Diabetes related wounds which in particular include diabetic foot ulcers are a very difficult set of complications. These wounds may take weeks or even months to heal and report to also affect mobility, independence and in large scale, quality of life. In severe cases they may cause infection, hospitalization, or in the worst, amputation. In the field of standard wound care which we have come to rely on greatly many patients are experiencing delayed and poor healing. This has caused us to look more into what is it that makes diabetic wounds so hard to heal and we are exploring advanced methods like stem cell therapy to support the healing process
Why Diabetic Wounds Are Difficult to Heal
In diabetic patients what we see is that the body’s normal healing process is disrupted. In which non diabetics present a sequence of stages in wound healing hemostasis, inflammation, proliferation and remodeling in diabetics this process is often broken.
Also at play in this issue are biological factors:.
- Reduced blood flow.
- Diabetes cause damage to blood vessels which in turn reduces delivery of oxygen and nutrients.
- Ongoing inflammation.
- Instead in a state of constant inflammation wounds may.
- Nerve damage.
- Loss of feeling which in turn causes go undetected injuries and repeat trauma.
- Disordered cellular activity.
- Key repair cells like fibroblasts and keratinocytes may not function well.
- Oxidation stress.
- Increased cell damage also delays tissue repair.
These factors produce an environment in which wounds do not heal even with proper care.
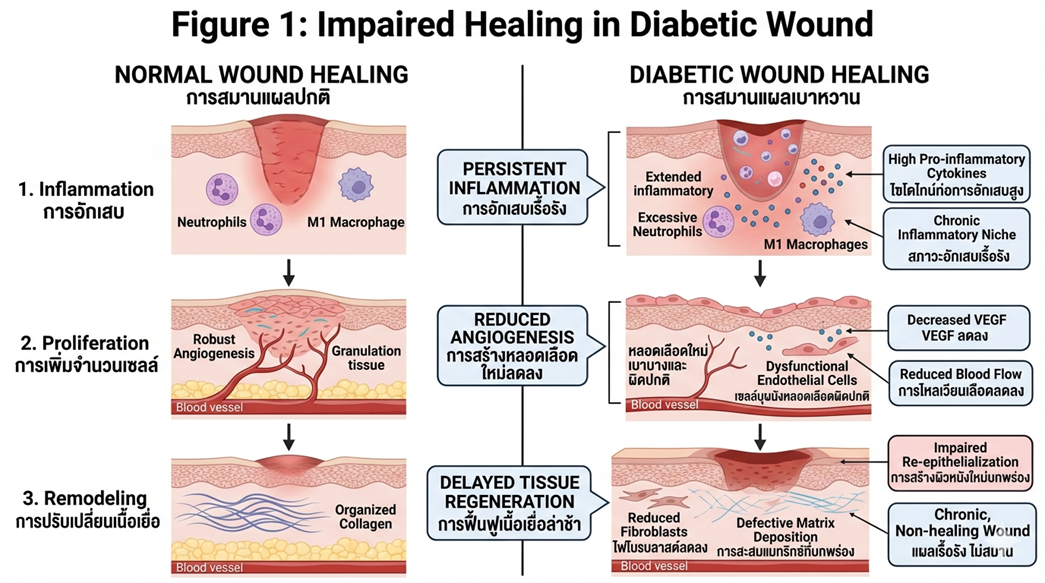
Illustration of impaired wound healing in diabetes, highlighting reduced angiogenesis, persistent inflammation, and delayed tissue regeneration.
Limitations of Conventional Treatment
Standard care of diabetic wounds is for symptom management and prevention of complications.
Here are some which do it:
- Wound care products and moisture management.
- Antibiotic treatment of infection.
- Wound cleaning of dead tissue.
- Pressure relief.
While we have these important treatments which do have their place they also have their limitations:
- They don’t repair impaired cellular repair processes.
- Healing may be a slow process or incomplete.
- Wounds can present again.
- Underlying medical issues are not fully addressed.
