically significant improvements in pain and disability. That is not the same as a cure, and the same review emphasized that imaging proof of true biological repair in humans remains limited. Still, it is enough to explain why It is enough to explain why stem cell therapy for back pain thailand sounds less like a fringe phrase than it did a few years ago sounds less like a fringe phrase than it did a few years ago.
The newest trial data made the picture even more interesting, not simpler. In 2025, the DREAM Study reported preliminary results from a double-blind phase IIB randomized trial of intradiscal autologous bone-marrow-derived mesenchymal stromal cells in patients with chronic low back pain from moderate-to-advanced multilevel disc degeneration. The treatment appeared safe, and the researchers reported structural changes such as improvement in disc height index. But the trial did not show superior pain or disability outcomes over sham treatment at six months. That is exactly the kind of result that makes this field feel real: promising enough to stay in the news, but not clean enough to justify overconfident marketing.
And that is where the article gets more honest than most promotional pages. A phrase like stem cell therapy for back pain thailand can sound as if the science has already arrived, when in reality the science is still negotiating with the biology. Intervertebral discs are hard places to regenerate. The 2025 systematic review points out that the disc has a hostile, avascular microenvironment, which is one reason translation from early promise to dependable clinical benefit has been difficult. The same review concludes that current trials still have significant methodological weaknesses that limit their immediate application to routine daily practice. In other words, the back pain story is moving, but it is not finished.
That unfinished status is exactly why the FDA’s language matters. The agency says regenerative medicine therapies have not been approved for orthopedic conditions such as disc disease or back pain, and it warns that products are often marketed as safe and effective even when they have not been adequately studied under an IND. The FDA also lists real risks associated with illegally marketed regenerative products, including infection, unwanted inflammatory responses, and treatment failure when approved options are available. So if a reader lands on a page about regenerative medicine thailand or stem cell therapy for back pain thailand, the most trustworthy message is not “this already works for everyone.” It is “this is an active and serious area of research, but it is not a settled routine therapy.”
That’s another reason, Degenerative Disc Disease has become especially topical news lately. It’s in the uncomfortable space between a massive demand from patients for treatment and incomplete clinical clarity. Those suffering chronic discogenic back pain don’t want to hear just about how to get by. Those researchers who are looking for things that will reduce symptoms while also changing the biology of an illness, don’t want simple quick fixes. And doctors are waiting to see whether this field dai marydis is going to be important in coming years — crispyCourses for the information page tell us that it has to develop before anyone judges how home runs are being scored. In 2025, the World Neurosurgery Review wrote: Preliminary studies show that new techniques can both alleviate pain and regenerate the diseased disc, but long-term efficacy remains unclear. And while progress requires clinical trials, biomaterials improvements, better selection standards for patients.
So the strongest way to write about regenerative medicine thailand is not to make it sound like magic. It is to make it sound current. The current story is this: Degenerative Disc Disease remains one of the most stubborn drivers of chronic back pain; conventional care still matters; stem-cell-based disc therapies are now supported by enough preclinical and early clinical work to command serious attention; but the evidence still stops short of giving the field a simple victory speech. For readers drawn to terms like stem cell therapy for back pain thailand, that is actually the more powerful message. It means the field is no longer pure hype, but it is still young enough that honesty remains part of good medicine.