Comprehensive Therapeutic Potential of UC-MSCs for PBC Patients seeking Treatment at a Leading Stem Cell Clinic Thailand
- Introduction to Primary Biliary Cholangitis and Modern Therapeutic Needs
Primary Biliary Cholangitis, commonly referred to as PBC, represents a chronic and progressive autoimmune liver malady that primarily targets the small bile ducts. When these ducts suffer from persistent inflammation and subsequent destruction, bile acids accumulate within the liver, leading to toxic cholestasis and eventually resulting in irreversible scarring or cirrhosis. For many patients, the diagnosis carries a heavy psychological and physical burden, as the unrelenting fatigue and debilitating pruritus significantly diminish their quality of life. While the medical community has relied on conventional treatments for decades, a substantial percentage of the patient population remains unresponsive or intolerant to these options. This therapeutic gap has necessitated the exploration of advanced regenerative medicine. Innovative approaches such as Stem Cell Clinic Thailand services are becoming increasingly vital. By utilizing UC-MSCs, researchers aim to address the underlying immune dysregulation rather than merely managing the symptomatic fallout of the disease.
- Pathophysiological Mechanisms and the Impact of Biliary Obstruction
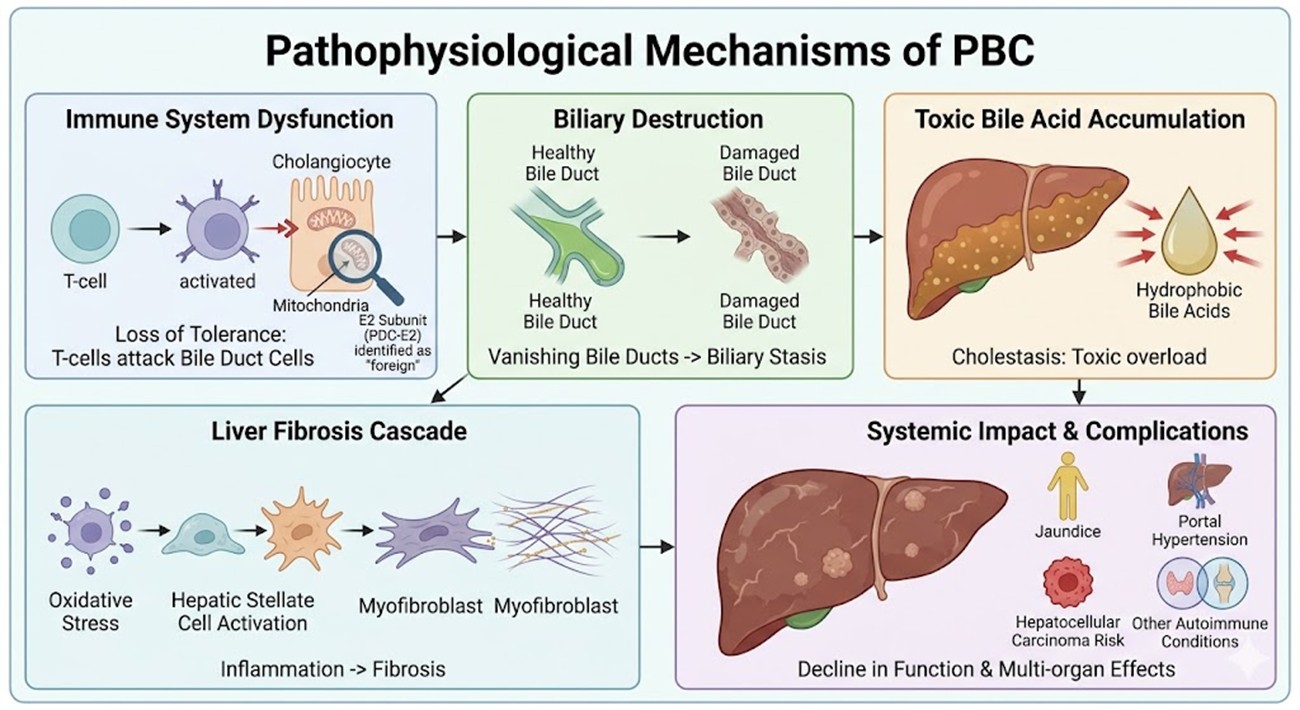
The development of PBC is characterized by a sophisticated interplay between genetic susceptibility and environmental triggers, leading to a loss of immune tolerance against biliary epithelial cells. Specifically, the immune system mistakenly identifies the E2 subunit of the pyruvate dehydrogenase complex within the mitochondria as a foreign threat. This triggers a T-cell mediated assault on the cholangiocytes. As the bile ducts vanish, the liver is subjected to a relentless influx of hydrophobic bile acids, which induce oxidative stress and promote the activation of hepatic stellate cells. This cascade facilitates the transition from localized inflammation to widespread fibrosis. Patients often experience a progressive decline in hepatic function, which can manifest as jaundice, portal hypertension, and an increased risk of hepatocellular carcinoma. The systemic nature of the inflammation means that the impact is not confined to the liver alone; it often correlates with other autoimmune conditions, further complicating the clinical management of the individual.
