Spinal dysfunction is a broad term that includes degenerative disc disease (DDD), spinal stenosis, and neurogenic impairment which in turn present with chronic pain and reduced mobility. These conditions play also into disc degeneration, inflammation, and structural breakdown of spinal elements. Presently we see that treatment options are mostly for symptom relief which we get from pharmacological agents, physical rehab and in very advanced cases we turn to surgery. But what we see is that these interventions do not in fact repair the damaged spinal structures at a cell level. What we have recently seen is that in the field of regenerative medicine there is great interest in the role of mesenchymal stem cells (MSCs) in particular those derived from the umbilical cord (UC-MSCs) in terms of their ability to modulate inflammation and support tissue repair in the spine. Also Thailand has become a region wide hub for stem cell based therapies which they present with specialized clinical infrastructure and integrated care models. In this report we look at the pathophysiology of spinal dysfunction, the issues with current treatments and also the role of stem cell therapy in Thailand as an investigative approach for better spinal health.
Introduction
Spinal dysfunction is a leading cause of chronic musculoskeletal pain and disability globally. Degenerative disc disease (DDD), spinal stenosis, and nerve compression syndromes are more frequent in aging populations and sedentary lifestyles.
The intervertebral disc is an important structure in the spine as it enables both flexibility and load distribution. Degeneration of these discs creates structural instability, inflammation and nerve irritation/pain with loss of function. Current treatment approaches in RA mainly target symptom reduction and functional improvement, but do not aim to reverse the underlying degenerative mechanisms. Consequently, there is a rising interest in regenerative medicine strategies targeting the facilitation of tissue repair and recovery of spinal functions.
- Pathophysiology of Spinal Dysfunction
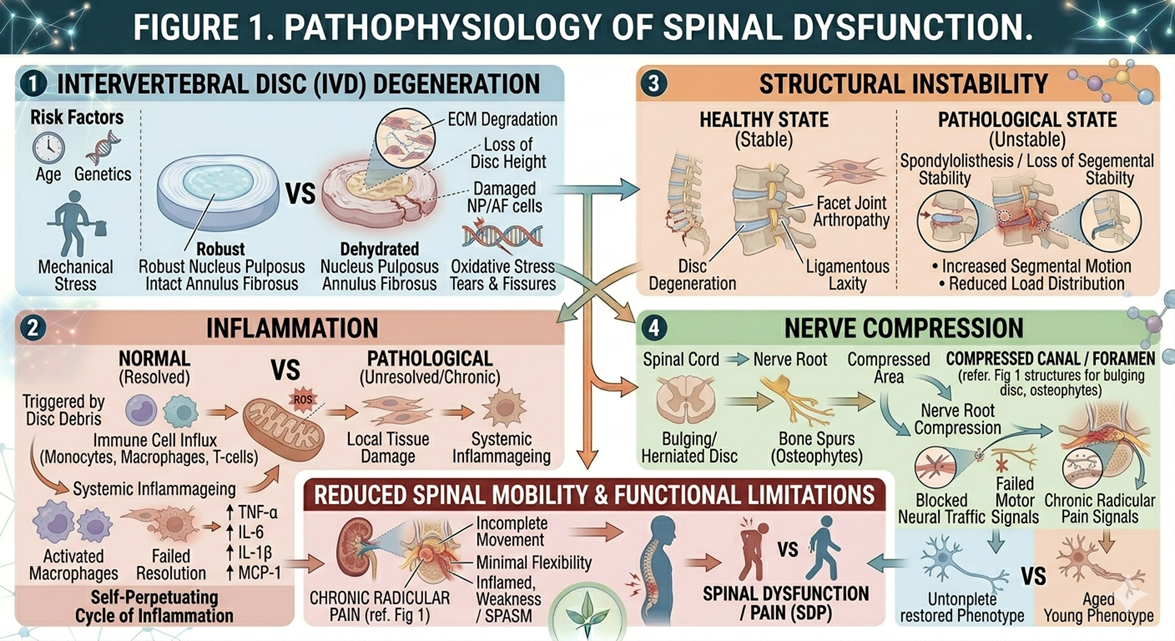
Spinal dysfunction arises from a combination of mechanical, biochemical, and cellular changes within the spine.
Intervertebral Disc Degeneration
Reduced disc height and elasticity due to the loss of proteoglycans, water content
Inflammation
Degenerative changes lead to an increased release of pro-inflammatory cytokines, which further contribute to pain and tissue damage.
Structural Instability
Changes in the biomechanics of the spine due to degenerated discs and weakened ligaments.
Nerve Compression
Disc bulge or foraminal stenosis can impinge nerve roots, resulting in radiculopathy.
Reduced Vascular Supply
Intervertebral discs receive relatively low blood supply, which hampers their natural healing processes.
Die these factors interleave to form a degenerative, inflammatory and functional cycle.
- Limitations of Conventional Therapeutic Approaches
Conservative or surgical modalities of treatment are the recognized standards for spinal dysfunction. Conservative treatments include pain control with nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy and lifestyle modification. Although these treatments can alleviate symptoms, they do not cure disc degeneration. Procedures like steroid injections could offer temporary alleviation but won’t restore structural damage. In more serious cases, surgical procedures — including spinal fusion or disc replacement — may be required. But this surgery is fraught with risk, and does not necessarily return the spine to normal function. Moreover, several patients are looking for options that can postpone or preclude the need for surgery.
