Revolutionary Regenerative Potential of UC-MSCs for Patients Cirrhosis during Stem Cell Therapy in Thailand
Chronic liver injury is a global challenge, often culminating in liver Cirrhosis. This condition carries a significant burden due to high morbidity and mortality. When the liver sustains prolonged damage from viral hepatitis, alcohol, or NAFLD, the organ’s repair process leads to extensive scarring. As healthy tissue is replaced by fibrous nodules, essential metabolic, detoxifying, and synthetic functions are compromised. Patients face devastating impacts, from jaundice to life-threatening portal hypertension and hepatic encephalopathy. While medicine manages symptoms, a regenerative approach is urgent since standard drugs often fail to reverse fibrosis. Consequently, UC-MSCs (Umbilical Cord-Derived Mesenchymal Stem Cells) offer a promising frontier for restoring liver function beyond the limits of conventional medicine.
- Understanding the Pathogenesis and Clinical Severity of Liver Fibrosis
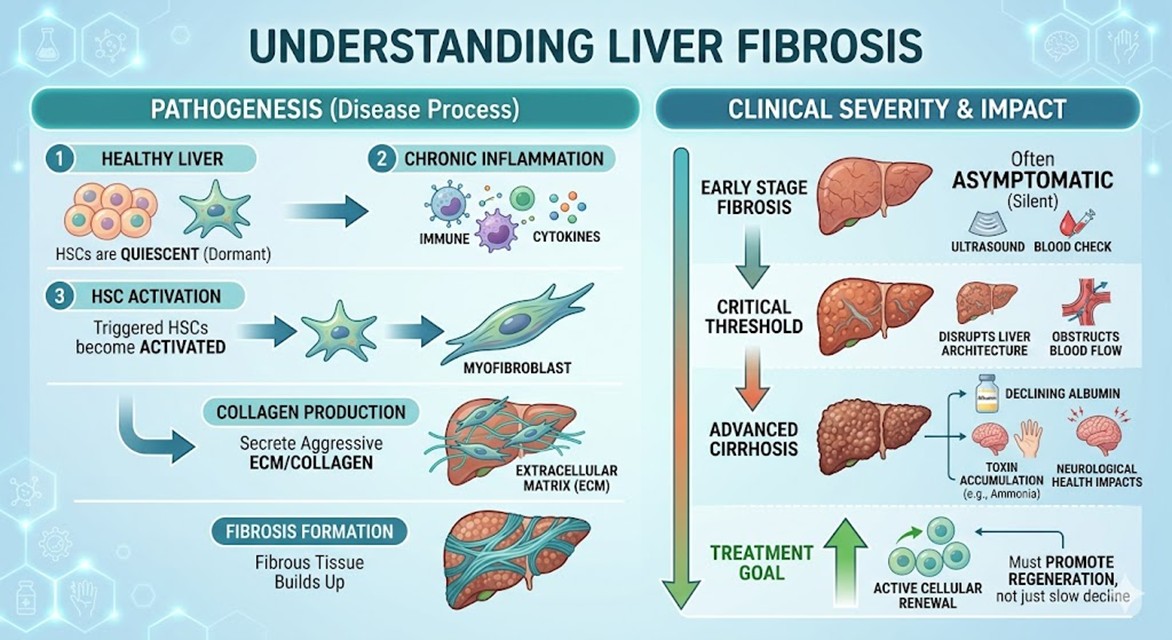
The progression toward Cirrhosis involves a complex cellular transformation. At the core is the activation of Hepatic Stellate Cells (HSCs). In a healthy liver, these cells remain quiescent; however, persistent inflammation triggers a shift into myofibroblast-like cells that aggressively secrete extracellular matrix (ECM) proteins, primarily collagen.
As fibrous tissue accumulates, it disrupts liver architecture, obstructing blood flow and nutrient exchange. While early stages are often silent, reaching a critical threshold leads to systemic failure. Severity is marked by declining albumin production and a failure to clear toxins like ammonia, impacting neurological health. The immense physical toll necessitates treatments that do more than slow decline—they must actively promote cellular renewal.
