Healing Chronic Diabetes Mellitus Wounds via UC-MSCs and Stem Cell Therapy Thailand
The global rise of Diabetes Mellitus has made non-healing foot ulcers a critical public health challenge, often leading to lower-limb amputations. These ulcers are not just skin breaks but systemic indicators of vascular and neurological impairment, causing persistent pain, life-threatening infections, and a drastically reduced quality of life. For many, the body’s loss of innate repair capabilities creates an immense psychological and financial burden.
Because conventional treatments often fail to fix the underlying cellular dysfunction, the medical field is shifting toward regenerative medicine. Stem Cell Therapy Thailand has emerged as a transformative frontier in this transition. By utilizing UC-MSCs, clinicians can now target the root causes of impaired healing rather than merely managing symptoms. This shift from reactive care to proactive tissue regeneration marks a pivotal advancement in modern endocrinology and wound therapy.
1.Pathophysiological Mechanisms of Diabetic Wounds
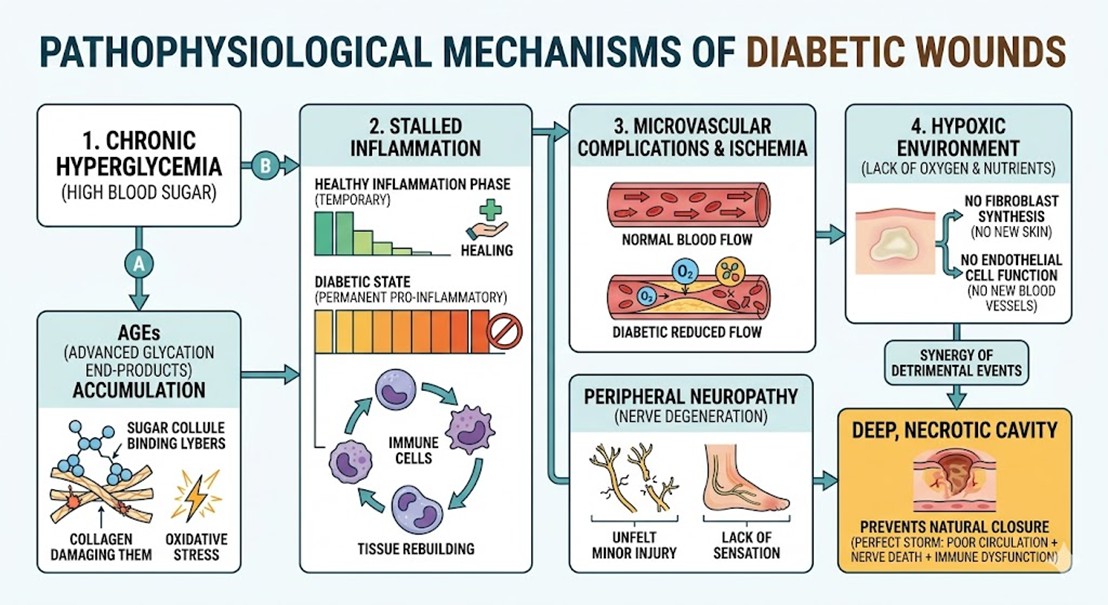
The biological environment of a patient with diabetes is characterized by chronic hyperglycemia, which triggers a cascade of detrimental cellular events. At the molecular level, high glucose levels lead to the accumulation of Advanced Glycation End-products (AGEs). These substances damage the structural integrity of collagen and promote a state of permanent oxidative stress. Furthermore, the inflammatory response in diabetic individuals is fundamentally stalled. In a healthy person, inflammation is a temporary phase that gives way to tissue rebuilding; however, in those with Diabetes Mellitus Wounds, the immune system remains trapped in a pro-inflammatory state.