- Mesenchymal Stem Cells in Spinal Regeneration
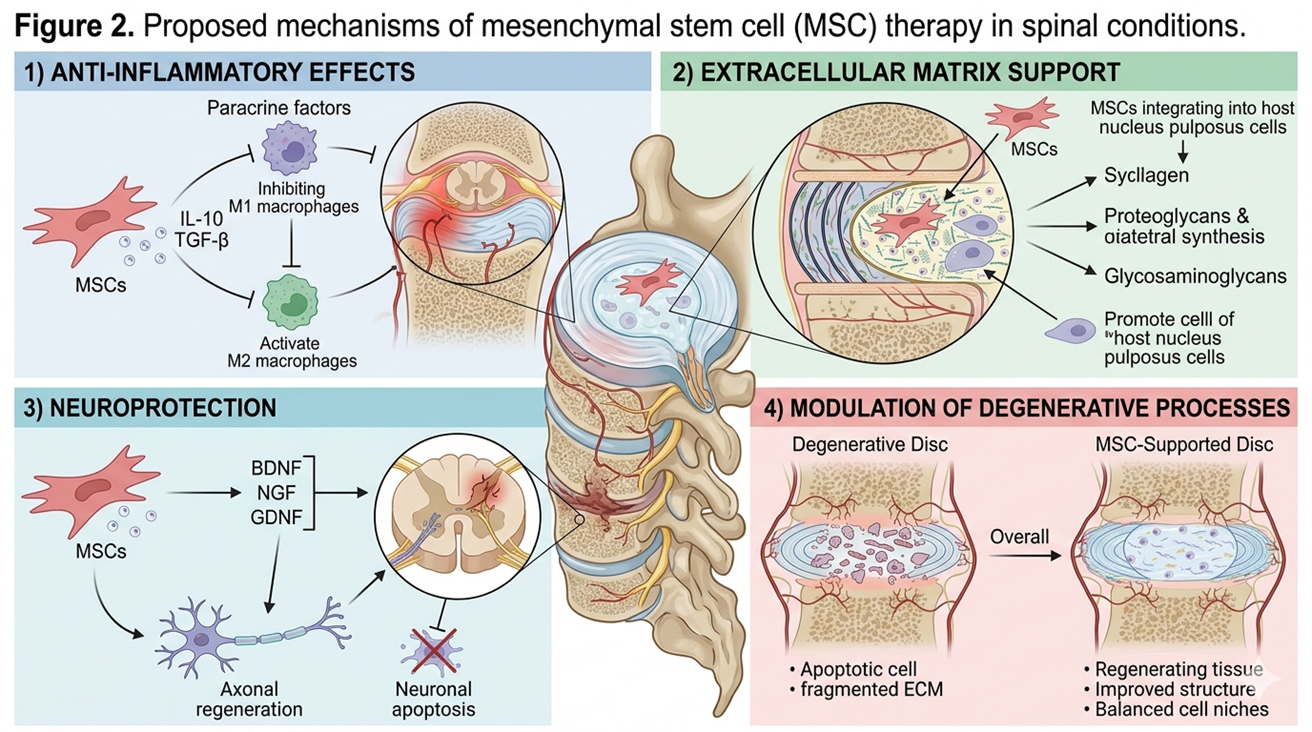
Mesenchymal stem cells (MSCs) which include umbilical cord derived MSCs (UC-MSCs) are a focus of research for their role in spinal tissue repair. Instead of directly replacing damaged tissue MSCs mainly in which they release bioactive substances and thus alter the local microenvironment. Also out that instead of direct repair of damaged tissue MSCs also don\’t do that what you may think rather, they secrete factors which in turn modify the local environment.
Proposed Mechanisms
Anti-inflammatory Effects
MSC-derived factors may reduce pro-inflammatory signaling within spinal tissues.
Extracellular Matrix Support
MSCs may influence the production of matrix components essential for disc integrity.
Hydration and Disc Support
Paracrine signaling may help support disc cellular activity and maintain structural properties.
Neuroprotective Effects
MSC-derived factors may support nerve health and reduce neural inflammation.
Modulation of Degenerative Processes
MSCs may influence pathways involved in disc degeneration and fibrosis.
Preclinical studies have shown improvements in disc structure and function in animal models. Early clinical studies suggest potential benefits, though further research is required.
Future Perspectives
The use of stem cell therapy for spinal dysfunction is a promising direction where the emphasis towards regenerative methods to address root organ tissue degeneration.
Future research directions include:
- Molecular mechanisms underlying MSC-mediated disc regeneration
- Optimizing delivery methods and dosing strategies
- Assessing long-term safety and clinical outcomes
- Find patient populations most likely to benefit
Cell-free methods like exosome-based therapies are also being investigated.
These therapies need to be tested in large clinical trials to determine their place in routine medical practice.
Conclusion
Spinal dysfunction is a multifactorial disease that involves disc degeneration, inflammation, and structural changes. While conventional therapies provide relief from symptoms, they do not repair harmed spinal tissues.
Stem cell–based therapies provide a promising approach to support tissue repair, modulate inflammation, and enhance spinal function with mesenchymal stem cells. The clinical applications in Thailand suggest growing interest towards regenerative, therapeutic approaches.
These therapies, though investigational, must be evaluated in future studies to determine its long-term clinical relevance. With advances in regenerative medicine, stem cell therapy could be an essential piece of future approaches to spinal health.