- Traditional Therapeutic Approaches and Inherent Limitations in Cirrhosis
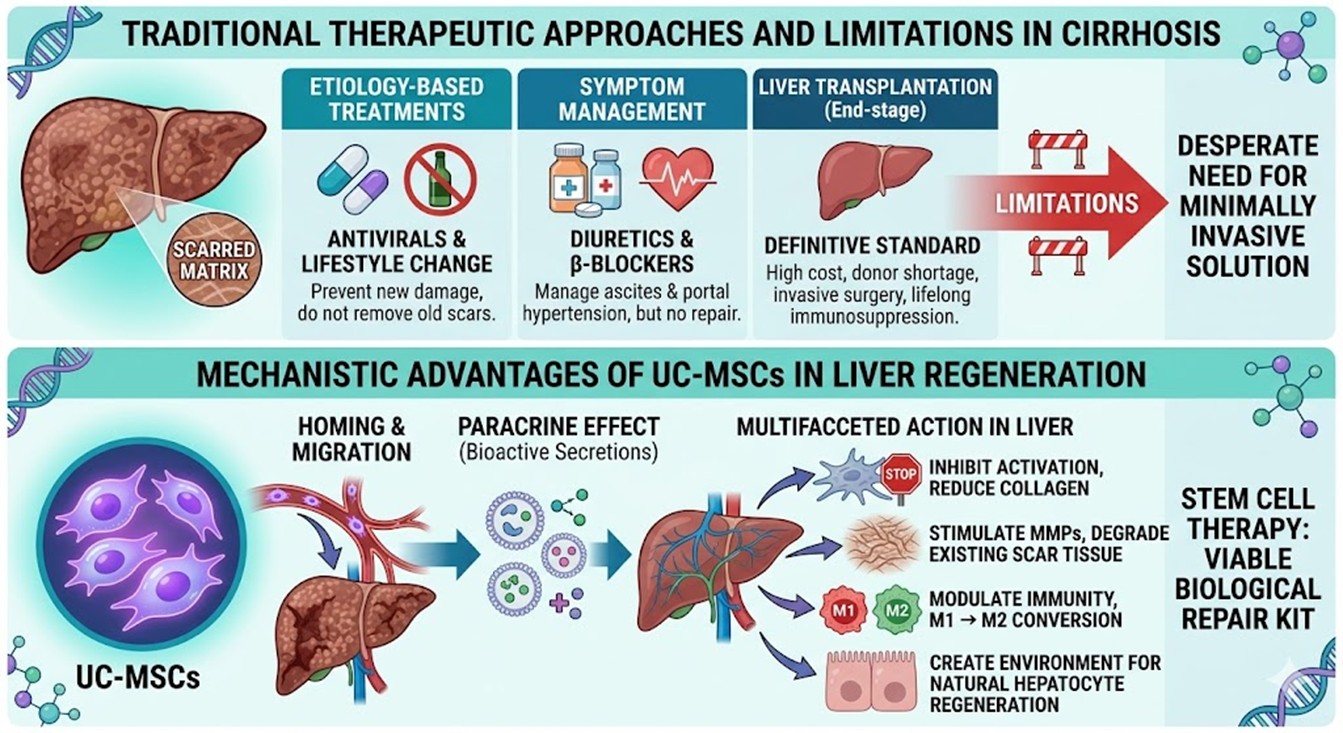
Currently, the clinical Cirrhosis management focuses heavily on etiology-based treatments, such as antiviral medications for hepatitis or lifestyle modifications for metabolic disorders. While these strategies can prevent further damage, they are largely ineffective at removing established scar tissue. Pharmacological agents like diuretics or β-blockers are used to manage symptoms such as ascites and portal hypertension, but they do not address the underlying architectural damage of the liver.
The definitive standard for end-stage liver failure remains orthotopic liver transplantation. However, this path is fraught with significant barriers. There is a chronic global shortage of donor organs, leaving many patients on waiting lists until their condition becomes terminal. Furthermore, transplantation requires lifelong immunosuppression to prevent organ rejection, which carries risks of secondary infections and kidney damage. The high cost and invasive nature of surgery make it inaccessible for many, highlighting a desperate need for a minimally invasive, biological solution like stem cell therapy to bridge the gap between symptom management and total organ replacement.
- The Mechanistic Advantages of UC-MSCs in Liver Regeneration
The transition toward using UC-MSCs in clinical research marks a pivotal shift in how we approach chronic organ failure. Umbilical cord-derived cells are favored over other sources, such as bone marrow, due to their non-invasive harvesting process, higher proliferation rate, and superior immunomodulatory properties. When introduced into a patient with Cirrhosis, these cells operate through several sophisticated biological pathways.
Firstly, UC-MSCs exhibit a powerful homing mechanism, where they migrate specifically to the sites of inflammation and tissue injury. Once localized in the liver, they execute a paracrine effect, secreting a cocktail of growth factors, cytokines, and extracellular vesicles. These secretions inhibit the activation of Hepatic Stellate Cells, effectively turning off the primary source of collagen production. Furthermore, they stimulate the production of matrix metalloproteinases (MMPs), enzymes that actively degrade the existing scarred matrix. By modulating the immune system, these cells also convert pro-inflammatory M1 macrophages into anti-inflammatory M2 macrophages, creating an environment conducive to the natural regeneration of hepatocytes. This multifaceted approach is why stem cell therapy is increasingly viewed as a viable biological repair kit for the liver.
- Integration of Stem Cell Therapy as a Modern Treatment Alternative
Choosing stem cell therapy involving UC-MSCs provides a level of therapeutic flexibility that traditional drugs cannot match. Unlike chemical compounds that target a single receptor, MSCs are living medicines that respond to the specific signals of the patient’s body. In the context of Cirrhosis, the primary goal is to shift the liver from a state of chronic wounding to a state of active healing.
UC-MSCs usage is particularly advantageous because these cells have low immunogenicity. They lack certain surface markers that usually trigger an immune response from the recipient, meaning they can be used in an allogeneic fashion without the high risk of rejection seen in organ transplants. This allows for off-the-shelf applications where cells can be prepared, characterized, and administered to patients in a timely manner. The therapeutic mechanism also includes the protection of existing hepatocytes from apoptosis (programmed cell death), thereby preserving what functional liver mass remains while the regenerative processes take hold.
- Future Perspectives and Thailand’s Role in UC-MSCs Research
Thailand is rapidly becoming a primary hub for regenerative medicine, supported by robust infrastructure and a clinical-friendly regulatory environment. The country’s transition into a destination for stem cell therapy stems from combining high-quality medical expertise with advanced laboratory capabilities for processing UC-MSCs. Strategic investments in biotechnology enable the cultivation of high-purity cell lines meeting international standards. As clinical trials prove the efficacy of UC-MSCs in reversing hepatic fibrosis, Thailand leads the integration of these therapies into routine practice. The synergy between academic research and clinical application will refine dosage protocols, making treatments more effective and accessible.
In summary, the progression from chronic inflammation to Cirrhosis historically offered few options beyond transplants. However, UC-MSCs provide transformative potential by targeting the cellular roots of fibrosis and restoring vital functions. While traditional methods manage immediate risks, mesenchymal cells offer a long-term regenerative solution. As Thailand advances its protocols, reversing liver damage is becoming a reality. This shift toward cell-based interventions represents a new chapter in medicine, providing hope for those with chronic liver disease.