- Limitations of Conventional Pharmacological Interventions
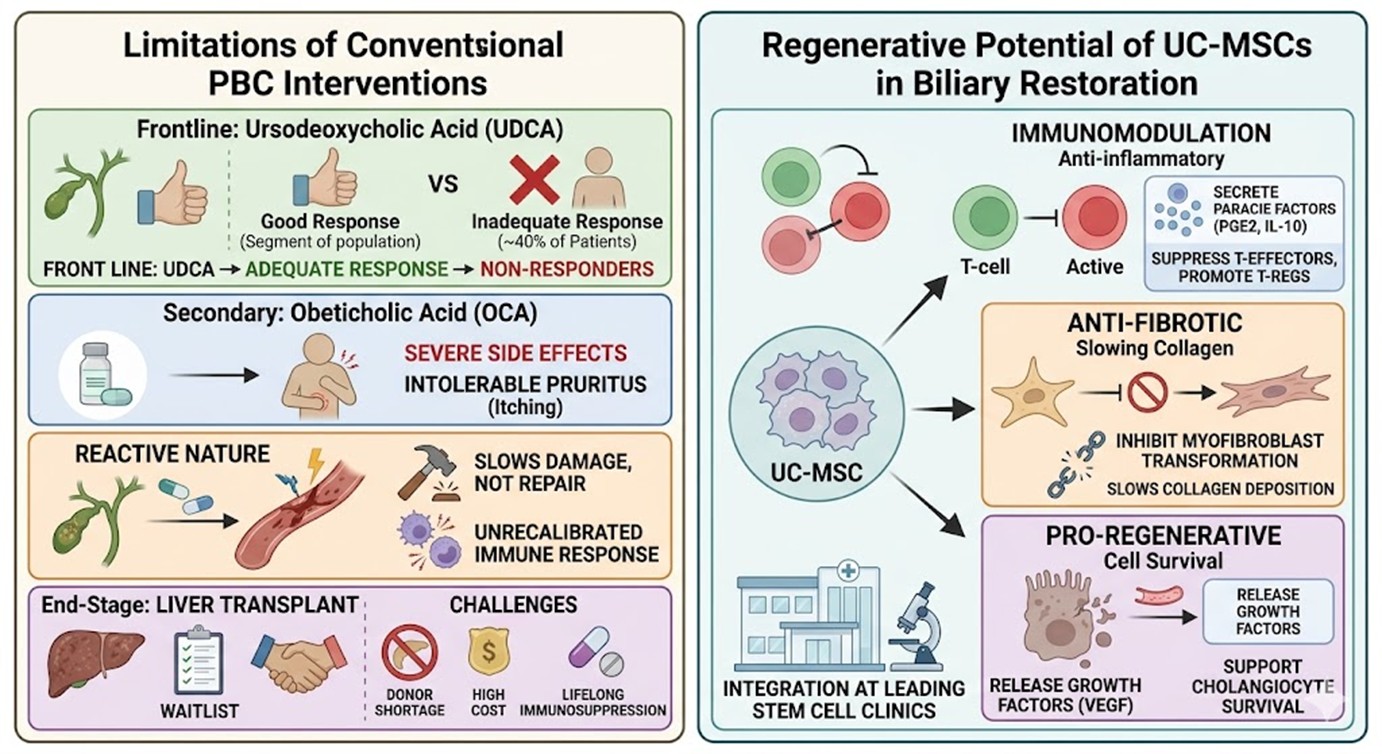
Currently, the frontline of defense against PBC involves the administration of Ursodeoxycholic Acid, which helps to improve bile flow and reduce liver enzyme levels. While effective for a segment of the population, approximately 40% of patients do not achieve an adequate biochemical response, leaving them at high risk for disease progression. Secondary options, such as Obeticholic Acid, exist but are frequently associated with severe side effects, most notably an exacerbation of skin itching that can become intolerable for the patient. Furthermore, these traditional therapies are largely reactive; they focus on slowing the damage caused by bile acids rather than repairing the biliary architecture or recalibrating the rogue immune response. Once the disease reaches the end-stage of cirrhosis, the only definitive solution is a liver transplant, which is fraught with challenges including donor shortages, high costs, and the lifelong requirement for immunosuppressive drugs.
- The Regenerative Potential of UC-MSCs in Biliary Restoration
The shift toward UC-MSCs as a primary candidate for PBC therapy is driven by their extraordinary immunomodulatory and trophic properties. Unlike adult-derived cells, umbilical cord-derived mesenchymal stem cells possess a more primitive state, offering higher proliferative capacity and lower immunogenicity. The mechanism of action is multifaceted. First, these cells exert a potent anti-inflammatory effect by secreting paracrine factors like prostaglandin E2 and interleukin-10, which suppress the overactive T-effector cells and promote the expansion of regulatory T-cells. Second, they address the fibrotic aspect of the disease by inhibiting the transformation of stellate cells into myofibroblasts, thereby slowing the deposition of collagen. Perhaps most importantly, UC-MSCs facilitate a pro-regenerative environment by releasing vascular endothelial growth factors that support the survival of remaining cholangiocytes. This comprehensive approach makes the integration of these cells a cornerstone of modern protocols at any leading Stem Cell Clinic Thailand facility.