Some patients are still at issue with chronic non healing wounds despite which they are receiving care.
How Stem Cell Therapy May Help
Stem cell therapy reports to put forth a different approach which is that of the biological environment of the wound. What we see is that Mesenchymal stem cells (MSCs) which include those from the umbilical cord tissue are the most studied. It is thought these cells mostly via paracrine signaling which is to say they produce bioactive molecules that in turn affect the nearby cells.
Which also include:.
- Control of inflammation.
- Reducucing overzealous inflammatory reactions in the wound.
- Development of angiogenesis.
- Supporting the growth of new blood vessels which in turn improves circulation.
- Growth factor communication.
- Improving cell to cell communication in repair processes which present in your text.
- Tissue activation.
- Supporting skin, fibroblasts, endothelial cells.
- Tissue remodelling.
- Developing the framework and health of new tissue.
These combined results may put the wound into a more active healing phase from a chronic non-healing state.
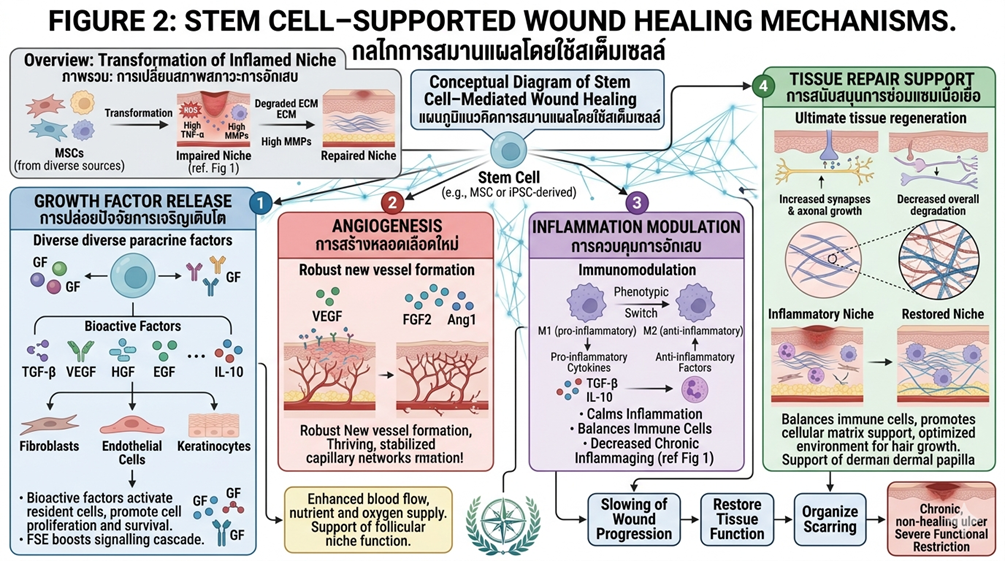
Conceptual illustration of stem cell–mediated wound healing, including growth factor release, angiogenesis, inflammation modulation, and tissue repair support.
Clinical Perspective and Realistic Expectations
It is very important to note that stem cell therapy does not guarantee a cure for diabetic wounds. Instead it is put forth as an addition to what is the body’s natural healing process.
Providers should note:.
- Results may fluctuate based on the severity of the wound and health.
- Treatment in addition to standard wound care.
- Early intervention improves results.
- Ongoing care is a must.
For many patients even small improvements in healing are reported to greatly affect daily life and reduce the risk of complications.
Conclusion
Diabetes causes poor healing of wounds which in turn is a result of low blood flow, chronic inflammation, nerve damage, and impaired cellular function. Though we use traditional treatments they do not always deal with the base biological issues. Stem cell therapy presents a regenerative approach which at a cellular level supports the wound environment. It does this through processes like inflammation control, angiogenesis, and tissue repair which in turn may improve healing.
Although we are still in the early stages of this approach it is a part of a larger movement which has seen the introduction of more advanced and biological wound care strategies. For many patients this also brings forth an extra option which in turn improves healing results and quality of life.