Microvascular complications also play a critical role. Reduced blood flow, or ischemia, ensures that the wound site is deprived of essential oxygen and nutrients. This hypoxic environment prevents fibroblasts from synthesizing new skin and stops endothelial cells from forming new blood vessels. Over time, the localized nerves also degenerate, leading to peripheral neuropathy. This means a patient may not even feel a minor injury, allowing it to expand into a deep, necrotic cavity before medical intervention is sought. The synergy of poor circulation, nerve death, and immune dysfunction creates a perfect storm that prevents natural closure.
2.Limitations of Traditional Diabetes Mellitus Wounds Management
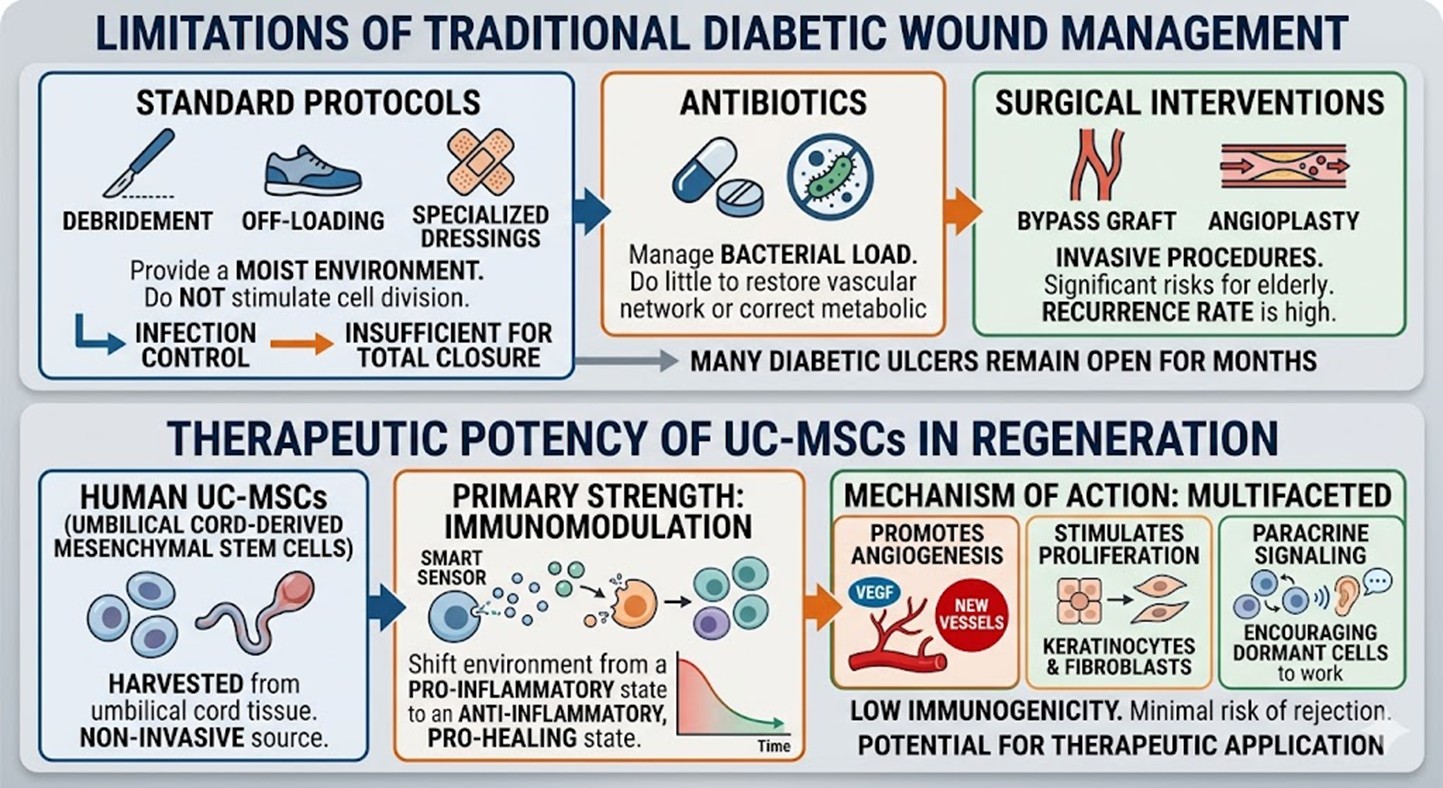
Current medical Diabetes Mellitus Wounds protocols for treating diabetic ulcers typically involve a combination of debridement, off-loading pressure from the affected limb, and the application of specialized dressings. While these steps are necessary for infection control, they are often insufficient for total closure of the wound. Standard dressings provide a moist environment but do not actively stimulate the biological machinery required for cell division and migration. Antibiotics can manage bacterial load, yet they do little to restore the damaged vascular network or correct the underlying metabolic signaling errors.