- Future Trajectory of MSC Therapies in the Thai Medical Landscape
Thailand has rapidly emerged as a global epicenter for advanced biotechnological applications, particularly in the realm of regenerative medicine. The future of treating PBC in this region looks promising due to a combination of stringent regulatory frameworks and a high concentration of specialized expertise. Why choose Thailand for such sophisticated care? The nation offers a unique synergy of world-class laboratory infrastructure and highly trained clinical professionals who are well-versed in the nuances of mesenchymal cell application. As clinical trials continue to demonstrate the safety and efficacy of UC-MSCs, the integration of these therapies into routine hepatology care is expected to accelerate. Furthermore, the supportive ecosystem for medical tourism ensures that patients seeking a Stem Cell Clinic Thailand experience receive not only cutting-edge science but also a holistic approach to recovery that is difficult to replicate elsewhere. This localized expertise is essential for tailoring protocols to the specific inflammatory profiles of PBC patients.
In conclusion, the management of Primary Biliary Cholangitis is undergoing a significant paradigm shift from palliative care to restorative science. The limitations of current chemical-based treatments have paved the way for biological solutions that can actually influence the immune system’s behavior. The application of UC-MSCs offers a dual benefit of reducing hepatic inflammation while simultaneously combating the progression of fibrosis. By addressing the disease at a cellular level, this therapy provides a beacon of hope for those who have exhausted traditional avenues. As the sector grows, the reputation of a Stem Cell Clinic Thailand will likely rest on its ability to deliver these high-tech treatments with precision and safety. Ultimately, the goal remains the stabilization of liver function and the restoration of a healthy life for those living with PBC, marking a new era where the focus is on healing the body from within.