Furthermore, many Diabetes Mellitus patients undergo surgical interventions to restore blood flow, such as bypass grafting or angioplasty. While helpful, these procedures are invasive and carry significant risks for elderly or frail individuals. Statistics show that even with high-quality conventional care, a substantial percentage of diabetic ulcers remain open for months or years, leading to a recurrence rate that is frustratingly high. The limitations of these older techniques have created a desperate need for a therapy that can reboot the healing process at a microscopic level, leading many to seek the specialized expertise found within Stem Cell Therapy Thailand.
3.Therapeutic Potency of UC-MSCs in Regeneration
Umbilical Cord-derived Mesenchymal Stem Cells, commonly known as UC-MSCs, offer a superior biological profile for treating complex wounds. These cells are harvested from the umbilical cord tissue after healthy births, making them a non-invasive and ethically sound source of regenerative power. Their primary strength lies in their remarkable immunomodulatory capabilities. When introduced to the site of Diabetes Mellitus Wounds, these cells act as smart sensors, secreting cytokines and growth factors that shift the wound environment from a pro-inflammatory state to an anti-inflammatory, pro-healing state.
The mechanism of action is multifaceted. First, UC-MSCs promote angiogenesis, which is the formation of new blood vessels. They release Vascular Endothelial Growth Factor (VEGF) to rebuild the damaged circulatory pathways, ensuring the wound receives the oxygen it needs to survive. Second, they stimulate the proliferation of keratinocytes and fibroblasts, the essential building blocks of the skin. Third, these cells exhibit paracrine signaling, effectively talking to the patient’s own dormant cells and encouraging them to return to work. Unlike other cell types, these mesenchymal cells have low immunogenicity, meaning the risk of the patient’s body rejecting them is minimal, making them an ideal candidate for therapeutic application.
- The Future of UC-MSCs and Diabetes Wound Therapy in Thailand
Thailand is now a premier hub for Stem Cell Therapy, driven by stringent regulations and world-class medical facilities. Thai researchers are leading clinical trials to optimize UC-MSCs for chronic conditions, particularly metabolic diseases. The country’s advanced infrastructure ensures high-tech, sterile processing, delivering potent and safe cellular products.
The future suggests these therapies will become a primary treatment pillar rather than a last resort. Through a strategic focus on biotechnology and medical tourism, Thailand offers cutting-edge science alongside comprehensive patient care. As long-term data on UC-MSCs for Diabetes Mellitus Wounds grows, Thailand’s integration of cellular medicine into healthcare is set to become a global benchmark, offering affordable access and high scientific standards.
Summary
Managing chronic diabetic ulcers requires moving beyond traditional, passive treatments. The biological complexity of these wounds—involving inflammation, vascular failure, and cellular senescence—demands the regenerative power of UC-MSCs. By harnessing natural signaling, this therapy overcomes healing hurdles that conventional methods cannot.
Advancements in Stem Cell Therapy Thailand provide hope for those facing amputation or chronic pain. By targeting deep cellular mechanisms like angiogenesis and immune modulation, UC-MSCs offer true tissue restoration. As research evolves, these sophisticated biological interventions will redefine global standards of care for metabolic complications, ensuring better outcomes and a higher quality of life.

